
We need to teach how doubt is not to be feared but welcomed. It's OK to say, "I don't know."
Mátyás Andorka
3.2K posts


@easypocus
consultant in ICM&anaesth.; POCUS: FAMUS+FUSIC supervisor, FUSIC heart, CACTUS lung mentor; regional anaesth.; airway lead; retired ATLS/ETC/ALS/GIC instructor

We need to teach how doubt is not to be feared but welcomed. It's OK to say, "I don't know."

This is a really important Doppler physics point that influences how you interpret renal doppler signals in VExUS. What you are seeing here is not a physiological change in renal venous flow. It's a change in Doppler sensitivity. The velocity scale on colour or PW Doppler is essentially the PRF (pulse repetition frequency). When the scale is set high, the system is tuned to detect higher velocities and very slow flow may fall below the detection threshold. When that happens, the slower parts of the venous waveform simply disappear from the display. The result is that only the faster portions of the waveform are visible, which can make flow appear interrupted or pulsatile. If you progressively lower the scale, the machine becomes sensitive to lower velocities and those previously invisible parts of the waveform reappear. The same flow can therefore go from: no visible flow → interrupted flow → continuous flow purely as a function of Doppler settings, not physiology. This matters because renal venous velocities are extremely low (often just a few cm/s), so inappropriate scale settings can easily create pseudo-pulsatility. For renal venous Doppler the scale therefore needs to be reduced until low-velocity venous flow is fully visible (while avoiding noise). Only then can waveform morphology be interpreted. The important implication is that some apparent renal venous “pulsatility” may reflect machine sensitivity rather than true flow interruption. This is something that I have not seen discussed in the VExUS literature. @ThinkingCC @khaycock2 @NephroP @ArgaizR thoughts?




Neurological emergencies demand rapid bedside insight into cerebral physiology. In this review we summarise the evidence for NeuroPOCUS—including TCD, TCCD and optic nerve sheath ultrasound—and outline the new UK accreditation pathway for paediatric & adult practice. 🧠 Non-invasive neuromonitoring is coming of age. #FUSIC doi.org/10.1177/175114…






Great summary of how to make ESP work! I can confirm (at an anecdotal level) that this works very well - actually with all the “poke on the bone, lift up the muscle” blocks: - ESP - (deep) serratus plane - external oblique intercostal - parasternal x.com/easypocus/stat…

My ESP blocks never used to work. Then we realized what we were doing wrong…. Why Your ESP Block Fails (And How To Fix It) youtu.be/KTmzwR-NziE


Today we took the #BRIC course for the first time to the Royal Bournemouth Hospital UK. Bronchoscopy is a vital skill in the intensive care and acute care settings. Prof suveer singh and his faculty normally teach at location Chelsea and Westminster hospital in London. but because of high demand we have now been teaching in Manchester and in other cities. This course is designed for pulmonologists, intensivists, anaesthestists, ICU nurses and respiratory technicians. More information briccourse.com @BrICcourse @Respitudoc @AmbuEurope




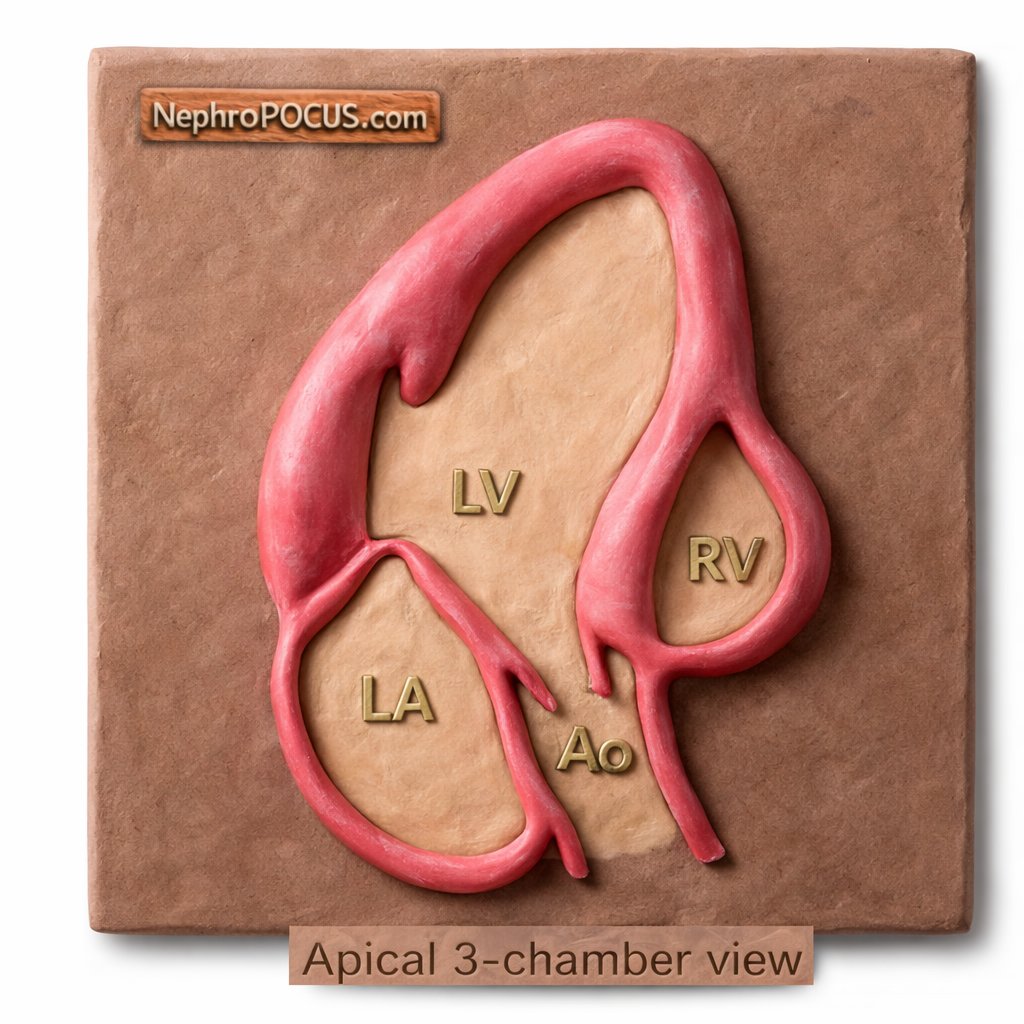


Critical closing pressure - how it should guide personalised care If CCP is a threshold (not a pressure), the clinical aim is simple: 👉 keep arterioles open 👉 preserve flow continuity from pump → tissue Not chase MAP or SVR in isolation. doi.org/10.3390/jpm160…