Alhassan Al Mostaneer
3.5K posts


Alhassan Al Mostaneer
@HSHM20
طبيب زمالة المخ والأعصاب | كليفلاند | الولايات المتحدة 🇸🇦 🇺🇸Neurology resident | UH Cleveland Medical Center @cwruneuro @UHhospitals #VascularNeurology










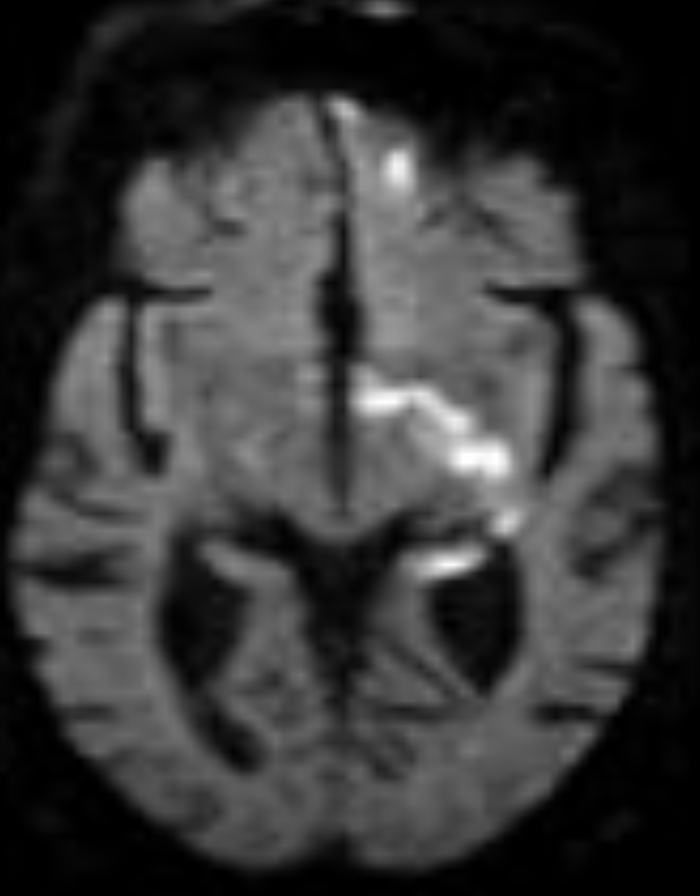


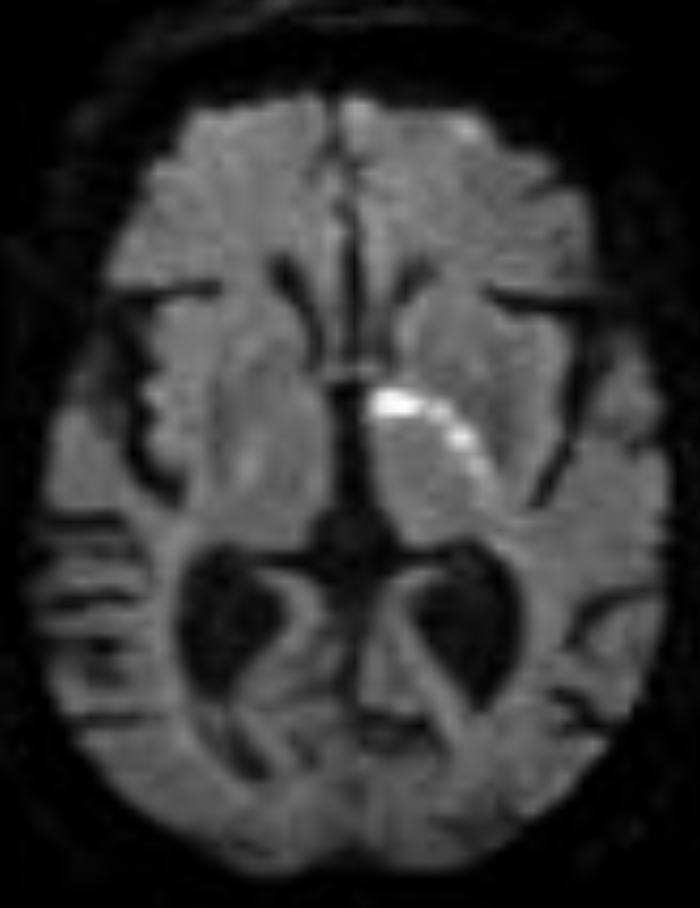
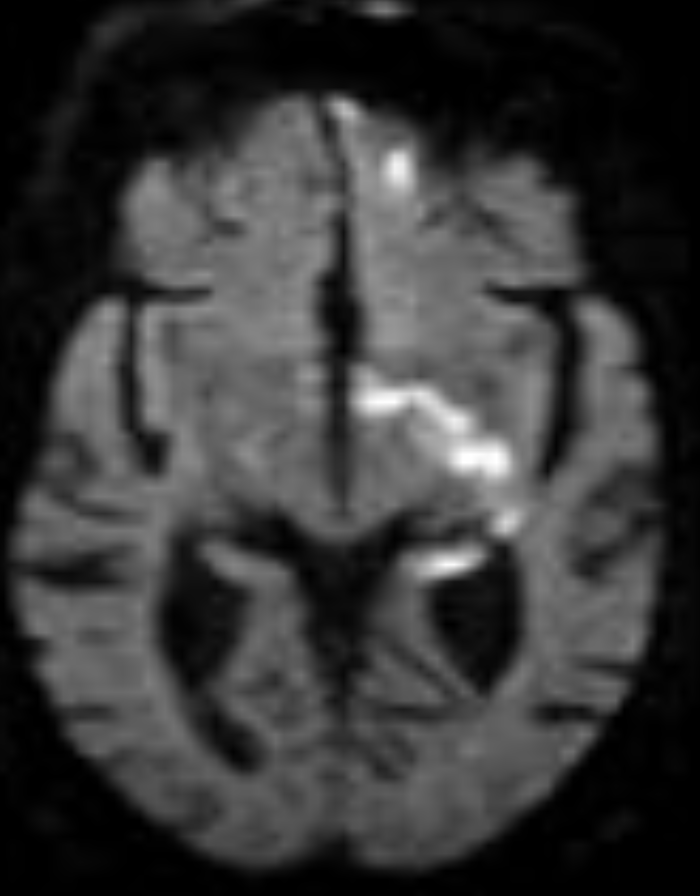
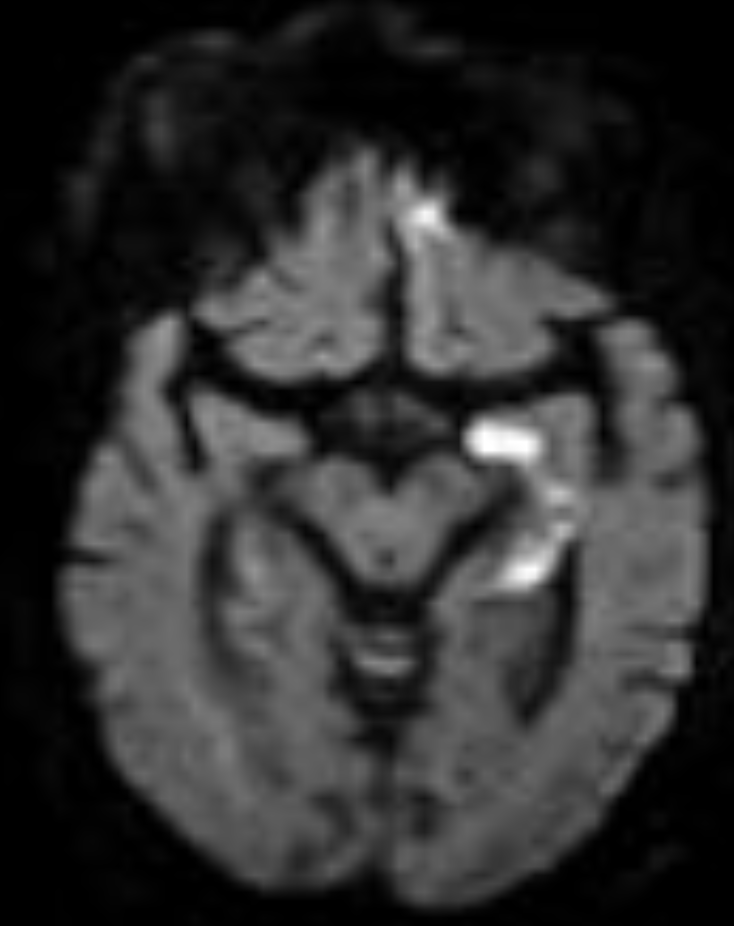
I'm sorry, it looks like the first image didn’t load. Here’s a clean lateral DSA of the internal carotid artery (ICA) to walk through the supraclinoid branches with the text below. 👇👇 Small branches. Massive consequences. Before the internal carotid artery (ICA) bifurcates, let’s walk through the key supraclinoid branches on this lateral DSA. Anchor yourself here. Follow along. The internal carotid artery supplies the anterior and superior brain. The vertebral and basilar system supply the posterior and inferior brain. This is a lateral diagnostic cerebral angiogram of the ICA. Remember: DSA subtracts tissue and only opacifies vessels. You are looking at the complete filling of the internal carotid artery. Left of your screen = anterior brain. Right of your screen = posterior brain. Now pay attention to the arrows. Just beneath the arrows, where the artery curves anteriorly, is the carotid siphon. This segment runs through the cavernous sinus. It is called the cavernous segment of the ICA. The ICA then pierces the dura mater superiorly at the level of the anterior clinoid process and enters the intradural space. That is why this segment is called the supraclinoid ICA. Get it? The first major branch after it enters intradural space is the ophthalmic artery (green arrow). This artery runs anteriorly. Why does this matter? A clot from a carotid plaque can embolize into the ophthalmic artery, then into the central retinal artery → sudden, painless monocular vision loss. Another major branch, labeled purple, is the posterior communicating artery (PComm). This vessel is part of the circle of Willis. It connects the ICA to the posterior circulation by joining the posterior cerebral artery. Now look closely. Running parallel to the PComm is a much smaller vessel, the anterior choroidal artery (red arrow). It is small. But an occlusion here can mimic a large vessel stroke. Why? Drop your thoughts below. 👇👇 #Neurology #NeuroTwitter #Stroke #DSA #Neuroanatomy #FOAMed Image source: Guzmán Pérez-Carrillo & Hogg. Curr Probl Diagn Radiol. 2010.