Sabitlenmiş Tweet
VictorHugoG.Johnson
5.5K posts


VictorHugoG.Johnson
@vikouerMD
Attending Nephrologist @NefrologiaINC | Cardiorenal @geshNHS | Critical Care Nephrology @UAB_NRTC | POCUS | Music Lover | Calisthenics
Muddy Banks Of The Wishkah Katılım Aralık 2009
440 Takip Edilen819 Takipçiler
VictorHugoG.Johnson retweetledi

Diuretic Resistance Risk and the Efficacy of Natriuresis-Guided Diuretic Therapy in Acute Heart Failure: Post Hoc Analysis From the PUSH-AHF Trial | JACC: Heart Failure jacc.org/doi/10.1016/j.…

English
VictorHugoG.Johnson retweetledi

🫀The failing right ventricle:
the most misunderstood chamber in critical care
For years, we focused on the left ventricle.
But in the ICU, the real killer is often the right ventricle.
->What is acute RV failure?
👉 Not just “weak contraction”
It’s a hemodynamic collapse syndrome:
RV dilation
↓ LV preload
↓ cardiac output
↑ venous congestion
➡️ → multi-organ failure
->The key pathophysiology (the vicious cycle)
1. ↑ Afterload (PE, ARDS, PH)
2. → RV dilation
3. → Septal shift → LV underfilling
4. → ↓ CO → hypotension
5. → ↓ RCA perfusion
6. → RV ischemia
👉 And the cycle accelerates
->The most important concept
👉 The RV does NOT tolerate pressure
Handles preload very well
Fails rapidly with afterload
➡️ Even small ↑ PVR → collapse
->Main causes you MUST think first
🔴 Pulmonary embolism
🔴 RV myocardial infarction
🔴 ARDS / mechanical ventilation
🔴 Decompensated pulmonary hypertension
🔴 Post-cardiac surgery
->Diagnosis is NOT obvious
There is no single sign.
👉 It requires suspicion + integration:
Clinical: congestion + hypoperfusion
ECG + biomarkers
POCUS (your best friend 🤓)
Hemodynamics
->Echo mindset (fast ICU approach)
👉 Don’t overcomplicate
Look for:
✔ RV dilation
✔ Septal shift (D-sign)
✔ TAPSE ↓
✔ Venous congestion
The real ICU mistake
❌ Treating RV failure like LV failure
->Management principles
👉 Think in 4 pillars:
1. Preload — “not too much, not too little”
Hypovolemic → small fluid
Congested → REMOVE fluid
👉 CVP is not a target, it’s a warning
2. Afterload, THE key target
✔ Treat PE
✔ Optimize ventilation
✔ Reduce PVR
👉 If afterload stays high → RV will fail
3. Contractility
Dobutamine
Milrinone
Levosimendan
👉 Choose based on context
4. Perfusion pressure
👉 Norepinephrine is your anchor
✔ Maintains coronary perfusion
✔ Supports RV function
->Ventilation: the silent killer
⚠️ Positive pressure = ↑ PVR
👉 Over-ventilate → worsen RV failure
->When nothing works
👉 Think early:
VA-ECMO
RV assist devices
🤓Key insight
This is NOT just a cardiac problem.
👉 It is a ventriculo–arterial coupling failure
When:
Ees / Ea ↓ → RV collapses
🤓Bottom line
✔ RV failure is preload dependent BUT afterload sensitive
✔ Small mistakes → rapid collapse
✔ Early recognition + physiology-based treatment saves lives
->Clinical mindset
👉 Don’t ask:
“Is the RV failing?”
👉 Ask:
“Why is the RV failing and, what is driving the afterload?”
📃Reference
Giannakoulas G. et al. European Heart Journal (2025) 00, 1–16 doi.org/10.1093/eurhea…

English
VictorHugoG.Johnson retweetledi

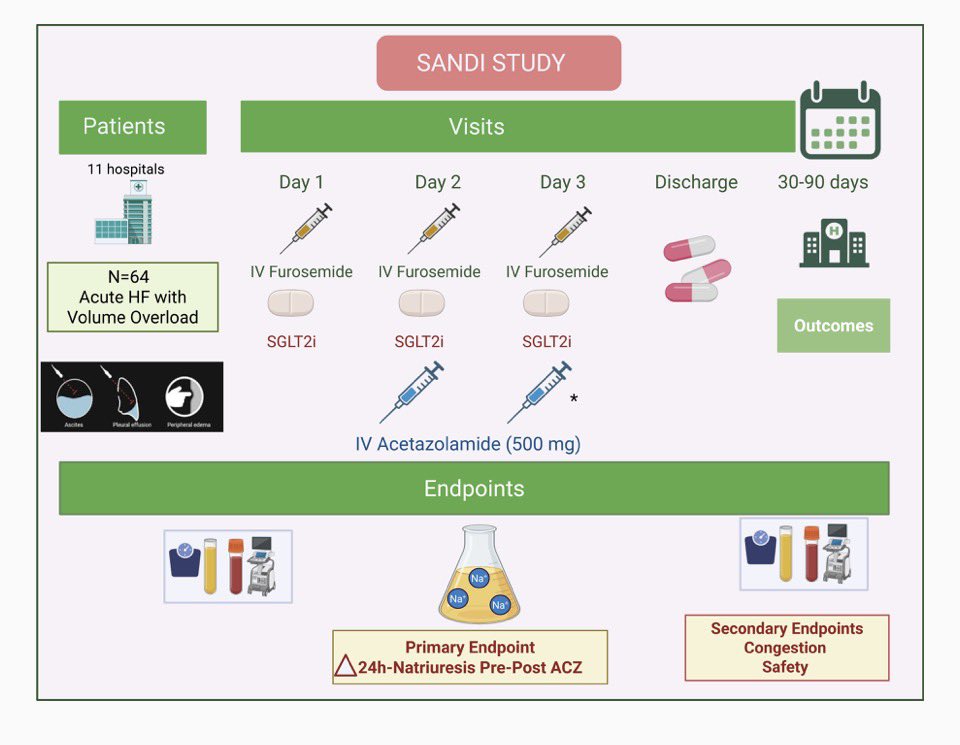
The SANDI study will determine whether adding acetazolamide to intravenous furosemide and SGLT2i enhances early natriuresis and diuresis in patients with AHF and persistent congestion
Lead by @MartaCoboMarcos
academic.oup.com/eschf/article/…
English
VictorHugoG.Johnson retweetledi

Dapagliflozin is not dialyzable and does not accumulate significantly in dialysis patients—supporting biological plausibility for safe use.
CME INDIA Clinical Pearls: SGLT2 Inhibitors in Dialysis (HD & PD)
▪️Evidence Gap Alert:
While SGLT2 inhibitors robustly reduce CKD progression, CV events, and mortality in non-dialysis CKD, patients on dialysis (HD/PD) were excluded from all landmark RCTs, creating a major evidence void.
▪️Mechanistic Shift in ESKD:
In dialysis patients, classical glucosuric/tubular effects are minimal due to low nephron mass; benefits are likely mediated via cardio-metabolic off-target pathways (↓ inflammation, ↓ oxidative stress, improved myocardial energetics).
▪️Pharmacokinetic Reassurance: Dapagliflozin is not dialyzable and does not accumulate significantly in dialysis patients—supporting biological plausibility for safe use.
▪️Signal from Early Data:
Small trials and observational cohorts suggest potential CV benefit, improved volume status, and preservation of residual kidney function, particularly in incremental dialysis—without major safety signals.
▪️Peritoneal Dialysis Uncertainty:
In PD, evidence is sparse and inconsistent—some studies show ↑ ultrafiltration and ↓ BP, while others show no effect on peritoneal glucose transport.
▪️Real-World Cohort Insight:
Retrospective analyses indicate lower CV events and mortality in dialysis patients using SGLT2i, but these are hypothesis-generating, not definitive.
▪️Safety Perspective:
No major red flags so far, but risk of volume depletion, hypotension, and rare euglycemic ketoacidosis warrants cautious patient selection.
▪️Clinical Position Today:
Routine use in dialysis cannot be recommended yet; use should be individualized and preferably within research settings or expert supervision.
▪️Future Direction:
Ongoing large RCTs are critical to define efficacy, safety, and patient selection—this could expand SGLT2i use into ESKD therapeutics beyond glycemia.
💢Take-Home Message:
👉 SGLT2 inhibitors in dialysis represent a promising but unproven frontier—mechanistically attractive, observationally encouraging, but awaiting definitive trial evidence before mainstream adoption.
academic.oup.com/ckj/article/19…


English
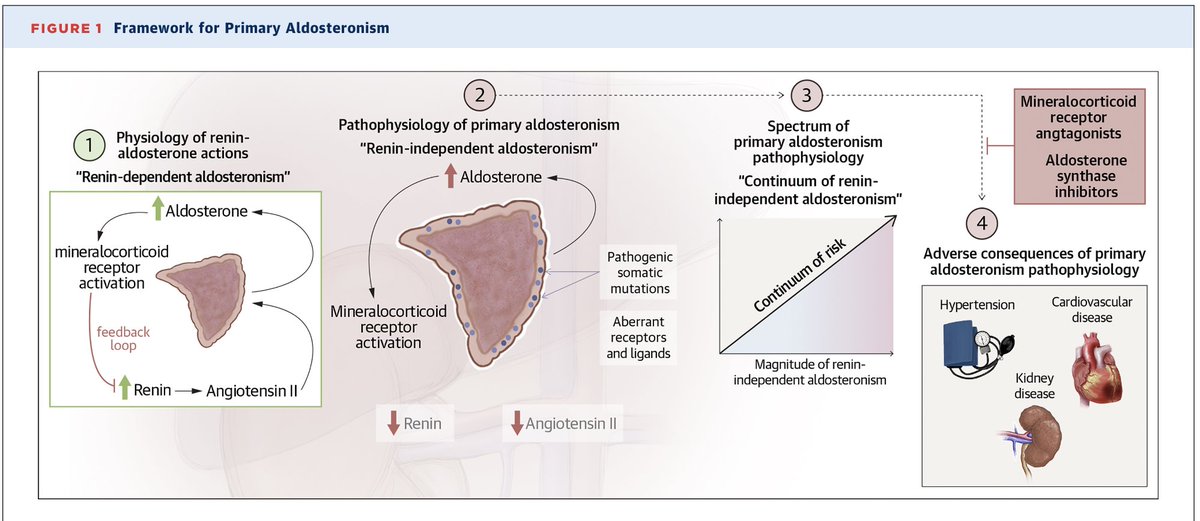
VictorHugoG.Johnson retweetledi

When eGFR drops after initiating treatment with empagliflozin or finerenone, we often stop these treatments. This is less likely to happen when eGFR is already low. The initial eGFR drop associates w/ diuretic use. Back off on the diuretics, not the disease modifying therapies.
Edgar V. Lerma 🇵🇭@edgarvlermamd
Acute eGFR Changes and Their Mediation of Albuminuria Reduction with Empagliflozin and Finerenone ca. 2026 from @asnpublications @AgarwalRajivMD @HeerspinkHiddo @mvaduganathan @P_Rossing @sankarnava #ISNWCN 🇯🇵 #WCN26 🇯🇵 #WCN2026 🇯🇵 #Nephpearls 👉 journals.lww.com/jasn/fulltext/…
English
VictorHugoG.Johnson retweetledi
VictorHugoG.Johnson retweetledi

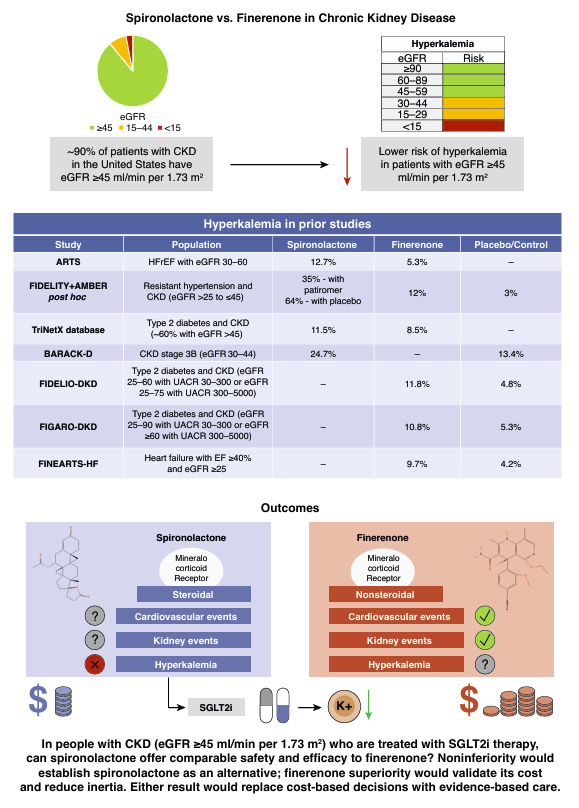
Steroidal MRAs may offer a more cost-effective treatment option for CKD. Learn why in this #ASNJASN #Perspective. kidney.pub/JASN1052
English
VictorHugoG.Johnson retweetledi

Is There a Role for Pentoxifylline in Diabetic Kidney Disease?
bit.ly/4rSpkru
@AgarwalRajivMD

English
VictorHugoG.Johnson retweetledi

The KDIGO 2026 Diabetes and CKD Guideline draft is available for public review through April 13, 2026.
You can download the guideline draft and submit comments via the feedback form on the guideline website: kdigo.org/guidelines/dia…
This update incorporates significant clinical and scientific developments that have emerged since the KDIGO 2022 Diabetes Guideline. It is specifically focused on three main areas: a new Chapter 1 covering definitions, prevention, and risk assessment, Chapter 2 related to glycemic monitoring, and Chapter 4 addressing comprehensive pharmacotherapy.
Reviewers may comment on any section of the draft, and contributors may be acknowledged in the final publication. All feedback is welcome and appreciated.

English
VictorHugoG.Johnson retweetledi

🚨En el síndrome cardiorrenal agudo la resistencia a diuréticos es frecuente; en casos refractarios, la ultrafiltración (extracorpórea o peritoneal) mejora retiro de volumen y diuresis.
🌊La diálisis peritoneal ofrece ventajas hemodinámicas, extracción de sodio y no requiere anticoagulación.
Gran trabajo de @laurazamoracerv
doi.org/10.3390/life16…
pmc.ncbi.nlm.nih.gov/articles/PMC12…
Español
VictorHugoG.Johnson retweetledi

WRF (GFR decline) in the CLOROTIC trial is not related with worse outcomes @NDTsocial
Great work lead by Wendy Mc Callum from @TuftsMedicalCtr
Acute declines in kidney function with thiazide plus loop diuretics vs loop diuretics alone in ADHF academic.oup.com/ndt/article-ab…

English
VictorHugoG.Johnson retweetledi

🆕 Cuando la descompresión no es igual para todos: lecciones hemodinámicas del RELIEVE-HF
Paulo Fernando García Chumbiray @PauloGCh1
Lee el análisis completo y descubre qué nos enseña realmente RELIEVE-HF sobre la selección de pacientes: cardioteca.com/insuficiencia-…
🔎 RELIEVE-HF fue un ensayo aleatorizado, doble ciego y con procedimiento simulado en 508 pacientes con IC sintomática; en el análisis global, el resultado fue neutro a 2 años.
❤️ En FE ≤40%, el shunt interauricular redujo eventos, especialmente hospitalizaciones por insuficiencia cardiaca, con separación progresiva de curvas.
⚠️ En FE >40%, se asoció a más eventos cardiovasculares e incluso mayor mortalidad, con interacción estadísticamente significativa.
🫀 La misma intervención estructural no tiene el mismo efecto en todos: la fisiología biventricular y el fenotipo ventricular son claves para decidir a quién puede beneficiar y a quién perjudicar.
Español
VictorHugoG.Johnson retweetledi

🚨 Just published! We validated an ultrasound-based score combining VExUS + LUS to guide decongestion in acute heart failure. A step forward toward more precise, ultrasound-driven management. Proud of our team! Congrats Henrique!
onlinelibrary.wiley.com/doi/epdf/10.10…

English
VictorHugoG.Johnson retweetledi

New editorial! 🚨
No Heart Failure Patient Left Behind: Making GDMT a Reality for All @JCardFail @TradIMYale @YaleCardiology
onlinejcf.com/article/S1071-…
English
VictorHugoG.Johnson retweetledi

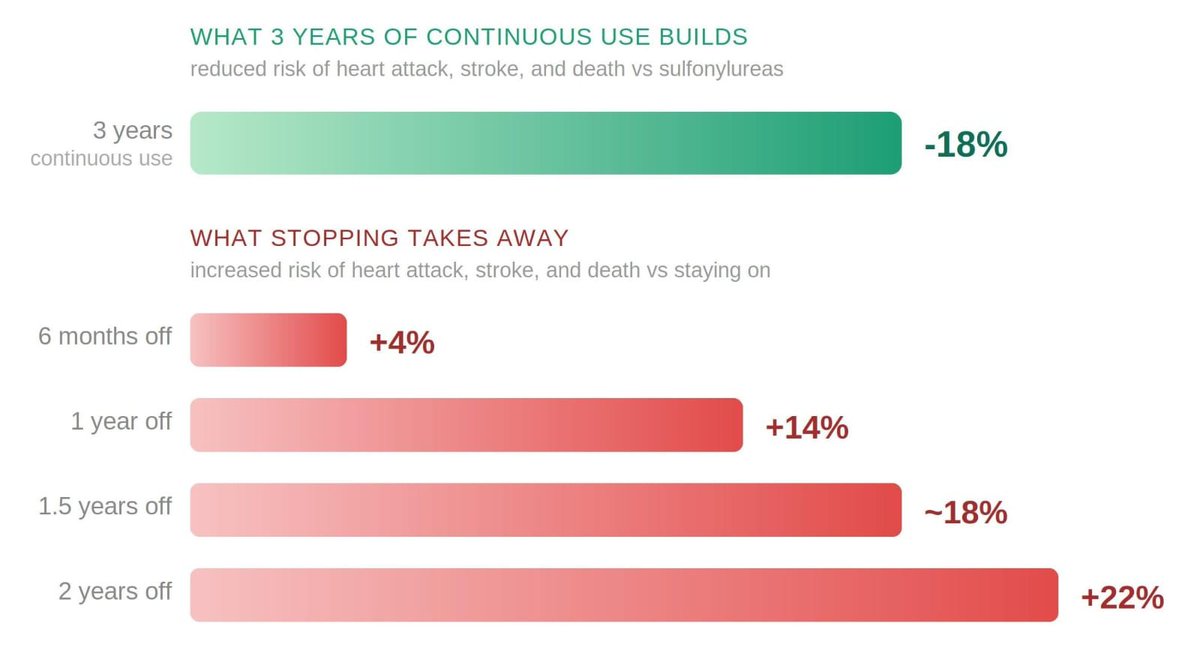
GLP-1 RA Discontinuation & Risks of Major Adverse CV Events
1️⃣ Stopping For 6 Months: 4% Increased Risk
2️⃣ Stopping For 1 Year: 14% Increased Risk
3️⃣ Stopping For 2 Years: 22% Increased Risk
bmjmedicine.bmj.com/content/5/1/e0…
@DrNadolsky @DrKarlNadolsky @NutritionMadeS3 @drmatthewnagra @BevTchangMD @MichaelAlbertMD
English
VictorHugoG.Johnson retweetledi

Efficacy and Tolerability of Sodium Zirconium Cyclosilicate or Patiromer in Managing Hyperkalemia
A Systematic Review and Meta-Analysis
Both SZC and patiromer effectively lower serum potassium and provide clinical benefits, with distinct safety considerations.
#Cardiology #MedTwitter #CardioTwitter #HeartHealth #Healthcare
@CMichaelGibson @DrMarthaGulati @hvanspall @ShelleyZieroth @AndrewJSauer @goKDIGO @safchat @Hragy @biljana_parapid
journals.lww.com/kidney360/abst…
English
VictorHugoG.Johnson retweetledi

Heart & kidney disease are closely linked, as individuals with chronic kidney disease (CKD) face a significantly higher risk of CV events & HF. In this #ACCEL Lite 🎙️, experts examine “Cardiovascular-Kidney Therapies in CKD”. ➡️ bit.ly/4bAfdBN
@RangaswJ @TaylorMHVIcard
English
VictorHugoG.Johnson retweetledi

Delighted that FIND CKD has meet its primary endpoint. Fantastic news for patients with non-diabetic CKD, including those with GNs, including IgAN
Thank you to Bayer, all the investigators, study teams & patients who have made FIND-CKD possible
bayer.com/media/en-us/fi…

English
VictorHugoG.Johnson retweetledi

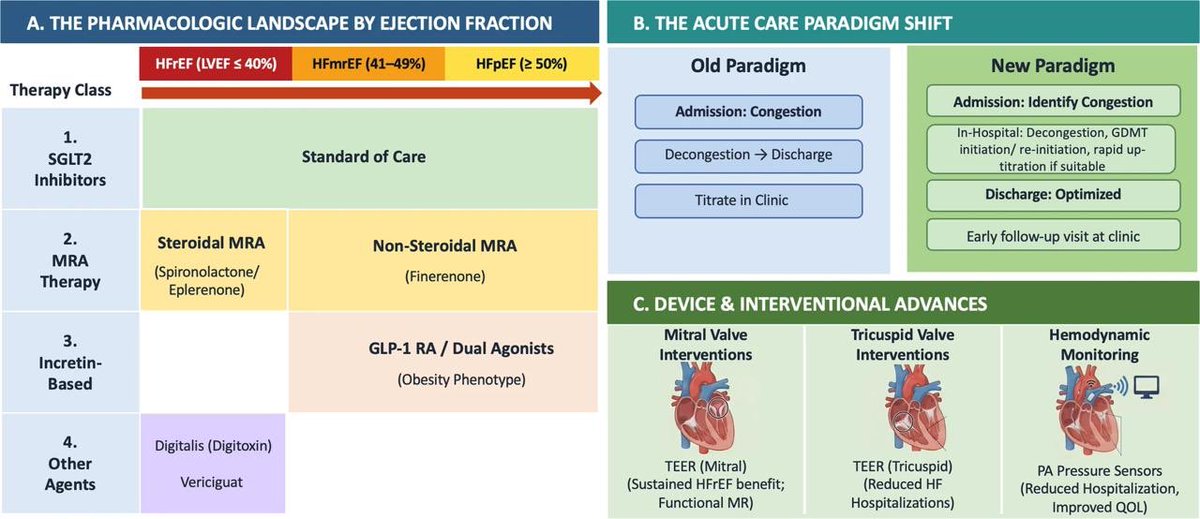
Heart failure evidence update 2026
Major developments include the emergence of non-steroidal mineralocorticoid receptor antagonists and incretin-based therapies for heart failure (HF) with mildly reduced and preserved EF, the validation of rapid guideline-directed medical therapy optimization strategies in acute HF, and new evidence supporting digitalis glycosides in HF patients with reduced EF. Device-based care has evolved with transcatheter edge-to-edge repair for valvular heart disease
#Cardiology #MedTwitter #CardioTwitter #HeartHealth #Healthcare
@mvaduganathan @SJGreene_md @gcfmd @biljana_parapid @DrMarthaGulati @hvanspall @hfcollaboratory @HFA_President @AndrewJSauer @dranulala @ShelleyZieroth
link.springer.com/article/10.100…
English
VictorHugoG.Johnson retweetledi

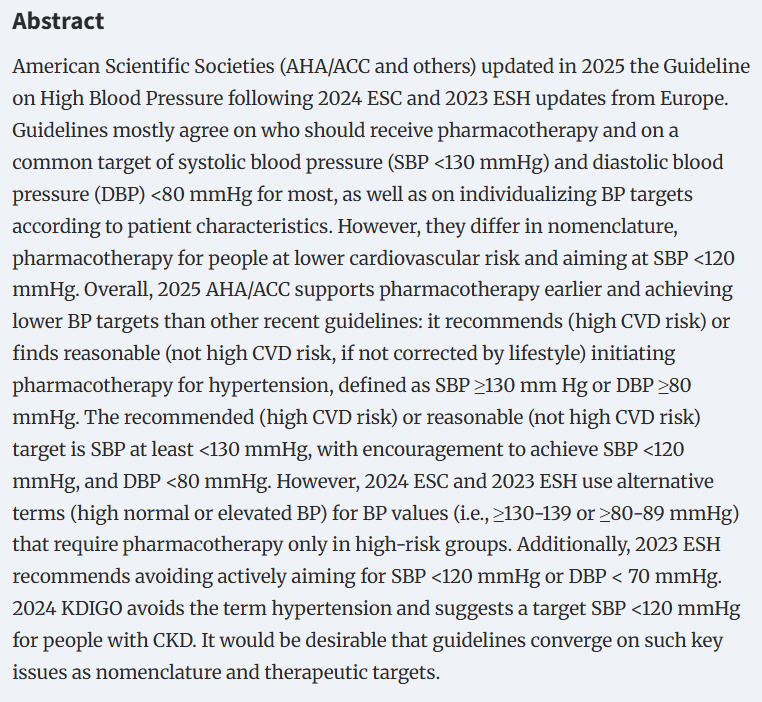
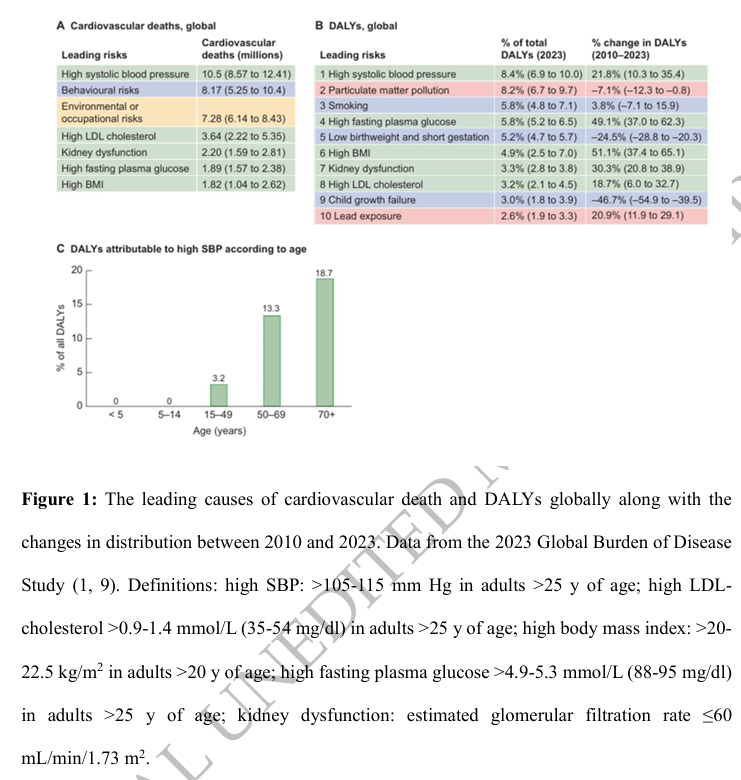
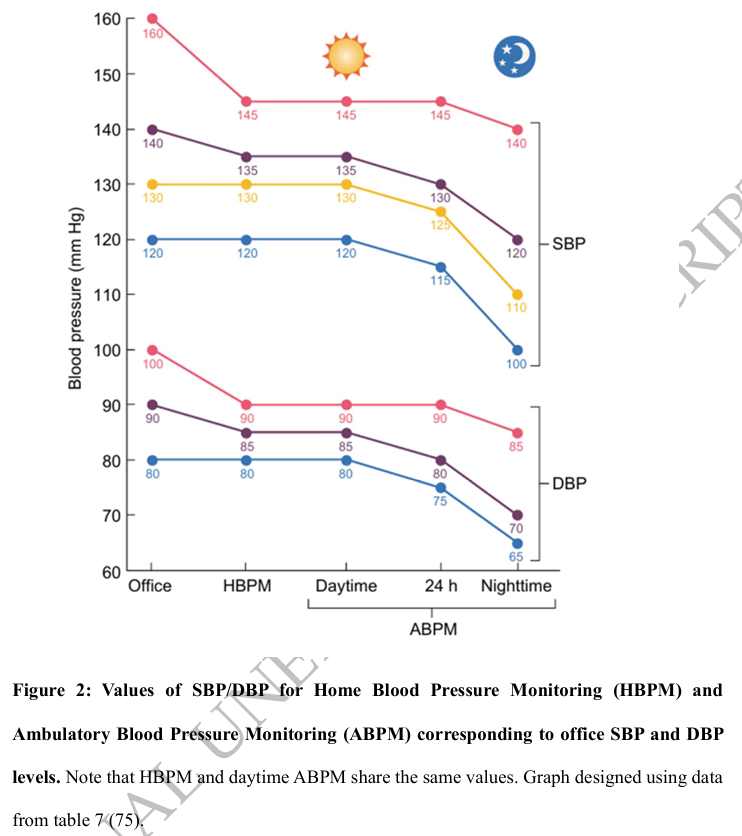
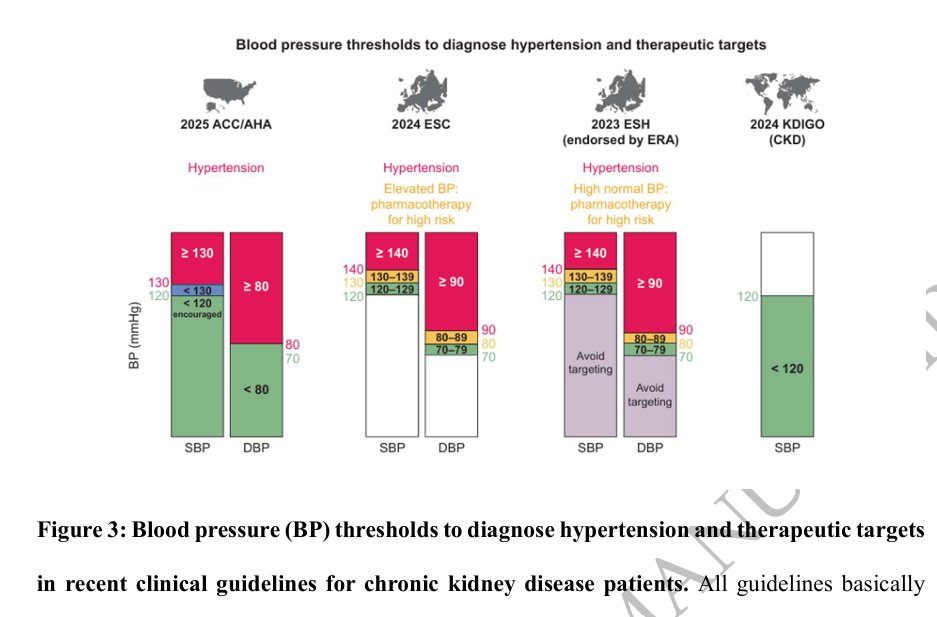
2025
AHA/ACC/AANP/AAPA/ABC/ACCP/ACPM/AGS/AMA/ASPC/NMA/PCNA/SGIM Guideline for the Prevention, Detection, Evaluation and Management of High Blood Pressure in Adults:
A Commentary from the European Renal Best Practice (ERBP)
🔓doi.org/10.1093/ndt/gf…

English