
Matthew Stachler
22 posts

Matthew Stachler
@MatthewStachler
Molecular Pathologist and Researcher of pre-malignant gastrointestinal diseases








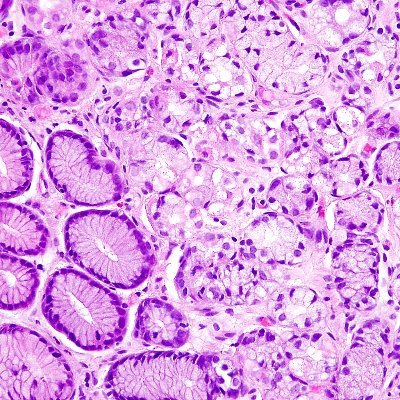





#GIPathJC Abnormal p53 immunohistochemistry status was found to predict progression regardless of histologic diagnosis (figure)







#GIPathJC Abnormal p53 staining was considered when 2 to 3+ nuclear positivity was present in >50% of cells in at least one crypt base or glandular profile, or in a contiguous focus of at least 20 surface epithelial cells






Happy Thanksgiving tomorrow ! - Tune in #GIPathJC next week Wednesday December 1 at 8:30 pm EST to join - @GIPathJC is also inviting questions for discussion by message at @GIPathJC -Guest expert @MatthewStachler of @UCSF @AGA_Gastro -Article link pubmed.ncbi.nlm.nih.gov/34757142/?s=09
