Bryce N. Balmain, PhD retweetledi

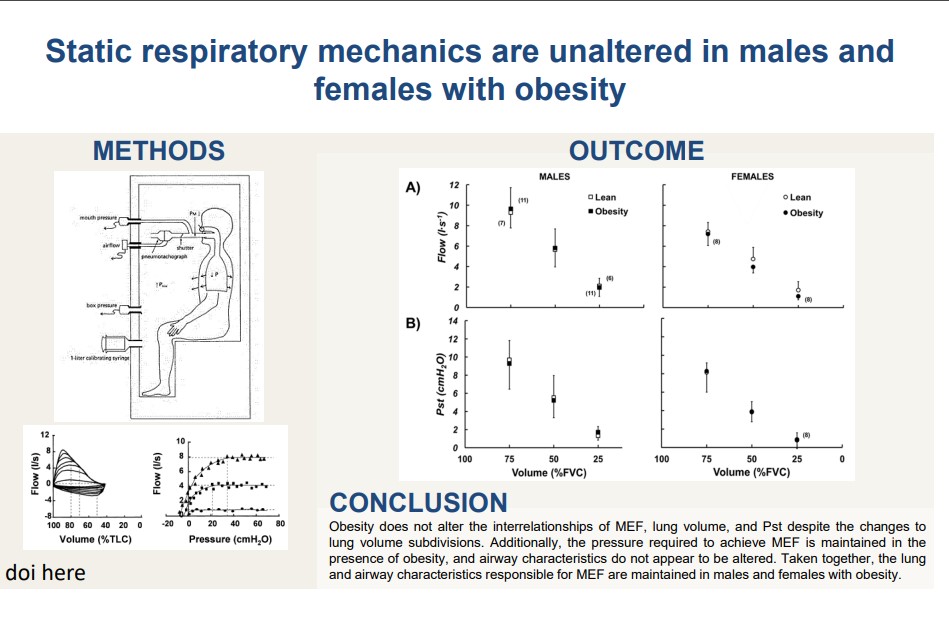
Happy to see our work from @mkstickland lab published online! Thank you to all co-authors for their contributions. @MirandaKirbyPhD @DrJ9378 @SanjaLovesData @seanvandiepen doi.org/10.1016/j.ches…
English
Bryce N. Balmain, PhD
83 posts

@BryceBalmainPhD
Assistant Professor & Integrative Physiologist | UT Southwestern Medical Center & Institute for Exercise and Environmental Medicine (IEEM)












We spoke to new NIH chief Monica Bertagnolli about risky pathogens, postdoc salaries and the year ahead go.nature.com/3tSgTVq










#OriginalResearch: In HFpEF, acutely lowering PCWP during exercise with nitro did not improve VO2 suggesting elevated PCWP during exercise not the primary cause of limits in exercise capacity #AHAJournals ahajrnls.org/3uTQDa6


