
Giacomo Maria Cioffi 🇨🇭🇮🇹🇨🇦
433 posts


Giacomo Maria Cioffi 🇨🇭🇮🇹🇨🇦
@gmcioffi
Interventional Cardiology Consultant • Former @McMasterU Fellow • OCT, IVUS, CHIP and CTO enthusiast


Among patients with atrial fibrillation at high risk for stroke and bleeding, left atrial appendage closure was not noninferior to medical therapy in reducing the risk of stroke, embolism, major bleeding, or death at 3 years. Full CLOSURE-AF trial results: nejm.org/doi/full/10.10… Editorial: Left Atrial Appendage Closure — Another Overused Method in Cardiology? nejm.org/doi/full/10.10…



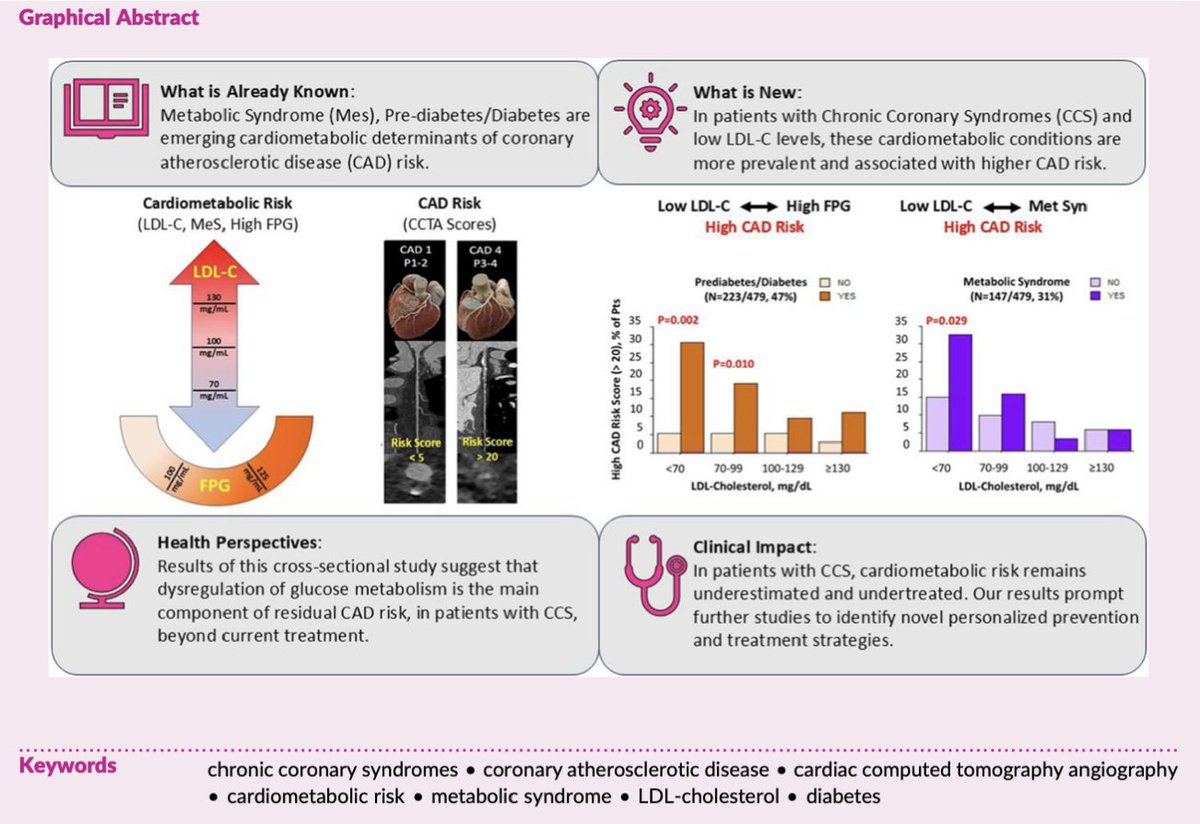













PROCTOR RCT in prior-CABG: when both strategies were feasible, SVG PCI had lower 1-yr MACE than native-vessel PCI (18.7% vs 34.3%) with less target-territory MI and revasc; similar mortality. Findings challenge “native-first” guidance, long-term data awaited. #TCT2025

This is very very problematic. Will be reviewing formally. Problems range from design/concept issues to statistical issues.

Today, FDA provided important updates on the risk of myocarditis after receiving an mRNA COVID-19 vaccine, noting the risk is higher in young men.











