Dr Pamela Page 💙 retweeté

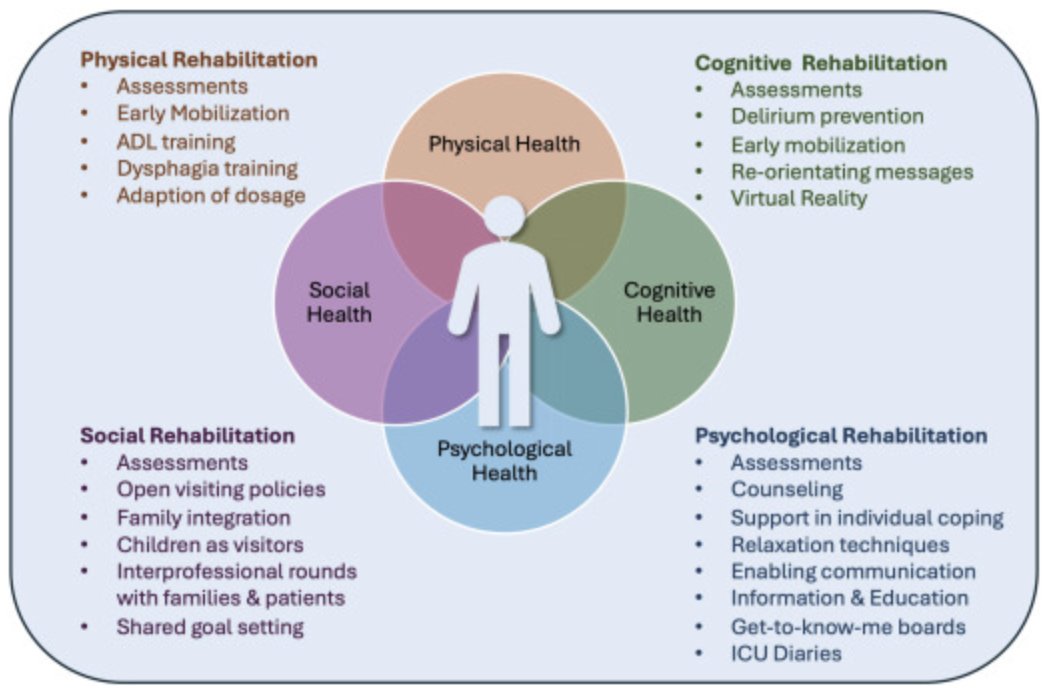
How to apply person-centered care, using personal questions by a get-to-know-me-board, a pad, or el. charts.
@Luda_Karnatovsk
Good reading: Moon 2026 pubmed.ncbi.nlm.nih.gov/41836938/

English
Dr Pamela Page 💙
7.2K posts


@PamPage16
Critical care nurse and academic, passionate about person and family centred care. 2019 Churchill Fellow, ICUsteps trustee.