Sabitlenmiş Tweet

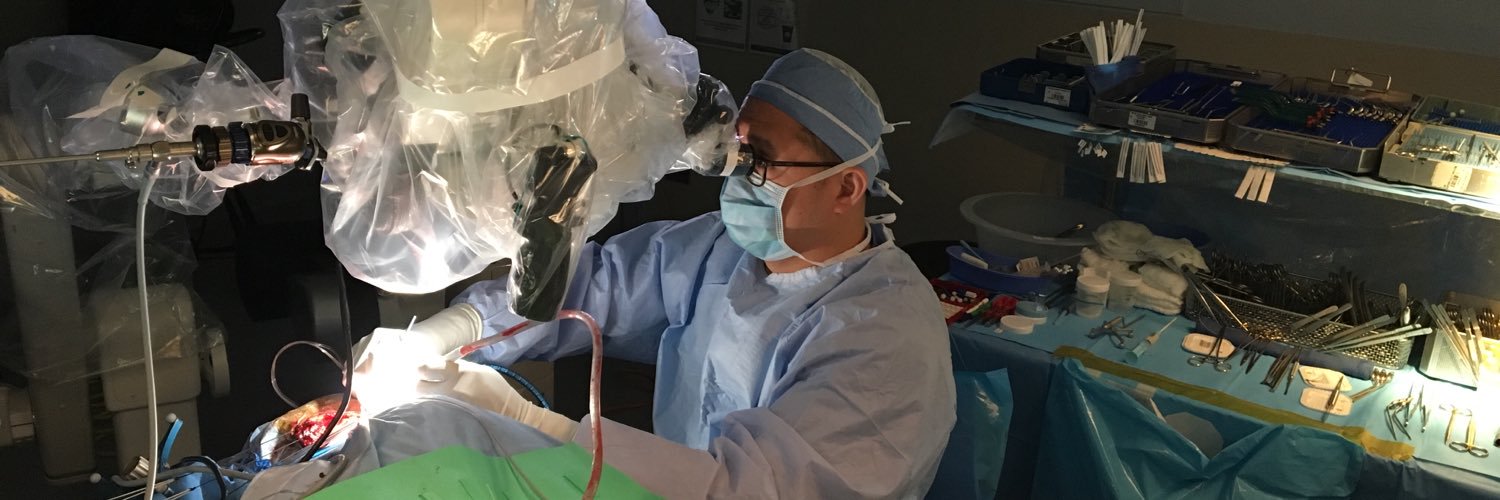
Clipping of giant ophthalmic and A1 lenticulostriate artery #aneurysms using suction decompression Dallas technique #OpVid @RUNeurosurgery @SaintBarnabasNJ @RWJBarnabas @NASBSorg @ASCsurgical @BAFOUND @ASAHStudy_Aust @joseph_quillin @CNS_Update @cvsection @AANSNeuro
Millburn, NJ 🇺🇸 English