Imad Damaj
2K posts

Imad Damaj
@DamajLab
VCU Pain And neuropathy Research Program Neuropharmacology of drug addiction and pain- nicotinic Lab







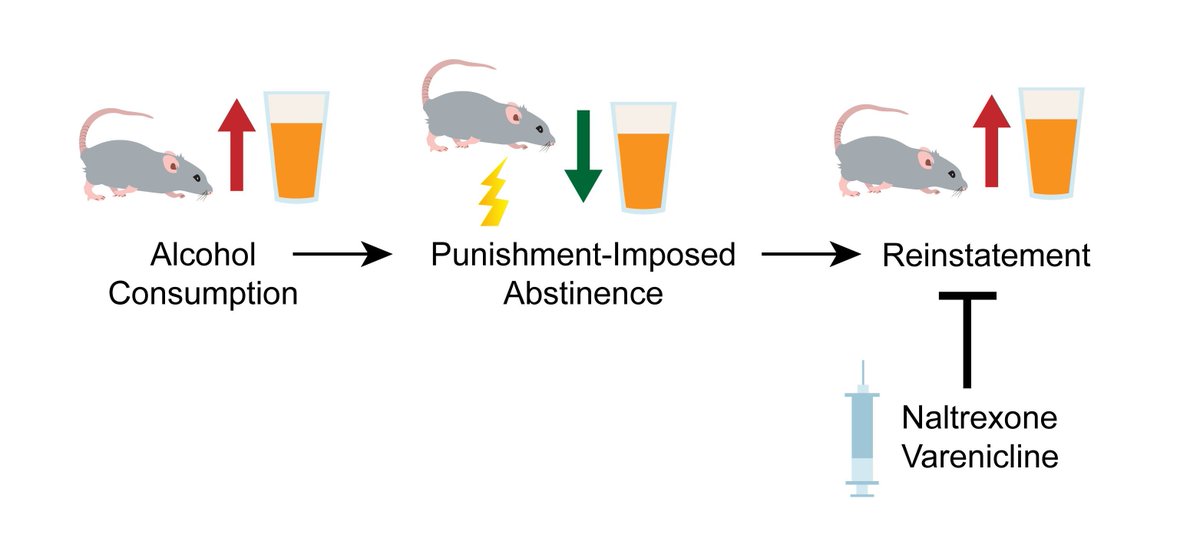
Low-dose semaglutide reduced alcohol craving and consumption in adults with alcohol use disorder. ja.ma/4gQUxaM



Supplements and chronic pain: What does the research say? A list of 5 supplements that may help with nerve and chronic pain, as part of a broader treatment plan: 1. Acetyl-L-Carnitine -Helps your cells make energy. - Studied in people with diabetic nerve pain. - May help nerves send signals better. 2. Alpha Lipoic Acid - Works as an antioxidant and affects calcium in cells. - May help with nerve pain. - Can cause an upset stomach in some people. 3. Vitamin C - Not just for colds. -Some research shows it may lower the chance of nerve pain after surgery. 4. Fish Oil (Omega-3s) - May help reduce inflammation and pain. - But it can make your blood thinner, which might raise the risk of bleeding. 5. Creatine - Often used by athletes for muscle strength. - Small studies suggest it might help people with fibromyalgia and similar conditions.







This is a cool paper, but not sure if the findings are impressive enough to be too excited about. The authors used a GWAS of a pain phenotype and decided to study a gene (SLC45A4) at a specific locus in detail. The genetic association itself is robust, replicates across multiple cohorts, but not clear if SLC45A4 is the causal gene. Despite the availability of rare variants in UK Biobank, no mention of SLC45A4 coding variant associations with pain. Quick look at the genebass, shows nothing striking for pain. Being the closest gene and not well characterized before, the authors studied the gene in detail using a range of functional experiments. In the process, they discovered that the gene encodes a polyamine membrane transporter and expressed in dorsal root ganglion (DRG) neurons, among others. They went on to create a knockout mouse. The phenotypes in the knockout seem to be similar to the wild type for the most part: - Anatomically and histologically, no differences. - Biochemically, there were differences in the polyamine levels in the spinal cord, DRG and plasma, which validates Slc45a4 as a polyamine transporter. - Behaviorally, no remarkable differences in sensory phenotypes, except for reduced sensitivity to thermal and chemical-induced pain in KO mice. Here is one critical, puzzling observation: the missense variant (p.Asn718Asp) in SLC45A4 (believed to be the causal variant) has no impact on the polyamine transport when recreated in the. Not only that, mutating the site to any other amino acid (Ala, Arg, Trp) had no impact on polyamine transport. Overall, the genetic association in humans and KO phenotypes in mice are interesting on their own, but no convincing connection between the two. Genetic targets for pain have been extraordinarily difficult as exemplified by recent setback by Vertex's Nav1.8 (SCN10A) inhibitors, which produced unimpressive results in clinical trials. This is despite that SCN10A had a strong human genetic association with pain (both common and rare variants). So, I'm not sure if SLC45A4 could be considered a promising drug target for pain yet. Maybe it is, but we can't say that with the current evidence. Middleton, Markússon, Newstead, Bennett, et al. Nature 2025 nature.com/articles/s4158…