Alex Stebner MD retweetledi

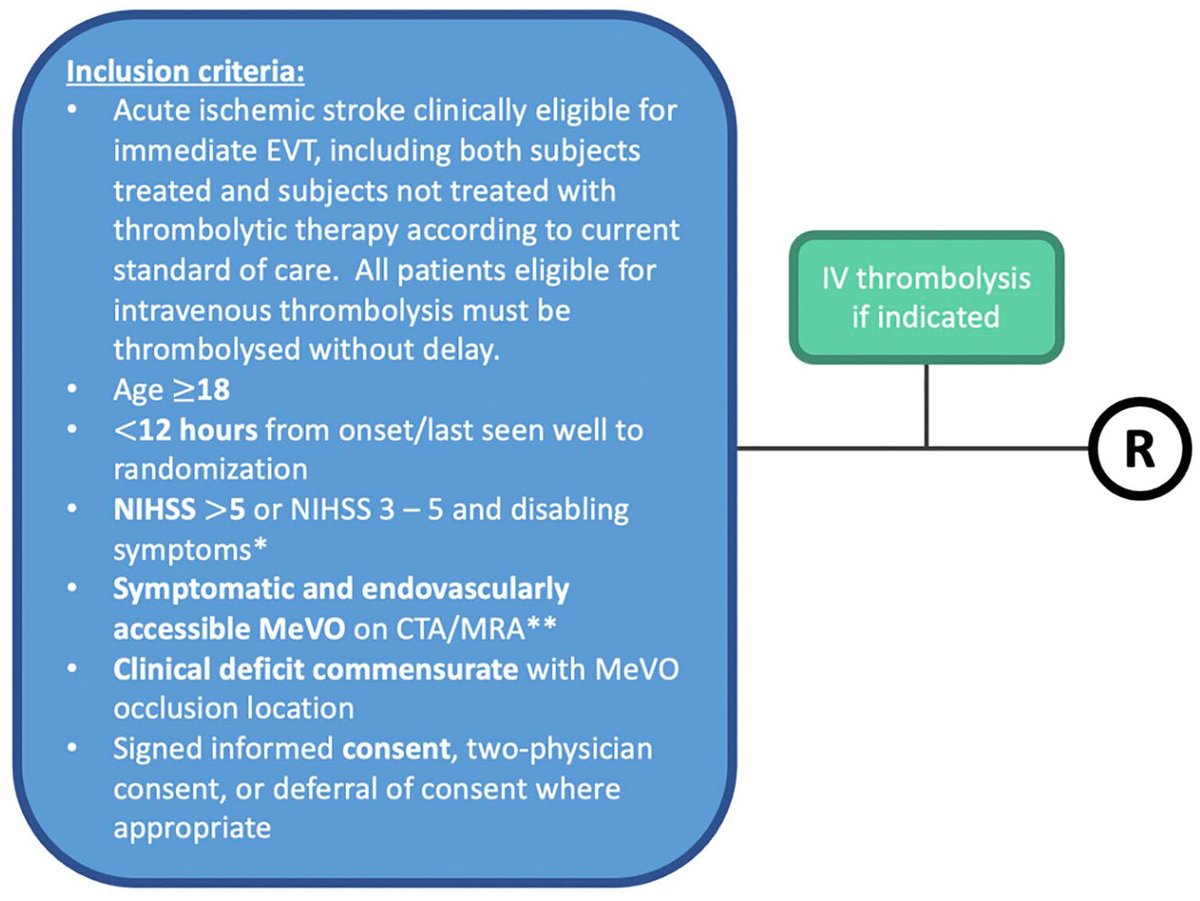
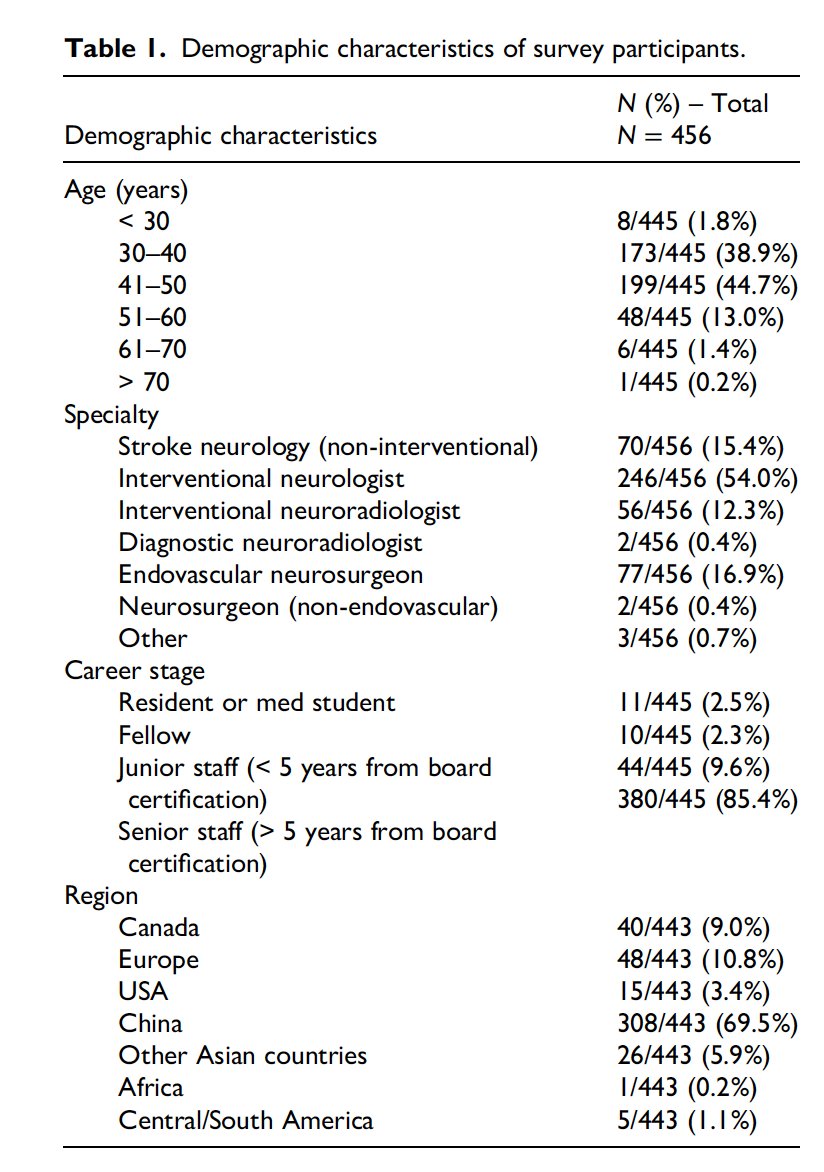
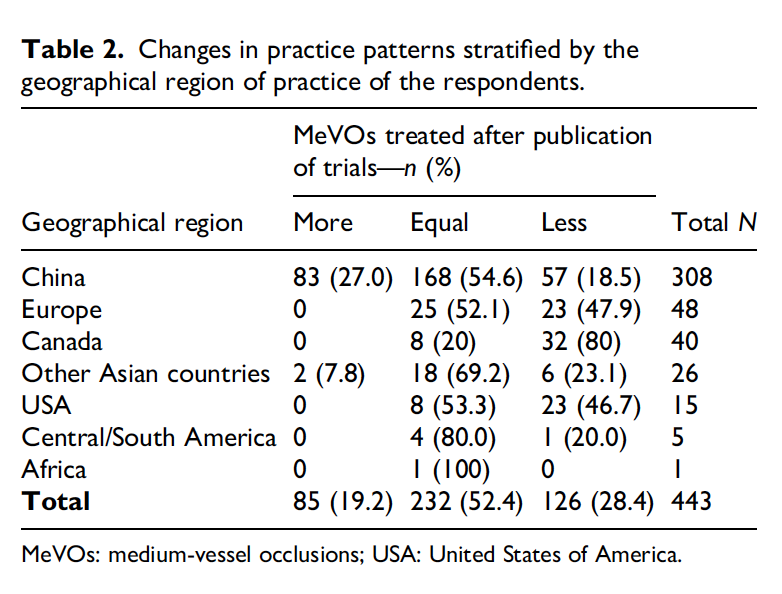
🤔How did the recent #MeVO #EVT trials change practice patterns worldwide??🏥🌎 Salome Bosshart, @MDStebnerAl and team will tell you in this paper!👀 journals.sagepub.com/doi/10.1177/15… @HotchkissBrain @DCNSNeuro @nishita_singh3 @draravindganesh

English