MuvennKannan retweetou

A #CardioNuggets 🧵👇
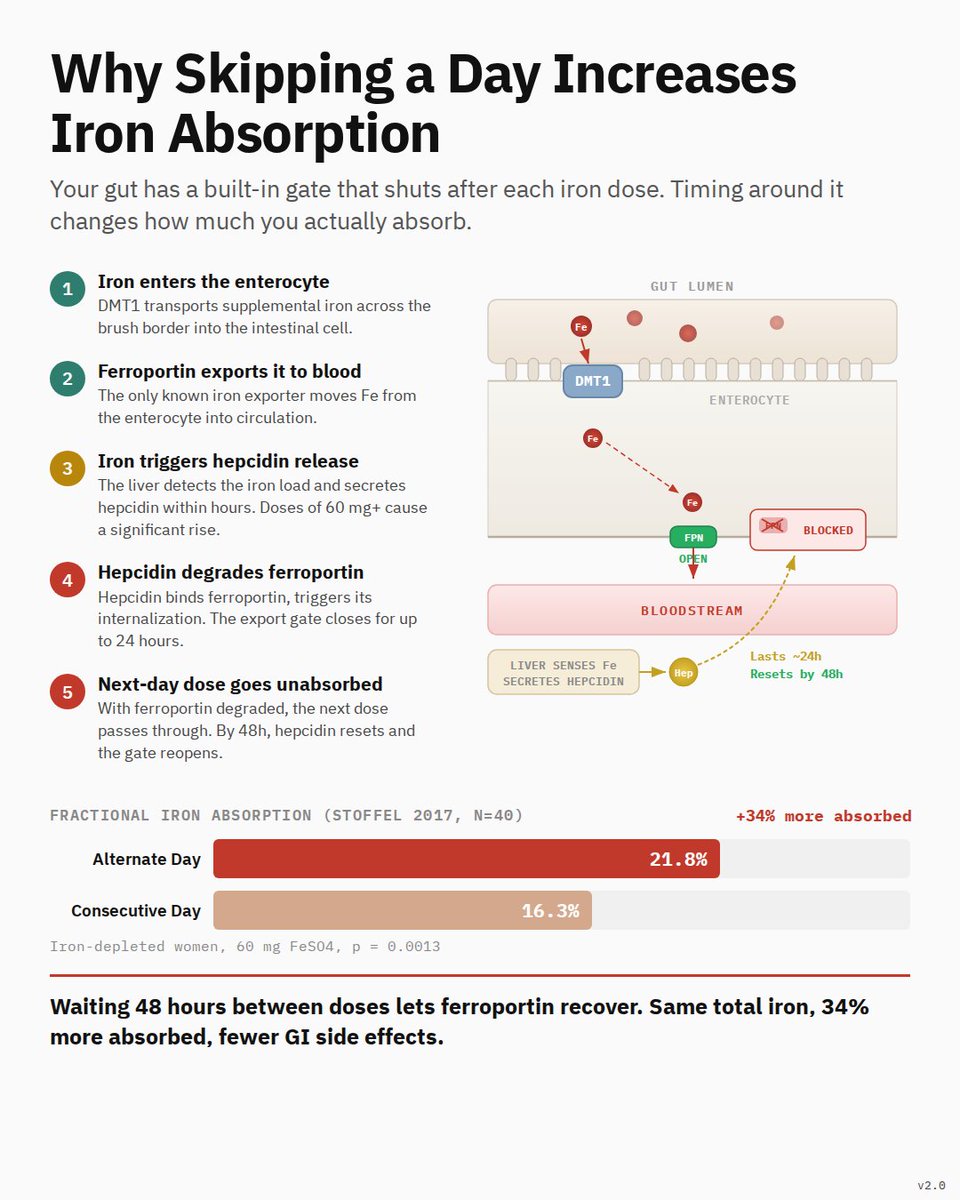
🫀Not all HOCM hearts are shaped the same.
There are 5 distinct LV cavity phenotypes, each with unique implications for obstruction, arrhythmia risk & management.

English
MuvennKannan
531 posts















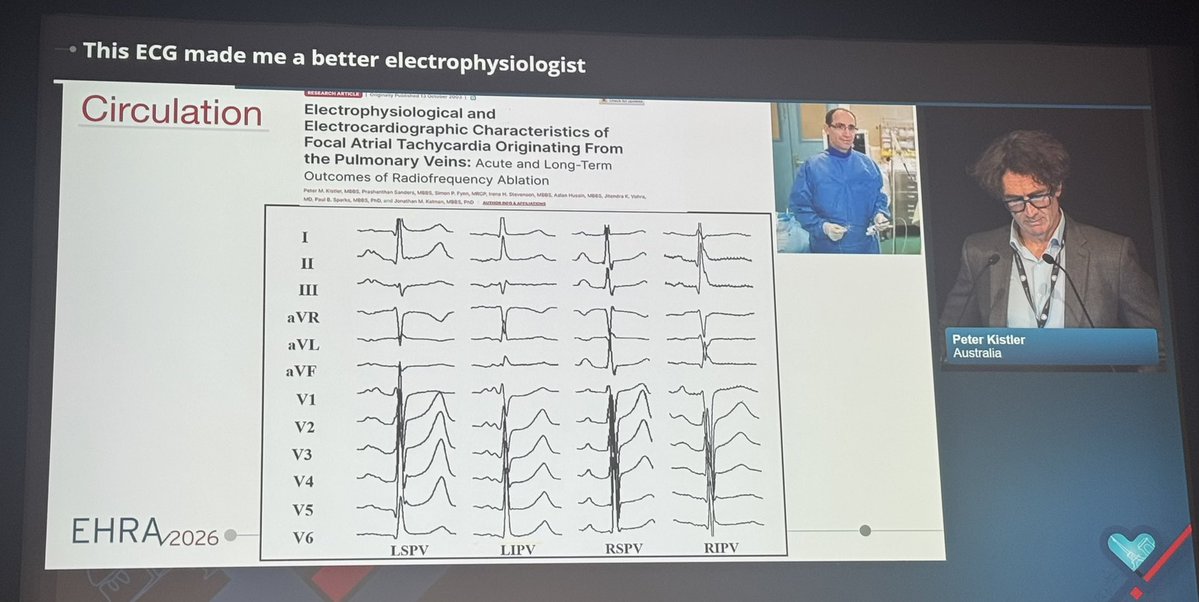
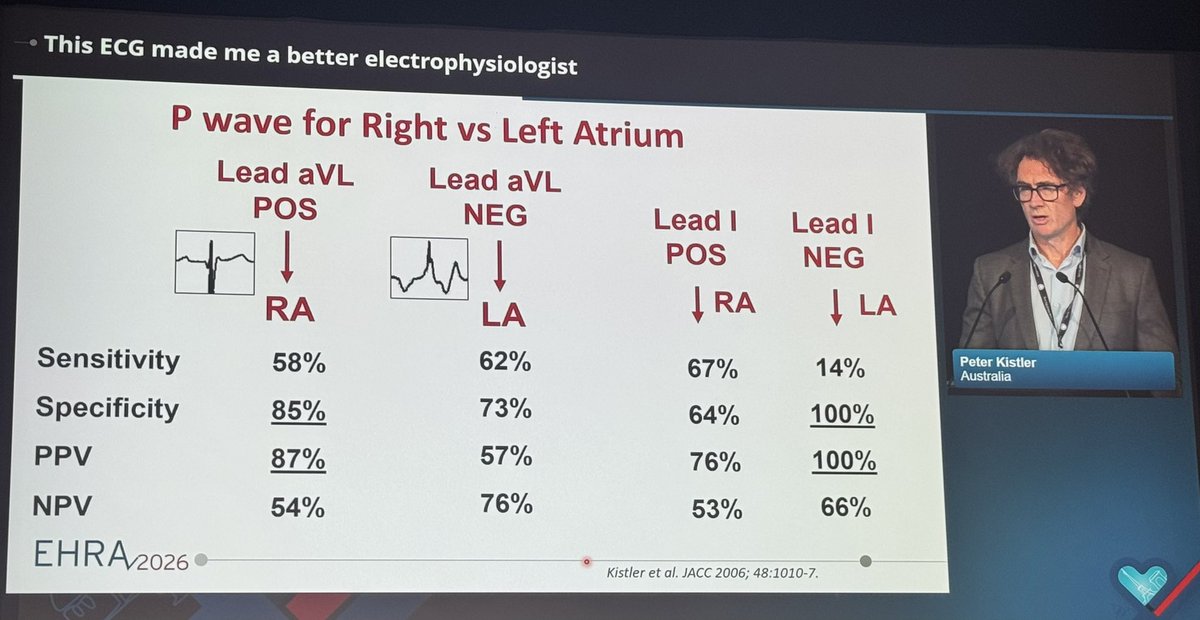


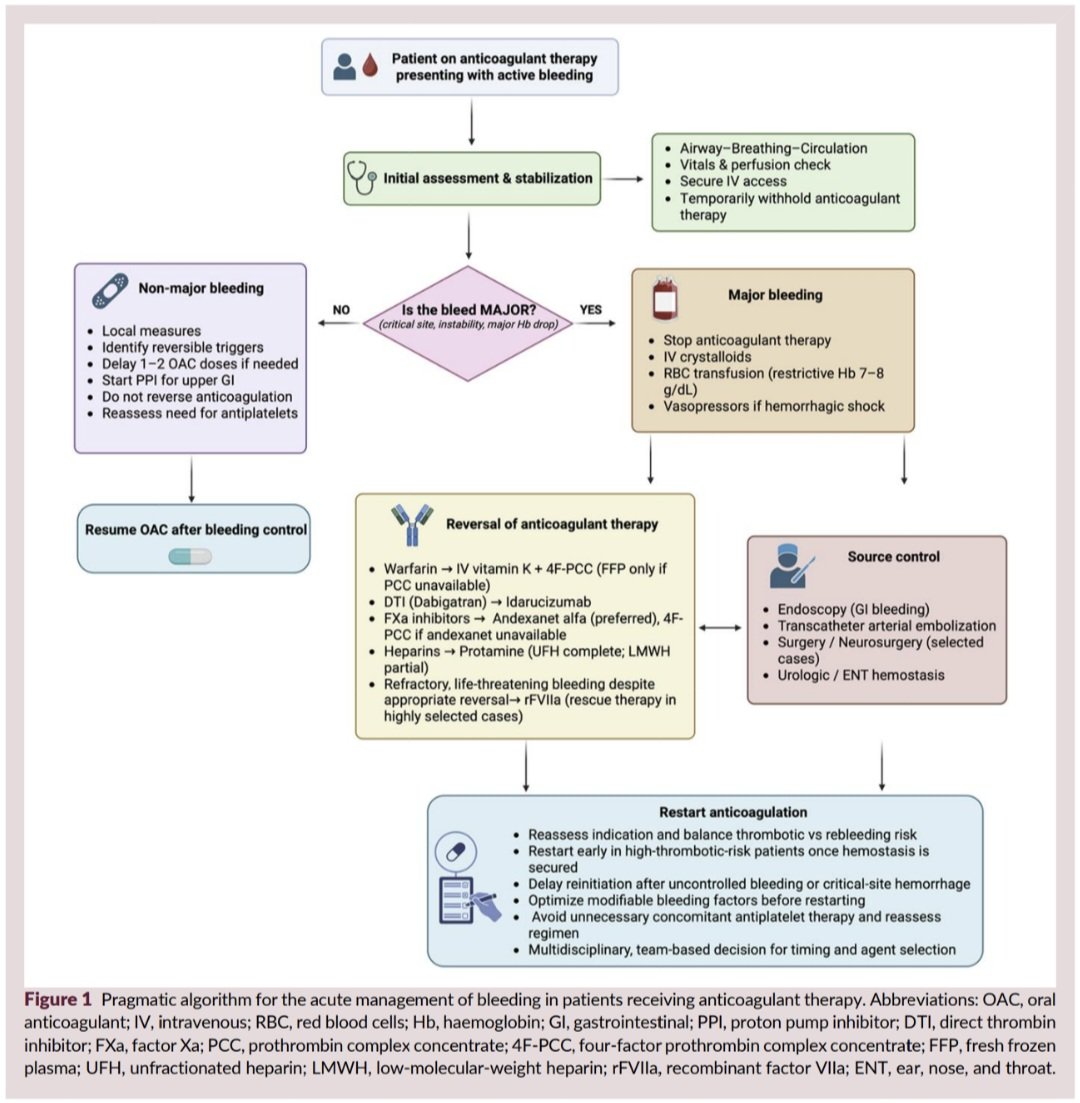
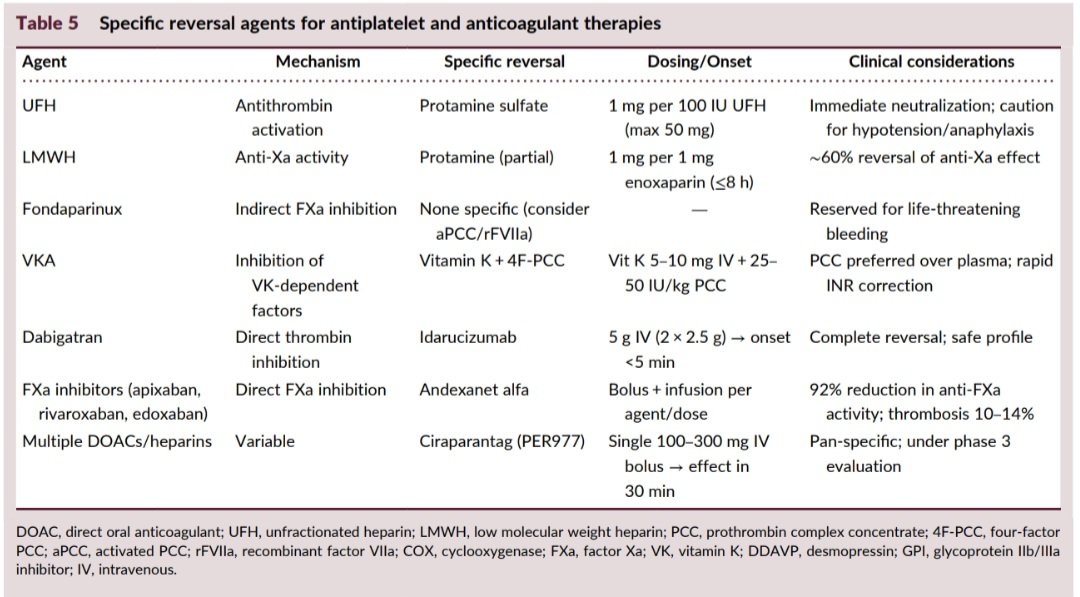



Do you know the correct answer ?? Drop your answer in the Comment ..... @dr_manish_ydv @Dr_Shiv_kumar_ @DrNovinoTailor @drobiy12 @hemo_shk @fzn733