Sabitlenmiş Tweet

➡️HOT FROM THE PRESS
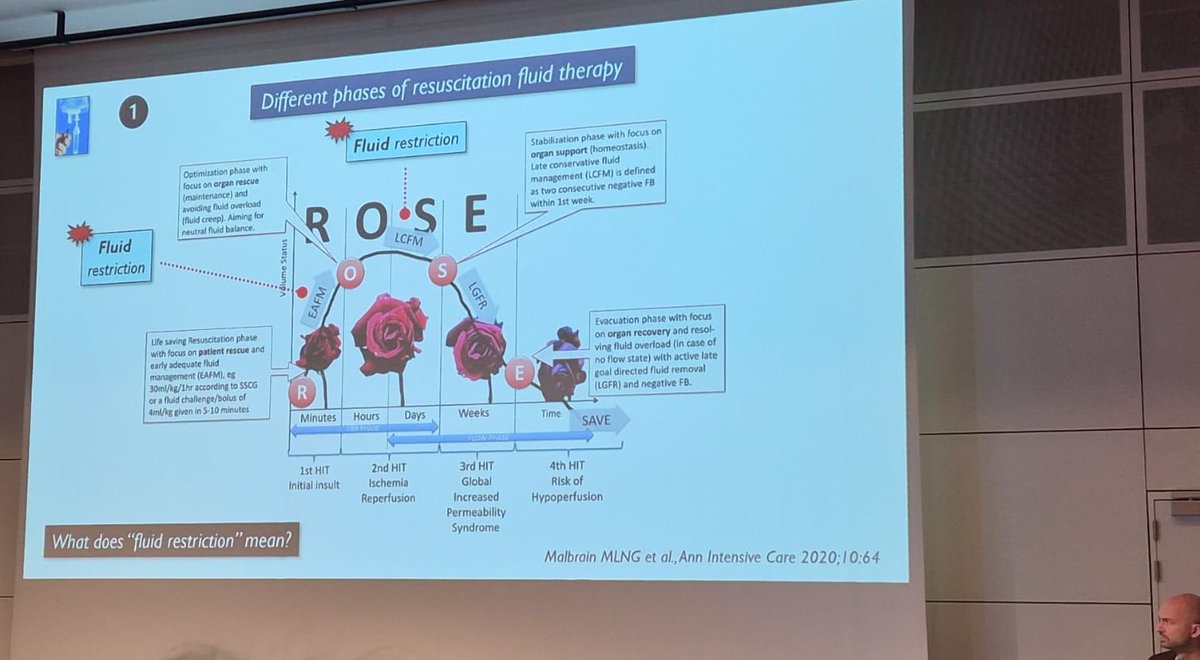
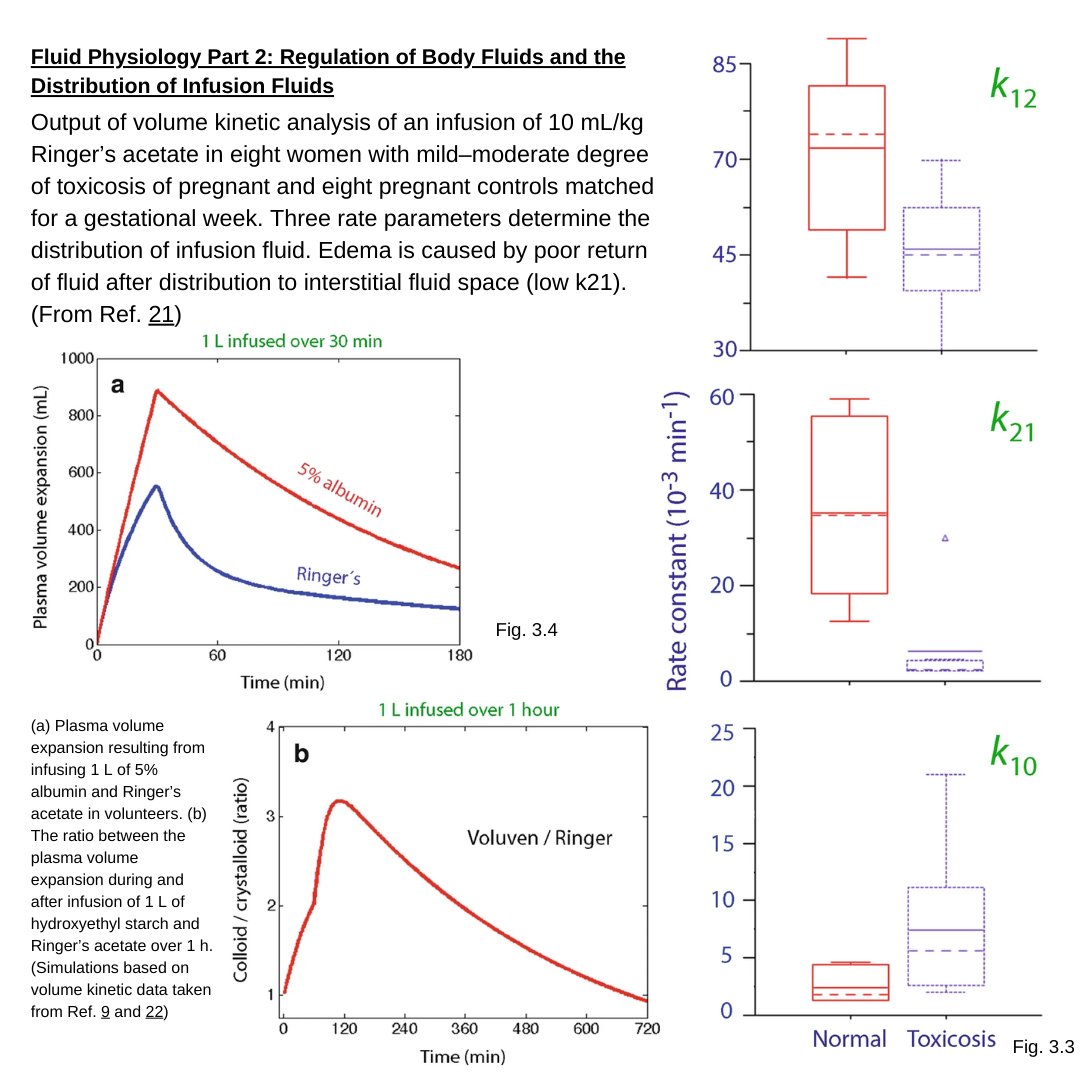
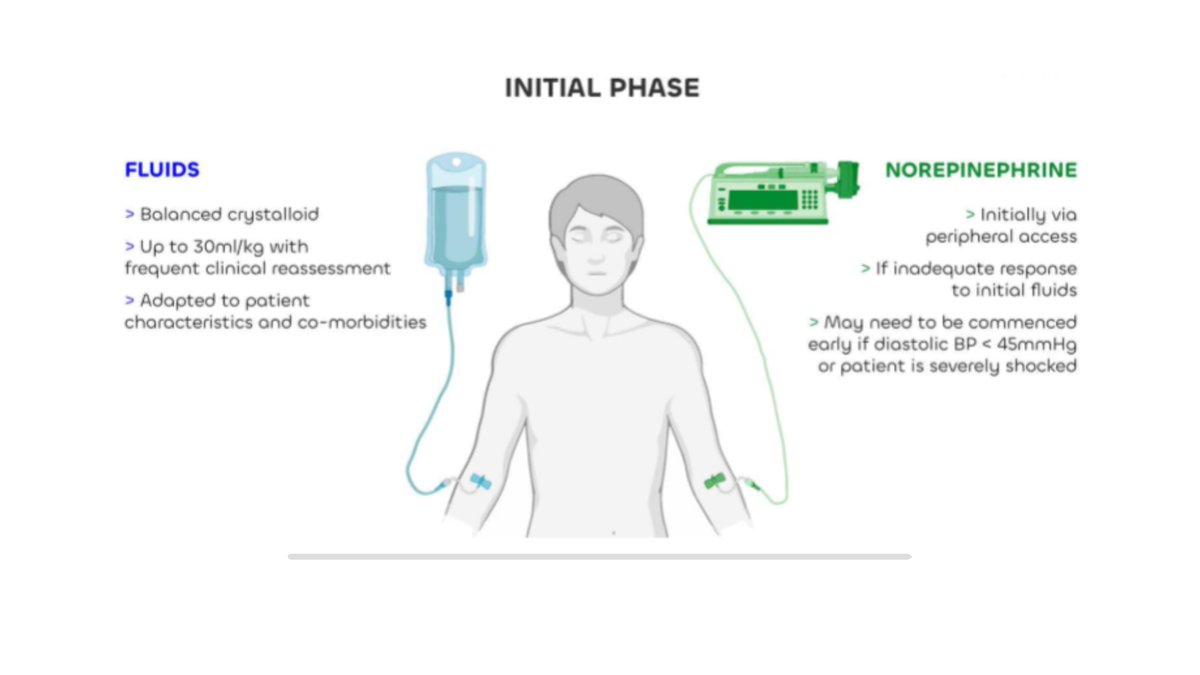
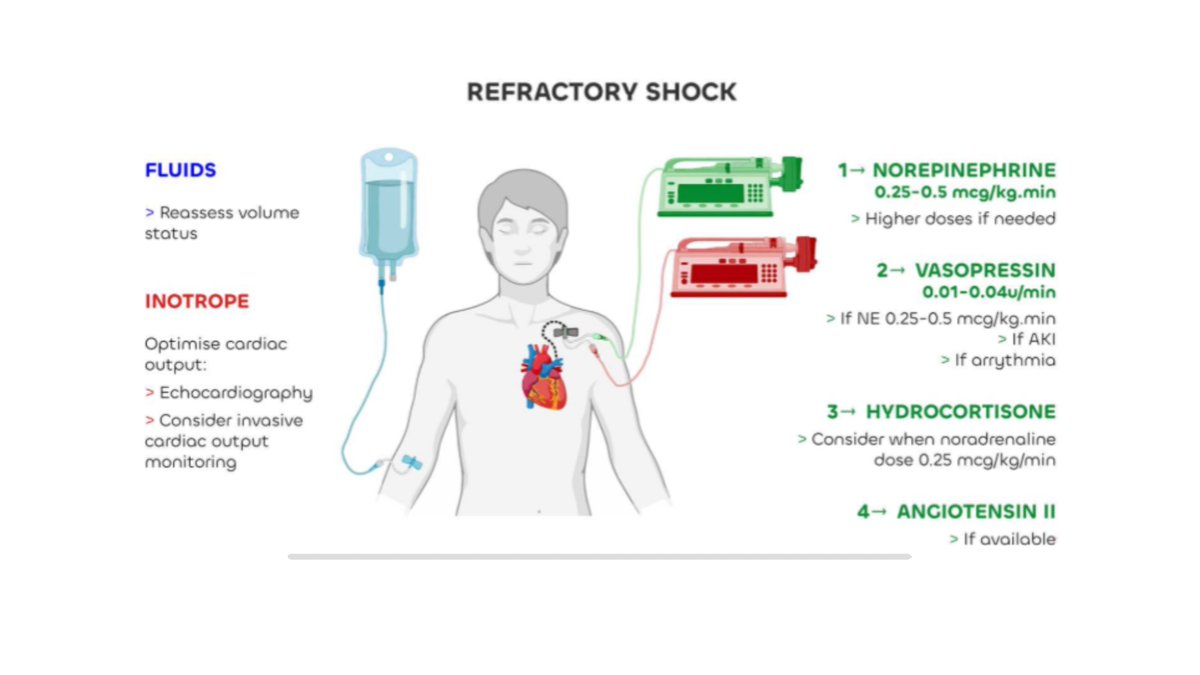
Multidisciplinary expert panel report on fluid stewardship: perspectives and practice
FULLTEXT link.springer.com/article/10.118…
#FOAMcc #FOAMed
@AzOudenaarde @Medaman_AtoQ

English
Manu Malbrain
13.7K posts


@Manu_Malbrain
Internist-intensivist, Professor Critical Care Research @OfLublin, views are my own, @Fluid_Academy, #IFAD2025 #FOAMed #Healthcare #Leadership









Thank you to SCCM's 2025-2026 Council, and welcome to the incoming 2026-2027 Council! Your hard work and dedication on behalf of the Society and its mission are greatly appreciated! #SCCM2026 #SCCM