Ollie Poole MD
600 posts

Ollie Poole MD
@RespReview
Anesthesiologist. MD. FRCPC. RRT. Cardiac Anesthesia fellow @ Peter Monk UHN















Strong start to anesthesia resident presentations @RespReview #POCUS can’t wait for the educational videos!! #ANESRD2023 @Ropivacaine






1/16 🤔Why does subarachnoid hemorrhage lead to deep/inverted "cerebral T-waves"? This ECG finding is so dramatic. But as we will see, these patients often have normal hearts. Why does an issue in the brain manifest on a test of the heart?


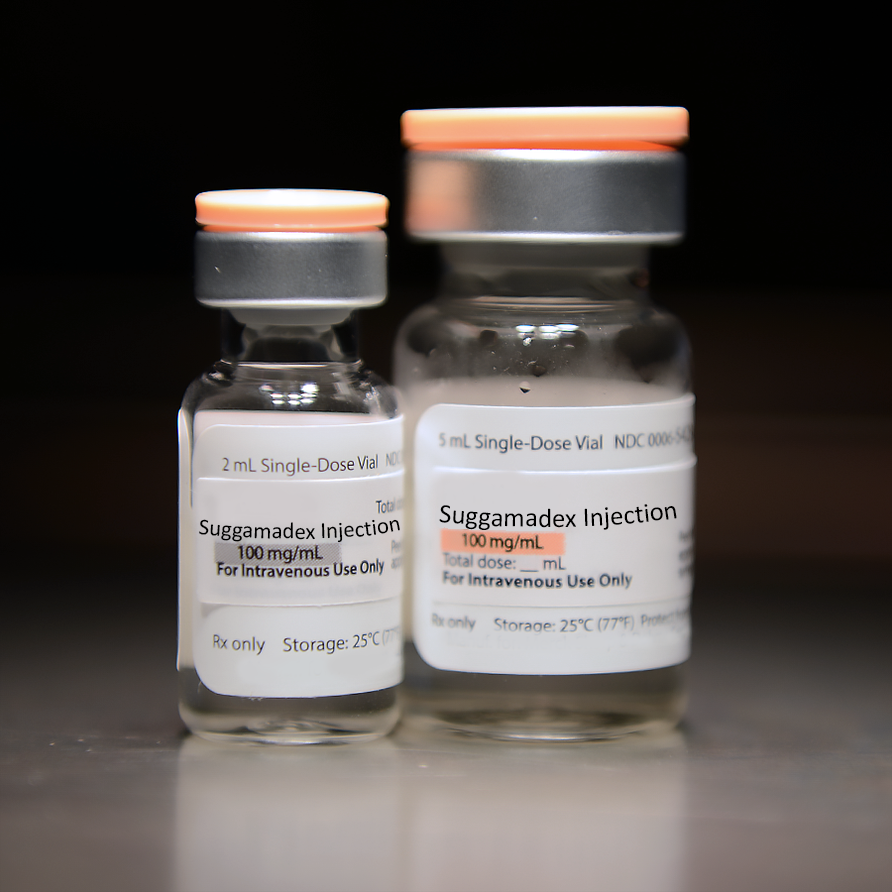
In a multicenter matched cohort analysis, sugammadex administration was associated with a 30% reduced risk of pulmonary complications, a 47% reduced risk of pneumonia, and a 55% reduced risk of respiratory failure compared to neostigmine. ow.ly/ocec50KbQb3





In a multicenter matched cohort analysis, sugammadex administration was associated with a 30% reduced risk of pulmonary complications, a 47% reduced risk of pneumonia, and a 55% reduced risk of respiratory failure compared to neostigmine. ow.ly/ocec50KbQb3