Michael Weisman
148 posts

Michael Weisman
@MWeismanMD
RadOnc. Thoughts are my own.


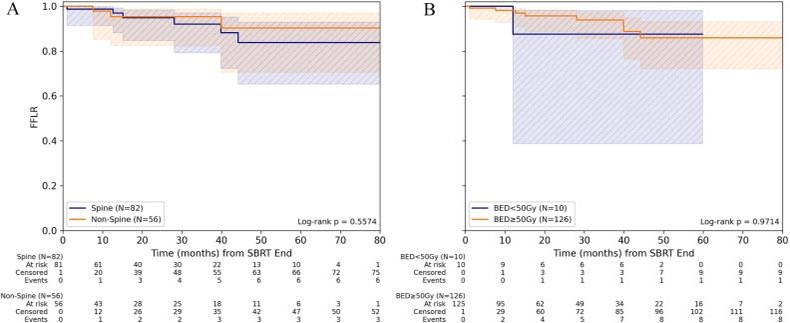
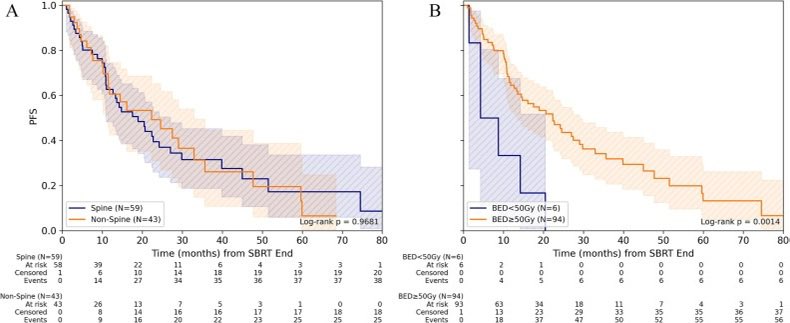
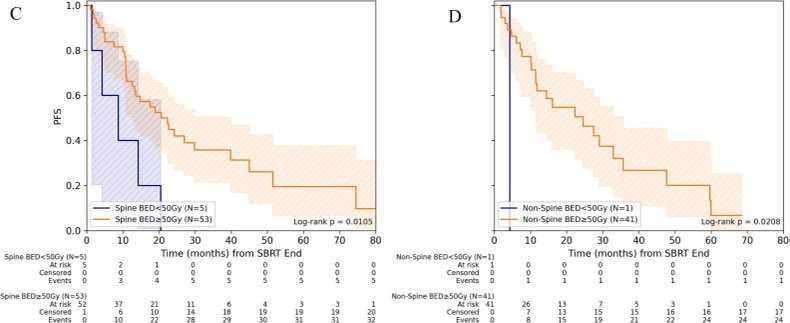





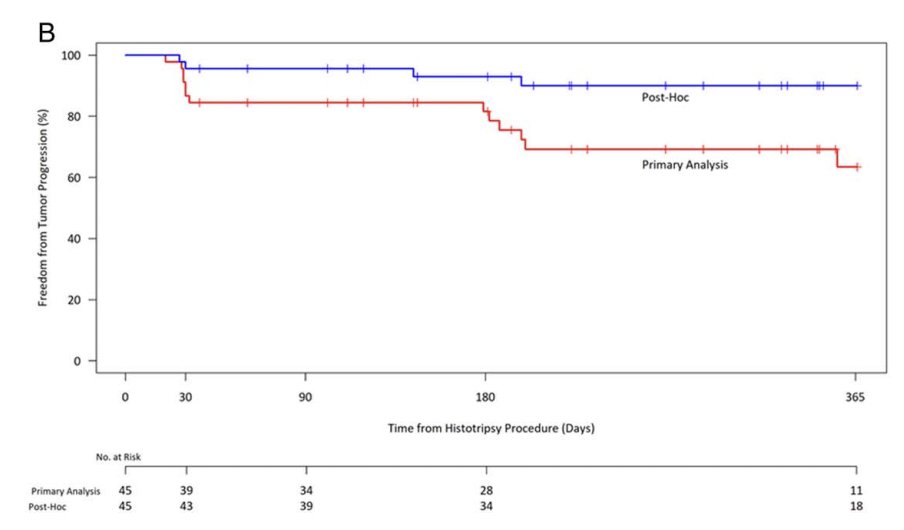
Hepatic histotripsy is a novel noninvasive ultrasound therapy for liver tumors, and 1-yr outcomes demonstrated that local tumor control and survival was consistent with other therapies. journals.lww.com/annalsofsurger…


NOTCH publication out now in @IJROBP ! 🧪 Involved neck only (INO) vs mucosal radiotherapy (MUC) for HNSCCUP INO RT for unilateral HNSCCUP offers similar 5-yr survival and disease control as MUC, and lower rates of enteral feeding Link: doi.org/10.1016/j.ijro…


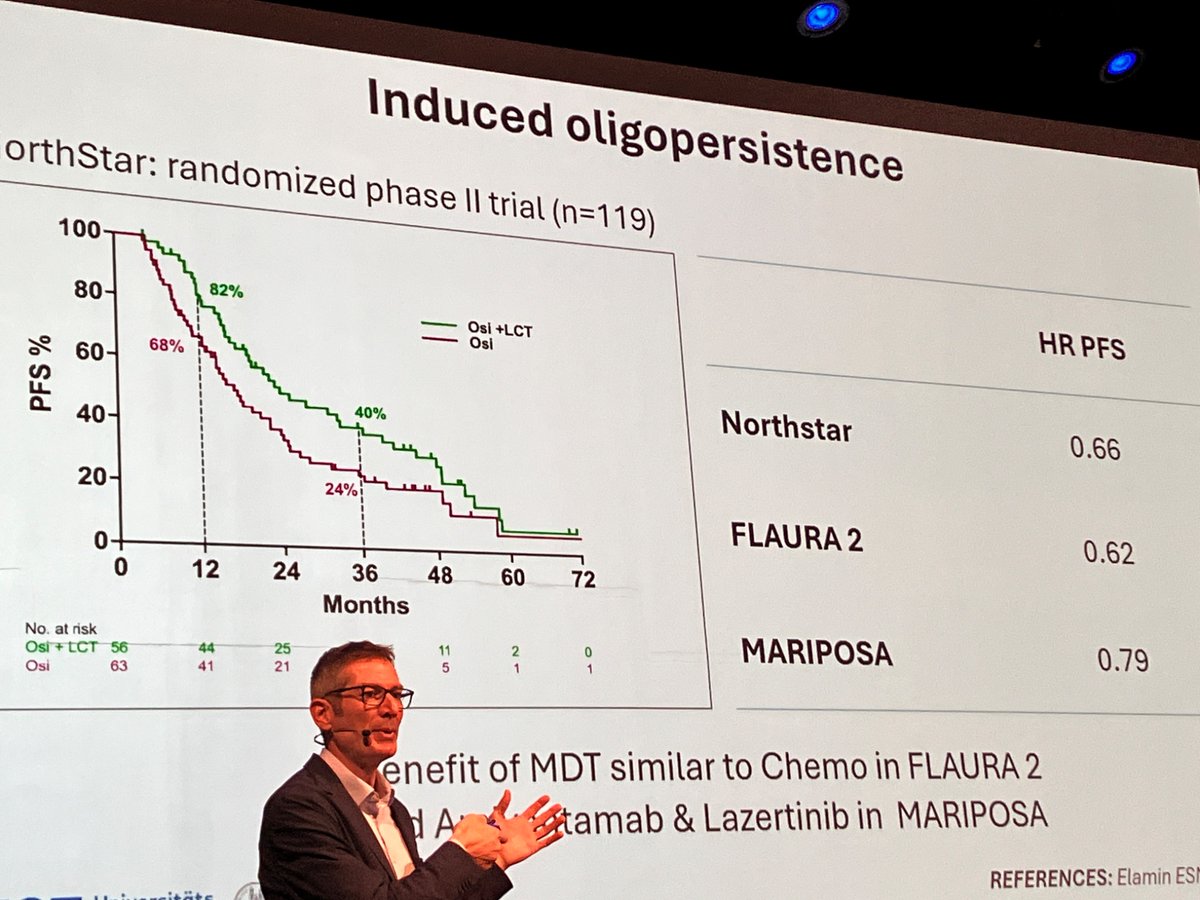

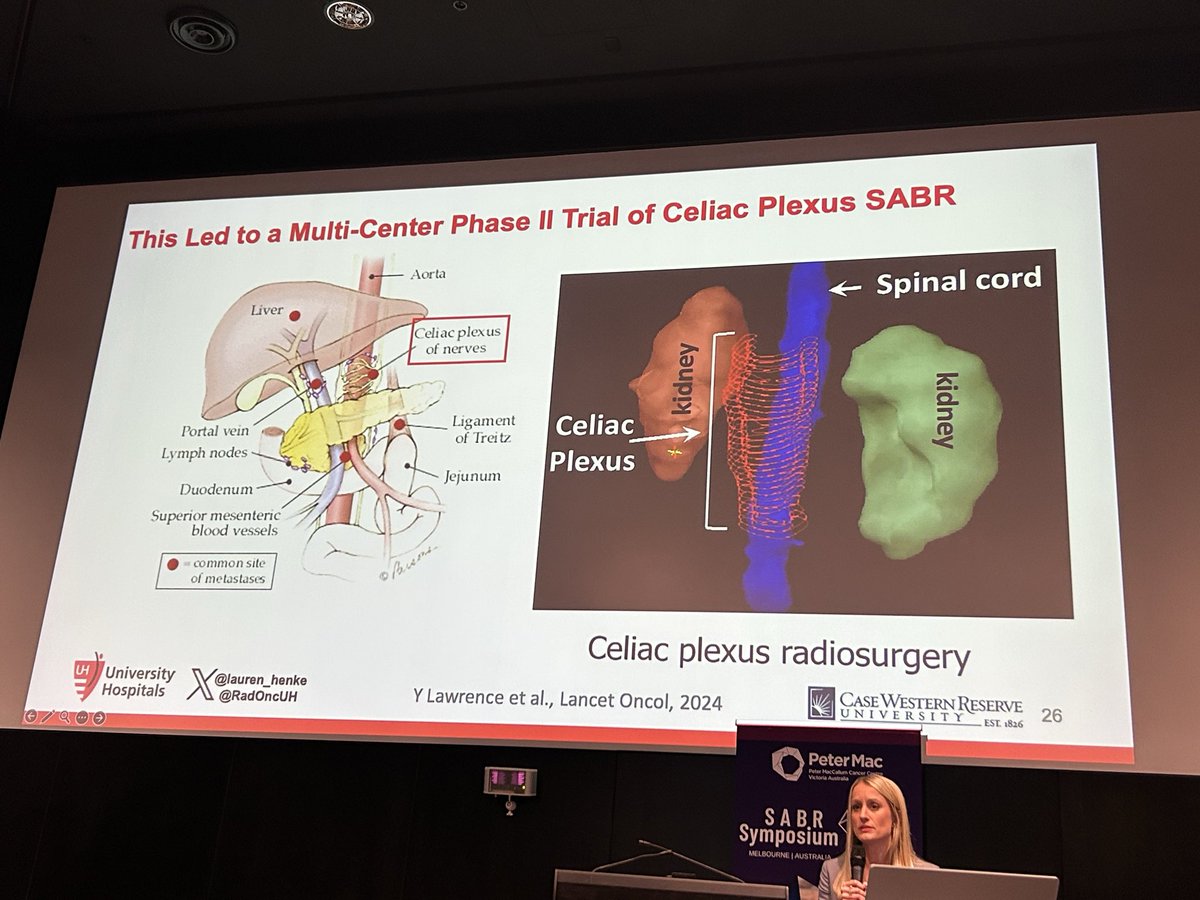

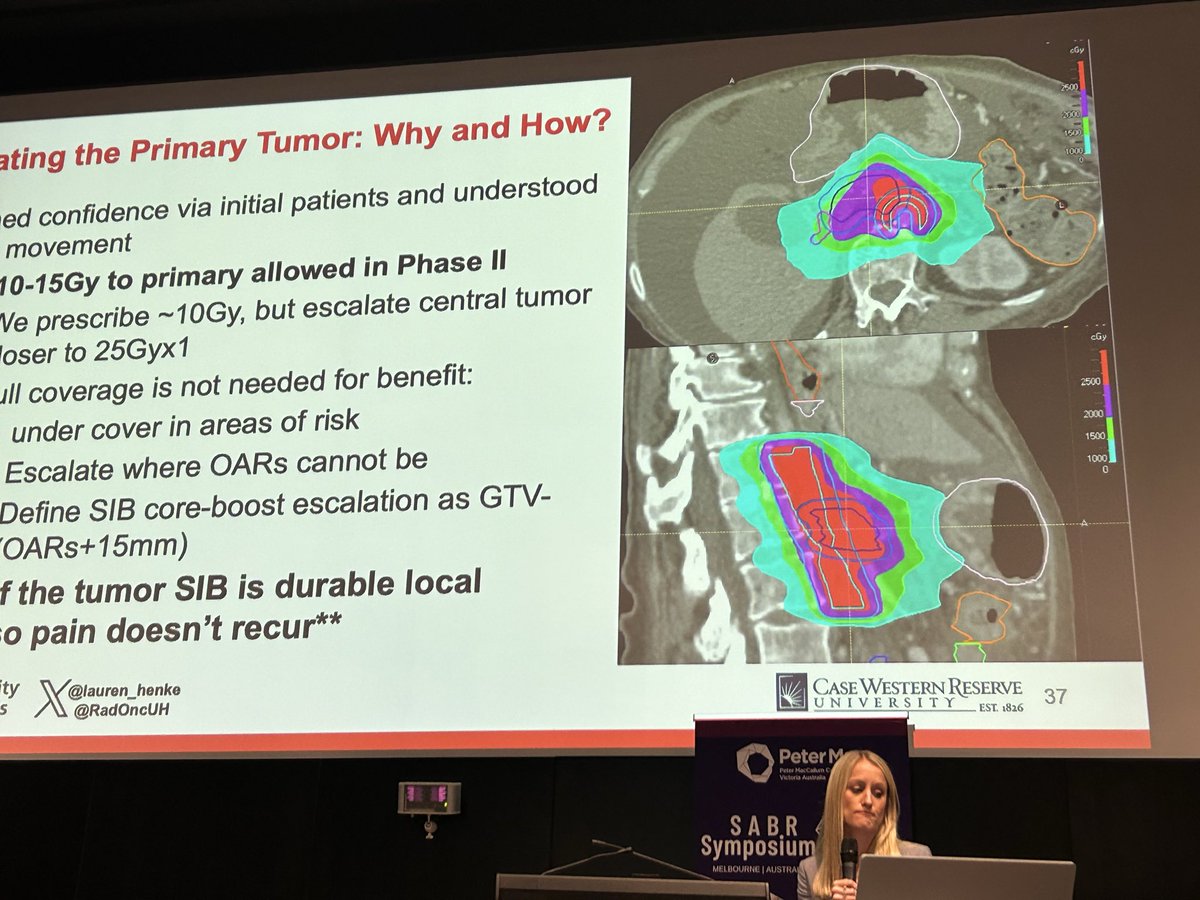






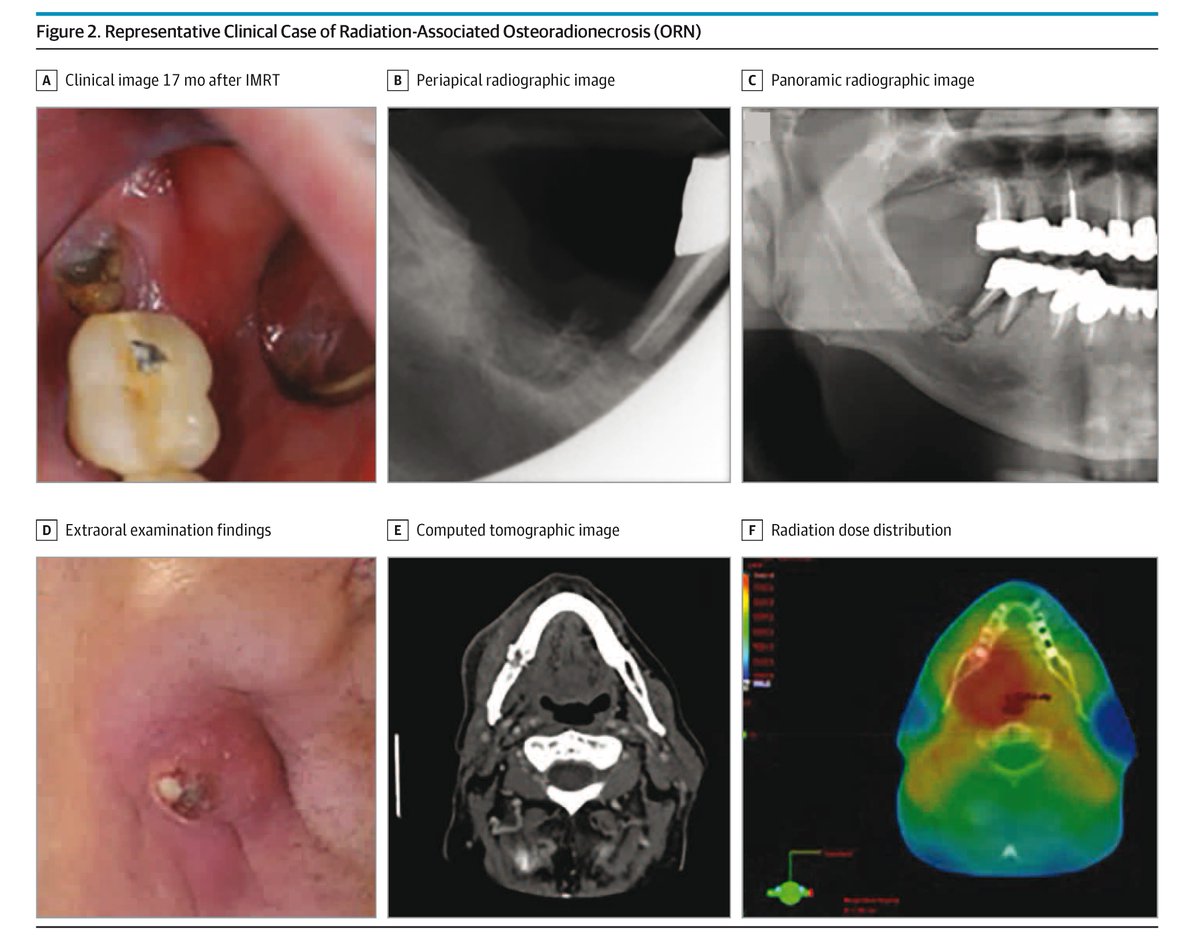
1/ Our latest - @JAMAOncology Viewpoint! Ablative radiotherapy has a dual effect on metastatic cancer that changes how we should interpret progression after treatment.


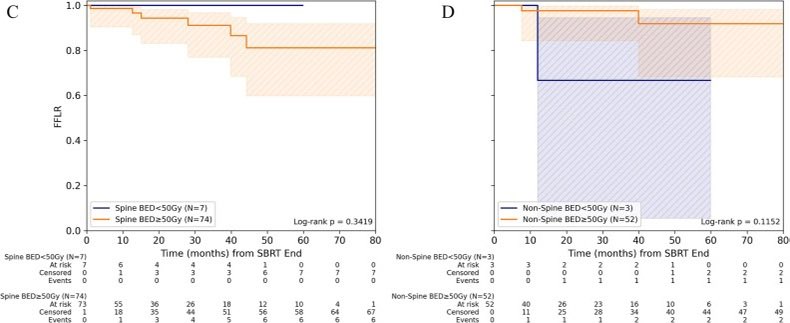
Protons for oropharyngeal cancer? Following the presentation of TORPedO results at #ASTRO25, it seems like it might come down to whether you believe in UK or US data - or, in the words of Dr Takiar, the session discussant, 'whether you believe in a round or a flat earth' #radonc