Sabitlenmiş Tweet
Manpreet
343 posts

Manpreet retweetledi

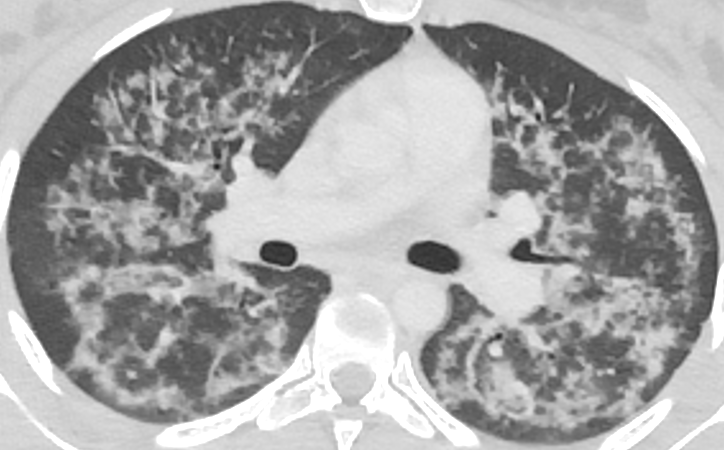
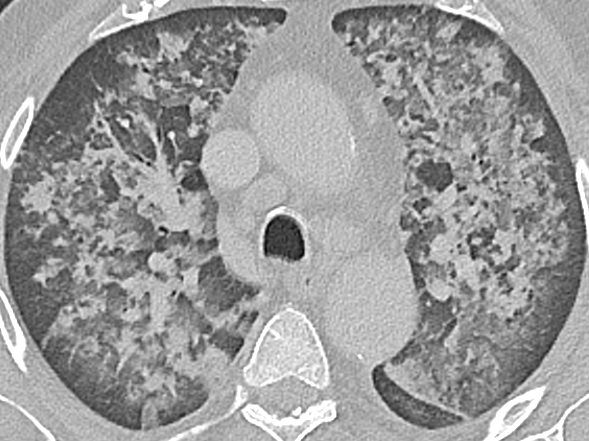
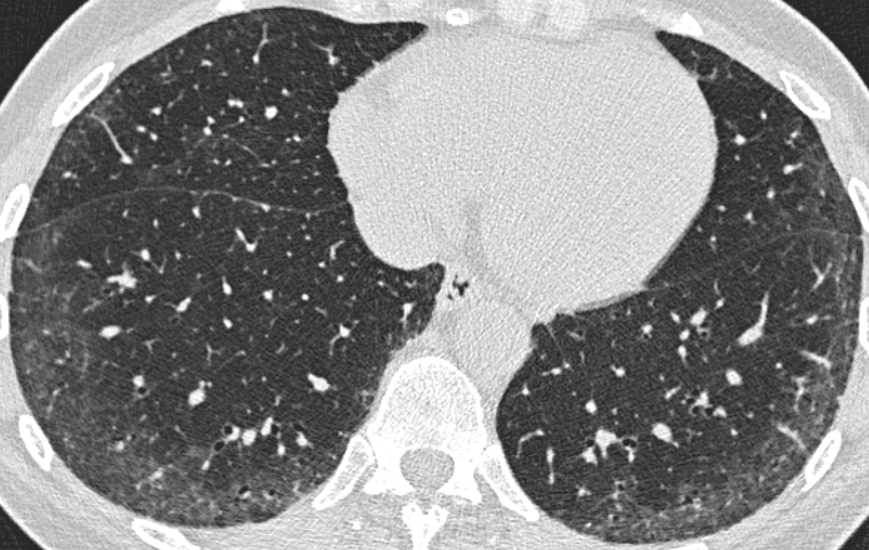
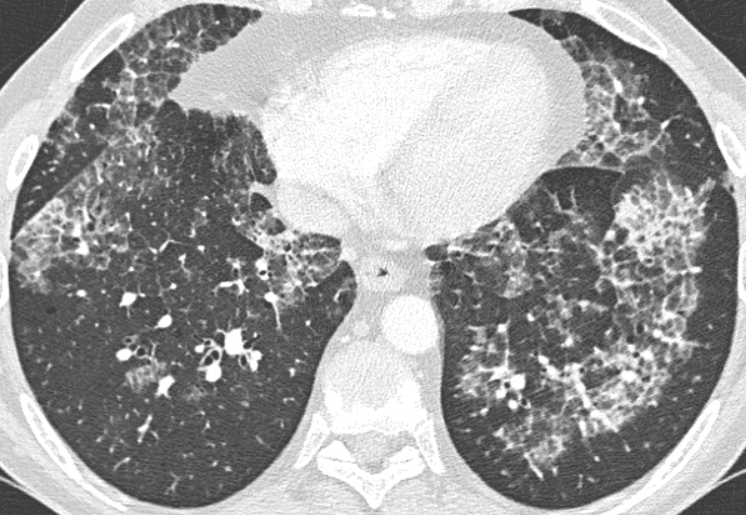
💧 DKA resuscitation: Normal Saline vs Ringer’s Lactate, does it really matter?
For decades, 0.9% NaCl has been the default fluid in diabetic ketoacidosis.
But… is it still the best choice?
🧪 New randomized ICU data (2025-2026)
👉 88 patients with severe DKA
👉 Ringer’s Lactate (RL) vs Normal Saline (NS)
👉 Same insulin protocol
📊 Primary outcome: DKA resolution at 48h
➡️ No difference
• RL: 56.5%
• NS: 50%
(p = 0.66)
⚖️ So… clinically equivalent? Not exactly.
The physiology tells a different story 👇
🧠 What RL does better
Compared to NS:
✔️ Higher bicarbonate early
✔️ Better potassium levels
✔️ Lower chloride at 48h
➡️ Translation:
• Less hyperchloremic metabolic acidosis
• Lower risk of hypokalemia
• More physiologic acid-base recovery
⚠️ What NS still does
❗ Same DKA resolution speed
❗ Same ICU stay
❗ Same mortality
➡️ So endpoints look “equal”…
…but physiology is not.
🚨 Why this matters in real ICU practice
Hyperchloremia is not benign:
• Worsens metabolic acidosis
• Increases respiratory workload
• Promotes renal vasoconstriction
• Delays recovery
And hypokalemia?
• Arrhythmias
• Insulin resistance
• Delayed metabolic correction
🧬 Clinical interpretation
This is not about:
❌ “Which fluid resolves DKA faster?”
This is about:
➡️ Which fluid creates a better internal environment for recovery
🔥 Take-home message
👉 NS is acceptable
👉 RL is physiologically smarter
➡️ Especially in:
• Severe acidosis
• High chloride states
• Patients at risk of hypokalemia
📚 Trifi A. et al. (2025)
Medicina Intensiva
doi.org/10.1016/j.medi…

English
Manpreet retweetledi
Manpreet retweetledi
Manpreet retweetledi
Manpreet retweetledi

⚠️ Vasopressor weaning in septic shock: the blind spot in current guidelines
We talk a lot about starting vasopressors.
We rarely talk about how to stop them safely.
And that may be a problem.
📌 The gap
The 2026 Surviving Sepsis Campaign provides:
✔️ Clear guidance on initiation
✔️ Clear escalation strategies
❌ But no guidance on de-escalation
👉 Yet this is one of the most frequent bedside challenges
🧠 Key clinical dilemma
Which should be stopped first?
• Norepinephrine?
• Vasopressin?
The answer is… unclear.
📊 Conflicting evidence
👉 Observational studies:
• Higher hypotension when vasopressin is stopped first
👉 Randomized trials (DOVSS, RENOVA):
• Higher hypotension when norepinephrine is stopped first
➡️ Completely opposite conclusions
💡 Why this contradiction exists
It’s not just what you stop.
It’s how you stop it.
👉 Abrupt discontinuation vs titrated reduction
✔️ Most RCTs used protocolized titration
❌ Observational studies often used abrupt withdrawal
➡️ Method matters as much as sequence
🧬 Physiology you should not ignore
• Endogenous vasopressin rises early
• Then drops within ~48h
➡️ Leading to relative vasopressin deficiency
👉 Removing vasopressin at this point may trigger hypotension
🧪 Potential future tool
👉 Copeptin (vasopressin surrogate)
• May predict hypotension after withdrawal
• Not yet ready for routine decision-making
🚨 Clinical reality
There is:
❌ No standardized weaning protocol
❌ No strong guideline recommendation
❌ Limited RCT evidence
But:
👉 This is a daily ICU decision
🔥 Take-home message
Vasopressor weaning is not a passive step.
It is an active hemodynamic intervention.
And currently:
👉 We are navigating it with incomplete evidence
📚 Mallmann C. et al. (2026)
Intensive Care Medicine
doi.org/10.1007/s00134…

English
Manpreet retweetledi

Manpreet retweetledi
Manpreet retweetledi
Manpreet retweetledi

🧠 Uremic Coagulopathy — High-Yield Pearls (Heme Perspective)
🩸 Pathophysiology → platelet dysfunction (NOT factor deficiency)
🧩 Mechanism → impaired platelet adhesion + aggregation
🔬 Key toxins → guanidinosuccinic acid, phenols, PTH
⚠️ vWF interaction ↓ → defective GP Ib–vWF binding
🧪 Platelet count → usually NORMAL
📉 PT/PTT → usually NORMAL
📉 Bleeding time / PFA-100 → PROLONGED
🩺 Clinical picture
🩸 Mucocutaneous bleeding (epistaxis, gingival)
🩸 Easy bruising, petechiae
🩸 GI bleeding common
🩸 Post-procedure bleeding risk ↑
🚨 Triggers worsening bleeding
❌ Uremia (BUN >60–80 mg/dL)
❌ Anemia (↓ Hct → worsens platelet function)
❌ Concomitant antiplatelets/NSAIDs
❌ Dialysis delay
🧪 Diagnosis (clinical)
✔️ CKD/ESRD context
✔️ Normal coagulation profile
✔️ Platelet dysfunction pattern
✔️ Exclusion of DIC / liver disease
💊 Management (stepwise — guideline-based)
🟢 1. Dialysis = DEFINITIVE
✔️ Rapid improvement within 24–48h
✔️ First-line in active bleeding
🟡 2. DDAVP (Desmopressin)
💉 0.3 mcg/kg IV over 20–30 min
⚡ Onset: 1–2 h
⏳ Duration: 6–8 h
⚠️ Tachyphylaxis after 1–2 doses
🟡 3. Correct anemia
🎯 Target Hb ≥10 g/dL
➡️ RBC transfusion improves platelet interaction
🟡 4. Cryoprecipitate
✔️ If bleeding persists
✔️ Works via ↑ vWF & fibrinogen
⏳ Effect within hours
🟡 5. Conjugated estrogens
💉 0.6 mg/kg IV daily × 5 days
⏳ Delayed onset (6–24 h)
🕐 Longer effect (1–2 weeks)
🔴 Avoid
❌ Platelet transfusion (limited role unless thrombocytopenia)
❌ NSAIDs / aspirin
🧠 Practical procedural prep
✔️ Dialyze pre-procedure
✔️ Give DDAVP 30–60 min before
✔️ Ensure Hb optimized
✔️ Consider cryo if high-risk
📊 Evidence pearls
📌 DDAVP → transient but effective (standard of care for urgent bleeding)
📌 Dialysis → cornerstone (KDIGO CKD guidelines)
📌 Estrogens → useful in recurrent bleeding when dialysis insufficient
🎯 MCQ
Patient ESRD + epistaxis + normal PT/PTT → best immediate therapy?
A) FFP
B) Platelets
C) DDAVP ✅
D) Vitamin K
👉 Answer: C (DDAVP) — fastest hemostatic correction
🧪 OSCE scenario
📍 ESRD patient needs central line
➡️ Plan: Dialysis → DDAVP pre-procedure → optimize Hb → avoid NSAIDs
#Hematology #Nephrology #Coagulopathy #CKD #KFSHRC
English
Manpreet retweetledi
Manpreet retweetledi
Manpreet retweetledi

Si te interesan los JAKinibs 💊 aquí tienes la súper revisión ✍️
Acceso abierto 🔑 nature.com/articles/s4157…

Español
Manpreet retweetledi

Her expressions, her voice, her aura 🔥
Pooja Sharma made Draupadi unforgettable 💥
ᏗᏕ@unfiltered_AS
It’s like this role was written only for them.
English

Pooja B sharma as Draupadi is Devine 🪷💯
No one can beat it
One of the best performances in ITV
Namit Malhotra sir should have considered her for the role of Urmila.. dearest sister of maa Sita
#Ramayan @malhotra_namit
English
Manpreet retweetledi

the whole monologue part
cinesthetic.@TheCinesthetic
When you hear “best scene in television history.” What’s the absolute first scene you think of?
English
Manpreet retweetledi

pooja sharma as draupadi
cinesthetic.@TheCinesthetic
an actor that was born for the role that they played
Eesti
Manpreet retweetledi
Manpreet retweetledi
Manpreet retweetledi
Manpreet retweetledi