Elizabeth Bárcena
2.3K posts


Elizabeth Bárcena
@elibb346
Hija de la Tierra y el Sol ☀ 🇵🇪 Anestesia y Reanimación. #orgullosodeseranestesista
Palma, Spain Katılım Ocak 2011
862 Takip Edilen219 Takipçiler
Elizabeth Bárcena retweetledi

Should we delay surgery after a preoperative cardiovascular events to prevent postoperative stroke? New retrospective cohort data from Luney et al #stroke #surgery #cardiac
bjanaesthesia.org/article/S0007-…

English
Elizabeth Bárcena retweetledi

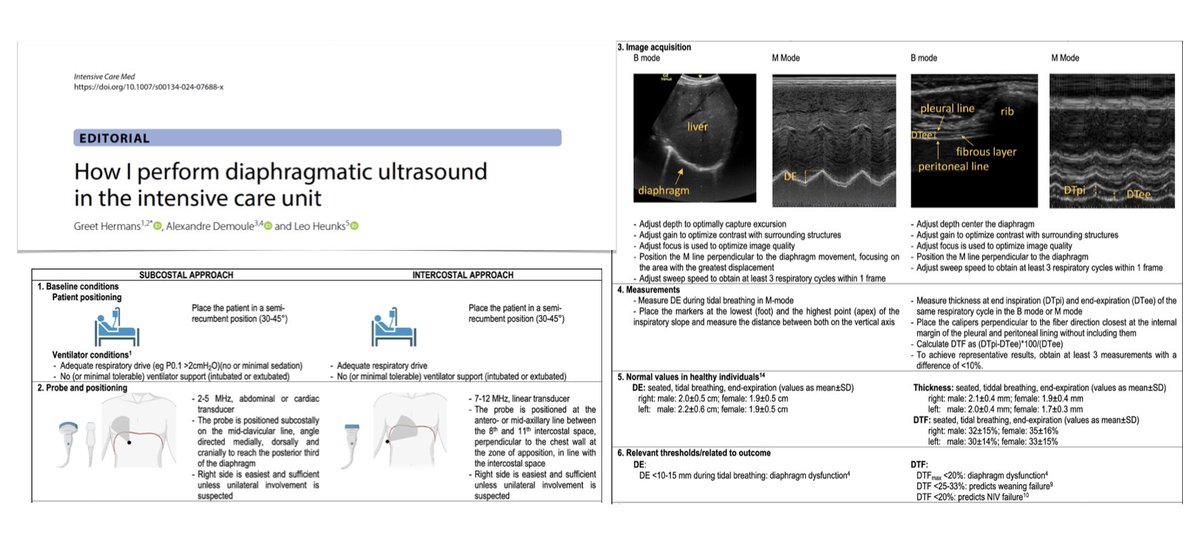
How I perform diaphragmatic #ultrasound in #ICU
🖥️ practical aspects: subcostal approach, intercostal approach
🖥️ areas of application in daily care
🖥️ future prospects
Free to read #FOAMcc #FOAMus #echofirst
🔓 rdcu.be/dYy6l
English

Los invito a leer esta excelente review que abarca y complementa en su primera parte el monitoreo hemodinámico no invasivo con POCUS , que realizamos día a día en nuestros pacientes graves y críticos, herramienta vital bedside ,muy útil para nuestra rápida toma de decisiones en disímiles escenarios, elaborada de manera práctica por estimados amigos y autores.
revistachilenadeanestesia.cl/revchilanestv5…
#POCUS, #ECODINAMIA #criticalcare

Español
Elizabeth Bárcena retweetledi

If you’re learning how to do lung ultrasound, the BLUE Protocol is a great place to start. This paper tackles what you need to know. 🎩 tip to the authors.
eddyjoemd.com/foamed/

English
Elizabeth Bárcena retweetledi

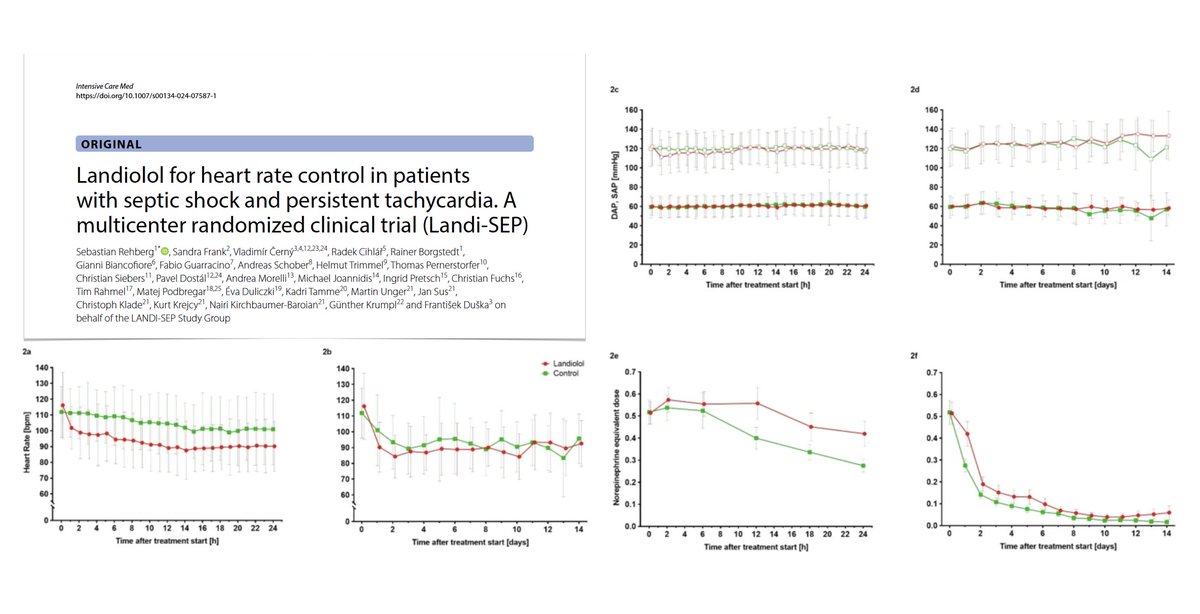
Landiolol for heart rate control in adults with septic shock & persistent tachycardia
🫀effective in ⬇️/maintaining HR, no ⬆️vasopressor requirements
⚖️ no differences in adverse events & outcomes
🪦 trend for ⬇️ mortality if AF, ⬆️ if sinus tachycardia
🔓 bit.ly/3XPIClS
English
Elizabeth Bárcena retweetledi

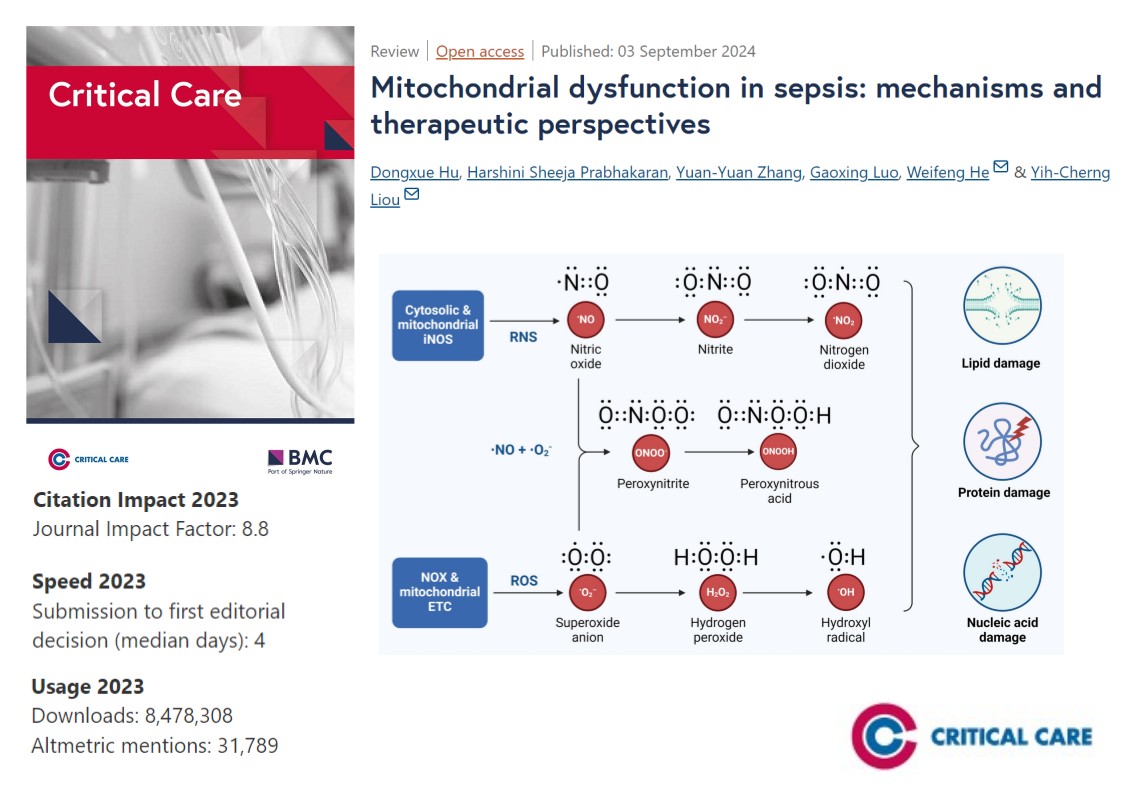
#CritCare #OpenAccess
Mitochondrial dysfunction in sepsis: mechanisms and therapeutic perspectives
Read the full article: ccforum.biomedcentral.com/articles/10.11…
@jlvincen @ISICEM #FOAMed #FOAMcc
English
Elizabeth Bárcena retweetledi
Elizabeth Bárcena retweetledi

2a Reunión EACTAIC España, el 12 y 13 de Noviembre, on-line y el viernes 15 de Noviembre talleres presenciales de ETE, ETT, Eco Abdominal y DTC en #unavmed. Opción de hacer ambos o solo 1 de los dos!! No te lo pierdas! Más info: reunion-eactaic-spain.com @sedar_es @Docencia_SEDAR

Español
Elizabeth Bárcena retweetledi

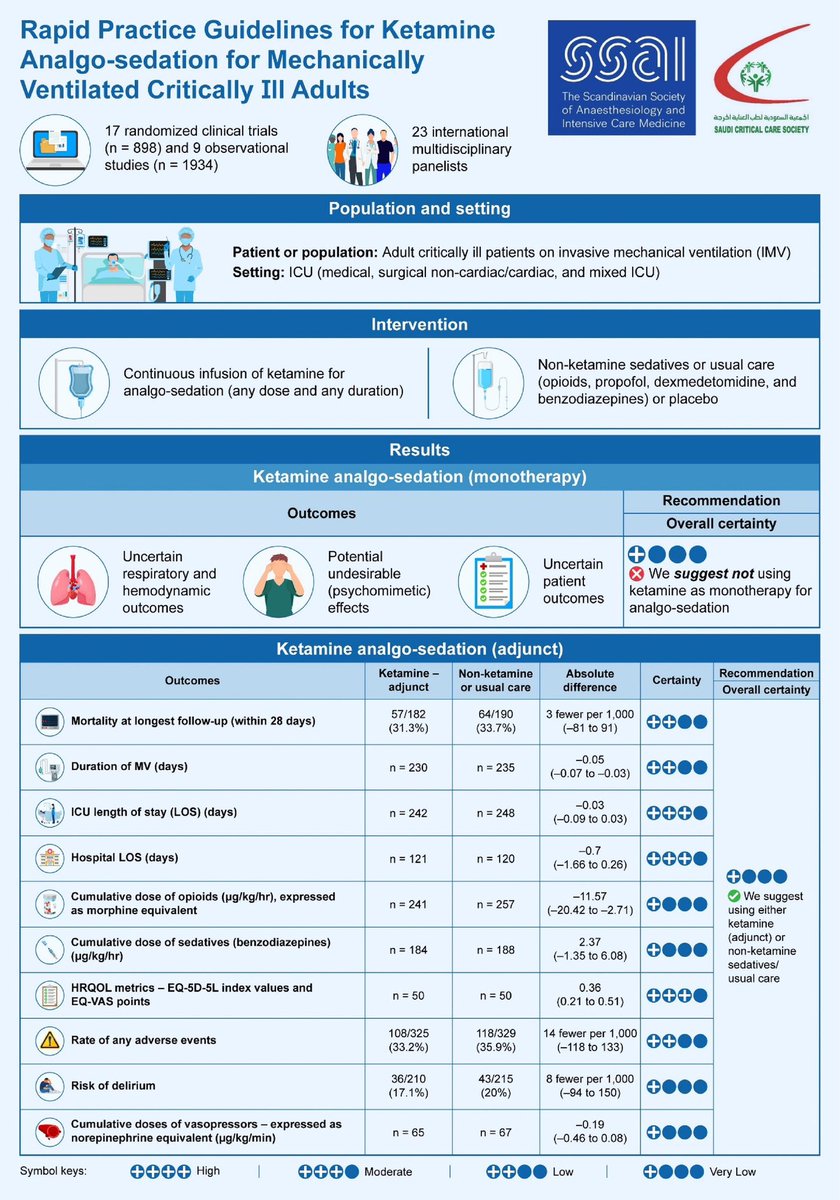
🙋♂️ New Ketamine Sedation Guidelines for Mechanically Ventilated Patients - Published Today!
🔗 doi.org/10.1111/aas.14…
#ICU #FOAMcc #Ketamine #SCCM #SCCMSoMe #ICURehab
@ActaAnaesthScan
@Marwa_Ramer @YaseenarabiYa @NazishHashmi1
@JamiePrivratsky
@Duke_Anesthesia
@DukeAnesFellows

English
Elizabeth Bárcena retweetledi

#DocenciaSEDAR: SONO ATLAS 🛠️ Otra herramienta docente disponible en la web para profundizar en la ecografía. Puedes encontrarla en 👉🏼 sonoatlas.cz
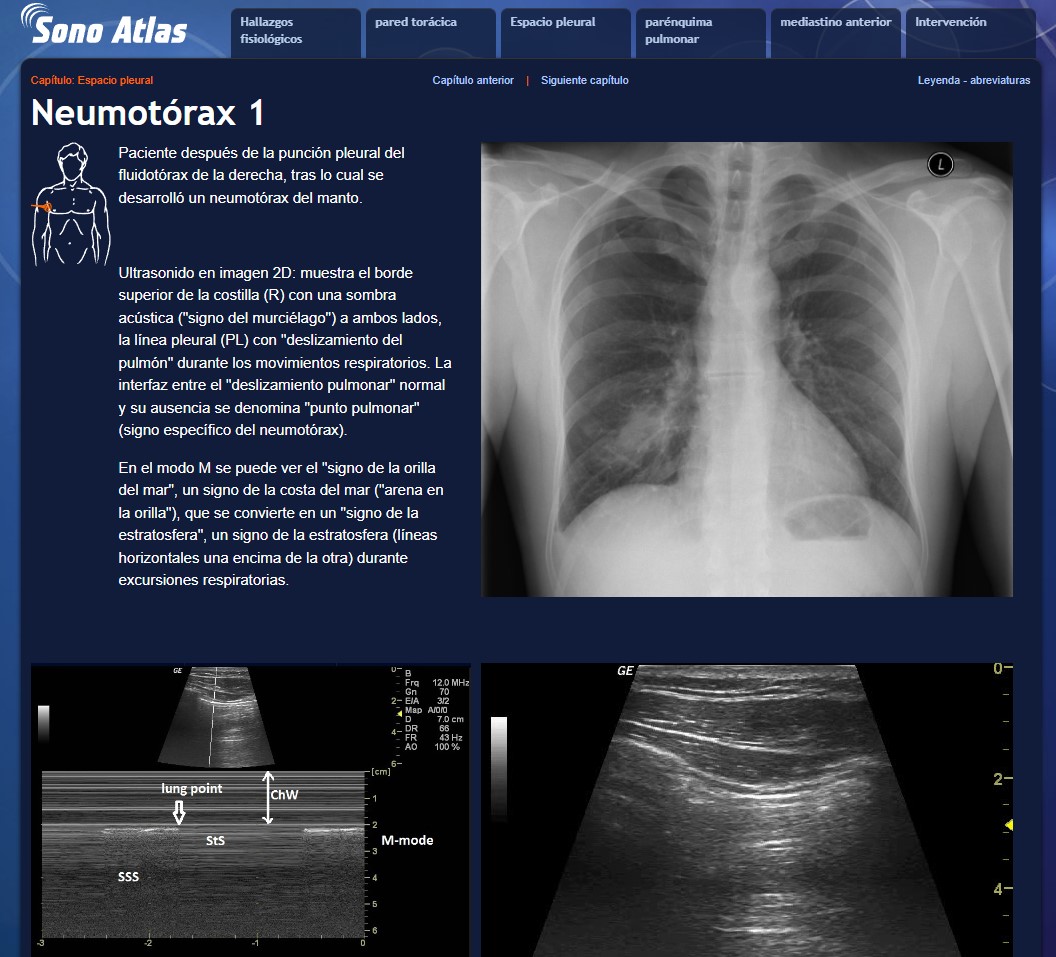
Español
Elizabeth Bárcena retweetledi

🚩 PRECISe Trial
➡️ multicentre RCT
➡️ High (2.0 g/kg/day) versus standard (1.3) protein provision
➡️ 935 pts within 1st ICU day
➡️ High protein resulted in worse EQ-5D-5L health utility score and no improvement in functional outcomes
CCR Journal Watch
criticalcarereviews.com/latest-evidenc…
English
Elizabeth Bárcena retweetledi

🔴New perspectives in the echocardiographic hemodynamics multiparametric assessment of patients with heart failure #2024Review #OpenAccess
🔹link.springer.com/article/10.100…
#cardiology #CardioTwitter #CardioEd
#MedEd #MedX #heart #cardioEd #CardioTwitter #Cardiology #cardiovascular


English
Elizabeth Bárcena retweetledi

🩸Blood transfusion during #ECMO, ELSO - Extracorporeal Life Support Organization position statement: selected patients may warrant pRBC transfusion to above levels generally accepted in critically ill patients
#FOAMcc #FOAMecmo on @asaiojournal
🔓 bit.ly/4bP5tSm

English
Elizabeth Bárcena retweetledi

European guidelines on peri-operative VTE prophylaxis: first update
Chapter 5: Mechanical prophylaxis
Mechanical prophylaxis aims to prevent VTE by promoting venous flow but improper application of compression stockings may cause complications.
🔗 ow.ly/TGHn50SAgkS
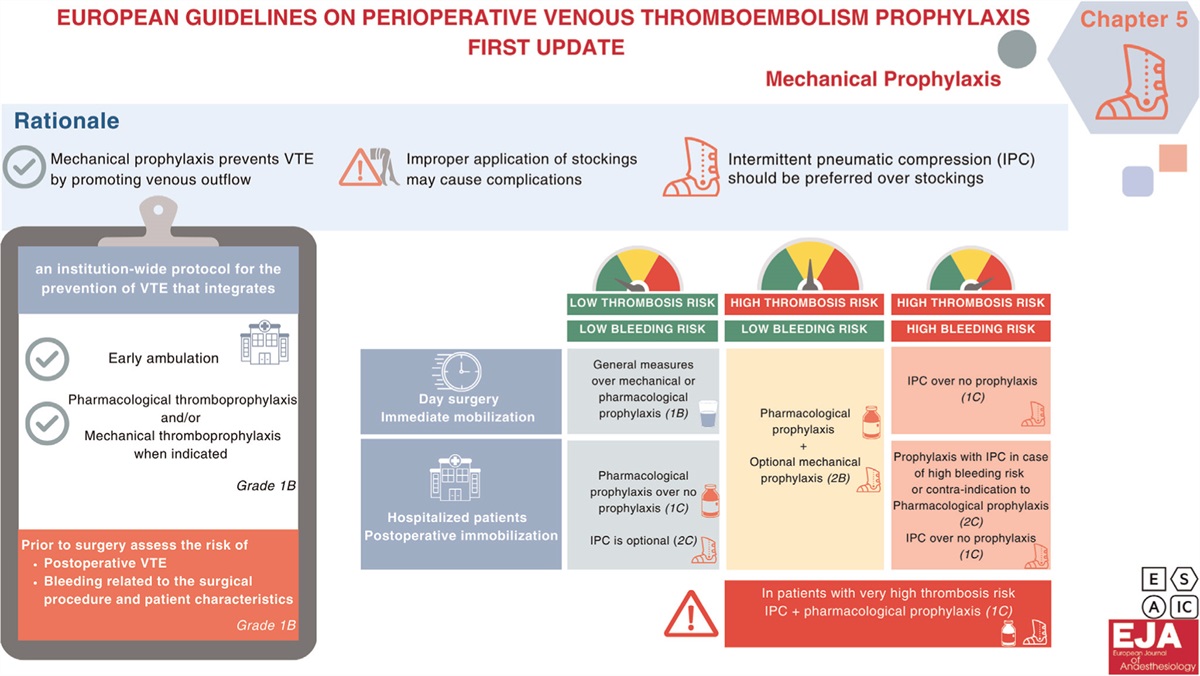
English

@MarcVives13 @EACTAIC @MedUNAV @sedar_es @SCISEDAR @JG_Anestesia @albimar23 @MontesinosSanti Disfrutamos mucho el del año pasado. Anotados 😊 seguro será excelente
Español
Elizabeth Bárcena retweetledi

La II Reunion de la @EACTAIC España” sera los días 12 y 13 de Noviembre online y 15 de noviembre presencial 100% hands-on en el Centro de Simulacion de @MedUNAV.
El link de la web del congreso es:
reunion-eactaic-spain.com
@sedar_es #CardioToVascSEDAR @SCISEDAR @JG_Anestesia

Español
Elizabeth Bárcena retweetledi

European guidelines on peri-operative VTE prophylaxis: first update
Chapter 1: Cardiovascular Surgery
Recommend early initiation (6-24 h) postsurgery of pharmacological VTE prophylaxis in the absence of significant bleeding risk in cardiac surgery.
🔗 ow.ly/8ZtW50Sx7Fm
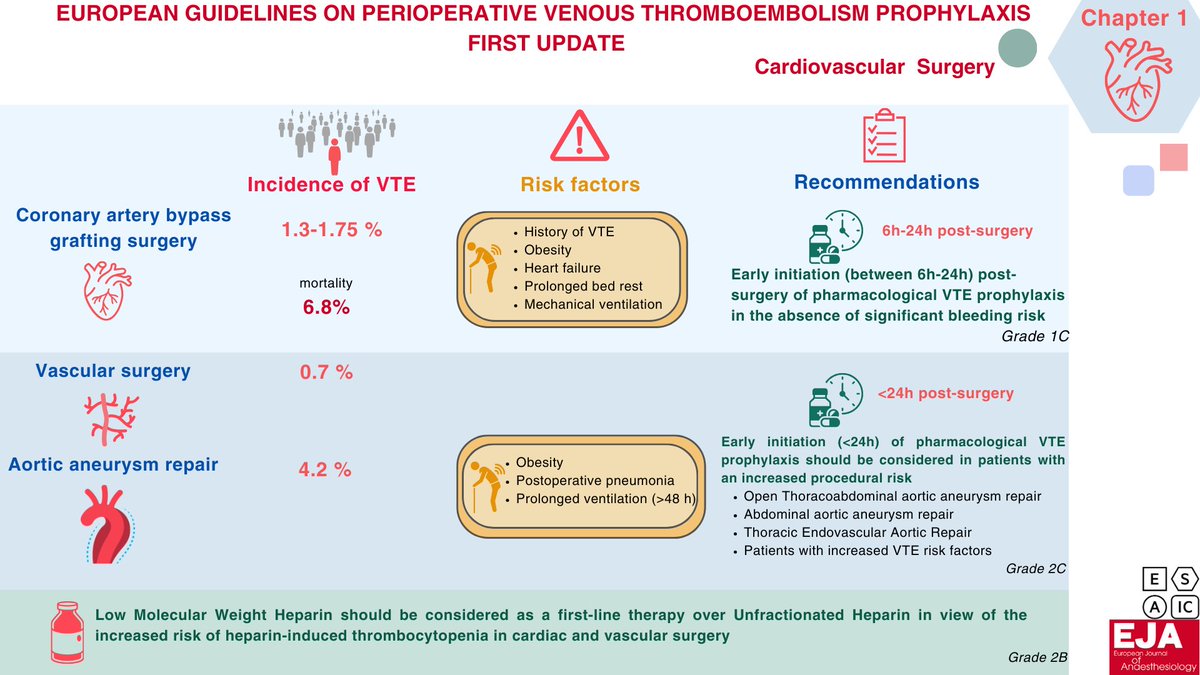
English
Elizabeth Bárcena retweetledi

PAPER OF THE DAY: Summary
The article "Is the NICE Guideline for Maintenance Fluid Therapy in Adults in Hospital Appropriate?" by Robert G. Hahn and Niels Van Regenmortel @icu_nivare evaluates the adequacy of the National Institute for Health and Care Excellence (NICE) guidelines for maintenance fluid therapy in hospitalized adults. The study compares the NICE recommendations with data from the authors' own research to assess their effectiveness in maintaining fluid balance and electrolyte homeostasis.
Key Points
NICE Guidelines Overview:
- NICE recommends 25-30 mL/kg/day of fluid and 1 mmol/kg each of sodium, potassium, and chloride.
- These guidelines are based on older dietary recommendations and may not reflect current needs.
Study Methods:
The authors conducted additional analyses on their own datasets:
- a 48-hour intravenous infusion study with 12 healthy volunteers, comparing high-sodium and low-sodium maintenance fluids.
- the urinary excretion of sodium and potassium from 719 volunteers and patients.
- a diet study on 20 hospital workers to estimate water and electrolyte intake.
Findings:
- Both high-sodium and low-sodium infusions resulted in fluid volume deficits and dehydration.
- High-sodium fluid maintained extracellular fluid volume (ECV) but decreased intracellular fluid volume (ICV) by 1.2 L.
- Low-sodium fluid caused a 1.7 L volume deficit affecting both ECV and ICV.
- Habitual water intake was estimated at 35-40 mL/kg/day, higher than the NICE recommendation.
- Sodium excretion was approximately 2 mmol/kg/day, double the NICE guideline, possibly because the usual dietary sodium intake of the participants is higher than the guideline-recommended amount of 1 mmol per kilogram or 2.3g per day.
Conclusion:
- The current NICE guideline may recommend insufficient water and sodium for adequate maintenance of ECV and ICV.
- Suggested adjustments: increase fluid to 35-40 mL/kg/day, sodium to 2 mmol/kg/day, and maintain potassium at 1 mmol/kg/day.
Clinical Implications:
- Guidelines should be revised to prevent dehydration and electrolyte imbalances in hospitalized patients.
- More frequent monitoring of urinary sodium could improve fluid and electrolyte management.
Limitations:
- This study has used data from healthy volunteers; results may differ in critically ill patients.
- Further research is needed to confirm findings in diverse patient populations.
FULL TEXT: doi.org/10.1016/j.clne…
READ MORE: fluidacademy.mn.co/spaces/1197666…
#FOAMed #FOAMcc #ICU #fluids #maintenance

English






