Ernest Spitzer
225 posts


Ernest Spitzer
@spitzertweets
#cardiology #clinicaltrials #leadership #innovation #evolution #thefutureisnow #warpjump (opinions are personal)






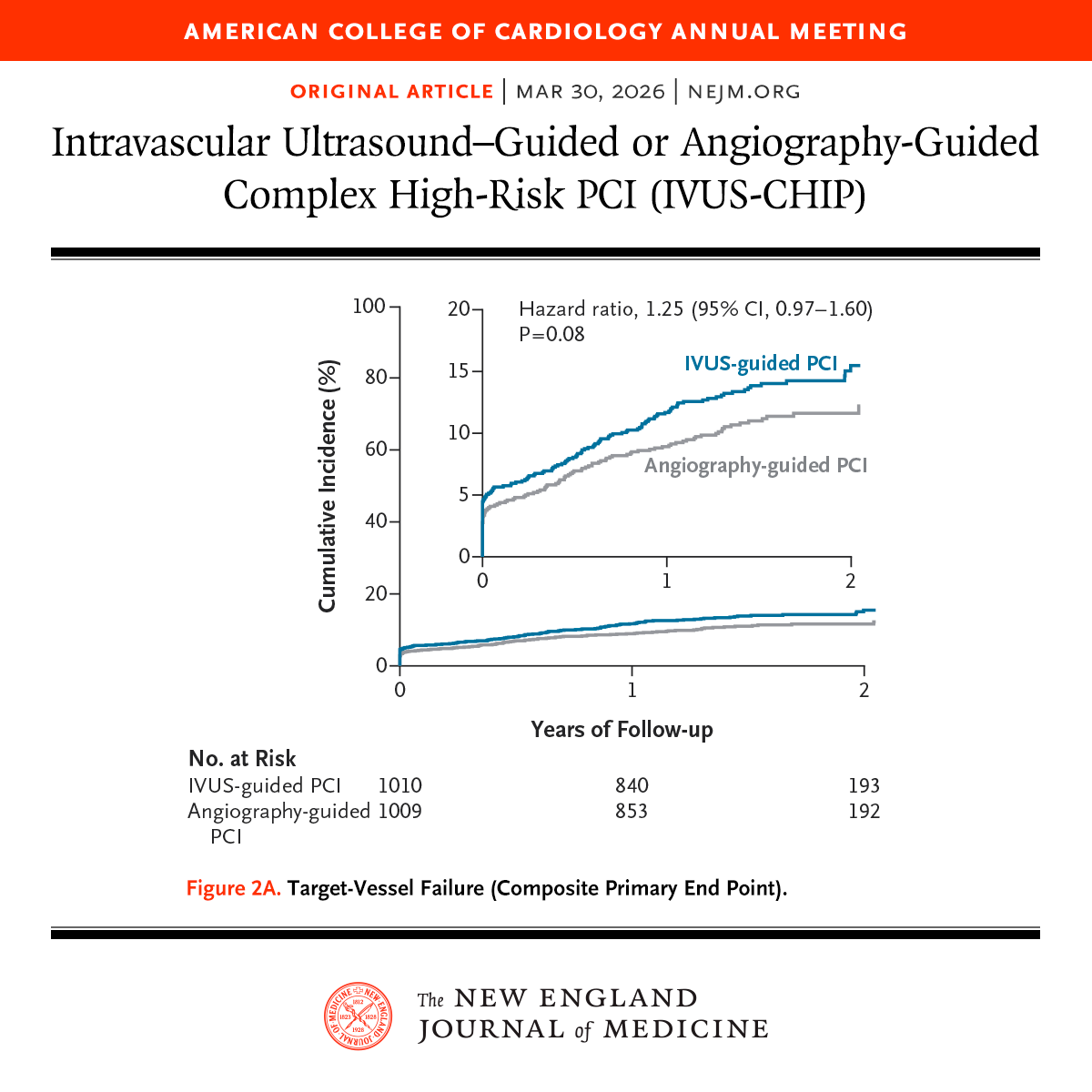
Presented at #ACC26: In the IVUS-CHIP trial involving patients undergoing complex high-risk PCI, the risk of target-vessel failure (a composite outcome) was not lower with intravascular ultrasound guidance than with angiography guidance. Full trial results: nejm.org/doi/full/10.10… Editorial: IVUS — A Zigzag Path to Success nejm.org/doi/full/10.10… @ACCinTouch










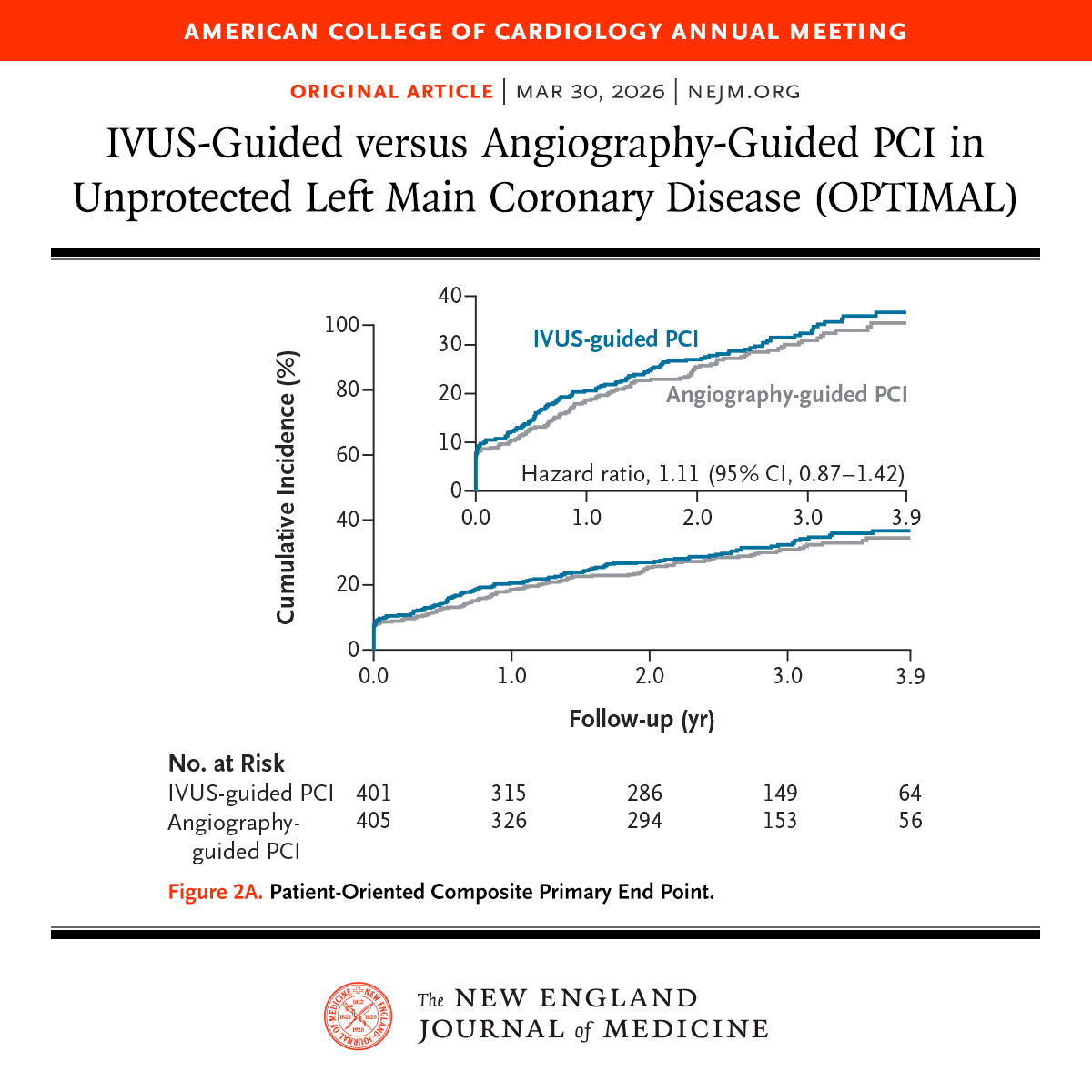
Presented at #ACC26: Among patients with unprotected left main coronary artery disease, intravascular ultrasonography–guided PCI did not result in a lower risk of ischemic events or death than angiography-guided PCI. Full OPTIMAL trial results: nejm.org/doi/full/10.10… Editorial: Seeing the Left Main Coronary Artery Clearly — Is IVUS Always Necessary? nejm.org/doi/full/10.10… @ACCinTouch


Presented at #ACC26: In the IVUS-CHIP trial involving patients undergoing complex high-risk PCI, the risk of target-vessel failure (a composite outcome) was not lower with intravascular ultrasound guidance than with angiography guidance. Full trial results: nejm.org/doi/full/10.10… Editorial: IVUS — A Zigzag Path to Success nejm.org/doi/full/10.10… @ACCinTouch






Presented at #ACC26: Among patients with unprotected left main coronary artery disease, intravascular ultrasonography–guided PCI did not result in a lower risk of ischemic events or death than angiography-guided PCI. Full OPTIMAL trial results: nejm.org/doi/full/10.10… Editorial: Seeing the Left Main Coronary Artery Clearly — Is IVUS Always Necessary? nejm.org/doi/full/10.10… @ACCinTouch