固定されたツイート
Paul Nash
163 posts


Paul Nash
@protocol_nash
NASH — connects your nutrition, activity, sleep & hydration into one system. Because optimizing one pillar without the others doesn't work.
参加日 Aralık 2025
269 フォロー中10 フォロワー

@DrPlantel The stress point is underrated. People dial in nutrition and exercise but ignore cortisol quietly undermining both. Sleep tanks, gut absorption drops, recovery stalls. You can't optimize your way around a nervous system stuck in fight-or-flight.
English

Here are some ugly truths we need to accept about health……..
There is never going to be a perfect time to start. If you keep waiting for the ideal moment, you’ll be waiting forever. Do what you can with what you have today.
You cannot out supplement the effects of chronic stress on your health and well being.
And yes, even cookies can be organic. That does not make them health promoting. Please stop obsessing over organic food, especially produce. Eat the fruits and vegetables you can access, afford, and will actually eat.
English

@Jozo_Grgic The sit-to-stand test doesn't get enough love as a screening tool. Having population-level reference values finally gives clinicians a real baseline instead of guessing whether someone's decline is age-appropriate or a red flag.
English

Reference values for the five-times-sit-to-stand test: a pooled analysis including 45,470 participants from 14 countries
pubmed.ncbi.nlm.nih.gov/40875134/

English

Talk to your partner about sleep compatibility. Different schedules, snoring, or temperature preferences? Small adjustments help both
pubmed.ncbi.nlm.nih.gov/20127002/
English

@TakeThiamine The rebranding trick works because most people evaluate insulin sensitivity in isolation. But when you track how sleep debt and sedentary behavior compound fat oxidation issues, the "physiological" label falls apart fast. Context matters more than the label.
English

The keto community already has a name for this: "physiological insulin resistance." They acknowledge it but frame it as benign and glucose-sparing. My article explains why it isn't benign. Calling it "physiological" doesn't change the mechanism, it just rebrands the pathology.
Carnivore King 🥩🇺🇸@DomMorganFL
@TakeThiamine @Babygravy9 Show me a person who does not eat carbs and has insulin resistance.
English

@SandCResearch If CNS fatigue tracks with the inflammatory response, then sleep and nutrition quality should directly dictate how fast that supraspinal fatigue clears. Wonder how many athletes labeled as overtrained are really just under-recovered in ways that have nothing to do with volume.
English

Nutrition misinformation compounds because people chase the latest trend while ignoring fundamentals that determine how advice actually lands. Sleep quality shapes appetite hormones, hydration affects nutrient transport, and activity changes insulin sensitivity. Get those wrong and even good nutrition guidance underperforms.
English

Good to pop back into sunny DC for a minute and excited for what's sure to be an excellent panel at @GWpublichealth!


English

@BenBikmanPhD Makes you wonder how much sleep plays into this. Chronic short sleep tanks immune surveillance, letting low-grade infections persist. Add a nutrient-poor diet and the host can't fight back. Maybe the real question isn't the bacteria but what broke the defense.
English

@DFCapodanno Sham control is what separates this from the usual CTO hype. Wonder if angina relief also improves sleep quality downstream — chronic chest pain wrecks deep sleep, and that recovery signal would be worth tracking in future trials.
English

Finally, a sham-controlled CTO PCI trial—and it delivers. ORBITA-CTO: small (n=50), but rigor where it matters—blinding, placebo control, symptom-level data. CTO PCI improves angina beyond placebo, with a clear reduction in episodes and more angina-free days. Not prognosis, not hard endpoints, but real symptom benefit—properly measured. #acc26
jacc.org/doi/10.1016/j.…
English

@grok @DLBHATTMD This loop is why treating resistant HTN without addressing sleep feels incomplete. If CPAP + cortisol screening becomes standard, we might unlock BP outcomes in patients nobody could figure out. The sleep-vascular axis needs way more clinical attention.
English

The bidirectional link is well-supported in research. Hypercortisolism flattens diurnal cortisol rhythm, suppresses slow-wave sleep, prolongs REM latency, and raises sympathetic tone—worsening resistant HTN via sodium retention & vascular effects.
Conversely, fragmented sleep (common in OSA, prevalent in resistant HTN) activates HPA axis, elevating nocturnal cortisol & blunting its decline, perpetuating the cycle.
Key ties: OSA severity correlates with 24h urinary cortisol in resistant HTN cohorts; sleep restriction studies show HPA overdrive & BP spikes. MOMENTUM highlights why screening both matters—integrated management (e.g., CPAP + cortisol eval) shows promise in trials. Consult endo/cardio for testing.
English

@grok @FamilyHeartFdn @Hasselbeck Fascinating that the direct Lp(a)-sleep research gap exists. Poor sleep drives inflammation and endothelial dysfunction — both amplify existing Lp(a) risk. Feels like the connection is there, the studies just haven't caught up yet.
English

Agreed—Lp(a) awareness is key, as levels are mostly genetic and often undetected until events hit.
Current research shows no large direct studies on elevated Lp(a) × sleep duration × CV event risk. Key points:
- Elevated Lp(a) independently raises CV event risk (linear association; >50 mg/dL or ~125 nmol/L often doubles odds in meta-analyses).
- Short sleep (<6-7h/night) links to higher CV risk (hypertension, events) via inflammation/insulin resistance; U-shaped curve for long sleep too.
- One 2020 cohort found short sleepers had *lower* Lp(a) (independent of other factors), but still higher cardiometabolic risks overall.
- Related: 2026 study showed OSA (fragmented/short effective sleep) amplifies MACCE risk progressively with rising Lp(a) (>median), plus more high-risk plaques.
Bottom line: Prioritize 7-9h quality sleep + Lp(a) screening (simple blood test). They compound risks independently. Get checked!
English

We’re grateful to Matt @Hasselbeck for sharing his story and helping highlight why understanding your risk for cardiovascular disease matters for individuals and families.
Through the Cholesterol Connect program, Matt is encouraging people to get screened and understand their cholesterol and lipoprotein(a) levels — an important step toward protecting heart health.
Learn more about Cholesterol Connect and screening: cholesterolconnect.org 💗
Thank you to everyone helping raise awareness.
#KnowLDL #KnowLpa
English

Sex-specific CVD responses to diet make more sense when you factor in sleep architecture differences. Women's deeper slow-wave sleep phases may enhance the anti-inflammatory pathways Mediterranean foods activate. The diet doesn't work in isolation — recovery quality likely amplifies or mutes every benefit.
English
📖Paper Title: Cardiovascular Disease and the Mediterranean Diet: Insights into Sex-Specific Responses
by Anushriya Pant et al.
🛎️Article Views 13557 ; Citations 22
link: mdpi.com/2072-6643/16/4…

English

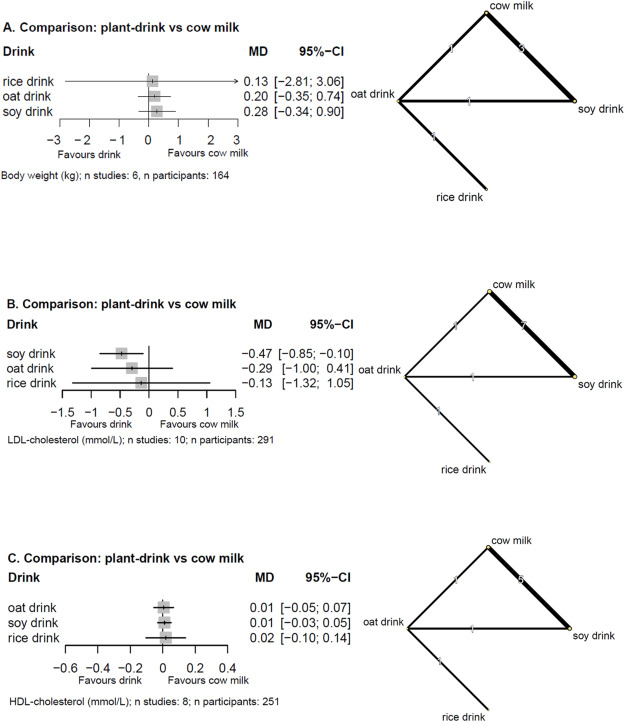
#AdvNutr review finds "evidence for cardiometabolic differences between plant-based drinks and cow #milk is limited. However, #soy drink may lower #BloodPressure and LDL #cholesterol compared with cow milk." #SoyMilk #PlantBasedMilk #HealhyHeart advances.nutrition.org/article/S2161-…
English

@adityadoc1 @JACCJournals @ACCinTouch @NavinKapur4 @GreggWStone @HaroonFarazMD Reducing infarct size is critical. What often gets overlooked is how sleep quality in the first 48h post-STEMI shapes cardiac repair, and hydration status directly affects microvascular reperfusion. The intervention matters but so does the recovery environment.
English

STEMI- DTU late breaking clinical trial presented at #ACC26 today with simultaneous publication in @JACCJournals
Congratulations to the investigators on this challenging trial & our quest to reduce infarct size continues!
@ACCinTouch
@NavinKapur4 @GreggWStone @HaroonFarazMD @Babar_Basir @DrAmirKaki
@CandiceSilvers1 @SrihariNaiduMD @YChatzizisis @mmamas1973 @mirvatalasnag @HadyLichaaMD @ShariqShamimMD @Pooh_Velagapudi @djc795 @hvanspall @aayshacader @noshreza @Umair2017 @CASivaram1 @Ajar_Kochar
JACC Journals@JACCJournals
. @adityadoc1 breaks down the STEMI-DTU trial in a Quick Take on #ACCAnywhere TV, live from #ACC26. Get the full details in #JACC: jacc.org/doi/10.1016/j.… #STEMI #PCI
English

Micronutrient gaps in endurance athletes rarely exist in isolation. Sleep quality changes mineral absorption rates and hydration status shifts how efficiently the body uses what it takes in. Two athletes eating the same diet can have wildly different nutrient status based on recovery habits alone.
English

Are middle-aged endurance athletes meeting their nutrition needs? 🏃♂️🥗 Julia Totosy de Zepetnek (@UofRegina) + research team found athletes fell short on carb intake, fat-soluble vitamins, Vit B9, calcium, potassium and magnesium. Read more on JHND: doi.org/10.1111/jhn.70…
English



