Smit Patel, MD, MPH retweetledi

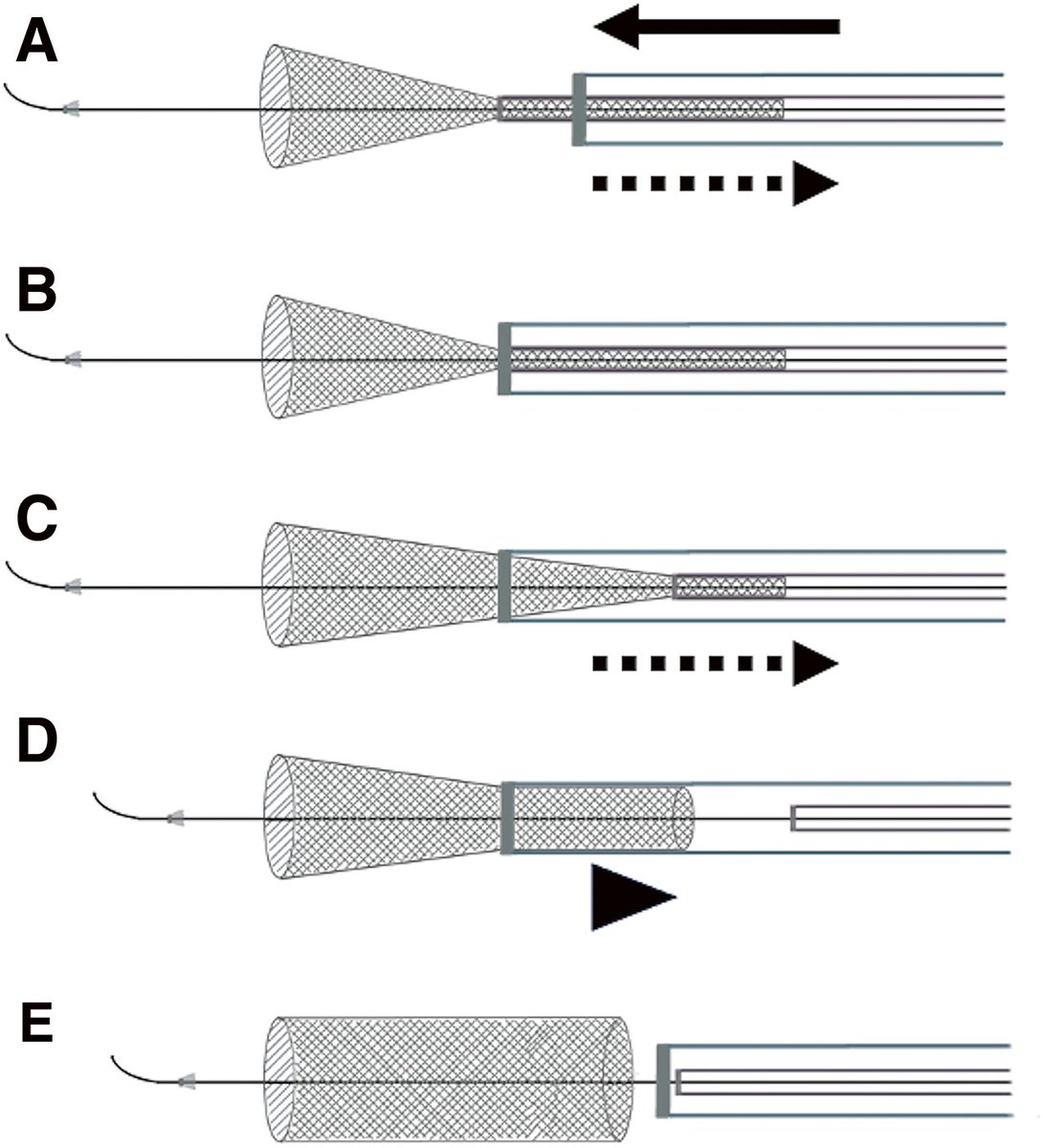
Paclitaxel Drug-Coated Balloon Angioplasty for Medically Refractory Intracranial Atherosclerotic Disease: A US Single-Center Experience With the AGENT Balloon
ahajrnls.org/4t21ZV4

English
Smit Patel, MD, MPH
1K posts


@SmitdPat
Neuro-endovascular Surgeon at Saint Francis Health System, Tulsa; Former Residency at @UConnHealth; Former Fellowships at @UCLAHealth & @hartfordhosp




















Patients with intracranial athero should now be targeted to LDL<55 mg/dl, given the new ACC/AHA lipid guidelines. This should be adopted in CAPTIVA and other ongoing trials, as well as routine practice @BrianHoh1 @ESOstroke @WorldStrokeOrg @AHAScience







