Sabitlenmiş Tweet

Mechanical ventilation doesn’t have to be confusing.
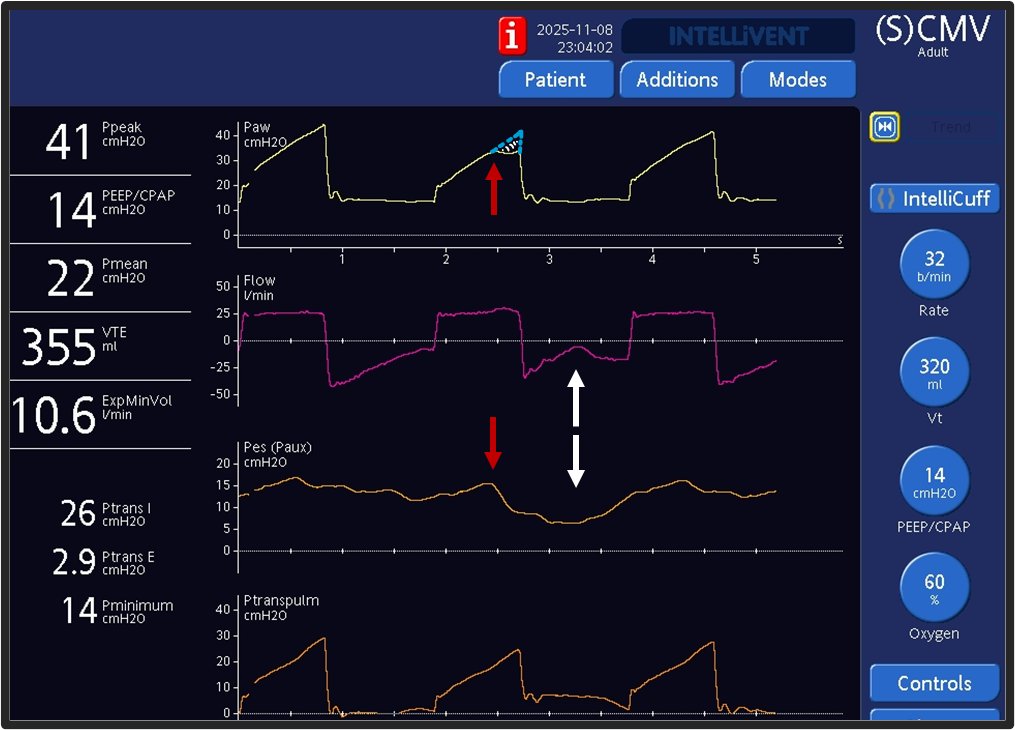
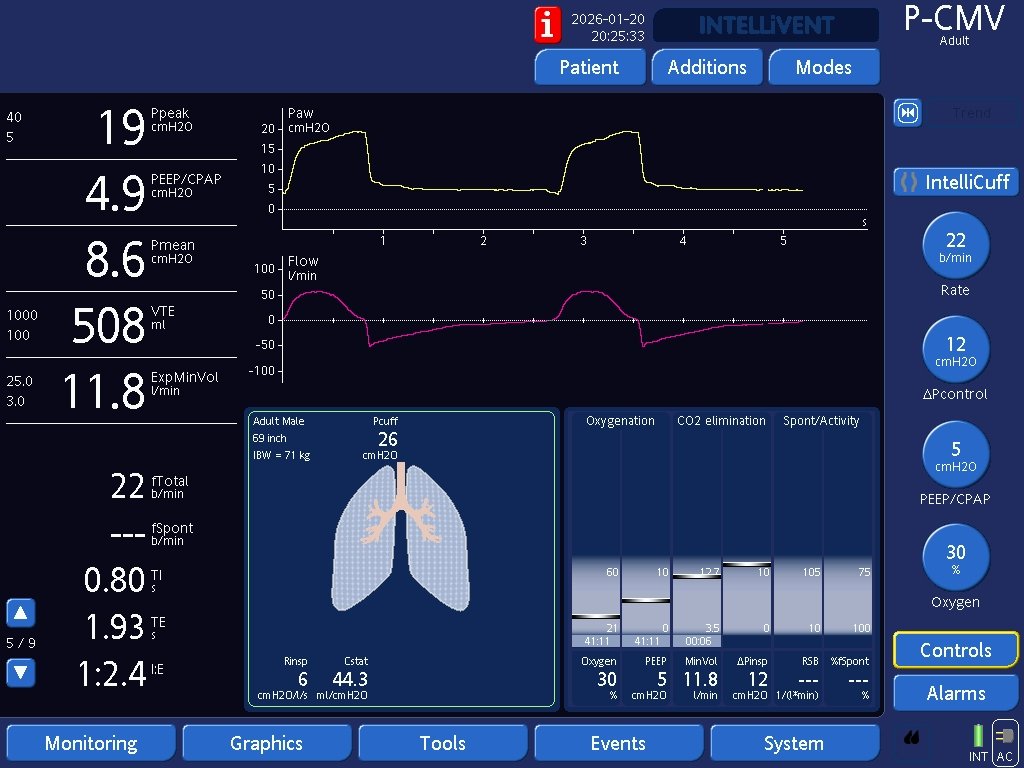
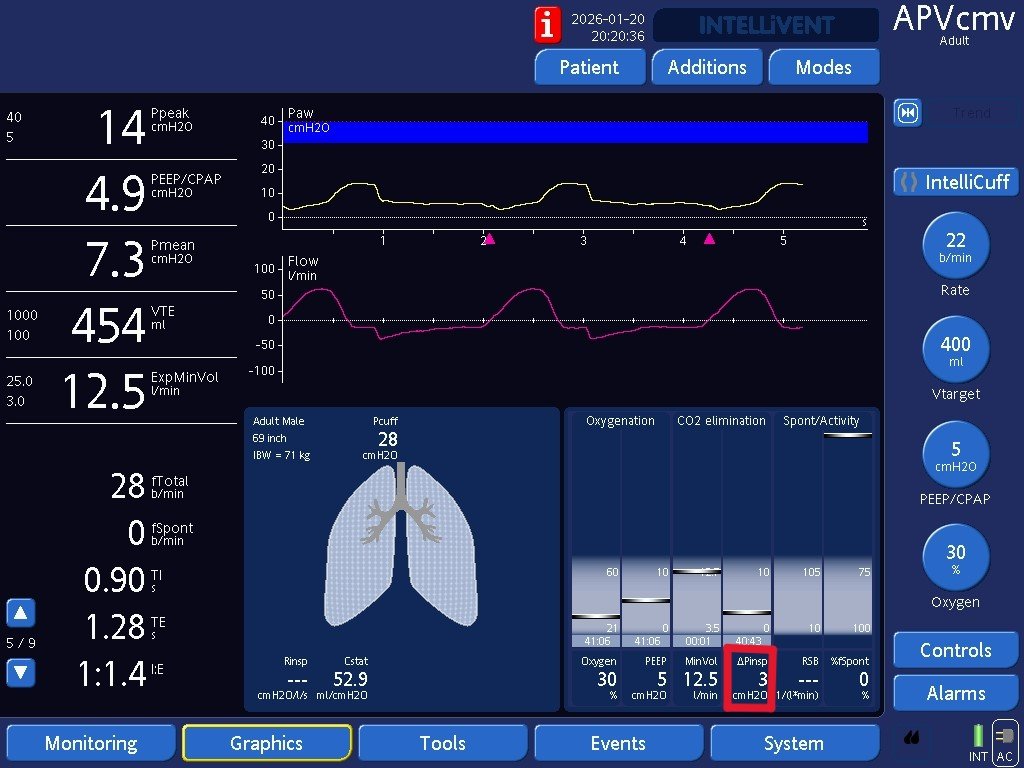
I teach a FREE structured course using real ventilator images —from fundamentals to advanced management.
🫁 For Critical Care fellows, motivated residents & RTs
🎥43 concise lessons (5–10 min each)
📚Practical, high-yield, clinically focused
Build a deeper understanding. Manage ventilators with confidence.
Access the course for FREE:
forms.office.com/r/GNhq7GxPbR
English