Sabitlenmiş Tweet

Time to update the #VExUS resources pinned thread 🧵📌
1/ Tweetorial on image acquisition.
#POCUS #MedEd
twitter.com/NephroP/status…
NephroPOCUS@NephroP
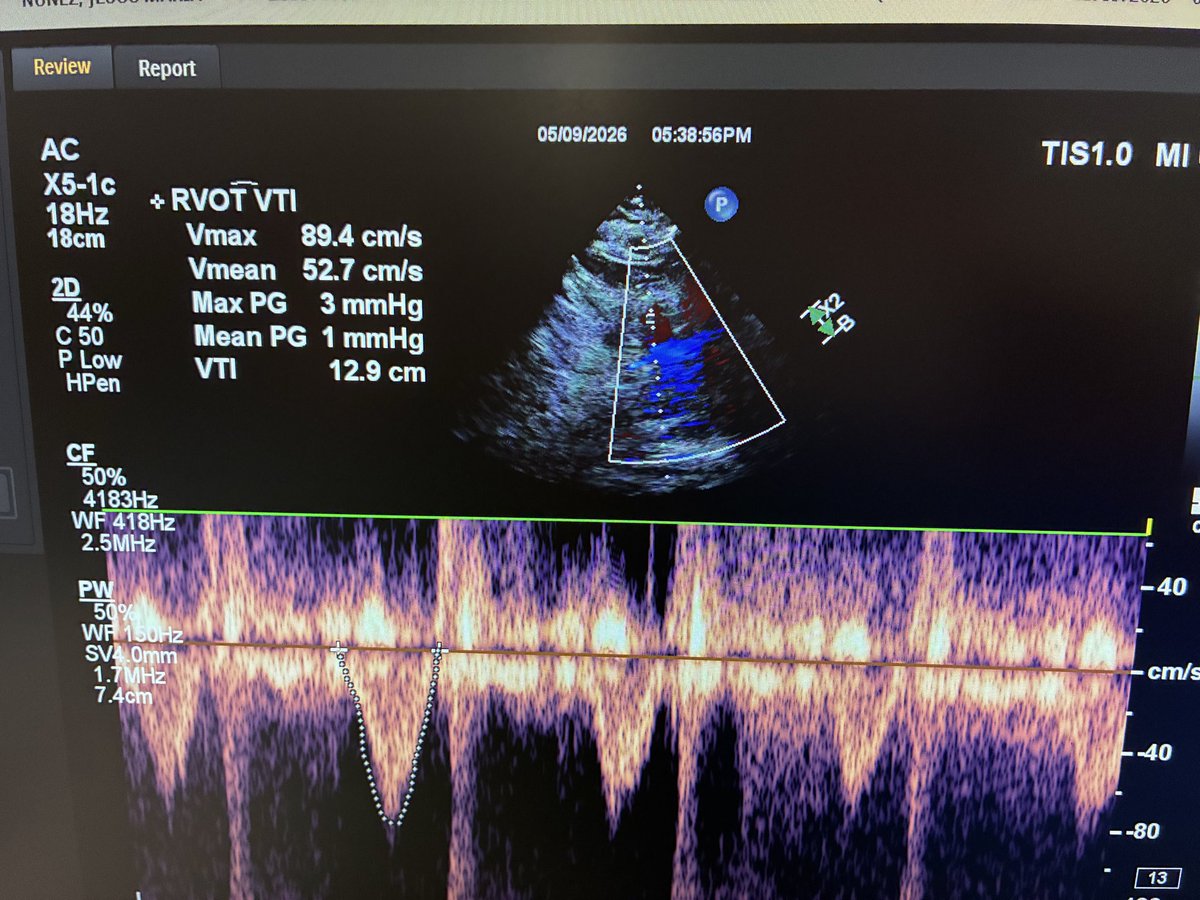
#POCUS #MedTwitter #Nephpearls Many #VExUS enthusiasts asked for a #tweetorial on image acquisition pearls. Did one b4 but time for an updated one 🧵 #1 Let's start with basics Color Doppler identifies the flow + tells the direction (blue is away & red towards the probe [BART])
English