Marianne Chapleau
1.3K posts


Marianne Chapleau
@M_Chapleau
Neuropsychologist turned Medical Science Liaison. Passionate about patient care & improving the dx and tx of neurodegenerative diseases. Views are my own.







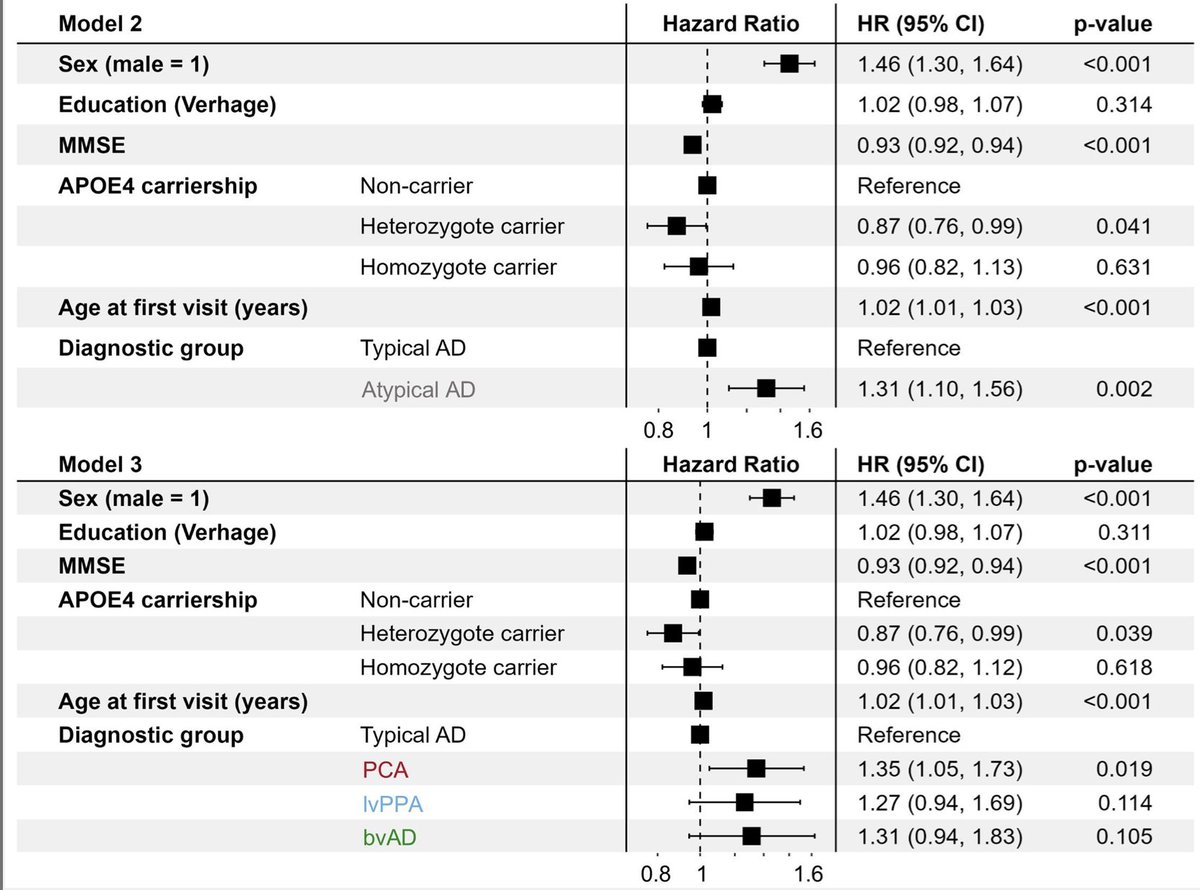





📢The CHMP recommends authorising a new treatment for early #AlzheimersDisease in the EU. Leqembi is intended for treatment of mild dementia and cognitive impairment in a restricted patient population with a specific genetic make-up. 👉 ema.europa.eu/en/news/leqemb…







Having started my career in basic neuroscience research, I have always understood Alzheimer disease to mean the pathophysiology associated with amyloid plaques and tau tangles. As a clinician, I appreciate that the relationship between Alzheimer disease and cognitive impairment is complex. 1. Clinically diagnosing the cause of cognitive impairment is different than diagnosing that the patient has Alzheimer disease (pathology). Many of my patients with cognitive impairment have multiple diagnoses (e.g., sleep apnea, medication-related cognitive dysfunction, depression, previous cerebral infarction), and sometimes have Alzheimer disease (based on biomarker testing). I do what I can to mitigate the effects of all of these conditions, and when Alzheimer disease is present I do not assume that it is the sole or even the primary cause of cognitive impairment. This is true across multiple potential etiologies: for example, I may diagnose someone with cerebrovascular disease and a prior infarct based on MRI findings, but determine that this condition is asymptomatic and not contributing to their cognitive impairment. 2. Given the simplicity of some biomarker tests and the difficulty of clinical assessment, there is a risk that clinicians may diagnose the etiology of cognitive impairment as Alzheimer disease without doing a full work-up. This is why appropriate use recommendations for biomarkers always mandate that biomarker results must be integrated with a clinical evaluation and not used as a “stand-alone.” 3. Alzheimer disease pathology accumulates silently for ~10-20 years before the onset of cognitive impairment. However, during this pre-clinical phase the accumulation of amyloid pathology is associated with many other biomarker changes that appear pathological (e.g., abnormal CSF synaptic biomarkers, brain atrophy, brain hypometabolism). While the brain is remarkably resilient to damage and individuals may or may not develop symptoms, the brain is sick and the pre-clinical phase is a disease state. 4. Suggesting that a disease only exists when organs are severely damaged and failing (dementia) seems counter to what we have learned in other areas of medicine. For example, patients diagnosed with hypertension or asymptomatic coronary artery disease may change their diet and medications to avoid a heart attack. Individuals with asymptomatic chronic kidney disease may or may not go on to require dialysis, but they can be monitored and sometimes treated. 5. There are valid concerns about the stigma and risks of asymptomatic individuals being labeled as having Alzheimer disease given that they may or may not develop cognitive impairment. The solution is simple—we don’t perform biomarker testing in asymptomatic individuals outside of research studies or clinical trials. Again, this has been mandated by appropriate use recommendations for biomarkers. We can help patients by promoting accurate understanding and appropriate use of biomarkers. #EndAlz



On doit améliorer l’accès et renforcer notre réseau public. C’est pourquoi on a l’intention de déposer un projet de loi qui ferait en sorte que les nouveaux médecins formés au Québec pratiqueraient dans le réseau public québécois durant les premières années après leurs études.






