Sabitlenmiş Tweet
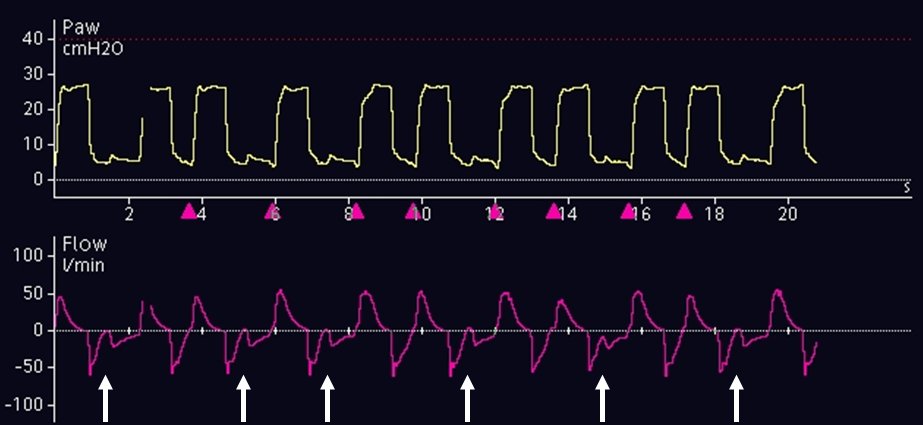
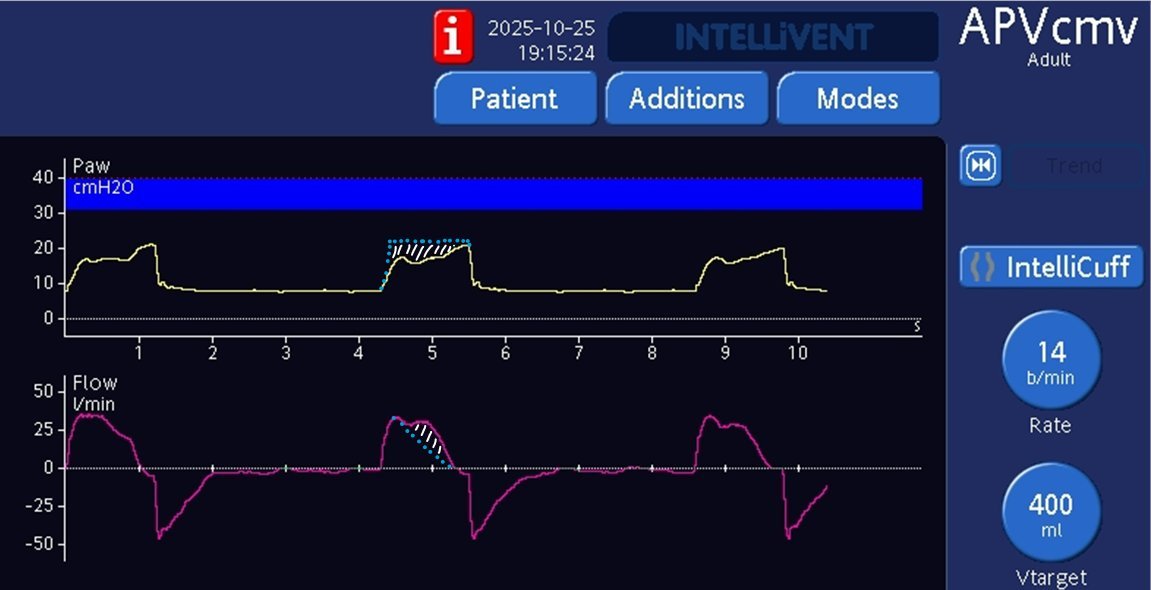
What is the short clip challenge? Check out this clip from our 2024 @IUSMDeptMed Grand Rounds. Are you ready to take the challenge? sign up here-->pulmonarypocus.com/contact-us
@NephroP @IUPCCM @OSUPCCM_Fellows @accpchest @POCUSJournal
English