Tweet fijado
🌵💋🐝
39.8K posts


🌵💋🐝
@CallMeIPIIN
Ouroboros in constant flux.
Tamale, Ghana Se unió Eylül 2010
597 Siguiendo811 Seguidores
🌵💋🐝 retuiteado
🌵💋🐝 retuiteado

I asked my gynecologist, who specializes in endometriosis, if he, after seeing so many cases, agrees with the claim that endometriosis is a rare condition. He laughed and said, “Absolutely not. What it is is underdiagnosed, misunderstood, and mismanaged.” That’s exactly what I’ve observed over the years talking to other women. I don’t have a medical degree, but I know a suspiciously "for a “rare” condition" high number of women with endometriosis.
English
🌵💋🐝 retuiteado

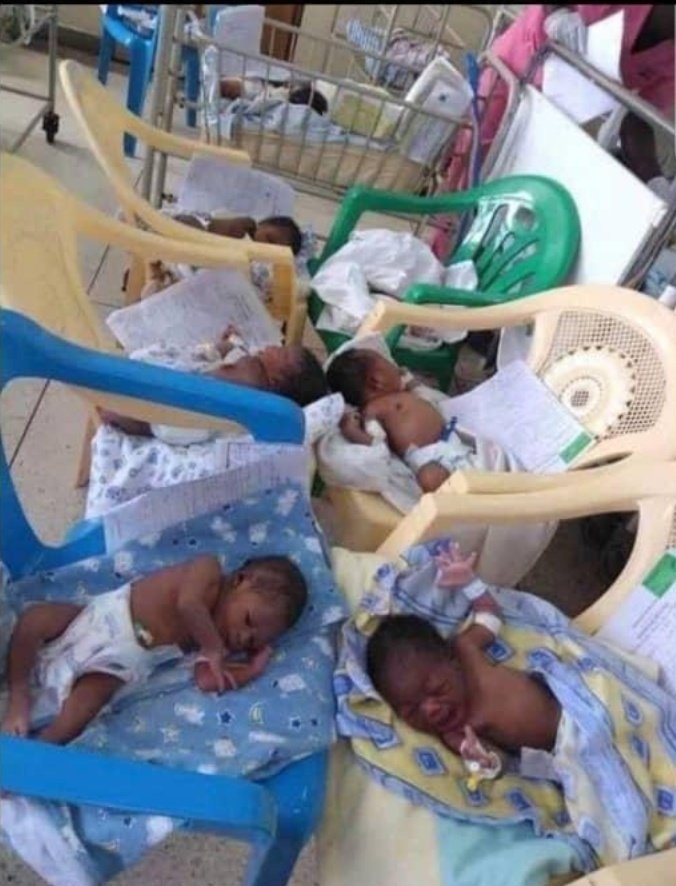
Many things can go wrong here and we'd still blame the devil when we're clearly our own problem
This is a government hospital by the way
This hospital has a leadership that oversees the affairs of the facility
They generate money from patient's care
How much is baby cot? We have many welders who can fabricate baby cot, and the cost would still be favourable. Why can't the leadership of this hospital do that?
If a child roll over and dies, the CMD will deny knowing that these things are happening under his nose.
We see things like this because, the leadership has refused to take responsibility, and frankly, they don't care.
English
🌵💋🐝 retuiteado

Imagine you are in a serious road traffic crash in Accra tonight.
Or imagine a friend/relative suddenly collapses at home from cardiac arrest.
In that moment, nobody is thinking about politics.
Your family is asking one question:
Can Ghana’s emergency system keep you alive long enough to reach definitive care?
That is the only question that matters.
⸻
Now ask the harder question:
What are your chances of surviving a time-critical emergency in a system where we’ve normalized the phrase “No Bed Syndrome”?
That phrase sounds like a hospital crowding problem.
It’s not.
“No Bed Syndrome” is a symptom of a poorly functioning emergency care system.
The bed is just the final explanation the public hears.
The failure often starts much earlier.
⸻
The World Health Organization is clear on this:
Emergency care is not a ward or bed.
It is a system, from:
→ The scene
→ To transport
→ To the facility
→ Too early inpatient care
Survival depends on the full chain, not just what happens at a hospital entrance.
So Ghana must stop discussing “No Bed Syndrome” as if it’s only a space problem.
It is the public name for an emergency system failure.
⸻
After every tragedy, we repeat the same cycle:
People blame one doctor.
One nurse.
One hospital.
The debate becomes emotional.
Then the country moves on.
That cycle is exactly why the problem persists.
Yes, individual accountability matters.
Yes, professional ethics matter.
Yes, hospital leadership matters.
But when multiple facilities fail one patient in sequence, the problem is no longer only individual.
It is structural.
Because:
A doctor cannot create a referral network during a crisis.
A nurse cannot produce an ambulance without fuel.
A hospital cannot function as a national emergency system on its own.
If we keep asking frontline staff to compensate for weak coordination, weak transport, weak communication, and weak operational rules…
…then Ghana will keep producing the same headlines.
⸻
A functioning emergency system requires:
→ Trained personnel
→ Vehicles and dispatch
→ Equipment and essential supplies
→ Communication and information systems
→ Clinical + operational protocols
→ Accountability that is measurable, not rhetorical
Public anger is valid because the public understands something policy debates often avoid:
A person in an emergency should not have to negotiate the health system while dying.
That is the real meaning of “No Bed Syndrome.”
It is not a phrase about beds.
It is a warning that Ghana has allowed emergency care to operate without the coordination, readiness, standards, and accountability required to save lives reliably.
⸻
If Ghana wants to prove that human life is truly a national priority,
This is where the proof must begin.

English
🌵💋🐝 retuiteado
🌵💋🐝 retuiteado
🌵💋🐝 retuiteado
🌵💋🐝 retuiteado

Dr Stephanie Chiaky Otuteye opens up about cyberbullying and the alleged unfair treatment she faced following her Miss Intercontinental Ghana win. #ShowbizAtoZ
English
🌵💋🐝 retuiteado

Can’t say same cos I have to wait at least 2-3 months before my salary is processed👍🏾
DEDE!@minutesimal_
9-5ers, nextweek is salary week
English
🌵💋🐝 retuiteado

I really don’t know how it works in other medical colleges in our country, but in my college the situation is pathetic.
You can’t work in such an environment.
Constant taunts from seniors.
Seniors firing juniors.
Expecting us to do clerical work.
Collecting hard copies of reports of every patient while taking shit from the lab assistants.
It’s like these lab assistants give us so much attitude as if they are doing some favor to us.
Imagine standing outside the labs for the entire night while we can only talk to them through this small window, which is 90% closed.
Imagine a poor intern (me) standing there at 3 a.m. with no sleep, probably 20k steps done, and begging for a report which, if not collected within certain minutes, can get me shouted at and humiliated.
We have been constantly called from the ward to carry blood samples from ward to lab because either the MTS is on lunch break, tea break, dinner break, is late, or is too busy.
We are so busy doing this stupid job that I haven’t got any chance to do any procedure or anything.
And my interest in doing any procedure has come down to zero.
I know nobody’s going to read this, and even if it is read by millions, nothing’s going to change.
We are supposed to be happy in this work because we are getting paid (peanuts!).
This is the worst experience.
Adding a picture of me pretending to smile till I actually am happy.


English
🌵💋🐝 retuiteado
🌵💋🐝 retuiteado
Sometimes a patient comes to the hospital for one problem, only for the doctor to discover something far bigger, especially when what brought them in is far easier to fix than the issue staring back at you.
It’s my routine to examine both eyes whenever a patient sits at the slit lamp. I use that moment to screen the “good” eye. So, I usually start there before moving on to the eye with the complaint. If I had a dollar for every time a patient stopped me to say, “Doctor, you’re examining the wrong eye,” I would be rich by now. All my mother’s financial problems would be solved.
I bring this up after weeks of reflection. Lately, I have been beaten down. Whenever young people walk into my clinic with a simple eye problem and leave with a shuttered world, burdened by multiple diagnoses, some medically incurable, I am left with a deep sense of helplessness.
There was one such case: a vibrant young soul who had sustained an eye injury two years earlier, resulting in a cataract. As usual, I began by examining the good eye. A careful look at the optic nerve head, the nerve that connects the eye to the brain revealed a subtle change, one many would easily ignore: a small inferior notch. It was a quiet sign of glaucoma in its earliest stage.
I could have brushed it off as “normal” had it not been for the additional training I had in India. After all, the eye sees only what it knows. But I didn’t. Dr. Divya, the ophthalmologist who taught me how to detect subtle changes on the optic nerve during my stay in India would have been proud.
Often, during prayer, I question God about the things that are unclear to me. One of those questions has always been my career path. Not long ago, as I paced back and forth in my living room, I asked Him again: 'Why did I have to go to India for training? I barely have the resources to use what I learned. I’m slowly losing the skills I worked so hard to acquire. What was it all for?'
Then I thought about this patient.
I realized that God can move heaven and earth for just one person. That I was hustling in India, hating the food, the weather, and the relentless work just so that one patient, from a deep village in Kaabong, could one day save money for an entire year, board a bus, and come to see me for a seemingly simple eye problem… while God had already foreseen the much bigger one that needed attention.
After spotting the abnormality, I checked his intraocular pressure. It was 30 mmHg, well above the normal range of 10–21 mmHg. That confirmed it: what I had seen on the optic nerve was no coincidence. He had glaucoma, caught at the earliest stage I had ever encountered. I say early because most patients come when it is already too late, when the optic nerve has been irreversibly eaten away.
As part of routine care, I checked his blood pressure. It was 180/103 mmHg. Alarmingly high—especially for someone so young. I sent him for renal and liver function tests and contacted a physician for review. Hypertension in a young person raises many questions.
The lab results returned normal, but that was not a relief either. Because what was causing it then? We agreed with the physician to see him after a month and instructed him to monitor and record his blood pressures daily so that we could decide the next phase of treatment.
Definitely the eye surgery had to be put on hold, but the Glaucoma treatment was initiated immediately.
So, a young soul who came in with a “simple” traumatic cataract walked out with a diagnosis of glaucoma in his good eye and systemic hypertension, two chronic conditions requiring lifelong medication and endless hospital visits.
Cases like this remind me that taking time with a patient is never mundane. That seeing the whole person, not just the eye, is not a cliché. And that checking the “good” eye is not optional. It is essential.

English
🌵💋🐝 retuiteado
🌵💋🐝 retuiteado
🌵💋🐝 retuiteado
🌵💋🐝 retuiteado

To:
Male medical ward for sphyg
NICU outborn for pulseoximeter
ENT ward for Suctioning machine
A&E for oxygen
GOPD for continuation sheet
Should I continue?🌝
Tolulope, the Unstoppable.@thedigitamaven
People who walk 10k steps, where do you guys walk to?😭
English
🌵💋🐝 retuiteado

There's more to this email than meets the eye.
Simons@Simon_Ingari
Stop using "please find attached" in your emails.
English
🌵💋🐝 retuiteado

Anyone in medicine
fluttershy@hwrtyed
laying in bed with the nervous system of someone who’s going to war
English











