
Jason J. Sico, MD, FAHS, FAHA, FAAN, FACP, FANA
454 posts


Jason J. Sico, MD, FAHS, FAHA, FAAN, FACP, FANA
@JSico_MD
Neurologist, Primary Care Internist, Headache Doc, Stroke Champion, Health Services Researcher, Patient Advocate, here to make a difference. Tweets are my own.
VA and Yale School of Medicine Katılım Aralık 2011
770 Takip Edilen645 Takipçiler

@razib_ul47671 4.6 and thanks
English

Honored to be on Capitol Hill with the Connecticut delegation for
@AANmembers #NOH26! 🏛️
We’re meeting with elected officials like @SenBlumenthal to advocate for:
✅ Permanent telehealth access
✅ Stable Medicare payments
✅ Robust NIH/BRAIN Initiative funding
Our patients deserve the best care, every day—no exceptions. 🧠💪
#AANadvocacy #BrainPAC #Neurology #HealthPolicy


English

s National Director of the VHA Headache Centers of Excellence, I’m proud to share our latest podcast on transforming #Migraine care for #Veterans. 🛡️
Key Pearls:
✅ Migraine is a complex neurological disease
✅ HCoE offers a multidisciplinary "whole health" approach
✅ Early intervention is key
Watch: facebook.com/share/v/1Airca…
@DeptVetAffairs @AANpublic @AHSHeadache @YaleMed #VHA #Neurology #Headache #MedTwitter #VAHealth
English

Advancing Neurological Care for Those Who Served: The AAN’s New Position on VA Brain Injury 🧠🛡️
I am incredibly proud to have served as the lead author for the American Academy of Neurology (AAN) new position statement regarding Brain Injury within the Veterans Affairs (VA) health system.
As a neurologist and National Director of the Headache Centers of Excellence in the VHA, I am deeply passionate about ensuring that our Veterans receive the highest quality neurological care. Brain injury is often an "invisible wound," but its impact on the lives of our heroes and their families is profound. This statement serves as a roadmap for advocacy, research, and clinical excellence to meet their unique needs.
Key Highlights of the Position Statement:
🏥 Specialized Access: We advocate for guaranteed access to board-certified neurologists and interdisciplinary teams for all Veterans suffering from Traumatic Brain Injury (TBI) and its complex sequelae.
🤯 Comorbidity Management: A dedicated focus on managing the "polytrauma triad," including the integration of care for post-traumatic headache, post-traumatic epilepsy, and sleep disorders.
🔥 Toxic Exposure Awareness: Formal recognition of the neurological risks associated with military exposures, including blast injuries and toxic substances from open burn pits.
🔬 Research Funding: A call for sustained federal investment in VA-led research to develop innovative diagnostics and treatments for chronic brain health conditions.
🤝 Strengthening Partnerships: Enhancing the collaboration between the AAN, the VA, and community providers to ensure no Veteran falls through the cracks of the healthcare system.
It was an honor to collaborate with a dedicated team of experts to bring this vision to life. Special thanks to my co-authors and the AAN Advocacy team: @NajibUmer | @RashmiHalker | @SarahNelsonMD | @JustinJordanMD | @AyubNeishay | @AANAdvocacy
Together, we are committed to moving the needle for Veteran brain health and ensuring those who served our country receive the world-class care they deserve.
#AAN #AmericanHeadacheSociety #AES #Veterans #TBI #BrainInjury #BurnPits #Neurology #VHA #Neurologist #BrainHealth #VeteranCare #NeurologyAdvocacy #HeadacheExcellence #EpilepsyAwareness

English

Proud to highlight this important new study led by my colleague and collaborator, John Ney, MD, from the Yale Department of Neurology. Published in JAMA Neurology, the research draws from the Global Burden of Disease 2021 data and reveals a staggering hidden burden: over half of Americans (approximately 54%, or 180 million people) are affected by neurological disorders, many without realizing it.
This positions the U.S. as having the highest prevalence of nervous system diseases worldwide, surpassing rates in high-, middle-, and low-income countries alike.
Key takeaways include:
• Neurological conditions are now the leading cause of disability globally, with stroke, Alzheimer’s disease and other dementias, diabetic neuropathy, and migraine driving the most significant impacts in the U.S.
• From 1990 to 2021, there’s been a notable rise in these disorders, underscoring the need for urgent attention.
These findings have profound implications for U.S. public health and health policy. They call for enhanced public awareness campaigns to encourage early recognition and intervention for symptoms like numbness, weakness, or severe headaches, which could prevent progression to severe outcomes like stroke. On the policy front, we must prioritize funding for basic science research to uncover disease mechanisms and accelerate innovative therapies, while expanding access to rehabilitation services and streamlining approvals for effective treatments (e.g., new migraine medications).
Additionally, integrating preventive strategies—such as promoting exercise, healthy diets, consistent sleep, and diabetes management—into national health initiatives could mitigate risks and reduce the overall burden.
As a neurologist based at Yale and the VA, I’m encouraged by collaborations like this with partners from the University of Washington, Emory University, and the American Academy of Neurology. Let’s use this data to drive meaningful change in neurology and beyond.
Read the full Yale Q&A here: news.yale.edu/2025/12/09/mas…
#Yale #YaleNeurology #JAMANeurology #Neurology #NeurologicalDisorders #PublicHealth #HealthPolicy #AAN #Neuroscience #BrainHealth #GlobalBurdenOfDisease
English

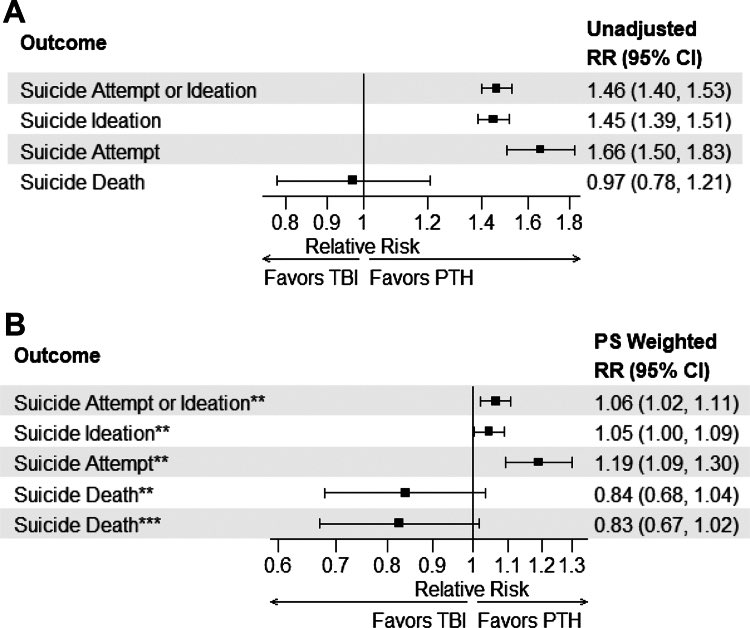
New research: Veterans living with post-traumatic headache face heightened suicide risk compared to those with TBI who do not have headache.
Key findings from our @VAResearch study:
•45% ↑ risk of suicidal ideation (RR 1.45)
•66% ↑ risk of suicide attempts (RR 1.66)
•9.7% vs 6.6% experienced suicidal ideation/attempts
Veterans with PTH deserve enhanced screening & mental health support. Suicide prevention must be a priority in headache care.
Study by @JSico_MD @LisaABrenner @SengElizabeth @AmyGrinberg @VA_HeadacheCoE & team
Read more: pubmed.ncbi.nlm.nih.gov/41321729/
#Veterans #VAResearch #Headache #TBI #Suicide #Prevention #Pain #PTSD #MentalHealth #SuicidePrevention #Neurology #VeteransHealth #Yale #YaleNeurology #HealthServices #HealthSystems
English
Jason J. Sico, MD, FAHS, FAHA, FAAN, FACP, FANA retweetledi

A powerful new statistic. And more so, a call to action on our @AANmember #BrainHealthForAll initiative 🙌✅ 🧠 #NeurologyProud
American Academy of Neurology@AANmember
One in two people in the US is affected by a neurological disease or disorder, according to a new systematic analysis by the American Academy of Neurology and @IHME_UW. Read the new research published in @JAMANeuro: hubs.la/Q03VHr0F0 #BrainHealth #AANscience #Neurology
English

Thinking "Out of the Box" for complex headache with Dr. Stephanie Nahas at #ScottsdaleHeadache! 🌵🧠
5 Clinical Pearls to take home:
1️⃣ The Readiness Ruler: Assess motivation to change on a 0-10 scale. If a patient is a "2", ask: "Why didn't you mark a 1?" to evoke their personal motivation.
2️⃣ Rational Polypharmacy: Use the "4 Columns" Mix & Match approach for acute bridging—combine a Serotonergic + Anti-CGRP/NSAID + Dopaminergic + Steroid.
3️⃣ Refractory Options: Consider Minocycline (100mg BID) to target glial cell inflammation or Memantine (titrate to 10mg BID).
4️⃣ Indomethacin: It's not just for Hemicrania Continua. Titrate rapidly (up to 100mg TID) for refractory migraine or "stabbing" headaches.
5️⃣ The "Difficult" Encounter: Stop fighting the disease. Make the clinician-patient relationship the target for change and validate their emotional experience.
@AHSHeadache #Migraine #HeadacheMedicine #MotivationalInterviewing #MedEd

English

Insightful #AHSAZ plenary by @rashmihalker this morning on the challenges of Medication-Overuse Headache (MOH) when the provoking drug can’t be stopped. 🧠💊
A few of the Key Takeaways:
🔹 MOTS Trial: Starting/optimizing preventive treatment is effective without mandatory withdrawal of the overused acute medication.
🔹 Evidence-Based Options: CGRP mAbs, OnabotulinumtoxinA, and Topiramate show efficacy in MOH.
🔹 Complex Cases: Butalbital & opioid overuse require gradual tapers and multidisciplinary care.
🔹 Bottom Line: Don’t wait—initiate prevention early!
#AHSAZ #AHS #HeadacheMedicine #Migraine #Neurology #HeadacheResearch #Headache #mugraine #MOH #HeadacheDisorders #CME #AmericanHeadacheSociety
English
Jason J. Sico, MD, FAHS, FAHA, FAAN, FACP, FANA retweetledi

💬 Viewpoint: The Joint Commission and Coalition for Health AI have issued guidance on responsible #AI use in health care, but without a unified evaluation system, US hospitals face liability and efficiency challenges as AI adoption expands.
ja.ma/48ALE2t

English

@DanielCPotts And our #Veterans are fortunate to have you caring for them, my friend
English
Jason J. Sico, MD, FAHS, FAHA, FAAN, FACP, FANA retweetledi

📢 New Neurology Podcast episode! 🎙️
In the @GreenJournal podcast from the American Academy of Neurology @AANmember Dr. Jessica Ailani interviews Dr. Francesca Puledda (@pul_fra) from @KingsCollegeLon on the @ihs_official practical recommendations for migraine, recently published in @JCephalgia !
Tune in here:
neurology.org/media/podcast/…
📄 Read the full articles in Cephalalgia:
Acute:
journals.sagepub.com/doi/10.1177/03…
Preventive:
journals.sagepub.com/doi/10.1177/03…
A must-listen for anyone interested in evidence-based migraine management!
Kudos to Francesca and Jessica for this clinical useful podcast! 👏 #Migraine #Neurology #Cephalalgia

English
Jason J. Sico, MD, FAHS, FAHA, FAAN, FACP, FANA retweetledi

🌍 Brain Awareness Week 2025: Shedding Light on Headache Disorders
Did you know that headache disorders are among the top three most common neurological conditions across most age groups? Let’s raise awareness and support research for better headache care!
#BrainAwarenessWeek #headache #neurology

English
Jason J. Sico, MD, FAHS, FAHA, FAAN, FACP, FANA retweetledi

HSR's Burgess and colleagues find that telehealth mindfulness-based interventions can accelerate and improve nonpharmacological pain treatment: The LAMP Randomized Trial i.mtr.cool/kmilbzecoq
English

One of my favorite places to be … #AHS2024 with some of my favorite people @ahsheadache
So honored to be among a group of people #dedicated to improving the lives of those with #headache and #migraine disease through #research #clinicalcare #education #advocacy #mentorship

English
Jason J. Sico, MD, FAHS, FAHA, FAAN, FACP, FANA retweetledi

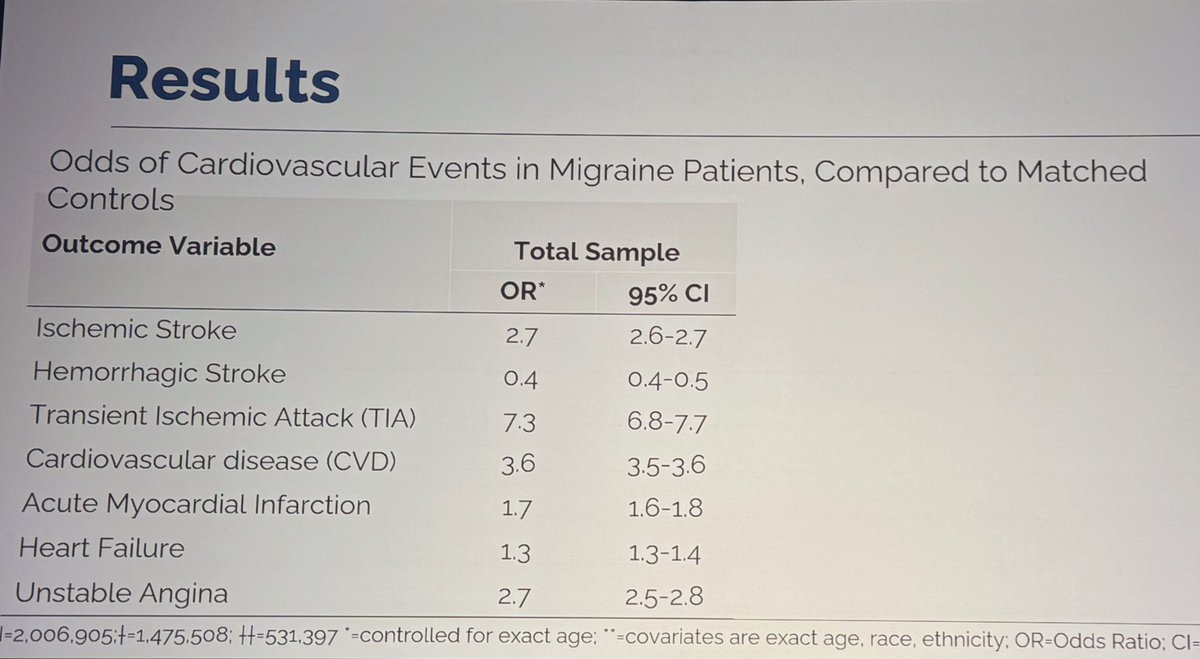
Great job Ali Schwartz, presenting data at #ahsam showing migraine is associated with higher odds of ischemic stroke and TIA at cross-section in both men and woman veterans. @ahsheadache @YUNews @EinsteinMed

English

Those living with #migraine are at increased risk of #ischemicstroke #TIA and other #cardiovascular events compared to demographically similar people without migraine.
So often we are thinking about offering migraine #prevention; should we be doing more about vascular prevention
English

I am so blessed to work with such gifted individuals from such disciplines as #neurology #medicine #psychologists #pharmacists committed to improving care #quality #delivery #equity for #Veterans living with #headache and #migraine disease @ahsheadache @DeptVetAffairs #AHSAM
Brittany Mays, MD@PMRHeadacheMD
Such an honor to be part of this fantastic network of headache specialists taking care of our veterans. Thank you to our fearless leader @JSico_MD #HCoE @ahsheadache #AHSAM
English
Jason J. Sico, MD, FAHS, FAHA, FAAN, FACP, FANA retweetledi
Jason J. Sico, MD, FAHS, FAHA, FAAN, FACP, FANA retweetledi

June is Migraine and Headache Awareness Month #MHAM
#AHSFirstContact is the go-to resource to enhance your #migraine and #headache knowledge offering resources for primary care practitioners interested in migraine diagnosis and management. Learn more: bit.ly/3P9A0AD

English




