고정된 트윗
Bryan Glezerson
8.4K posts

Bryan Glezerson
@BryanGlezerson
Neuro-anaesthesiologist, certified diagnostic EEGer @TheNeuro_MNI. Int: technical standards/generalizability in anaesthetic EEG. TIVAdiva. Periop Neuro. Oudie.
Montréal, Québec 가입일 Nisan 2011
1.7K 팔로잉1.8K 팔로워

@Chronotrope @Leedsmedic @charlottetr @BJAJournals @MichiIntrona If you take the propofol low enough I find you can usually reconstitute a nice alpha band in most people. Exception, of course, is the elderly/frail, and for some reason in patients with severe Parkinson’s Dementia, almost independent of age.
English

@Leedsmedic @charlottetr @BJAJournals @MichiIntrona Must say I don’t really understand the “high remi” thing. Why is it continued after pinning? Produces a grotty EEG!
English

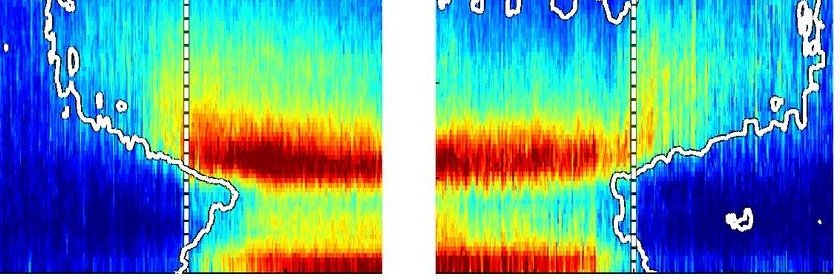
Anaesthetists could benefit from routinely assessing the raw EEG and its spectrogram, rather than relying solely on an index produced by a depth of anaesthesia monitor.
New editorial by McCulloch et al #anaesthesia #anesthesia #perioperative
bjanaesthesia.org/article/S0007-…

English

Anaesthesia is not a vascular access service and you cannot get good at “difficult” cannulas by not doing them.
Also, paediatricians and oncologists are very good at cannulation: call them instead #tipsfornewdocs
Finally, do not do this:

English

Lemme show you how to do mask anesthesia while charting on paper by holding the clipboard to the OR table with my hips.
Dr. Glaucomflecken@DGlaucomflecken
English

@wongdiagnosis @glbryson And to location in the permanent record as well as to research.
English

@BryanGlezerson @glbryson I call that resilient against IT outages and hacking
English

@beckimarshRA Oh I think if you’re doing a TEA then adding IT morphine may do little. But as an alternative to an epidural, it certainly has a measurable effect on postoperative pain.
I suspect it is sadly not only in the NHS that compromises must be made in anaesthetic choices.
English

@DrRobbieErskine @derekedsmith @milliken_don @colinjmccartney @EMARIANOMD That seems to be my observation as well.
English

@BryanGlezerson @derekedsmith @milliken_don @colinjmccartney @EMARIANOMD This is so true.
Women after LSCS just get on with it (wife’s experience x3) and Side effects become lost in the focus on caring for the litt’n
English

Does anybody else get the sense that outside of OB and pediatric spines, intrathecal hydrophilic opioids are grossly underutilized?
@DrRobbieErskine @colinjmccartney @EMARIANOMD
English

@DrRobbieErskine @glauncel @colinjmccartney @EMARIANOMD I think I would as well. But what sparked this post was that I found myself with a particularly intransigent and unobliging surgeon who refuses that her patients receive high quality regional analgesia. So I adapted and did the next best thing; was quite pleased with the result!
English

@glauncel @BryanGlezerson @colinjmccartney @EMARIANOMD I would choose paravertebral, TEA, abdo wall RA over IT opioids for supraumbilical/fmlanl/thoracics
English

@derekedsmith @milliken_don @DrRobbieErskine @colinjmccartney @EMARIANOMD I think expectations may also be different between parturients and other laparotomised patients.
English

@BryanGlezerson @milliken_don @DrRobbieErskine @colinjmccartney @EMARIANOMD I’m always conflicted based on some of the literature that shows doses 200-300mcg+ to show benefit, when in CS I never go above 150mcg as the evidence for doing so is poor as risk of pruritis increases with marginal to no benefit in terms of analgesia.
English

@milliken_don @DrRobbieErskine @colinjmccartney @EMARIANOMD It is indeed. No doubt in the short term they are more comfortable, though!
English

@glauncel @DrRobbieErskine @colinjmccartney @EMARIANOMD Seems you can get around 20mg of spared parenteral morphine in 24h with <500mcg IT morphine.
I have been impressed recently by its efficacy at low doses.
English

@BryanGlezerson @DrRobbieErskine @colinjmccartney @EMARIANOMD Monitoring when additional opioids are required may also be an issue. Upper abdominal, flank or thoracic incisions may require more IT opioid to be effective.
English

@milliken_don @DrRobbieErskine @colinjmccartney @EMARIANOMD The best literature on IT morphine is all alongside at least foundational analgesia, so that’s what I did.
I am also quite heavy handed with steroids. I have been sadly underwhelmed by the literature in support of ketamine/dexmedetomidine/lidocaine on pain outcomes after PACU.
English

@BryanGlezerson @DrRobbieErskine @colinjmccartney @EMARIANOMD That's not an uncommon experience. Diamorphine is available to us and I do use it, but for major open surgery my anecdotal experience is that morphine lasts longer. I favour a lido/ket/clonidine/mag/tylenol/decadron multimodal IV approach alongside it.
English

@glauncel @DrRobbieErskine @colinjmccartney @EMARIANOMD And yet IT a morphine 100-200mcg is universally provided for cesarean under spinal.
Literature suggests that doses under 500mcg have similar rates of PONV and respiratory depression to PCA alone. Itchiness is the only noteworthy side effect.
pubmed.ncbi.nlm.nih.gov/32660719/
English

@BryanGlezerson @DrRobbieErskine @colinjmccartney @EMARIANOMD Unpleasant side effects limit their use.
English

@milliken_don @DrRobbieErskine @colinjmccartney @EMARIANOMD Which of course is made all the more shocking because it is UNIVERSAL in cesarean delivery in North America to use IT morphine. So one wonders why this is not more standard in other laparotomies.
English

@milliken_don @DrRobbieErskine @colinjmccartney @EMARIANOMD So it’s interesting, Don. I think that Canadian adult anaesthetists have forgotten about this.
But I worked at a different hospital than I normally do this week and one of the gynae-oncologists refuses epidurals. So I did spinal morphine 200mcg and for 48h the patient is 0/10.
English