Lau Saugman
1.9K posts

















Pain on the outside of your hip is one of the most common problems I see in my practice. Walkers get it. Runners get it. People who've never been to a gym get it. For decades, we called it bursitis and injected it. We were treating the wrong thing.


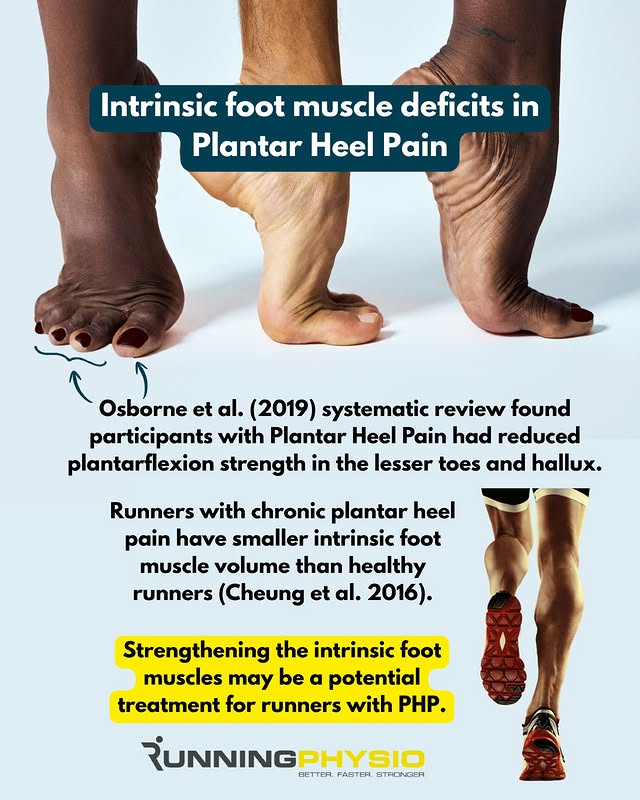
Correct diagnosis is the first step in effective management of plantar heel pain. In her “Assessment of Plantar Heel Pain” Practical, Dr Melinda Smith shows exactly how she evaluates plantar heel pain to guide differential diagnosis and treatment planning. You’ll learn how to: 📋 Ask the right questions ✅ Conduct a thorough physical exam 🔎 Perform foot-specific strength testing ...and much more! Don’t miss this opportunity to watch how an expert works through a complete assessment of plantar heel pain. Watch Melinda’s assessment process for free now 👇 physio-network.com/practicals/


Quick physio tip 👇 If someone falls into femoral IR, use a resistance band + cue them to press out slightly. Think: kneecaps = headlights 🚗 → keep them facing forward. Simple cue, huge impact on movement quality. #PhysioHack #PhysicalTherapy #RehabScience



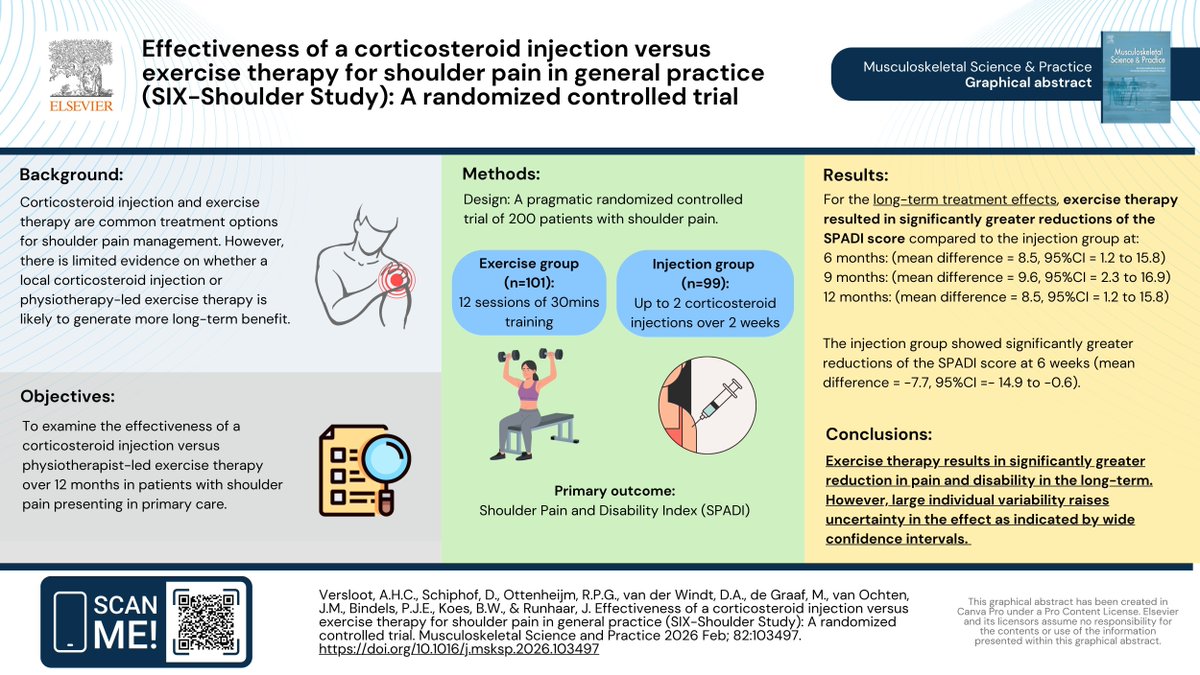
This systematic review concluded that there was “no difference in effectiveness of physiotherapy versus control interventions at short term, medium term, and long term.” Here’s 5️⃣ reasons why we shouldn’t be too worried 🧵