Sabitlenmiş Tweet

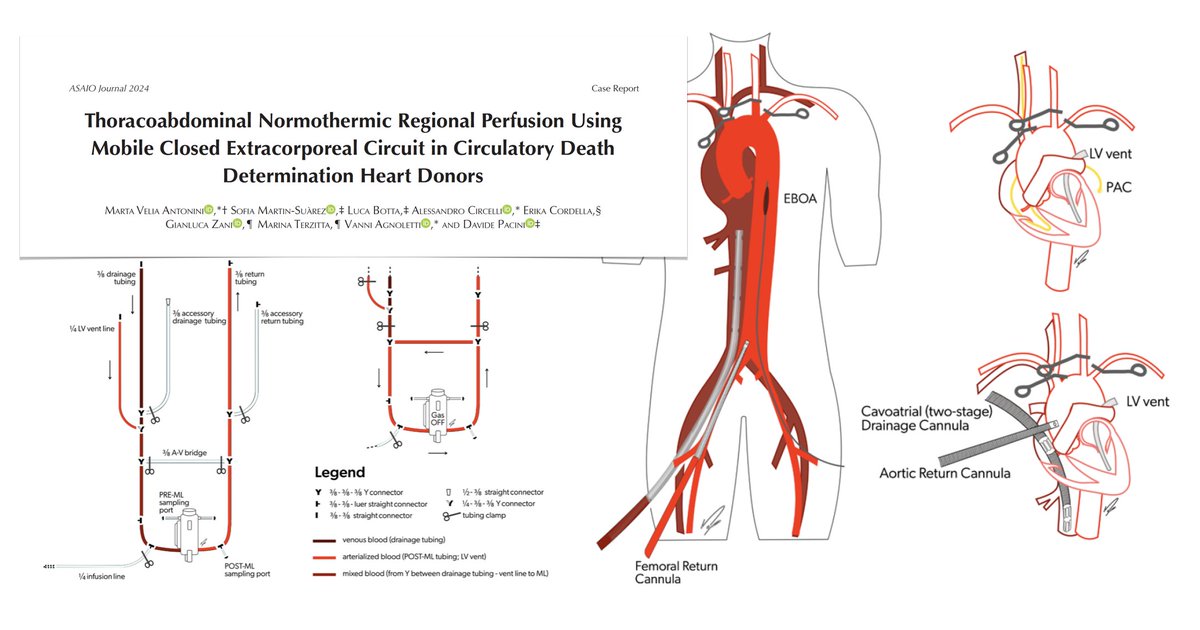
TA #NRP in cDCD heart donors using closed #ECMO circuit, modified to provide
🩸🌡️effective NRP despite prolonged fWIT
🫀LV venting
🫀 fast conversion to central configuration as needed
⭕️ shunt for recirculation
🫧 air management
#FOAMcc @asaiojournal
🔓bit.ly/TANRPasaio
TA-NRP using fully mobile, closed #ECLS circuit could be safe strategy to support combined thoracic/abdominal organs recovery also in peripheral centers without cardiac surgery program, contributing to the expansion of DCD programs, increasing availability/quality of grafts, improving recipients’ outcome. @ESOTtransplant @gabriel_oniscu @LuPoten @Unibo @AUSLRomagna
English