
ID:IOTS podcasting / idiots-pod.bsky.social
2.6K posts


ID:IOTS podcasting / idiots-pod.bsky.social
@IDiots_pod
Now on BlueSky! https://t.co/FykdlCepsQ. The UK’s Prémièrẽ Infectious Disease Podcast










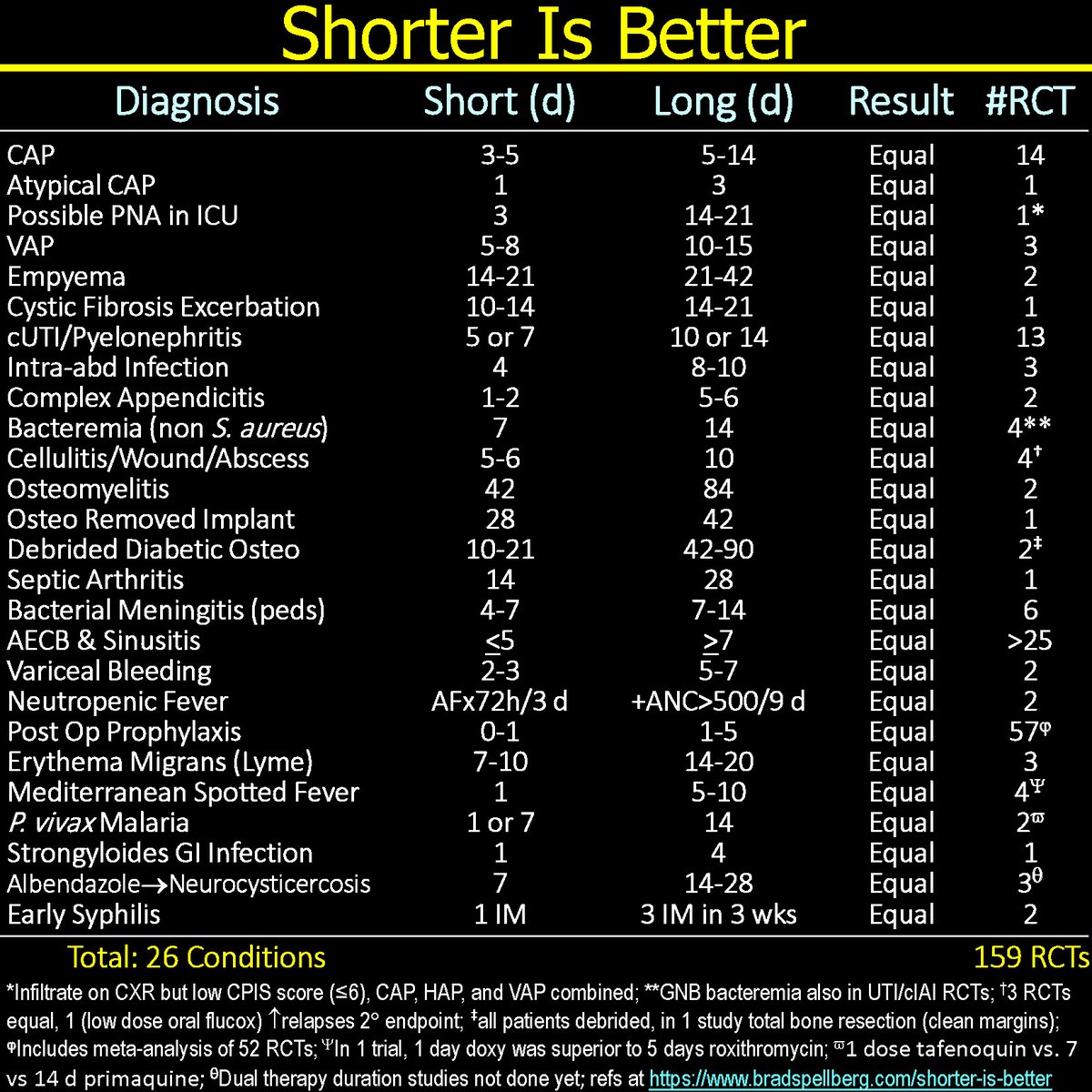









We all know how hard it is to put down zombies. It’s time to World War Z the zombie tests, ESR and CRP!

@ABsteward I do too! Course i wrote the protocol for that trial! And do love rifampin for Pseudomonas.

I joined the wonderful Baroness Bennett @natalieben & my favourite podcast buddies @IDiots_pod to discuss #microbiotoxicity & #biocides - including how legislation can help protect our #microbiomes. Check it out! 💙🧫🦠 idiotspodcasting.buzzsprout.com/1782416/episod…







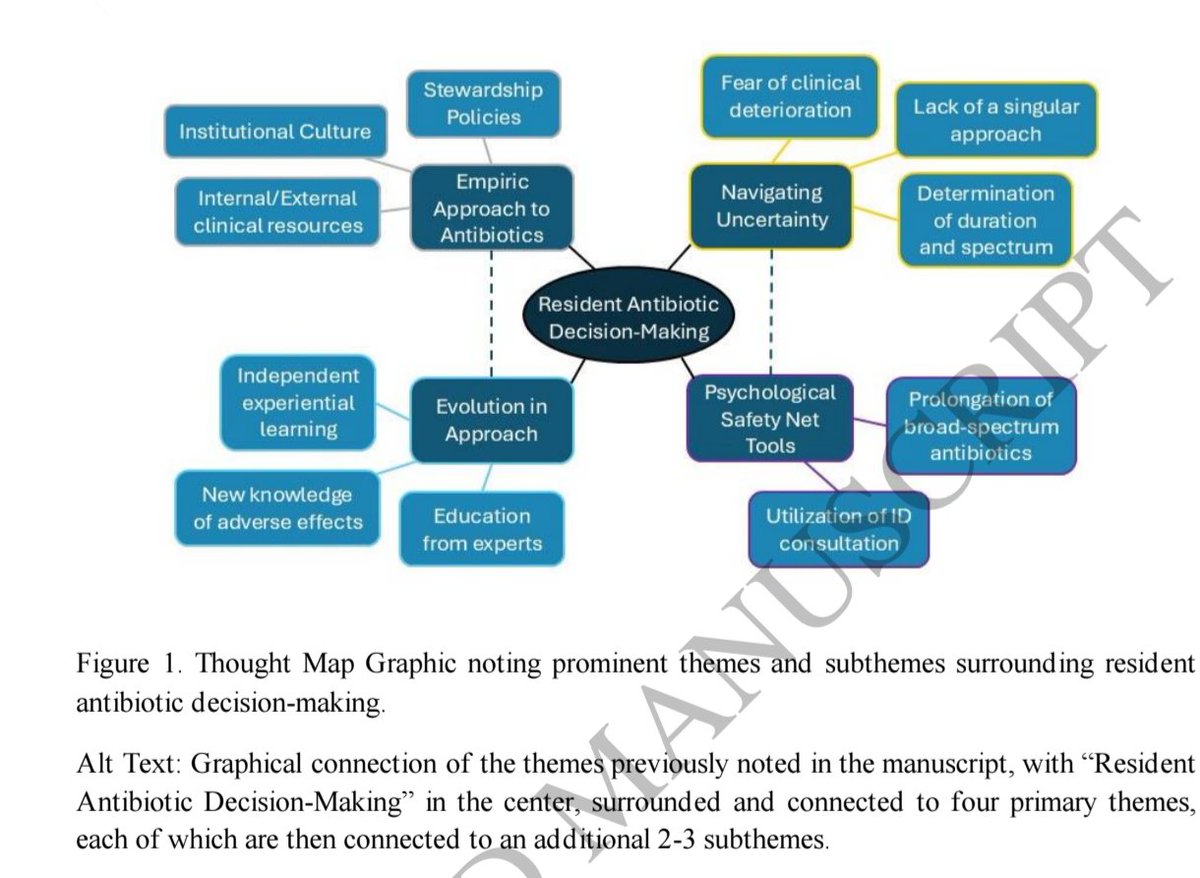



🆕🔥Systematic review and meta-analysis Linezolid versus clindamycin for toxin inhibition in severe skin and soft tissue infections No significant difference in ICU and hospital length of stay were noted between linezolid and clindamycin-based regimens. Lower rates of AKI were reported with linezolid. However, given the study design and potential risk of bias these results should be interpreted with caution link.springer.com/article/10.100…

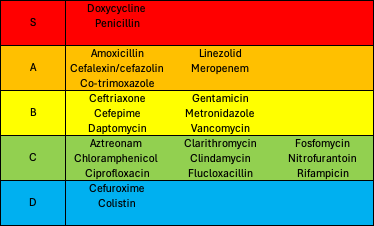
Yo ho ho, 4 our listeners dearest We present an ABx tier list Ranking drugs from S to D In a manner so Christmassy So sit back relax & have a drink As we discourse in cladist think And if u rank a different way We forgive u this Christmas Day #idXposts podcasts.apple.com/gb/podcast/id-…







