ทวีตที่ปักหมุด
To Retweet any publications/news related to lymphoma/myeloma/leukemia or any Heme/path cases please tag @qan2019
English
Hematology Media Center (HMC)💡
13.3K posts

@US_HMC
Interest in the field of myeloma/lymphoma/ Myeloma/Lymphoma/Leukemia/#mmsm #pathology #hematology #lymsm











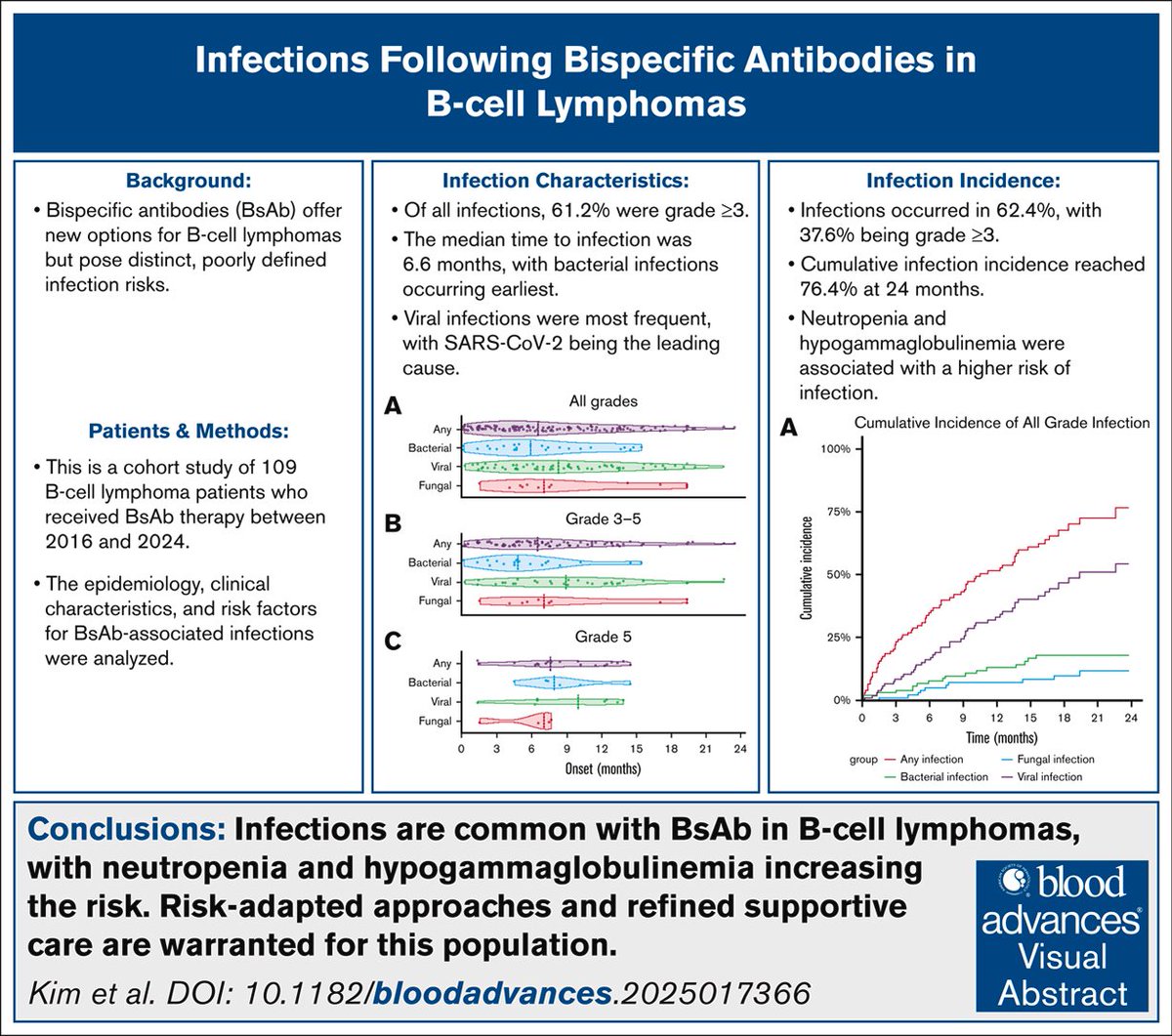
Very-low-dose decitabine and rhTPO for thrombocytopenia in lower-risk myelodysplastic syndrome link.springer.com/article/10.100… #mds