
Jonathan Strauss
98 posts

Jonathan Strauss
@JBStraussMD
MD, MBA| Associate Professor, Vice-Chair for Education, Dept of Radiation Oncology @NUFeinbergMed, #RadOnc
Katılım Ocak 2019
689 Takip Edilen853 Takipçiler

@NehaVapiwala @ken4englewood @MSteinbergMD @BrianJDavisMDPh @ajacobmiller @ARRO_org @ASTRO_org How quickly must programs shrink the residency cohort to meet the new faculty:resident ratio?
English

We heard you, fellow rad oncs. Proud (relieved?) to announce final board approval of improvements to RO residency program requirements. Crossed the multi-step finish line - now the real work begins. @ken4englewood @MSteinbergMD @BrianJDavisMDPh @ajacobmiller @ARRO_org @ASTRO_org
ACGME@acgme
At its February meeting, the #ACGME Board approved focused revisions to the Program Requirements for a number of specialties/subspecialties, effective July 1, 2022. Visit the Program Requirements and FAQs and Applications page of the specialty on the ACGME website for more info.
English

SLN + (N1, no ALND)
BCS: WBI + RNI/Can also consider high tangents
Mastectomy- I manage same way as BCS. No ALND and strongly consider PMRT even if 1 + SLN. Can consider no RT as well but less data with SLN+ no ALND.
#5
English

Management of the axilla is one of the most challenging and rapidly evolving areas of breast cancer RT(#bcsm). Wanted to present common scenarios and management, lots of different and correct ways to proceed @theRADSofKHAN @IBCradiation @reshmajagsi @JBStraussMD @RTendulkarMD #1
English

@CShahMD Re: cN1 pN1mic after NAC. This makes sense to me until Alliance A011202 reports on the value of cALND in this setting. Some data suggest a higher than expected risk of residual nodal disease in this setting. pubmed.ncbi.nlm.nih.gov/32086652/
English

Neoadjuvant-
cN1pN1mic/N1-3- ALN, RT with RNI
cN2-3- ALND, RT with RNI regardless of response
#10
English

@CShahMD @ChelainG @subatomicdoc @DrN_CancerPCP @fumikochino @Rad_Nation @ErinGillespieMD @MylinTorres @IBCradiation @HinaSaeedMD @GitaSuneja @SueEvansMDMPH @EricDonnellyMD @SFShaitelmanMD @BenSmithMD @KimCorbinMD @CShahMD and others: do you ever sequence 5 fraction RT prior to chemo now that it wouldn’t lead to a delay?
English

@JBStraussMD @ChelainG @subatomicdoc @DrN_CancerPCP @fumikochino @Rad_Nation @ErinGillespieMD @MylinTorres @IBCradiation @HinaSaeedMD @GitaSuneja @SueEvansMDMPH @EricDonnellyMD @SFShaitelmanMD @BenSmithMD @KimCorbinMD I agree @JBStraussMD . I dont consider IORT (electron or low energy) equivalent to other forms. In terms of data for local control, the strongest data is with interstitial and then 3DCRT (toxicity concerns)/IMRT. I routinely use 30/5 IMRT and consider this standard of care now
English

@CShahMD @ChelainG @subatomicdoc @DrN_CancerPCP @fumikochino @Rad_Nation @ErinGillespieMD @MylinTorres @IBCradiation @HinaSaeedMD @GitaSuneja @SueEvansMDMPH @EricDonnellyMD @SFShaitelmanMD @BenSmithMD @KimCorbinMD I tend to use 5.2 Gy x 5 daily with 3D CRT and usually prone — an approach pretty similar to yours. combining 5 fx approach and PBI gives acute toxicity that is dreamy.
English

@CShahMD @ChelainG @subatomicdoc @DrN_CancerPCP @fumikochino @Rad_Nation @ErinGillespieMD @MylinTorres @IBCradiation @HinaSaeedMD @GitaSuneja @SueEvansMDMPH @EricDonnellyMD @SFShaitelmanMD @BenSmithMD @KimCorbinMD But I welcome differing opinions from this august group! Perhaps someone can convince me that my skepticism of some PBI techniques is unfounded?
English

@CShahMD @ChelainG @subatomicdoc @DrN_CancerPCP @fumikochino @Rad_Nation @ErinGillespieMD @MylinTorres @IBCradiation @HinaSaeedMD @GitaSuneja @SueEvansMDMPH @EricDonnellyMD @SFShaitelmanMD @BenSmithMD @KimCorbinMD I would also say that ELIOT and TARGIT-A have not sold me on small volume IORT as PBI.
English

@CShahMD @ChelainG @subatomicdoc @DrN_CancerPCP @fumikochino @Rad_Nation @ErinGillespieMD @MylinTorres @IBCradiation @HinaSaeedMD @GitaSuneja @SueEvansMDMPH @EricDonnellyMD @SFShaitelmanMD @BenSmithMD @KimCorbinMD I think we will have more success making PBI truly standard if we acknowledge that not all techniques are equally optimal. Specifically, that techniques that encompass a small volume of the breast may fall short of equivalence with WBRT or large volume PBI.
English

@ErinGillespieMD @ChelainG @theRADSofKHAN @LiorBraunstein @CahlonOren Just read this editorial. Love it. Agree completely. And would add that although it is always nice to see long follow up, delays in implementation of shorter fractionation schemes have costs, too. I hope your clarion call sounds in the halls of the NCCN soon.
English

🇺🇸 #bcsm #radonc "Are 5-Year RCT Results Sufficient for Implementation of Short-Course Whole Breast RT?" 🤔
Our editorial reviewing 5- vs 10-yr results from similar prior studies is in print 📰in #PracticalRO:
practicalradonc.org/article/S1879-…
@theRADSofKHAN @LiorBraunstein @CahlonOren
English

@toddscarbrough In the Conclusions section, the authors suggested protons could be useful for dose escalation in GBM. 😱 That strategy has failed more often than Pinky and the Brain. But use in lower grade gliomas, that I get!
English

As rare as the jackalope
A randomized (small, phII) IMRT vs proton trial from MDACC
No diff's in any oncological outcomes (or neurocog decline)
More gr 2 or greater tox's in IMRT arm (p=0.02)
Fatigue IMRT > proton (p=0.05)
(from ACR Journal Advisor)
academic.oup.com/neuro-oncology…
English
Jonathan Strauss retweetledi

#FixPriorAuth bill now backed by majority of House! Major milestone for #HR3173. #radonc @ASTRO_org
politi.co/3mDmbMD via @politico

English

@TylerSbrt @UCSDRadMed In lymphoma the introduction of chemo allowed us to safely dose-reduce RT. Perhaps the superfluousness of superflab indicates it is time to revisit the ideal PMRT dose in the modern era, especially as we treat more stage II dz
English

@TylerSbrt @UCSDRadMed …then maybe we should ideally use bolus but reduce our prescription dose? Why give the ribs 50 Gy but the true targets 40 Gy?
Perhaps it us time to rethink how much dose we need in an era of low volume microscopic disease and excellent systemic therapies.
English

No more bolus for typical patients getting post-mastectomy RT?
I love a paper that starts with cobalt and ends with: "Yeah, this thing we've been doing forever probably does more harm than good, and we can stop now." #bcsm #radonc
Thoughts?
@UCSDRadMed
Erin Gillespie, MD MPH@ErinGillespieMD
#bcsm #radonc "The use of bolus should be limited to highly selected [PMRT] cases..." 🤯 New consensus 📰 in Green Journal: sciencedirect.com/science/articl…
English
Jonathan Strauss retweetledi

@subatomicdoc @IBCradiation @ErinGillespieMD @MylinTorres @Icro_Meattini @CShahMD Thanks for the input. What significant side effect did you see?
English

@IBCradiation @ErinGillespieMD @MylinTorres @Icro_Meattini @CShahMD @JBStraussMD I've used pentoxifylline selectively since ~2006. I've had some people with side effects, one serious. It does require closer followup but when it works it's been a major help for improving patient QoL.
English

“Once we hear the story and accept it as true, we rarely bother to question it.”
#bcsm #radonc can we revisit pentoxifylline (PTX) 💊 for RT fibrosis? 🤔
📰 RCT for prevention #RedJournal: sciencedirect.com/science/articl…
📰 RCT for tx @ASCO_pubs: pubmed.ncbi.nlm.nih.gov/12829674/
@Sushilberiwal
Ross Local Schools Curriculum Dept@RLSDcurriculum
An excerpt from page 4 of Think Again by @AdamMGrant. I’ve got a sneaking suspicion that the other 250 pages are going to be 🔥.
English
Jonathan Strauss retweetledi

Charlotte Coles reports the results from the IMPORT-HIGH trial. A masterclass in trial design and delivery - this is why the UK is rightly renowned for practice-changing #radonc trials - but also on how to report a trial clearly and succinctly 👏 #ESTRO2021
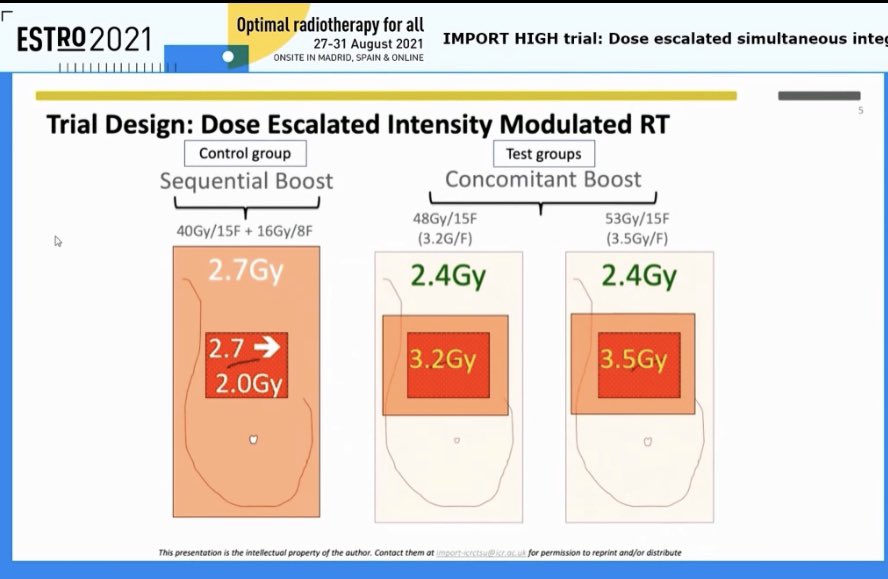
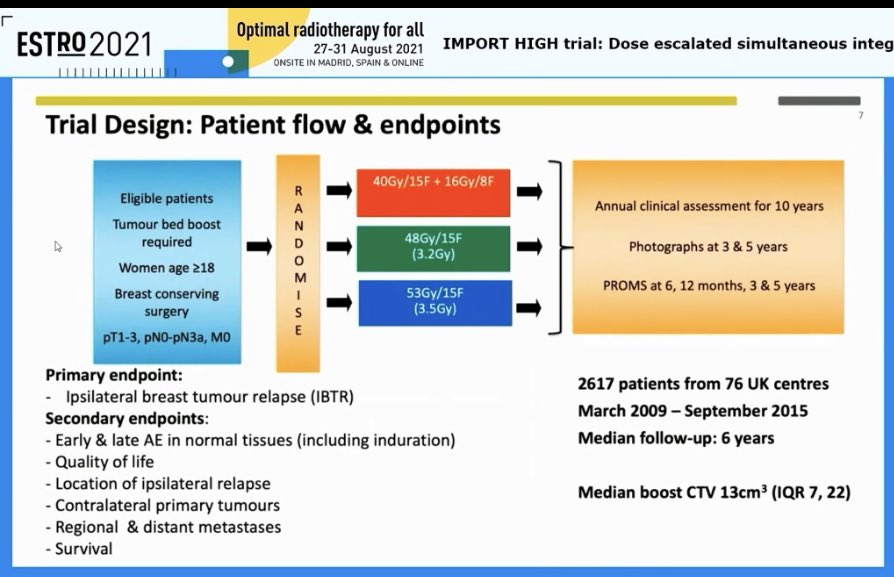
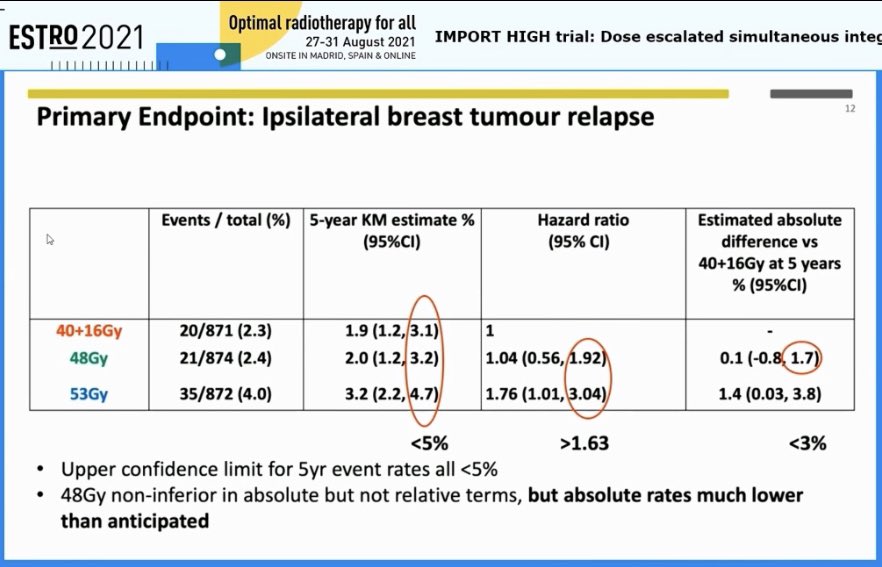

English




