MuvennKannan
529 posts











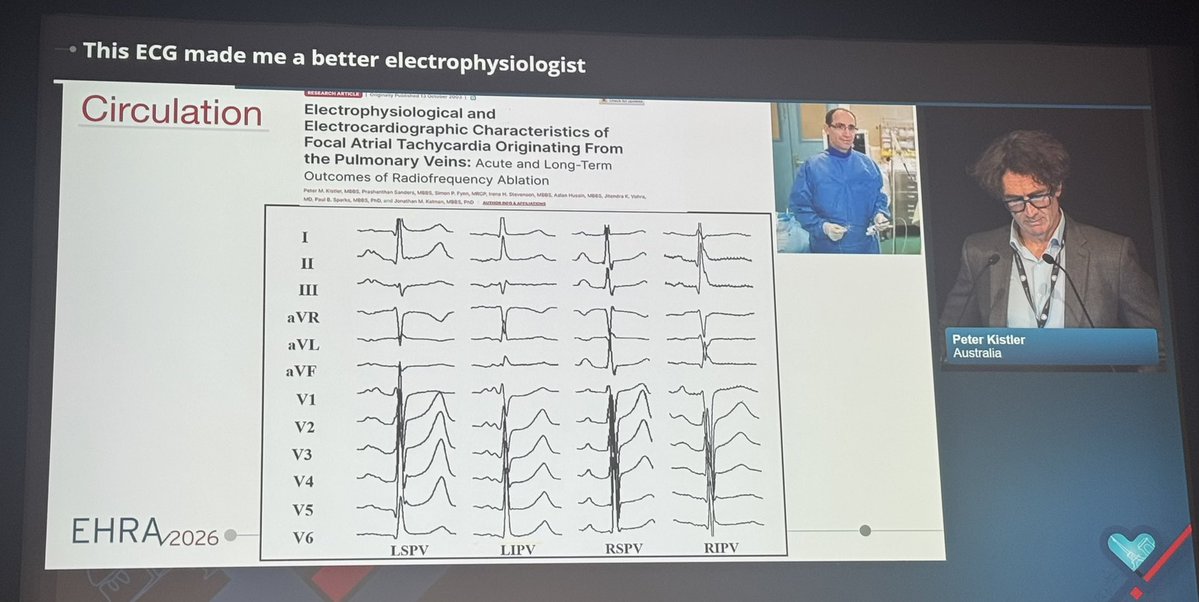
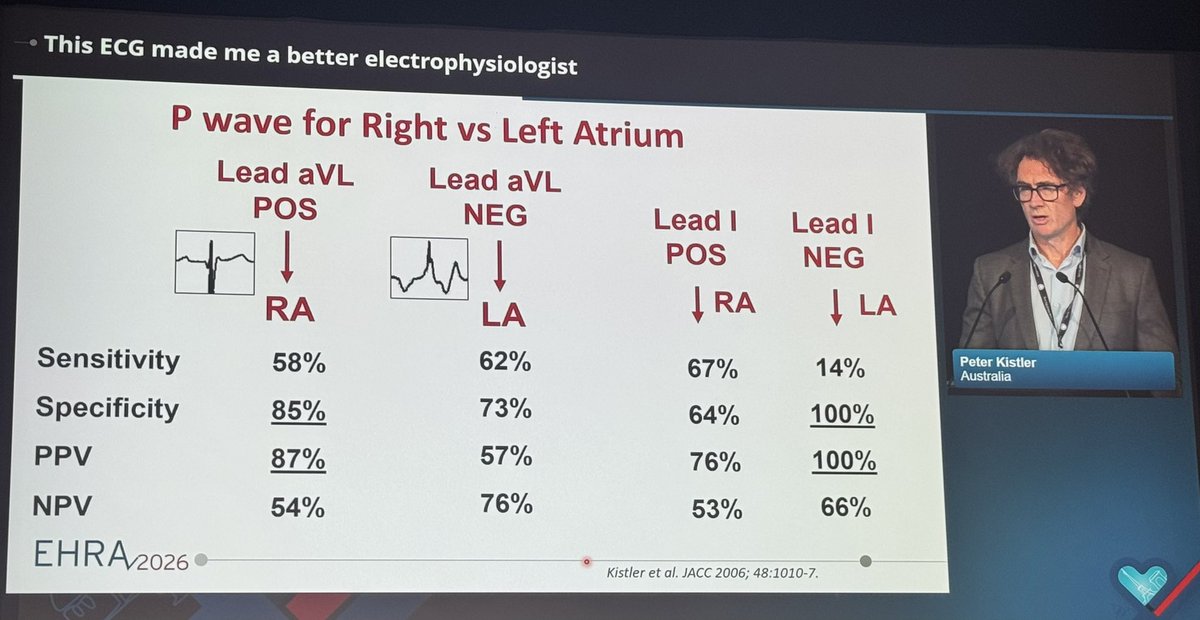


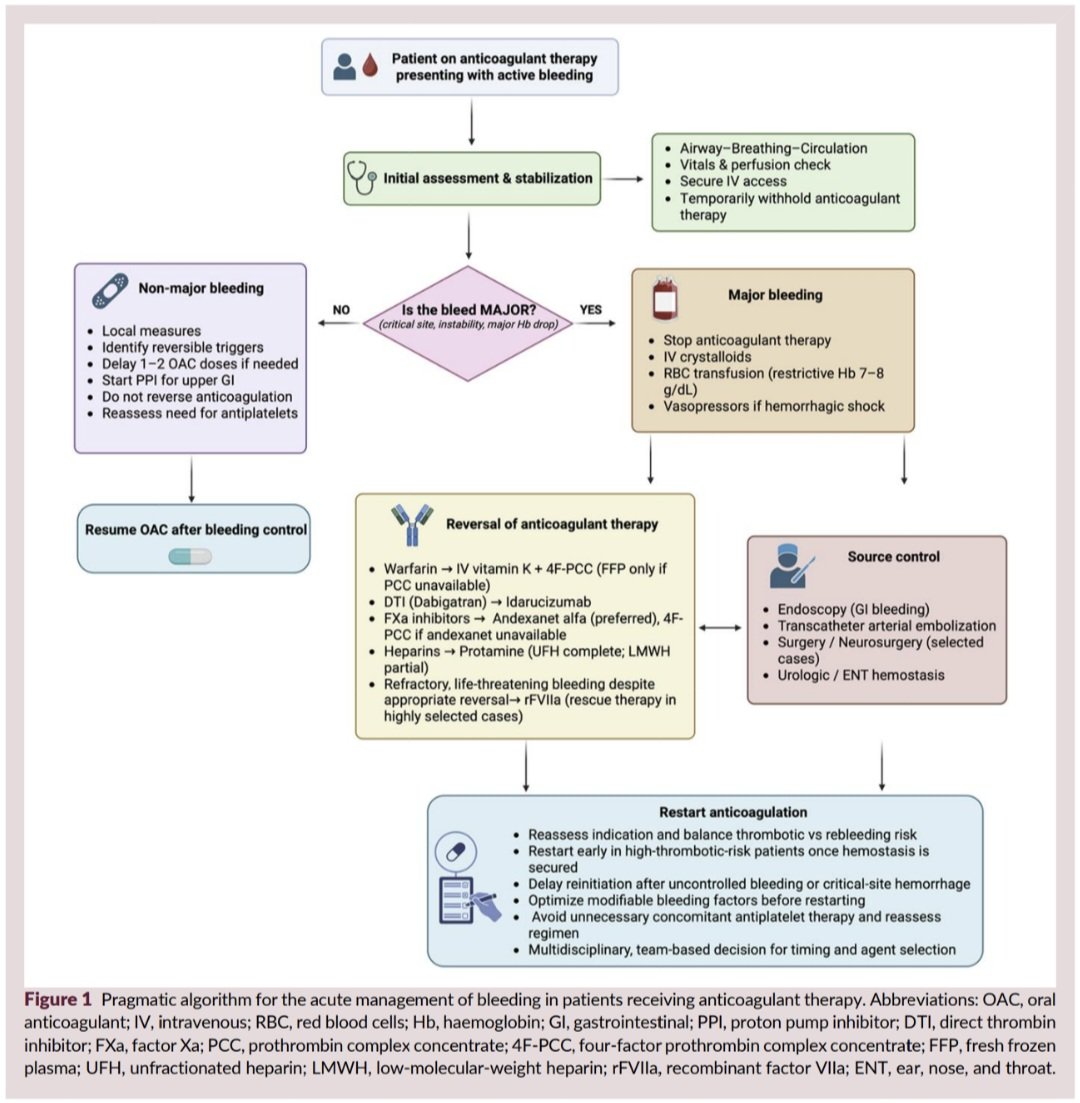



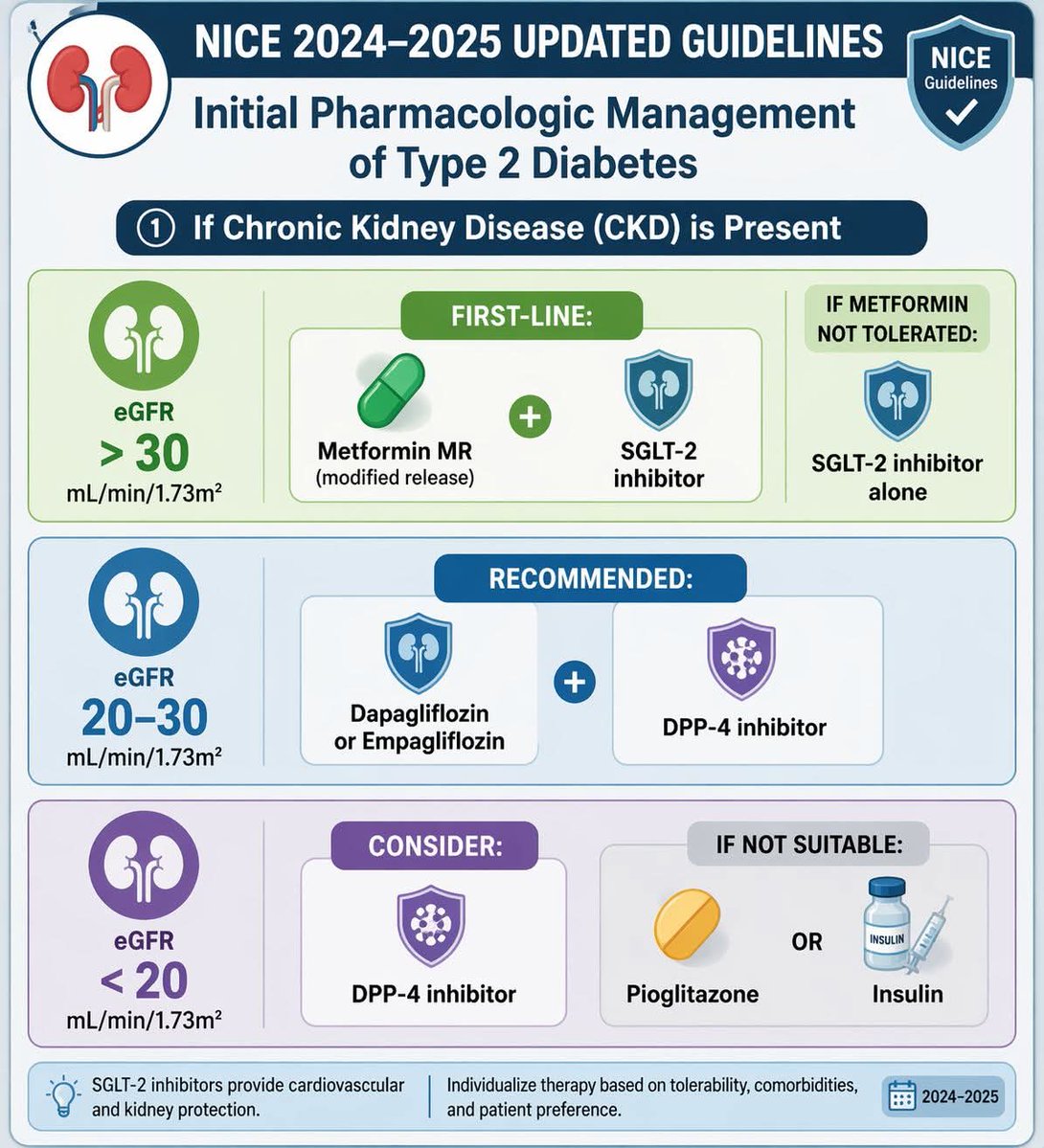
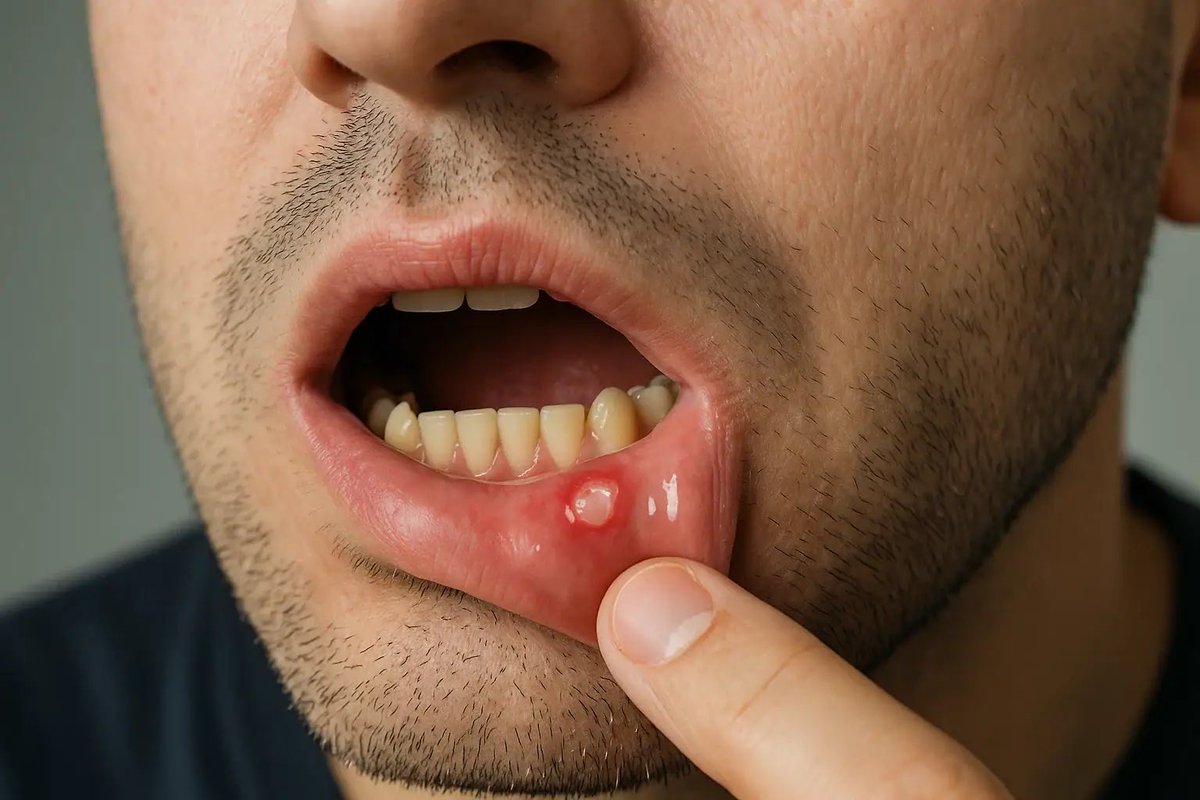
Do you know the correct answer ?? Drop your answer in the Comment ..... @dr_manish_ydv @Dr_Shiv_kumar_ @DrNovinoTailor @drobiy12 @hemo_shk @fzn733





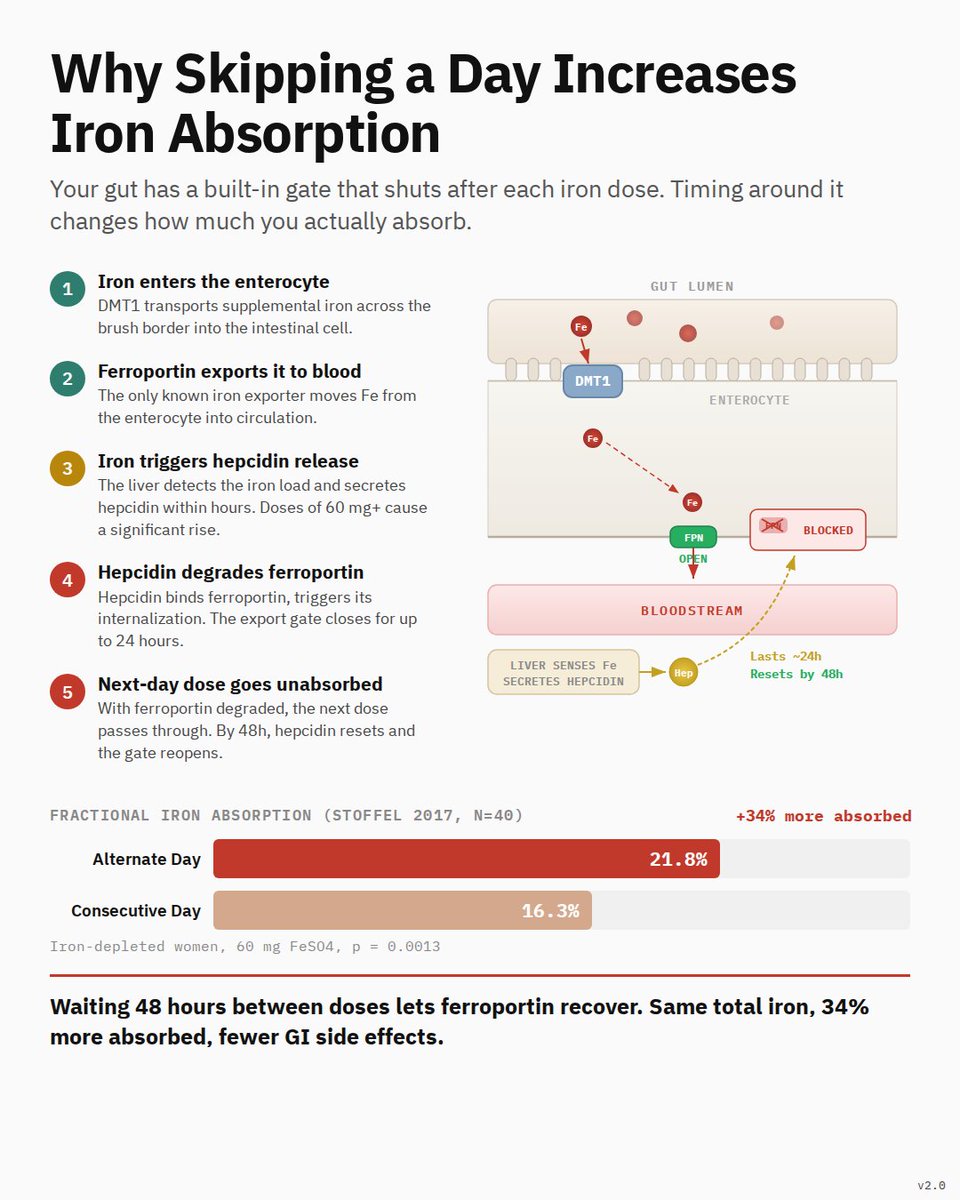






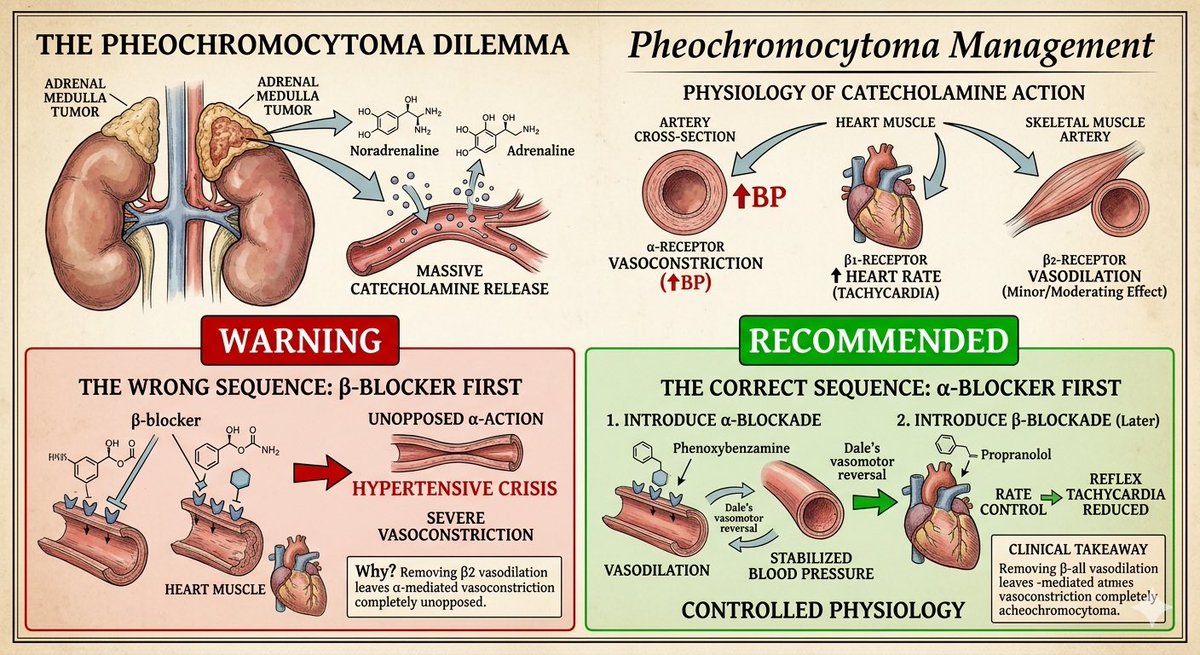
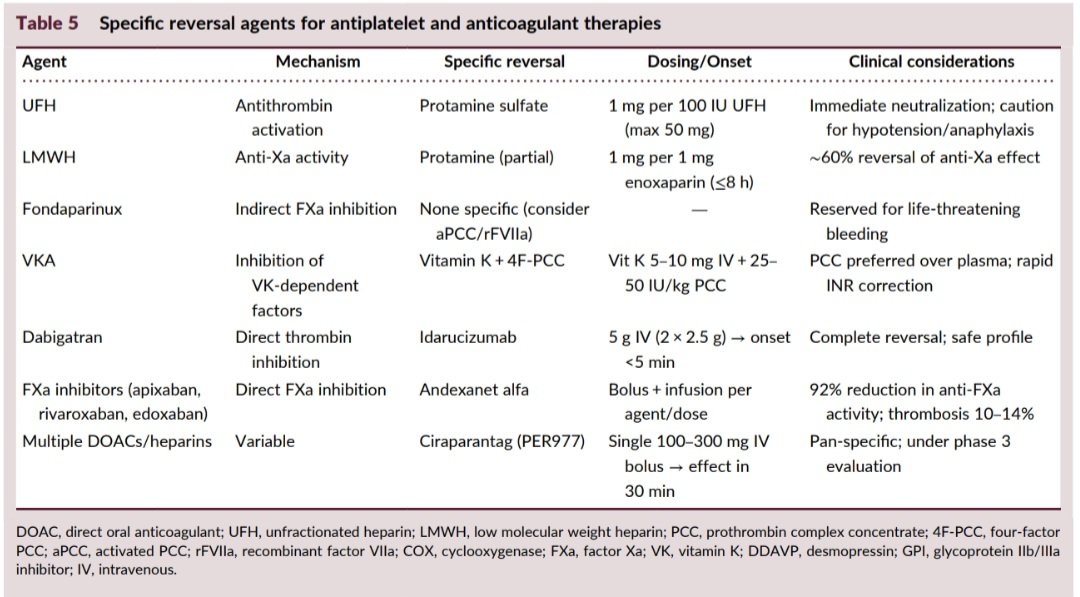
🚨 Endocrinology pearls you should never miss as a clinician 1️⃣ If you see elevated calcium, this is how you should think as a clinician? Most people remember “Stones, Bones, Groans & Psychiatric Overtones.” But that mnemonic doesn’t help you find the cause. What matters is a structured approach. When you see hypercalcemia, pause! think systematically. 🟢 FIRST RULE - CHECK PTH Your first lab is PTH. Don’t shotgun investigations. Don’t jump to imaging. PTH divides hypercalcemia into two diagnostic pathways. 🟢 INTERPRET THE PTH Only two possibilities: 🔻 PTH ↑ / inappropriately normal → PTH-mediated hypercalcemia 🔻 PTH ↓ → Non-PTH mediated hypercalcemia This single fork determines the entire work-up. 🟢 PATHWAY 1 : PTH HIGH → THINK PARATHYROID 🔴 Primary Hyperparathyroidism (Most common outpatient cause) Usually due to parathyroid adenoma (~85%). 🟢Mechanism :- PTH acts at three sites: 🔺Bone → osteoclast activation → calcium release 🔺Kidney → ↑ calcium reabsorption 🔺Kidney → ↑ vitamin D activation → ↑ gut absorption Net effect → persistent hypercalcemia. 🔻Typical Labs ↑ Calcium ↑ PTH ↓ Phosphate ↑ ALP ↑ Urinary calcium 🔻Why phosphate low? PTH causes phosphaturia by inhibiting Na-phosphate transporters in proximal tubule. 🔴 Familial Hypocalciuric Hypercalcemia (FHH) Mutation in calcium-sensing receptor. 🔻Typical Labs Mild ↑ Calcium Normal / mild ↑ PTH LOW urinary calcium ← key clue Normal phosphate Patients are asymptomatic → no surgery needed. 🔴 Tertiary Hyperparathyroidism Seen in long-standing CKD. Chronic stimulation → parathyroid glands become autonomous. 🔻Typical Labs ↑ Calcium ↑↑ PTH ↑ Phosphate ↓ Vitamin D 🟢 PATHWAY 2 :- PTH LOW → NON-PTH CAUSES If PTH is suppressed, calcium is coming from somewhere else. 🔴 Malignancy-Associated Hypercalcemia (Most common inpatient cause) Mechanisms: PTHrP secretion Osteolytic metastasis Excess vitamin D (lymphoma) 🔻Labs ↑ Calcium ↓ PTH ↑ PTHrP ↑ ALP 🔴 Multiple Myeloma Due to osteolytic bone destruction. 🔻Labs ↑ Calcium ↓ PTH ↑ ESR ↑ Total protein M-spike on SPEP CRAB C → Calcium R → Renal failure A → Anemia B → Bone lesions 🔴 Vitamin D Toxicity Usually from supplement overdose. 🔻Labs • ↑ Calcium • ↓ PTH • ↑ 25-OH Vitamin D • ↑ Phosphate 🔴 Granulomatous Diseases (Sarcoidosis, TB) Macrophages produce excess 1-α hydroxylase → ↑ active vitamin D. 🔻Labs ↑ Calcium ↓ PTH ↑ 1,25-OH Vitamin D ↑ ACE 🔴 Milk-Alkali Syndrome Excess calcium + absorbable alkali. Common sources: Calcium carbonate antacids Calcium supplements Calcium + vitamin D tablets Classic triad Hypercalcemia Metabolic alkalosis Renal dysfunction 🟢 CLINICAL CHEAT CODE If Calcium ↑ Step 1 → Check PTH PTH ↑ → Parathyroid causes PTH ↓ → Malignancy, Vitamin D excess, Granulomatous disease, Drugs One lab directs the entire diagnostic pathway. #MedTwitter #MedX #Endocrinology