Respiratory Science retweetledi
Respiratory Science
141 posts


Respiratory Science
@RespiratorySci
I’m interested in improving, simplifying and advancing respiratory science and research.
RespiratorySC Katılım Ekim 2022
29 Takip Edilen744 Takipçiler
Respiratory Science retweetledi

Patients with ACOS experience more severe respiratory symptoms and a poorer quality of life compared to those with only asthma or COPD. They also face a higher risk of exacerbations and more frequent hospital admissions. The path to developing ACOS can vary:
- It may evolve from COPD due to changes in airway structure and inflammation.
- It could stem from asthma following exposure to harmful substances.
- Alternatively, it might arise as a unique disease entity with its own specific pathology.



English

What is ACOS?
Asthma-COPD overlap syndrome (ACOS) refers to patients who exhibit characteristics of both asthma and chronic obstructive pulmonary disease (COPD). This condition highlights the complexity of diagnosing and managing airway diseases.
Generally, ACOS is identified in patients over the age of 40 who have persistent airflow limitations and either a history of asthma or significant improvement in lung function after using a bronchodilator.
#RespiratoryHealth #ACOS #AsthmaCOPDOverlap

English

📉 Results:
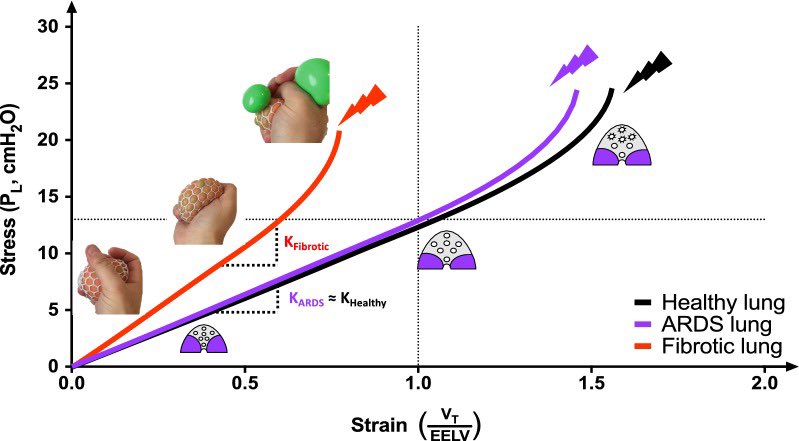
At lower pressures used in the study, EUIP lungs didn't expand much differently from ARDS lungs. However, the overall stiffness was significantly higher, increasing the risk of injury as pressures increased. The curve plotting lung stress versus strain was notably steeper in EUIP lungs. This means even small degrees of lung stretch could push these lungs into a danger zone where injury is more likely. The roles of elastin and collagen, crucial components of lung tissue, were examined. In EUIP, the contribution of collagen at high strains made the lungs stiffer. This study suggests that typical "safe" ventilator settings for ARDS may not be safe for EUIP patients. Adjustments in these settings are critical to prevent further lung damage.
English

New Research on Understanding Lung Damage in Patients with Lung Fibrosis:
EUIP stands for "Exacerbation of Usual Interstitial Pneumonia." It's a condition where patients experience rapid worsening of lung fibrosis, a disease where lung tissue becomes scarred and stiff. This makes breathing difficult and impacts oxygen exchange. Patients with EUIP are particularly sensitive to damage from mechanical ventilators, which are crucial for supporting critically ill patients. This sensitivity increases their risk of further lung injury and even death.
English

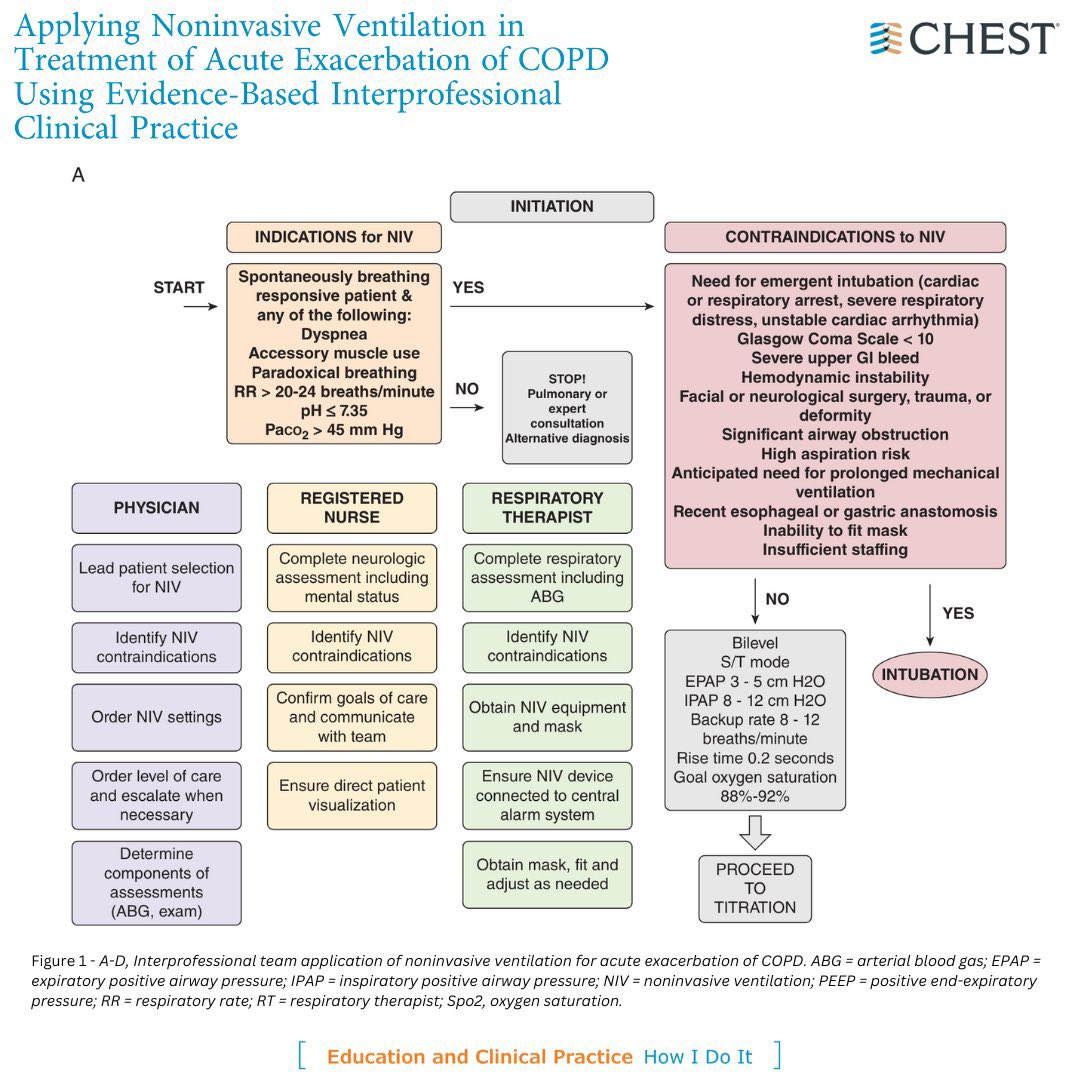
When someone with COPD (Chronic Obstructive Pulmonary Disease) has a severe worsening of their symptoms, which we call an acute exacerbation, doctors often need to help them breathe better. One effective way to do this is through something called Noninvasive Ventilation (NIV). This method helps the patient breathe without the need for more invasive procedures like inserting a tube into the airway.
What is Noninvasive Ventilation (NIV)?
NIV is a treatment that uses a mask connected to a machine to push air into the lungs. It helps increase oxygen levels and remove carbon dioxide, which can build up during a COPD exacerbation.
When and How is NIV Used?
Indications (When to Start NIV):
- The patient is awake and can breathe on their own but is struggling.
- Symptoms include:
- Difficulty breathing
- Using extra muscles to breathe
- Breathing seems out of sync
- Fast breathing (more than 20-24 breaths per minute)
- Blood tests show high levels of carbon dioxide (Paco2 > 45 mm Hg) or a low pH (≤ 7.35).
Contraindications (When NOT to Use NIV):
- Immediate life-threatening conditions where the patient cannot breathe at all (like cardiac or respiratory arrest).
- Very low consciousness level (Glasgow Coma Scale < 10).
- Severe bleeding in the stomach or upper intestine.
- Very unstable blood pressure or heart problems.
- Recent surgery on the face, head, or stomach that might interfere with wearing a mask.
- High risk of inhaling vomit into the lungs.
- Other specific medical reasons.
Steps for Applying NIV:
1. Initiation:
- A doctor decides if NIV is suitable.
- A nurse checks the patient’s neurological and respiratory status.
- A respiratory therapist makes sure there are no contraindications and prepares the NIV machine and mask.
2. Settings:
- The machine is set to help both during inhaling (IPAP) and exhaling (EPAP).
- Adjustments are made based on the patient’s needs and comfort.
3. Monitoring and Adjustments:
- Continuous monitoring to ensure the patient is improving.
- Adjustments are made based on ongoing assessments and blood gas results.
Role of the Healthcare Team
Implementing NIV requires a team approach:
- Physicians oversee the medical treatment, including deciding on NIV.
- Nurses monitor the patient’s overall condition and communicate any changes.
- Respiratory therapists are specialized in managing the equipment and making necessary adjustments.
Goal of NIV
The main goals are to make breathing easier for the patient, avoid the need for more invasive treatments like intubation, and improve survival rates by managing the exacerbation effectively.
By using a structured approach and teamwork, NIV can be a lifesaver for patients experiencing severe COPD exacerbations.
English

Post-capillary PH happens after blood moves through lung capillaries, usually linked to heart conditions. High PAWP shows the heart's struggles affect lung pressure.
Treatment differs: pre-capillary PH uses drugs targeting lung arteries, while post-capillary PH manages heart issues. Precise diagnosis via catheterization informs the right approach.
Picture in this tweet taken from (@aayshacader) Tweet: x.com/aayshacader/st…

English
Respiratory Science retweetledi

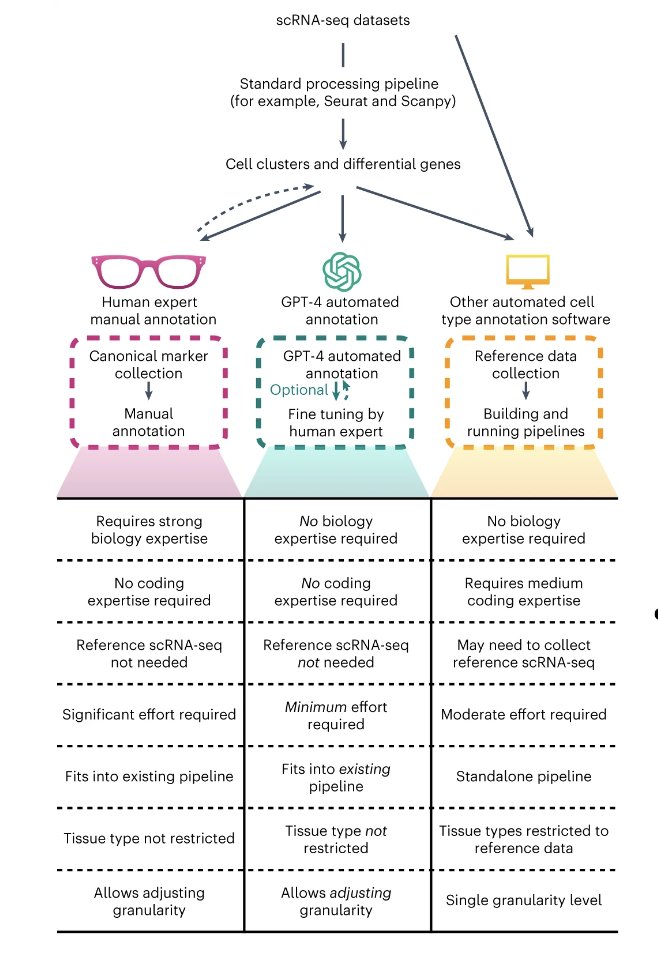
A new study evaluates the performance of GPT-4 for single-cell type annotation. @ZhichengJi @HWenpin
nature.com/articles/s4159…
English

Scientists have learned a lot about Acute Respiratory Distress Syndrome (ARDS). Despite new knowledge, finding good drug treatments is tough, partly because ARDS varies a lot.
Researchers found two types of ARDS: one with too much inflammation and one with too little. Each responds differently to treatments, which could help us find what works best.
In the ROSE trial, the team found more severe ARDS patients with high inflammation. This could guide future treatment based on a patient's specific ARDS type.
They also found genes related to inflammation were very active in severe ARDS patients. Understanding these genes could help us predict and treat ARDS better.
Studies show that blood tests and gene tests in ARDS patients give different information. This means we need to consider many types of tests to understand ARDS fully.
Finally, the way they use treatments like muscle relaxants in ARDS may need to change. We should focus on the patient's specific disease and how they're responding to treatment.
Source: bit.ly/3Vx4pOs
@ATSBlueEditor

English