Dr. Ambily K
872 posts


@drambilyk
MBBS MD DM. Consultant nephrologist, AIMS Thrissur. @glomcon fellow 2022-23. @KidneyKolumns EB member 2024-25. @winicon2024 #SoMe team.











🚨 Cardio pearls you should never miss 5️⃣ 1️⃣ Confused whether it’s VT or wide-complex SVT? Before jumping to algorithms, remember this: Some ECG findings are exclusively seen in Ventricular Tachycardia. If you spot them the debate ends.👇 2️⃣ 🔴 Features classically seen in VT (not in SVT with aberrancy): • AV dissociation • Capture beats • Fusion beats • VA Wenckebach • 2:1 VA block • Markedly wide QRS (>160 ms) Now let’s understand why. 3️⃣ 🔵 AV Dissociation In VT: Ventricles are the primary pacemaker. Atria continue under sinus control. → P waves and QRS march independently. In SVT with aberrancy: Atria are part of the circuit or activated 1:1. → No independent atrial rhythm. True AV dissociation does not occur. 4️⃣ 🔵 Capture Beat In VT: A sinus impulse occasionally conducts through the AV node and “captures” the ventricles → produces a relatively narrow QRS. This is only possible if ventricles are depolarizing independently. In SVT: Ventricles are already activated via the His-Purkinje system. There’s nothing to “capture.” 5️⃣🔵 Fusion Beat In VT: A sinus impulse and ventricular impulse occur simultaneously. Two wavefronts collide. → Hybrid QRS morphology. Requires AV dissociation. In SVT: There is only one antegrade wavefront via AV node. Fusion cannot physiologically occur. 6️⃣ 🔵 VA Wenckebach In VT: Retrograde conduction from ventricle → atrium may progressively delay → then drop. This produces VA Wenckebach. This proves ventricles are driving the rhythm. In SVT: Atria are essential to the circuit. You cannot have progressive VA block like this. 7️⃣ 🔵 2:1 VA Block In VT: Only every second ventricular impulse conducts retrogradely to atria. Again ventricles are independent. In SVT: Atrial activation precedes ventricular activation. You won’t see isolated ventricular-to-atrial block patterns. 8️⃣ 🔵 Markedly wide QRS (>160 ms) VT originates in myocardium. Depolarization spreads cell-to-cell → slow conduction → very wide complex. SVT with aberrancy still uses part of the His-Purkinje system. QRS is wide but usually not extremely wide. 9️⃣ 🔴 Common Pitfalls in WCT Diagnosis • “Patient is stable → must be SVT.” • “Young age → unlikely VT.” • “Looks like typical BBB.” • Giving AV nodal blockers before being sure. Hemodynamic stability does NOT rule out VT. When in doubt → treat as VT. 🔟 If you see capture beats, fusion beats, or AV dissociation you are not dealing with SVT. Electrophysiology makes it clear. #MedTwitter #MedX #Cardiology


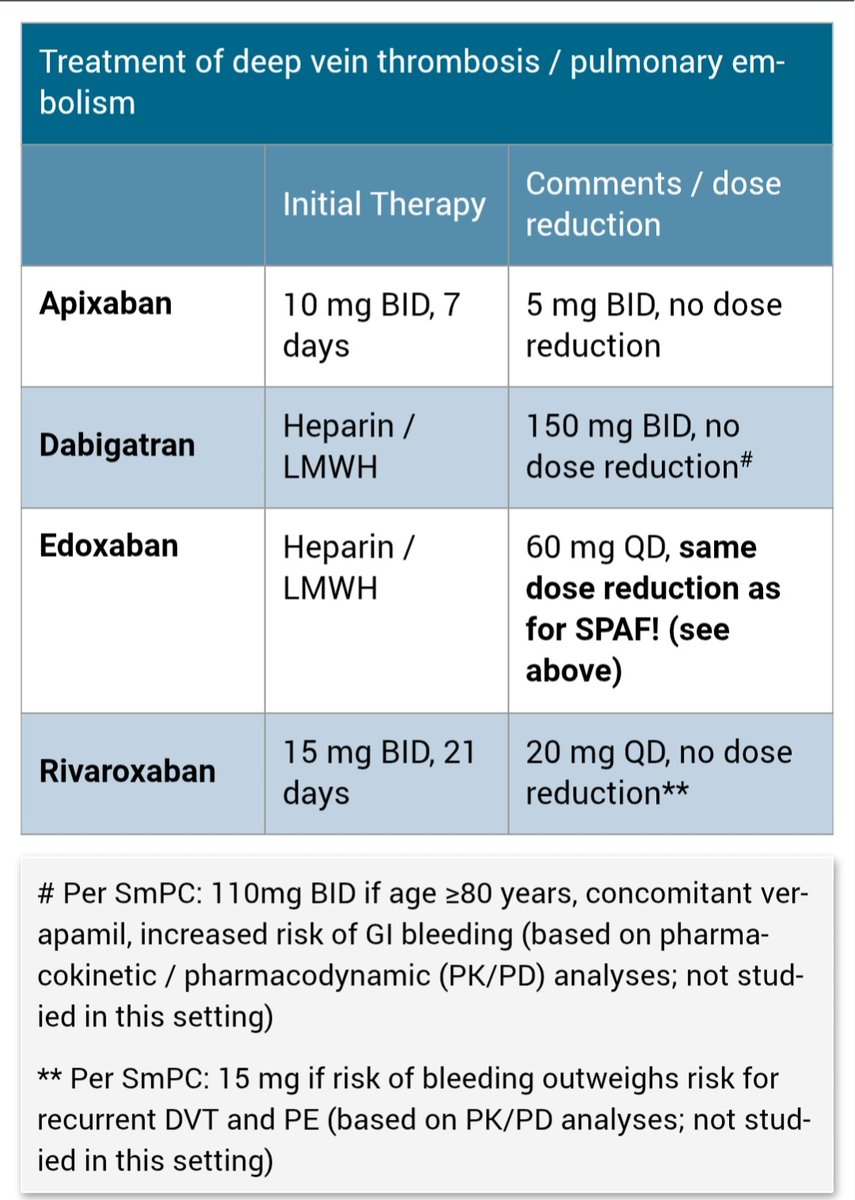
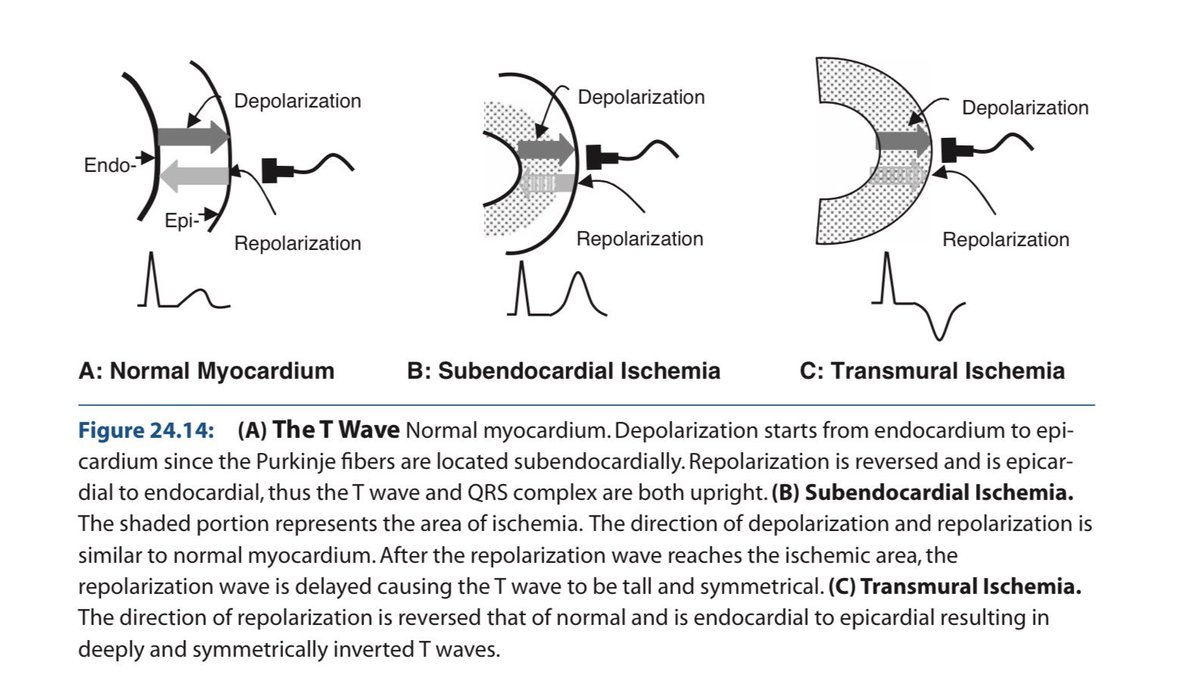
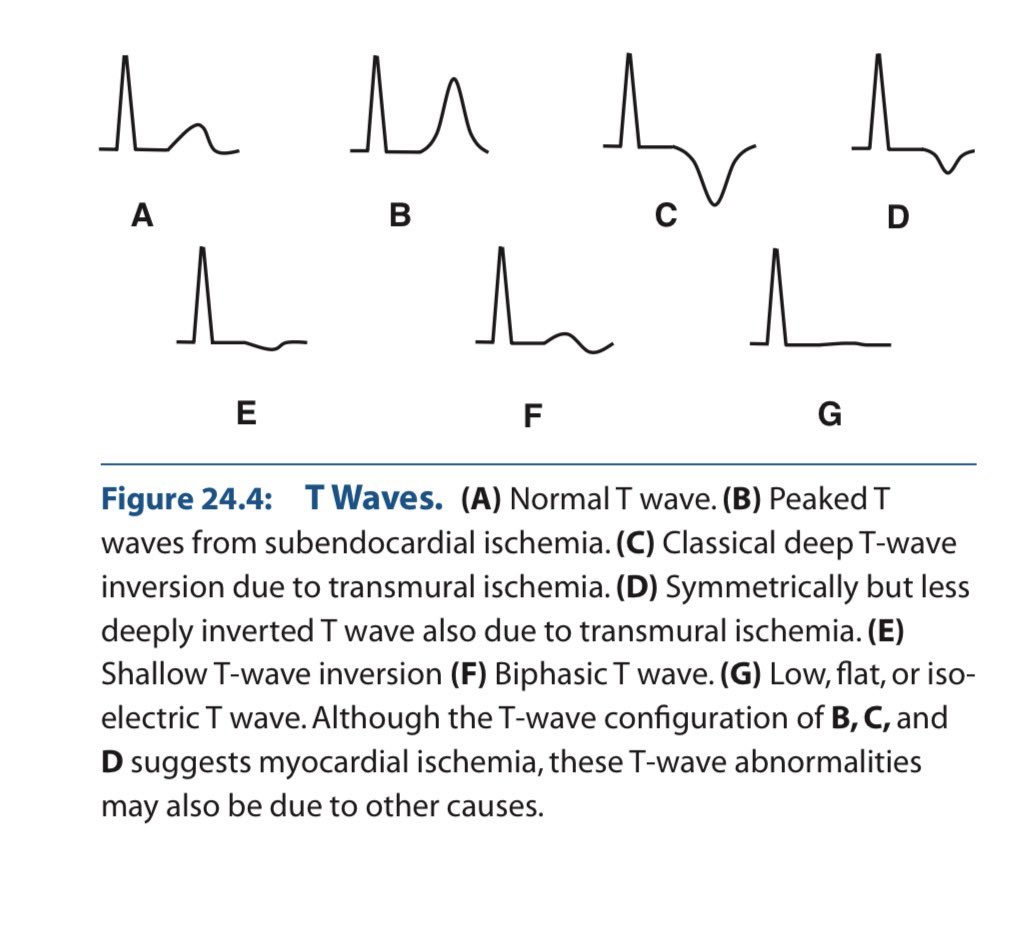
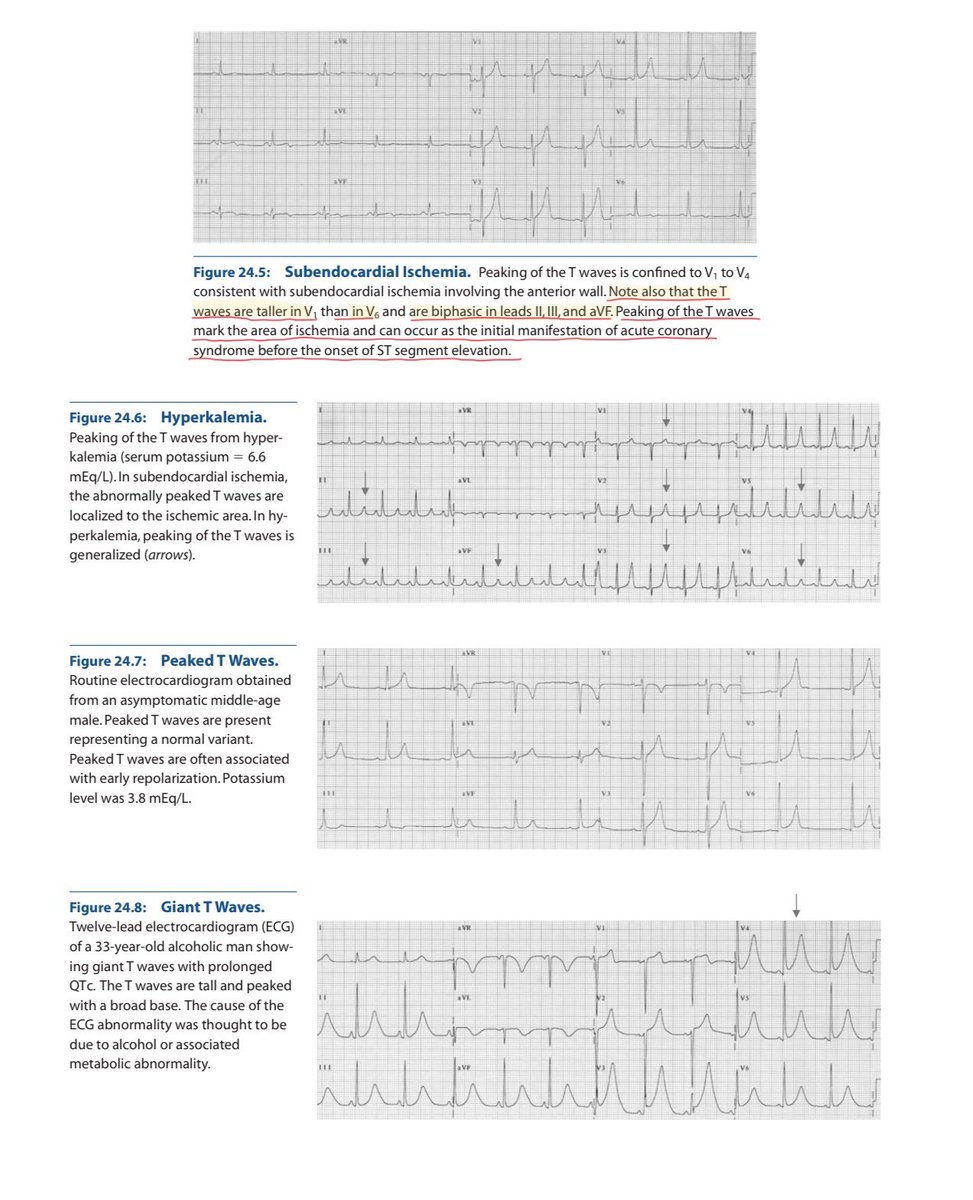
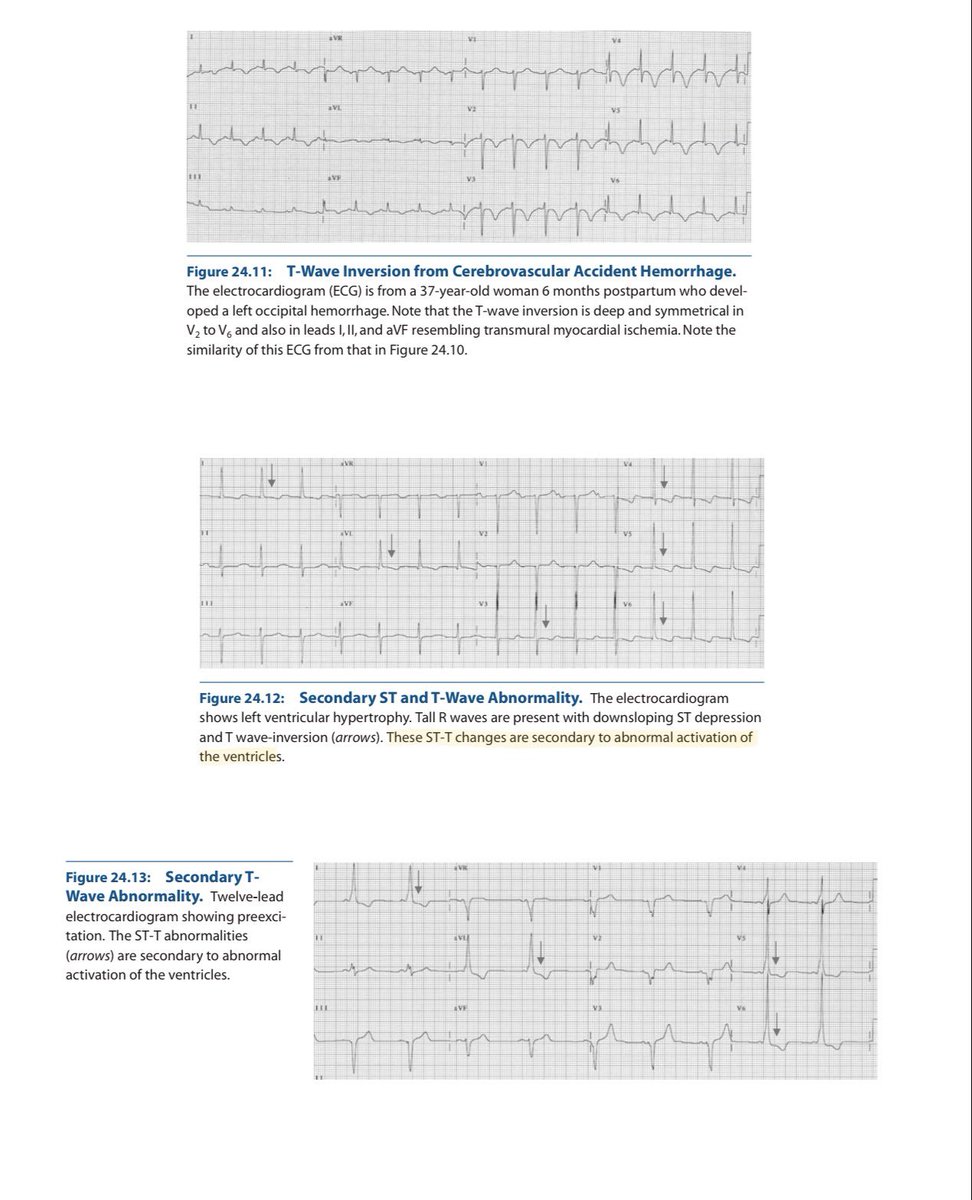
🚨 Cardio pearls you should never miss 6️⃣ The T wave in the ECG is a story about repolarisation not a random squiggle. When it inverts, something changed in the direction or timing of ventricular recovery. Let’s clear the confusion once for all & understand in depth. 1️⃣ Why is the normal T wave upright? ✔ Purkinje fibers are subendocardial in location. So: Depolarization → Endocardium → Epicardium Repolarization → Epicardium → Endocardium Epicardial cells: 🔻Shorter action potential duration 🔻Larger transient outward K⁺ current (Ito) 🔻Faster phase 3 repolarization Repolarization is a negative wave moving opposite depolarization → vector aligns with QRS. 👉 Upright T wave. 2️⃣ Subendocardial ischemia (early) Inner myocardium + Purkinje network suffer first. Ischemia causes: 🔻ATP depletion 🔻KATP channel opening 🔻Extracellular K⁺ accumulation 🔻Shortened action potential in ischemic zone 🔻Slowed Purkinje conduction ECG: → Tall, symmetric, broad-based T waves (Hyperacute phase) 3️⃣ Transmural ischemia Repolarization sequence reverses abnormally. Vector flips. → Deep, symmetric T-wave inversion Seen in: 🔻Evolving MI 🔻Wellens pattern 🔻Reperfusion Deep + symmetric + territorial + dynamic = ischemia until proven otherwise. 4️⃣ Hyperkalemia Global extracellular K⁺ elevation. ECG: 🔻Narrow, tented T waves 🔻Short QT Sharp, narrow spikes ≠ broad ischemic T waves. 5️⃣ Hypokalemia Delayed repolarization. ECG: 🔻Flat T waves 🔻ST depression 🔻Prominent U waves U waves help differentiate from ischemia. 6️⃣ CNS / Neurogenic T waves Catecholamine surge → myocardial stunning. ECG: 🔻Deep, diffuse T inversions 🔻QT prolongation 🔻Not vascular territory specific Distribution matters. 7️⃣ LVH & Strain Pattern This is not primary ischemia. It’s repolarization abnormality secondary to abnormal depolarization. In LVH: 🔻Increased myocardial mass 🔻Prolonged depolarization 🔻Delayed repolarization in hypertrophied wall ECG: ✔ High-voltage QRS ✔ Downsloping ST depression ✔ Asymmetric T-wave inversion (Usually lateral leads: I, aVL, V5–V6) Key point: Strain T waves are asymmetric, gradual downstroke + rapid return. Ischemic T waves are symmetric. 8️⃣ Cardiomyopathies Hypertrophic cardiomyopathy (HCM) 🔻Deep T inversions (often in precordial leads) 🔻May mimic ischemia 🔻Often associated with large voltages Apical HCM 🔻Giant negative T waves in precordial leads Dilated cardiomyopathy 🔻Nonspecific ST-T changes 🔻Often diffuse Mechanism: Structural remodeling alters repolarization gradients. Not vascular. Not dynamic like ACS. 9️⃣ Final Differentiation Framework ✔ Symmetric + territorial + dynamic → Ischemia ✔ Narrow tented + short QT → Hyperkalemia ✔ Flat T + U waves → Hypokalemia ✔ Diffuse deep T + long QT + neuro event → CNS ✔ High voltage + asymmetric lateral T inversion → LVH strain ✔ Giant precordial inversions + echo changes → HCM ✔ Stable V1–V3 inversion in young → Benign variant T waves reflect: • Repolarization timing • Potassium currents • Myocardial thickness • Conduction sequence • Autonomic tone If you understand vectors + ionic physiology, the ECG becomes logical. Electrophysiology > memorized patterns. (Ref: Marriott’s Practical Electrocardiography; Surawicz & Knilans) #MedTwitter #MedX #ECG #Cardiology