J Peace 3
7K posts

J Peace 3
@JPeaceJPeace
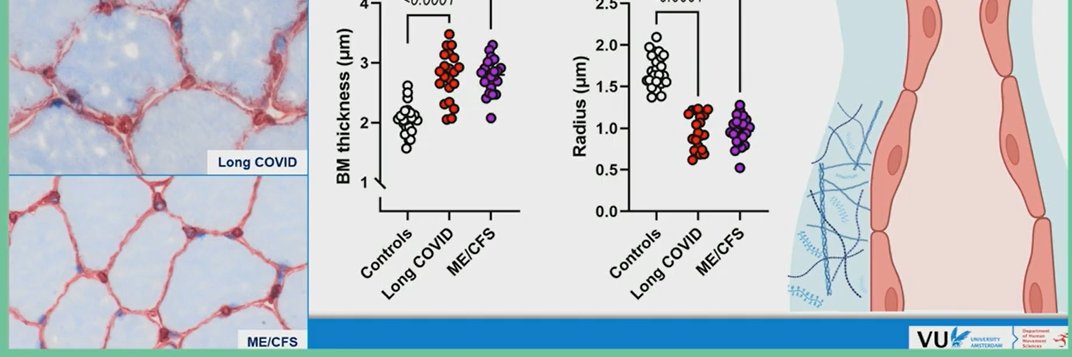
Long Covid is predominantly a disease of the function and structure of the microvasculature.










A new preprint from our @DerbyUni x @StellenboschUni Long COVID research team has now been published. Findings suggest that exercise may worsen symptoms in Long COVID due to microclot fragmentation. [link to preprint]: researchsquare.com/article/rs-671…


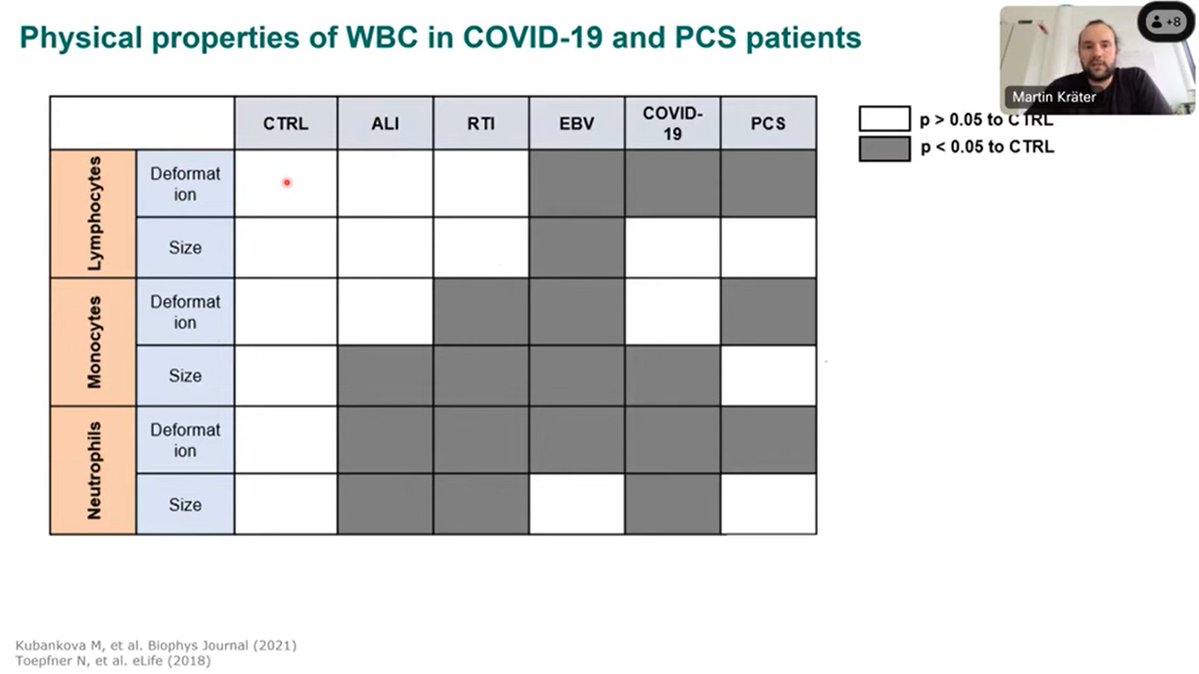
LC PATIENTS BANNED FROM BLOOD DONATION Rearchers have shown the mechanical properties blood cells change in patients with long covid. But yet the usual blood tests do not look for these changes to determine if someone has LC. We need better tests! youtube.com/watch?v=Eds4MQ…




Latest paper from @CallumThomas96 and our research group showing a reduction in oxygen extraction in the calf muslces during low intensity exercise/activity. This has important implications for energy production and functional status... physoc.onlinelibrary.wiley.com/doi/10.14814/p… #longcovid



The moment I said the word “Covid,” the primary care appointment was already over. Not in any professional sense or in any way I had ever experienced before. I watched it unfold right in front of me. This is the story of the most blatant gaslighting by a medical professional I experienced during my Long Covid journey. I was there because something had been very wrong since I had Covid. My blood pressure was suddenly high. My resting heart rate wouldn’t come down. I was dizzy, getting constant headaches, chronic fatigue, blurred vision. None of it had ever been an issue before. I explained everything. Then I said the forbidden words. “Could this be from Long Covid?” He didn’t answer. Instead, he smiled. Not in a reassuring or curious manner. Something was off. He reached out, patted my shoulder, and told me to “calm down the chaos in my mind.” Then he said, almost hysterically, “So I was at the airport the other day….” “At the luggage carousel. A woman collapses. People start screaming. ‘Is there a doctor? We need CPR’…” I sat there frozen, mortified. “I go over to help,” he continues. “But I didn’t have to.” A pause. A sneering grin. “Because she CAME AROUND again!” He leans in slightly, “On the CAROUSEL!” Then he laughs and turns to his computer, already typing up my visit summary. Just like that, the appointment shifts into something unreal. No acknowledgment of anything I said. Just a joke. A deflection within a small performance so he could avoid the conversation entirely. I could hear the final clicks of the keyboard. As quickly as he had entered, he was gone. I was still sitting there with a racing heart, the dizziness creeping back in, trying to process what had just happened. Because I understood it then clearly. He was done with me the second I said “Covid.” Everything after that was just his way of leaving without actually walking out. That was the most disturbing part: Realizing the person I went to for help had already decided not to hear me, and laughed his way out of the conversation and out the door.




