Sabitlenmiş Tweet
Rajan kanth
2.3K posts

Rajan kanth
@kanthMD
On a Journey..!!!
WellSpan Health, York, PA Katılım Nisan 2009
500 Takip Edilen313 Takipçiler
Rajan kanth retweetledi

I’ve been an orthopedic surgeon for nearly 30 years, and a few patterns have become impossible to ignore. One is that many musculoskeletal problems in adults aren’t sudden injuries. They’re the moment when declining capacity and awful metabolic health finally reveals itself.
Over the decades your strength fades, muscle mass declines, as your aerobic capacity tanks. Tendons and connective tissues lose substance, stiffness, and resilience. For years the body compensated... quietly. Then one day a knee hurts during a run to get the train, or shoulder aches reaching overhead, or a back tightens lifting something simple.
At that point the story usually becomes more about structural damage. An MRI gets ordered. Welcome to high-tech, low-medicine. And the MRI almost always finds something. A meniscus tear. A rotator cuff tear. A disc bulge. Why? Because by midlife these findings are extremely common — even in people with no pain at all. If you have a tear in one shoulder, image the other shoulder... you probably have the same tear there. But I digress.
Once the scan appears, the narrative changes. The image becomes the diagnosis. Now the patient believes something is broken, and the focus often shifts to fixing what the MRI shows.
What often gets lost in this is the reason the symptoms appeared in the first place. Many so-called “atraumatic” orthopedic complaints are not purely mechanical failures. They are the moment when reduced strength, declining tissue capacity, and sometimes broader metabolic health issues finally reach a tipping point. Our tissues change over the decades... get over it.
In other words, the MRI didn’t create the problem. Well... it sort of did in this scenario. But all the MRI showed was something that was already there.... because of your age, lifestyle, health and so on.
The real driver of symptoms is often loss of physiologic reserve. Less muscle. Less tendon or aerobic resilience. Less tolerance for load, etc.
Once the MRI enters the picture, the risk becomes overtreatment. This is probably the number one reason people have surgery. When in many cases the most powerful intervention was never the scan or the procedure.
It was rebuilding capacity.
Strong muscles stabilize joints. Aerobic fitness improves metabolic health and tissue perfusion. Gradual loading restores tolerance.
But people often don't take PT seriously prior to surgery. They often take PT very seriously afterwards. Therefore, PT is probably the reason you feel better, despite the surgery.
The irony is that the treatment many people ultimately need is the same thing that might have prevented the problem in the first place.
Staying strong. Staying active. Maintaining the reserve that protects our joints/tendons/muscles/abilities as we age.
English

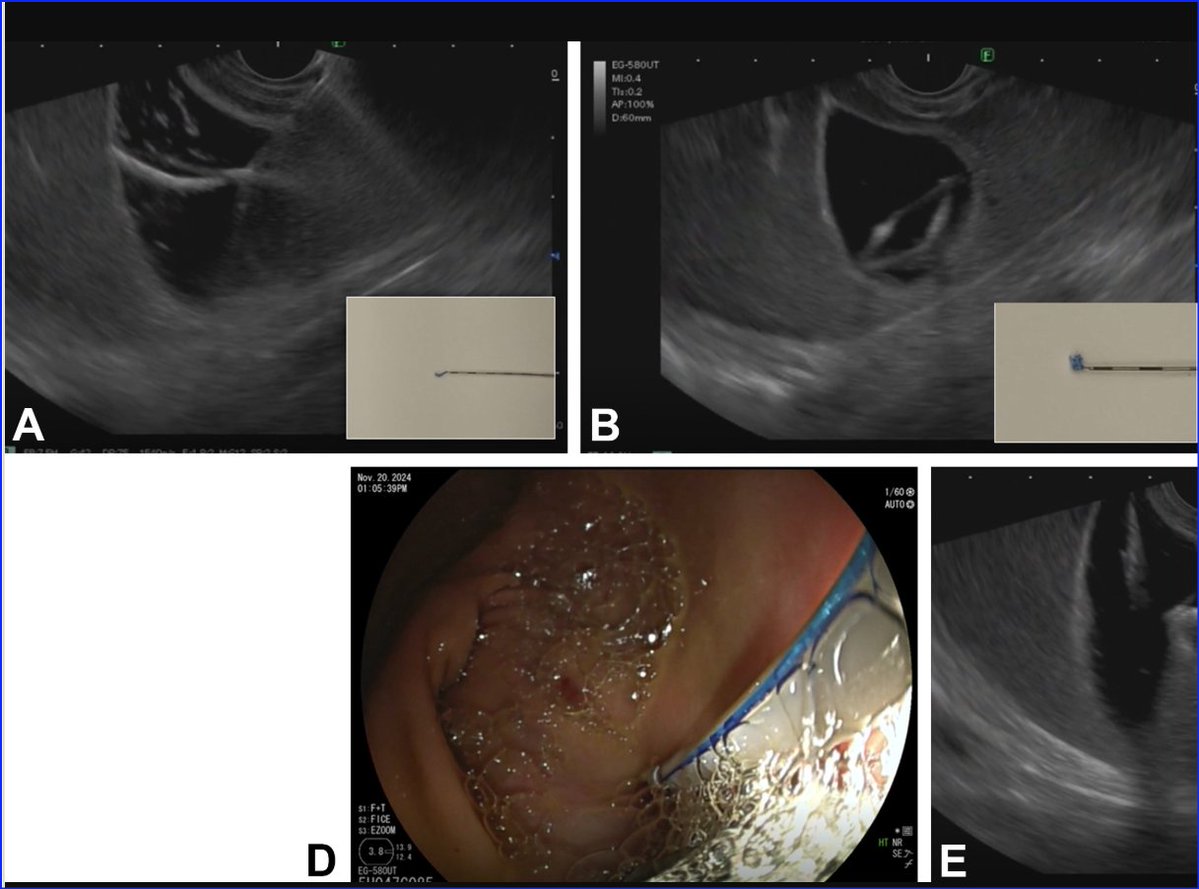
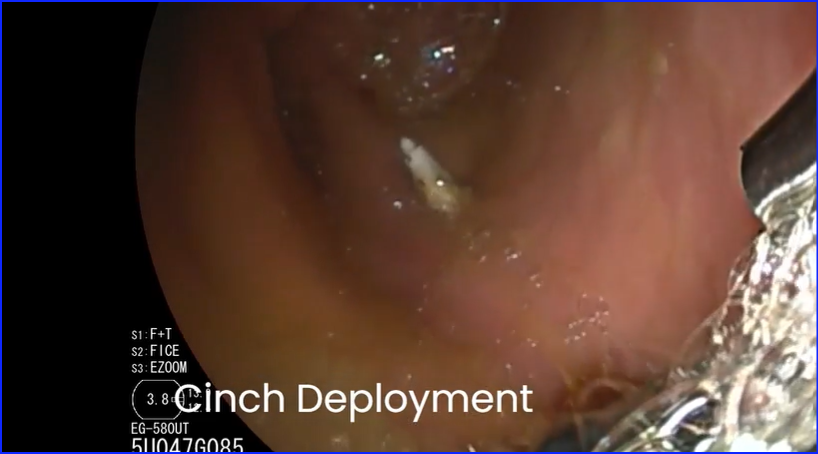
Transmural gallbladder drainage using a novel endosonographic-guided suture (with video) - Gastrointestinal Endoscopy #EUS #Suture # giejournal.org/article/S0016-…

English

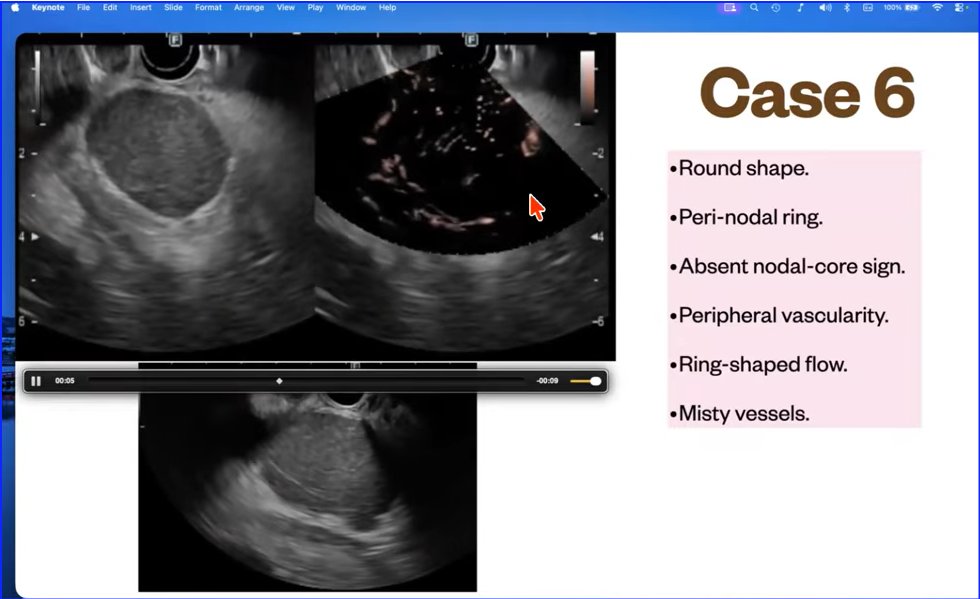
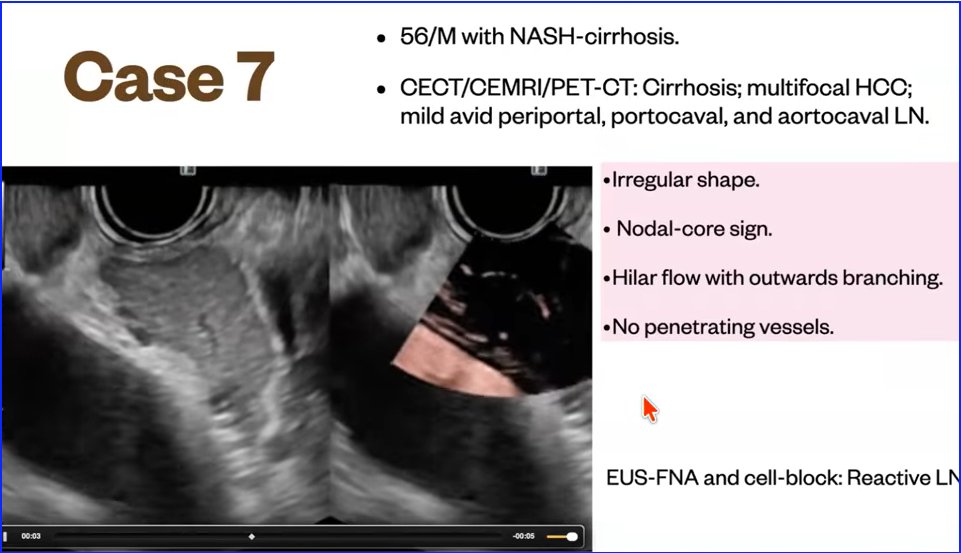
Lymph Node exam - EUS @ASGEendoscopy @drkeithsiau @DouglasAdlerMD @EUSandEndoscopy @NeethiDasu @PrabinSharmaMD

English

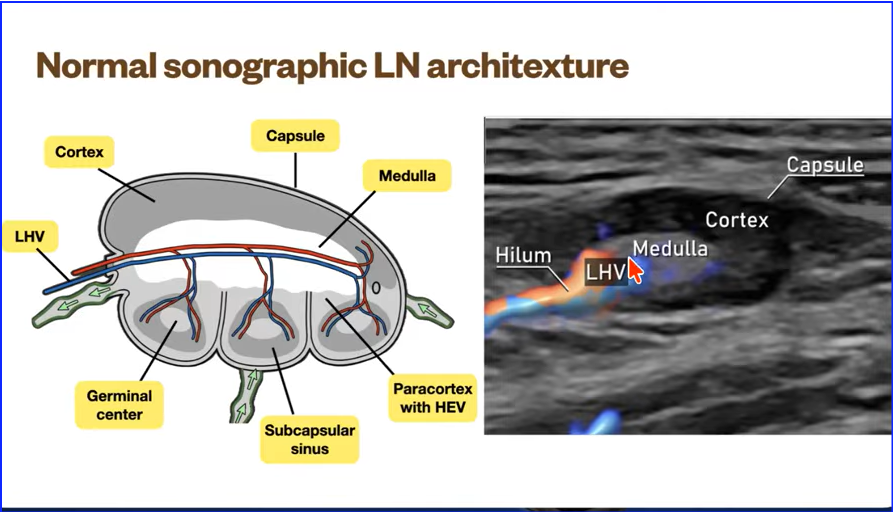
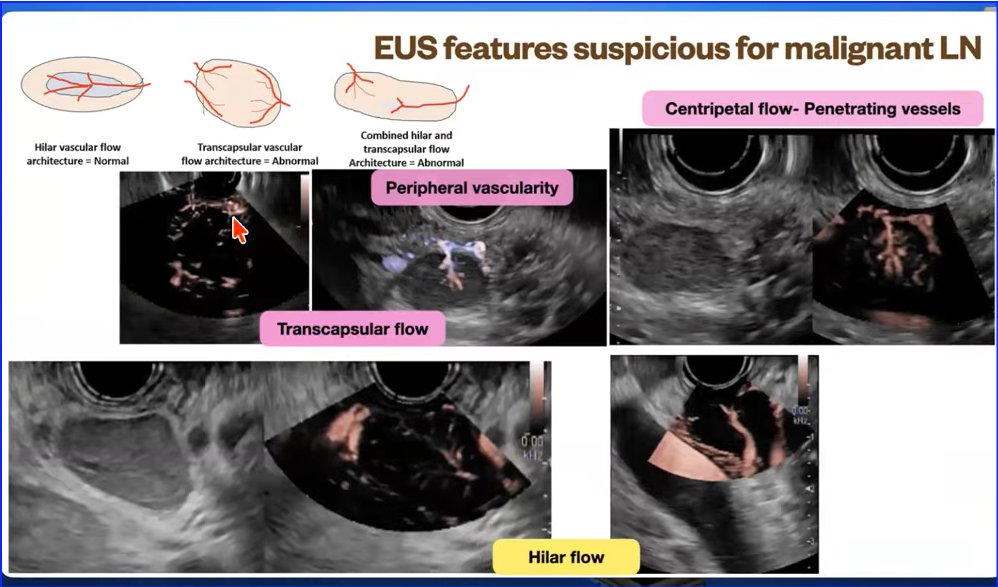
Lymph Node characteristics Findings on EUS exam
Pink Highlighted LN--> Malignant
Yellow Highlighted LN--> Benign
EUS by by Dr Vikram Bhatia
Source youtu.be/XBY448TO2WU?si… #EUS #GItwitter #LN #Malignancy

YouTube


English

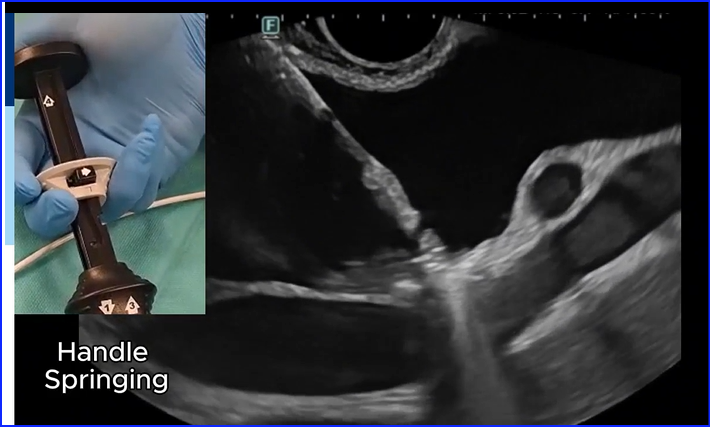
Failure of release of the Hot AXIOS distal flange: "handle springing" as a rescue technique thieme-connect.de/products/ejour… #GItwitter #Metwitter #EUS #AXIOS
English

Asymptomatic Walled‐Off Pancreatic Necrosis: Natural Course and Risk Factors for Intervention --- size of > 5.6 cm predicted the need for intervention with 88.5% sensitivity and 54% specificity. #GITwitter #MedTwitter #WON #Pancreatitis onlinelibrary.wiley.com/doi/10.1002/ue…
English
Rajan kanth retweetledi

In my state of Pa, 40% of obstetric patients are on Medicaid.
-Medicaid uses a single bundled payment for the entire "global obstetric package," which = 13 antepartum visits, delivery, and 6 weeks of postpartum care.
Don’t forget all the phone calls and messages.
-Reimbursement Amount: from what I found the reimbursement Medicaid pays an obstetrician on average is around $1,100 for that global package including delivery.
-now let’s add malpractice: Pa OB average malpractice rate per year is around $70,000, ( up to 100K in cities) BUT, we are the only state in the nation with an additional malpractice payment called MCARE adding another $20k per year to the cost of malpractice we have runaway verdicts out of Philadelphia. We also have Venu shopping, which means you could be in the western part of the state and dragged into Philly for a case.
Mind you, we haven’t discussed the stress of going through malpractice plus adding potential travel to it.
All of the above is why there are 23out of 67 counties in Pa with no delivery hospital.
Well, this is mostly rural, in my county of books, the hospital where I delivered my two children and worked for 13 years, just closed their OB unit because the obstetricians left. With everything that I’ve written above, who could blame them?
But who suffers most? The patients.
rural.pa.gov/download.cfm?f…
Edward S.@edwards183
@mass_marion Cool. Cut all Medicaid CMS reimbursement rates by 50% and repeal the FMAP formula under Section 1905(b) that gives states lower per capita up to 66% more funding. (Of course we would see just about every rural hospital outside of the wealthy states fail in a manner of 6 months)
English
Rajan kanth retweetledi

Two-sample FIT as a tool to avert colonoscopy in symptomatic patients: a prospective multicenter cohort study
Find the article at: doi.org/10.1055/a-2650…
Sarah Moen et al. @ESGE_news

English

Robot performs first realistic surgery without human help hub.jhu.edu/2025/07/09/rob… via @HubJHU #Medtwitter #surgery
English
Rajan kanth retweetledi

Rajan kanth retweetledi

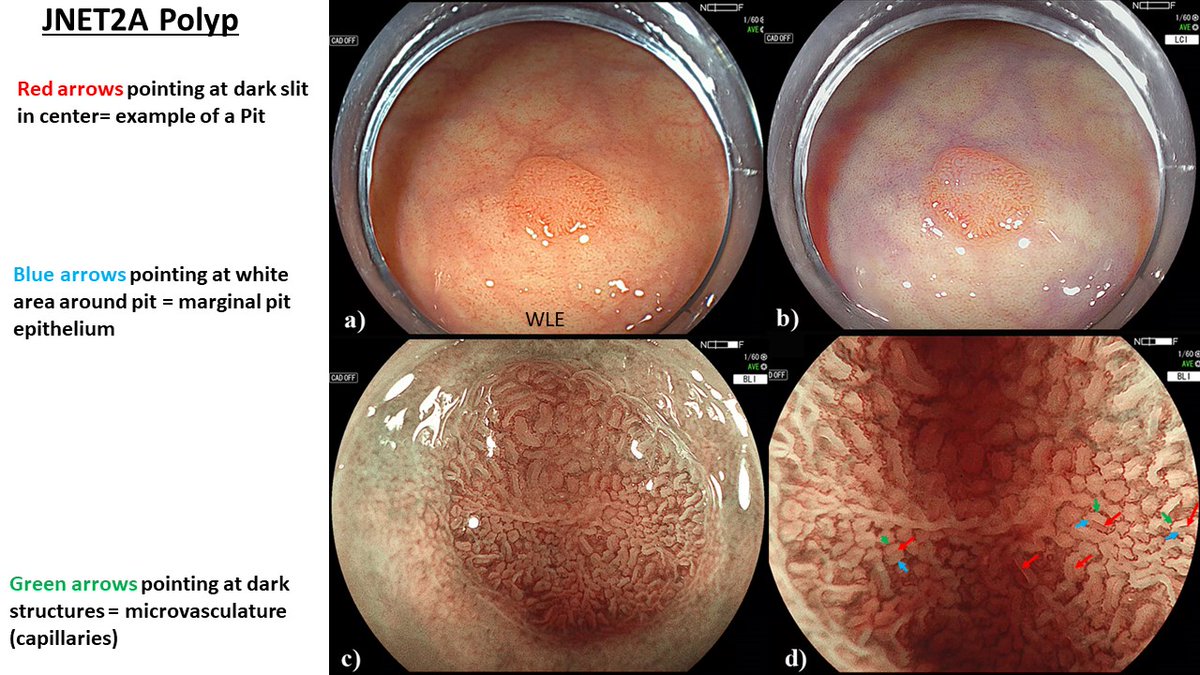
🔎 JNET 2A lesion.
Do you see it?
🔴 Barley visible central slit → pit.
🔵White marginal epithelium around it.
🟢Dark microvascular network.
Optical diagnosis isn’t guesswork - it’s systematic.
Learn a structured approach to lesion characterization.
opticaldx.com
Robert Bechara@RobertBechara
A typical endoscopic appearance of autoimmune atrophic gastritis, with an interesting finding of WGA. Learn how to recognize, assess, and approach gastric atrophy in a structured way at the Queen’s Optical Diagnosis Course 🗓 April 11–12, 2026 🔗 opticaldx.com
English

A bubble-free strategy for saline-immersion endoscopic submucosal dissection: optimized electrosurgical settings and continuous low-pressure saline perfusion thieme-connect.de/products/ejour… #MedTwitter #ESD

English

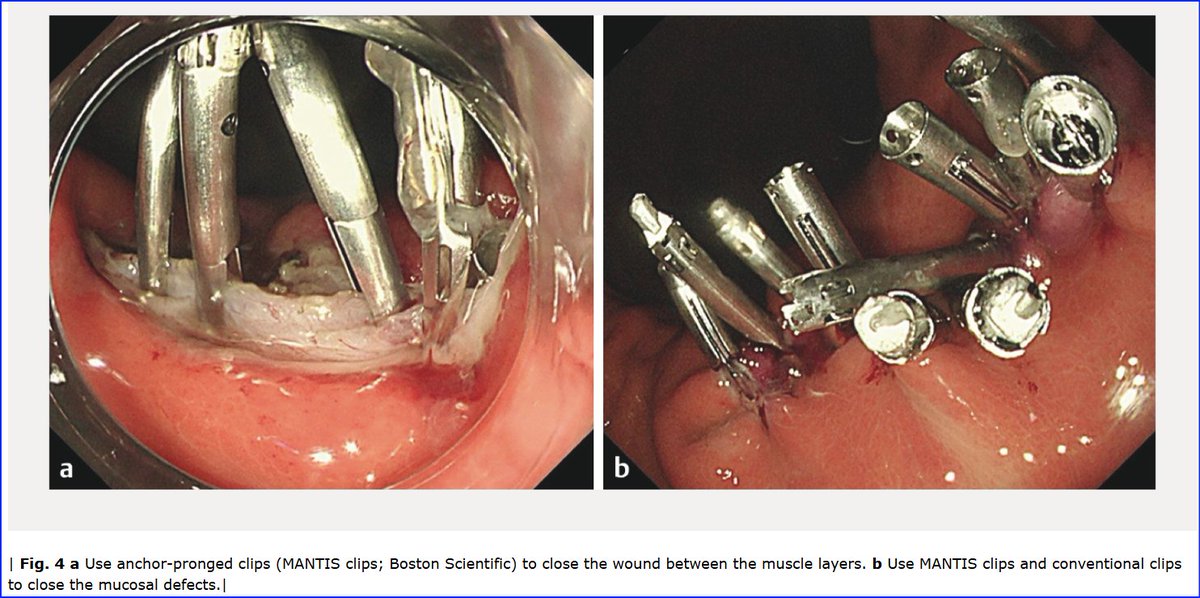
Two-layer closure method using anchor pronged clips for endoscopic full-thickness resection thieme-connect.de/products/ejour… #MedTwitter #ESD #EFTR
English
Rajan kanth retweetledi

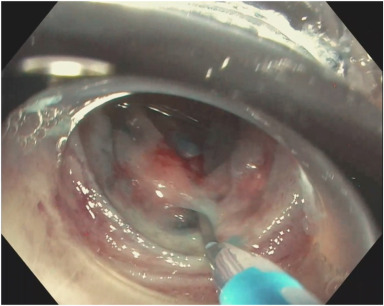
VideoGIE Editor's Choice: "Rendezvous-assisted endoscopic retrograde pancreatography using a dual-wire balloon technique for stenotic pancreaticojejunostomy in post-Whipple anatomy" by Petr Vanek et al. videogie.org/article/S2468-…
#GITwitter
Română
Rajan kanth retweetledi

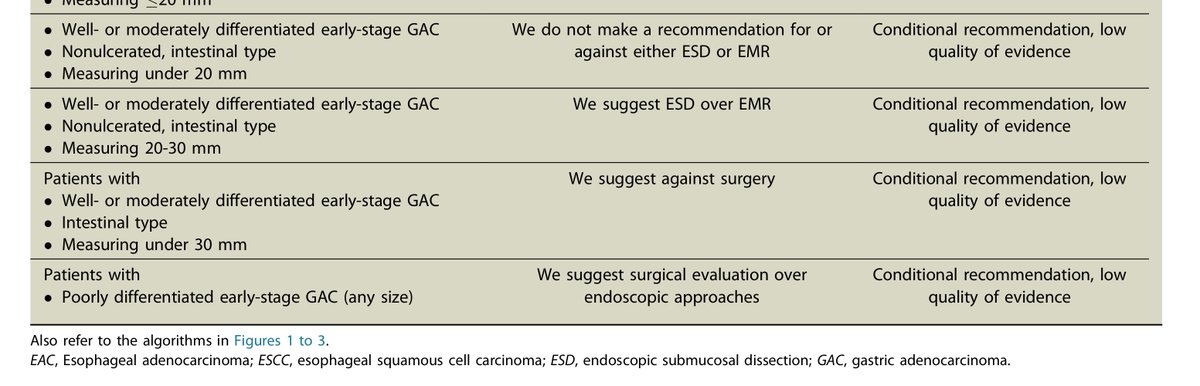
ASGE guideslines for early gastric cancer:
giejournal.org/article/S0016-…
🔑Lesions < 2 cm, well differentiated, intestinal: EMR = ESD
🔑 Size 2-3 cm, well differentiated, intestinal = ESD
🔑 > 3 cm or poor differentiation= Consider surgery

English

Fluoroscopy-guided, sheath-assisted biopsy for indeterminate intraductal biliary masses thieme-connect.de/products/ejour… #EUS #MedTwitter #GITwitter
English
Rajan kanth retweetledi

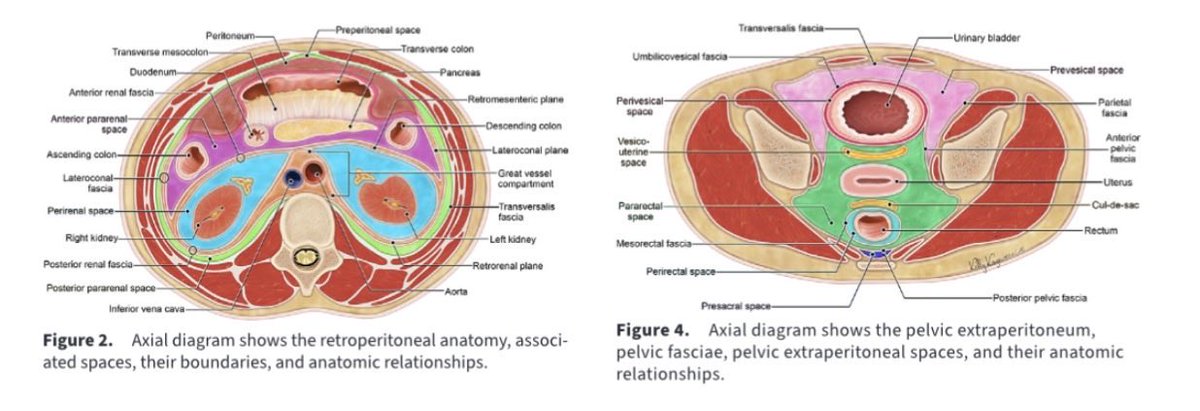
Here we go! Another excellent review from @RadioGraphics: “Retroperitoneum and Pelvic Extraperitoneum: Anatomic Landmarks, Imaging Features, and Patterns of Disease Spread” 🩻📊
A must-read deep dive—not just for radiologists, but for general surgeons, oncologists, ER docs & more!
✅ Complex fascial planes
✅ Key anatomy (vessels, lymphatics, nerves) on CT and MRI
✅ Disease spread patterns: fluid collections, hematomas, urinomas, abscesses, tumors (RCC, lymphoma, sarcomas), inflammation (pancreatitis, IgG4), trauma & beyond
✅ Flowcharts for diagnosis, mass classification & spread
🥇 Huge congrats to the Authors on this outstanding work!
RadioGraphics keeps delivering amazing content that helps doctors, trainees & patients—thank you 🙏
🔗 pubs.rsna.org/doi/10.1148/rg…
#Radiology #AbdominalImaging #Retroperitoneum #CT #MRI @RadioGraphics @cookyscan1



English

Endoscopic Ultrasound guided Obliteration of Gastric Varices: ... youtu.be/Ufed1iisEDI?si… via @YouTube #MedTwitter #gitwitter #EUS #Varices

YouTube
English

EUS for Gastric Varices :Tracing the Feeder Vessel youtu.be/nlu-0fa8vsU?si… via @YouTube #MedTwitter #gitwitter #EUS #Varices

YouTube
English

Rendezvous-assisted ERCP using a dual-wire balloon technique for pancreaticojejunostomy (Hurricane balloon catheter. Removing the wire stiffener allowed a second 0.021-inch wire to be placed alongside 0.18) #MedTwitter #EUS #gitwitter videogie.org/article/S2468-…
English