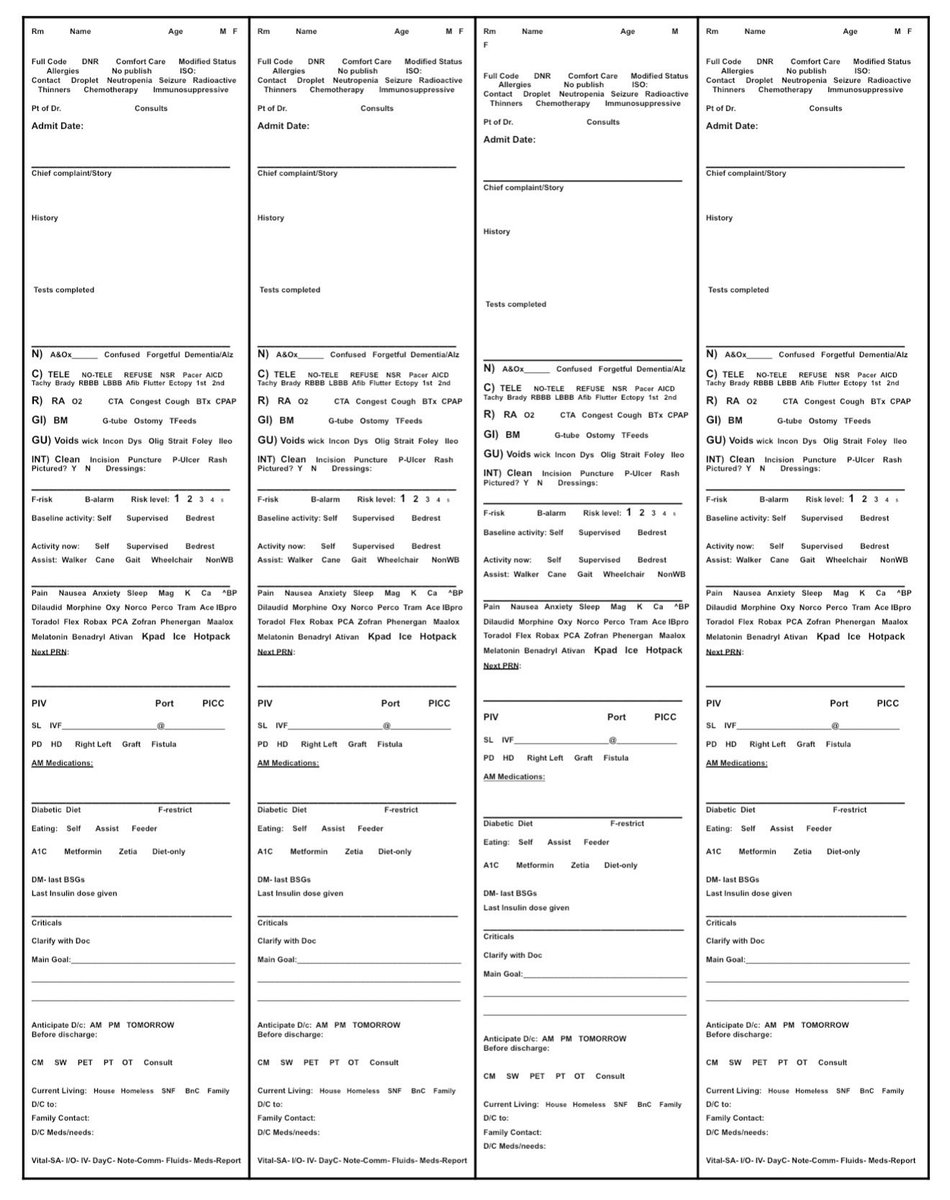
✅ 3 Tips for Writing Better SOAP Notes 📝
(from this Nurse who’s written/read thousands of them)
👍Most notes can be way better.
Here’s how 👇
Tip 1: Tell a clean chronological story 📖
❌Don’t jump around! Patients rarely tell their story in order — it’s your job to organize it.
•Start from when they felt normal → what happened → ER arrival ⏰
•Weave pertinent positives/negatives right after new info (no dumping at the end!)
•Delete “of note” — it’s a red flag you’re out of sequence ❌
This one change makes your note 10x clearer.
💪Students: it shows attendings you’re thinking through differentials 🧠
Tip 2: Know your audience 👥
Your note has 3 key readers:
1Other providers 🩺
✅Crisp HPI + easy A/P: short bullets (3-5 max), actual dates (no “tomorrow” or “POD#2”)
2Social Work & Case Management 🤝
✅Always include estimated discharge date + disposition. They’ll love you and patients will move faster ⚡
3The business side 💼 (coders, insurance, compliance, lawyers)
✅Document smartly so you get paid and stay protected. Use your CDI team!
Tip 3: Be succinct ✂️
This isn’t a novel.
Post-residency, no one wants walls of text or 15 differentials.
Keep it skimmable.
Communication > showing off 📉
✅Summary:
•Tip 1: Chronological story 📖
•Tip 2: Write for your audience 👥
•Tip 3: Be succinct ✂️
Better notes = better care, better billing, happier team ❤️
Who has strong note-writing hacks? Drop them below 👇

English