Diego Orofino
527 posts


Diego Orofino
@dorofino
Founder, Synapse Research Systems | Enterprise AI for Healthcare & Regulated Industries | 25+ Yrs Building Data Infrastructure | Azure, .NET, AI/ML



@MassiveBio is collaborating with @OpenAI to expand global access to clinical trials. 🌍 Through @OpenAI's Impact Hours program, we're enabling real-time trial parameterization and free pre-screening services in high-population regions, ensuring that life-changing treatment opportunities are available to patients everywhere, not just those near major research centers. This is what AI-driven precision oncology looks like in practice: breaking down the barriers that have long kept underserved patients from accessing the trials that could change their lives. Read the full announcement → massivebio.com/massive-bio-ex… #ClinicalTrials #AIinHealthcare #PrecisionOncology #HealthEquity #CancerResearch #OpenAI #DigitalHealth


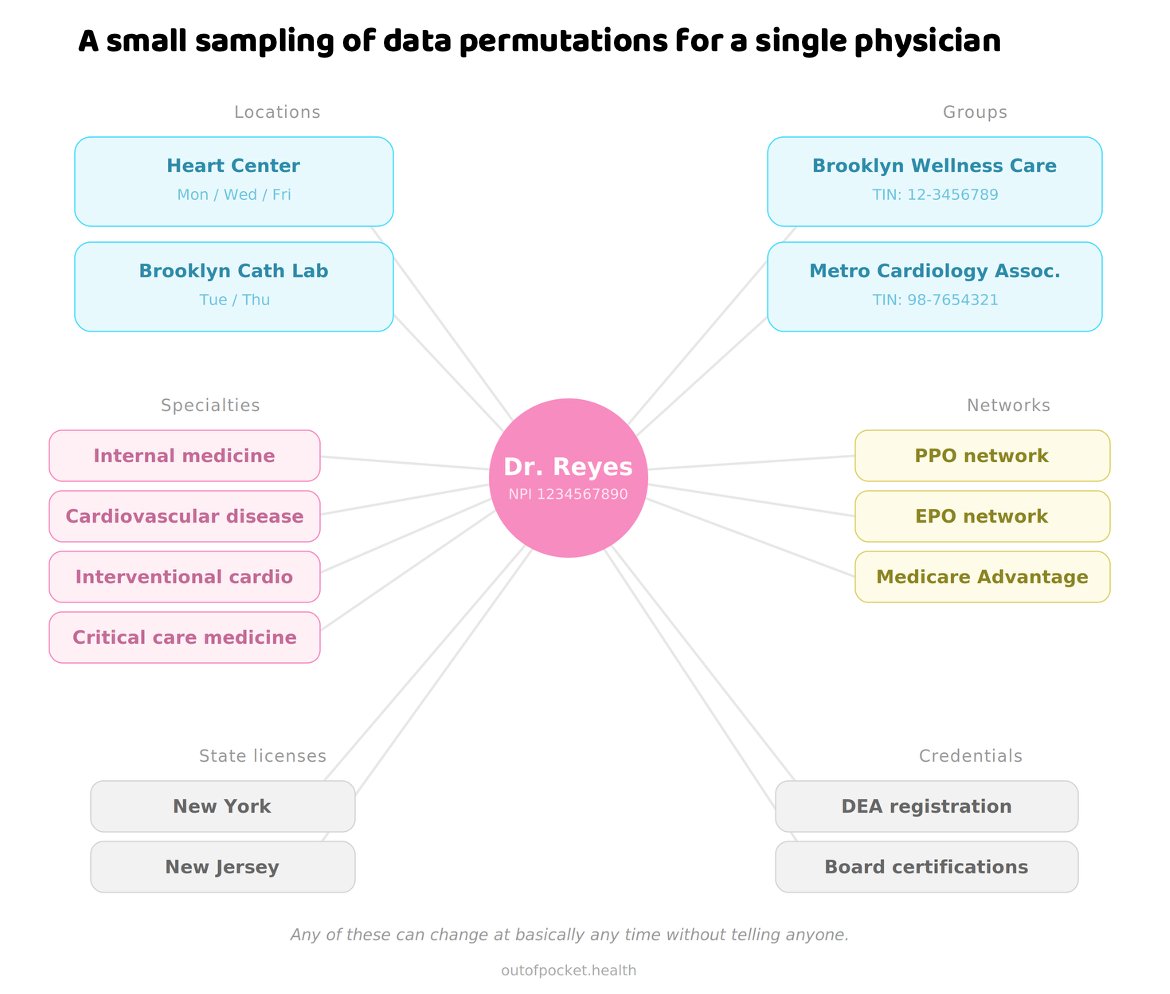







The “healthcare administration” chart is inaccurate, but it does reflect the inefficiencies in the system. We discussed this with @EladLevyMD on our latest episode of @DRsLoungePod: In the hospital, it takes about 20 people to get a person through surgery. In a physician-run ASC, they got it down to 4. Those efficiency gains aren’t captured in charts like these, because all 20 people in the hospital setting are categorized as clinical staff. The reduction in staff is important. It means the surgery is less expensive. It’s also faster and more efficient. That means more people get access to the care they need. Fantastic conversation.