Mark Fahlen
950 posts

@markfahlen
Solo practice nephrologist in the Golden State, husband, father, swimmer, skier, and landlocked surfer. #nephrology #solopractice #dialysis




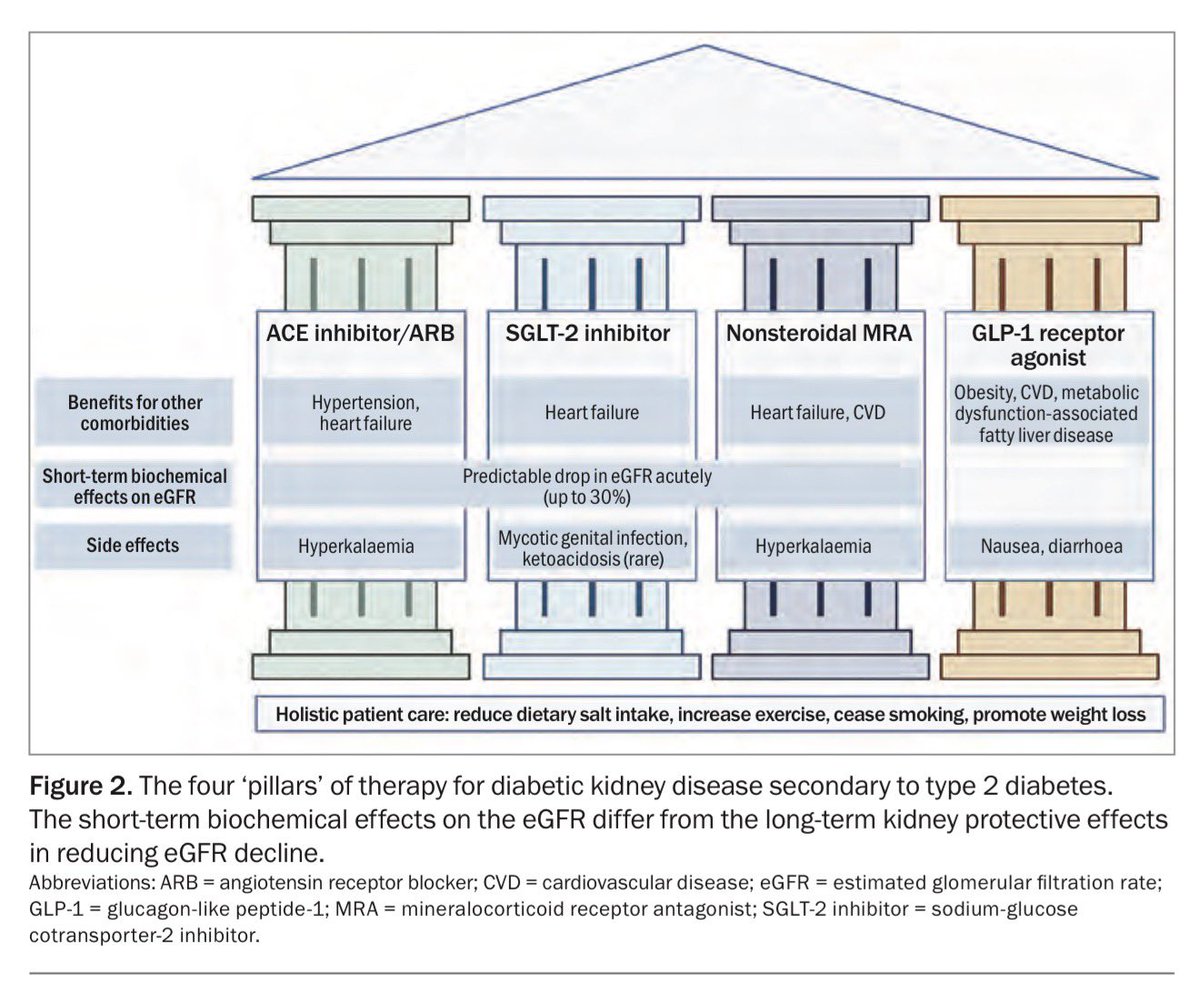
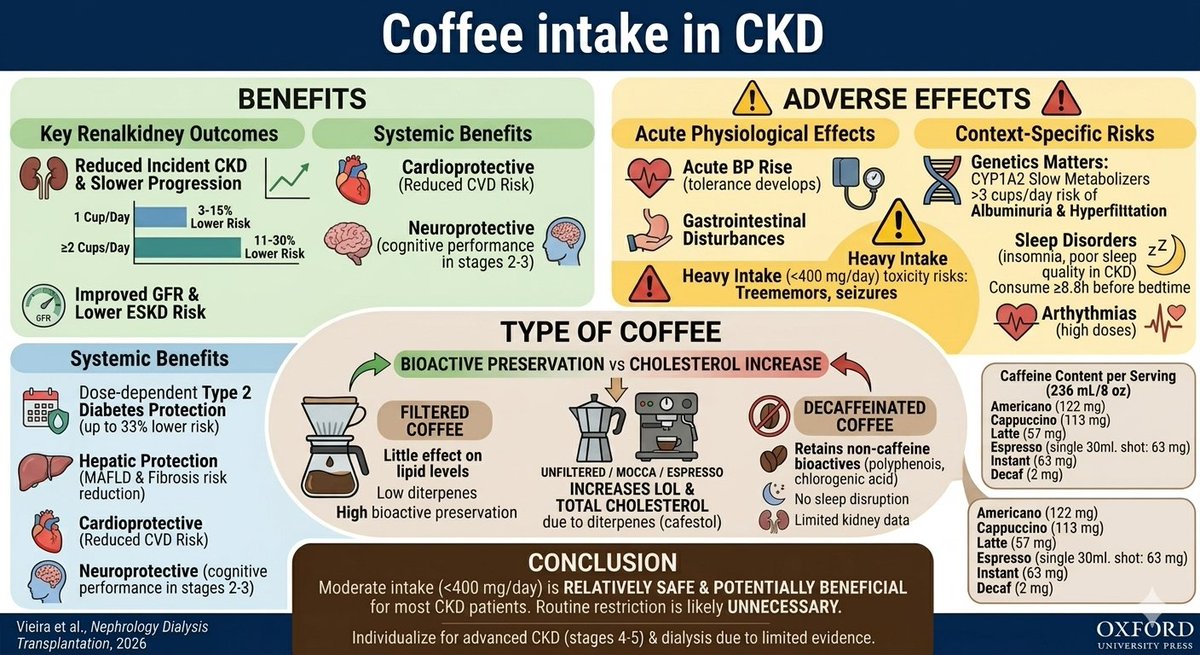
🚰 Hemodialysis is no longer just about diffusion. 💡 The future is convective. #Hemodiafiltration (#HDF) combines diffusion + convection to achieve superior clearance of middle molecules and protein-bound toxins. 📚 Trials like • ESHOL Trial • CONTRAST Trial • CONVINCE Trial suggest better survival and cardiovascular outcomes with high-volume HDF. 🎯 Target convection volume: ➡️ ≥ 23 L/session Why nephrologists are increasingly embracing HDF: ✅ Better middle molecule clearance ✅ Improved hemodynamic tolerance ✅ Better phosphate control ✅ Reduced inflammation ✅ Potential survival benefit “More than filtration. It’s better purification. It’s better care.” #GSR #BuddingNephros #Nephrology #Dialysis #KidneyDisease #CKD #NephTwitter #MedTwitter #HDF
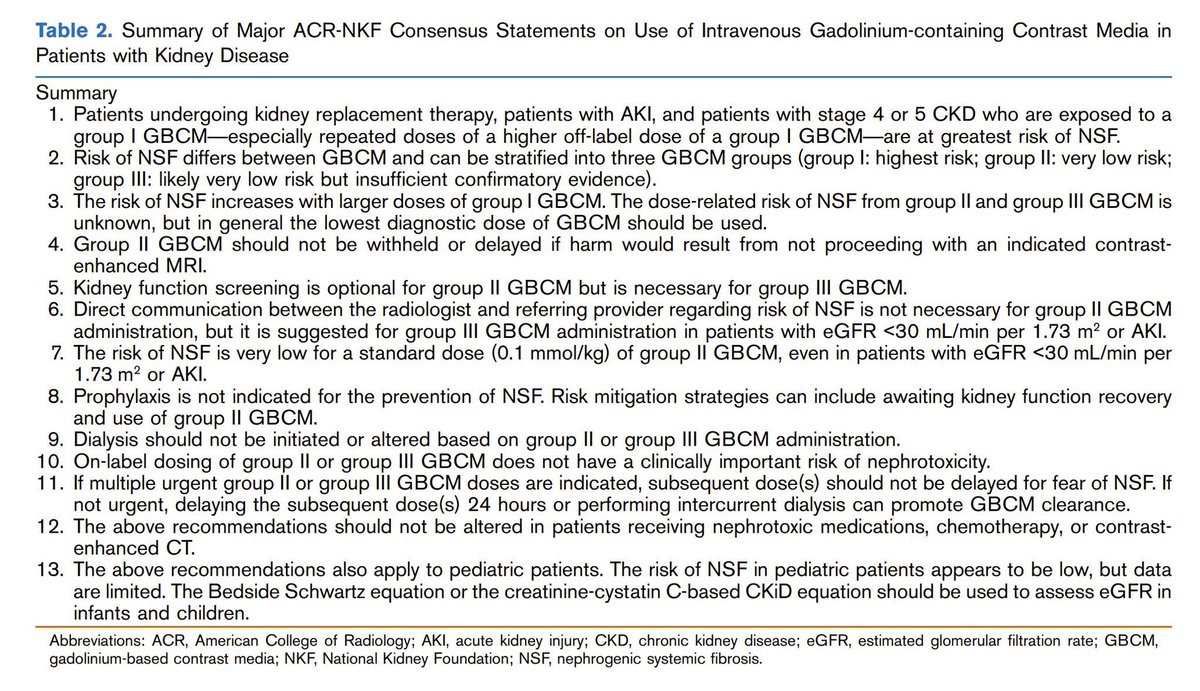




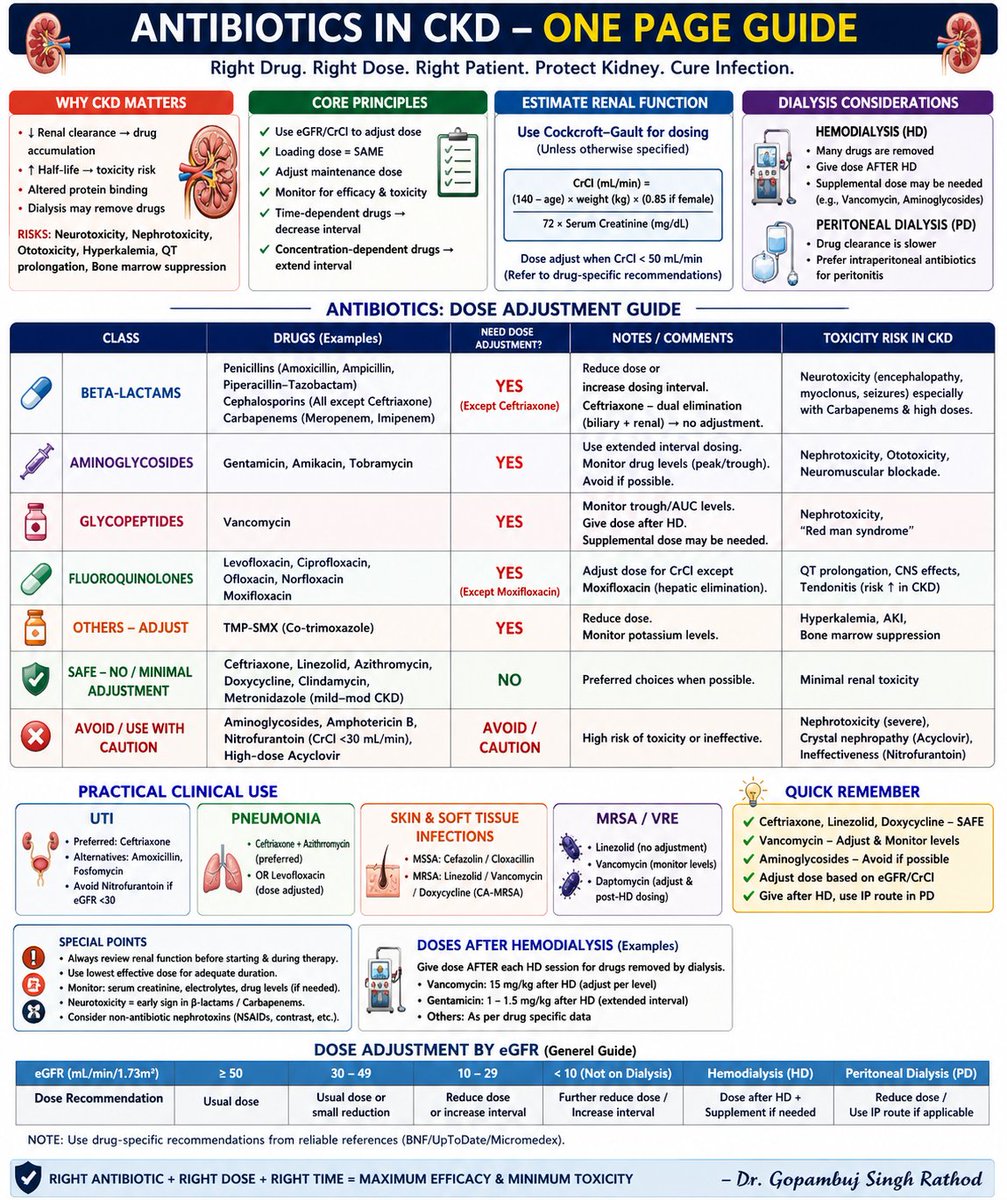







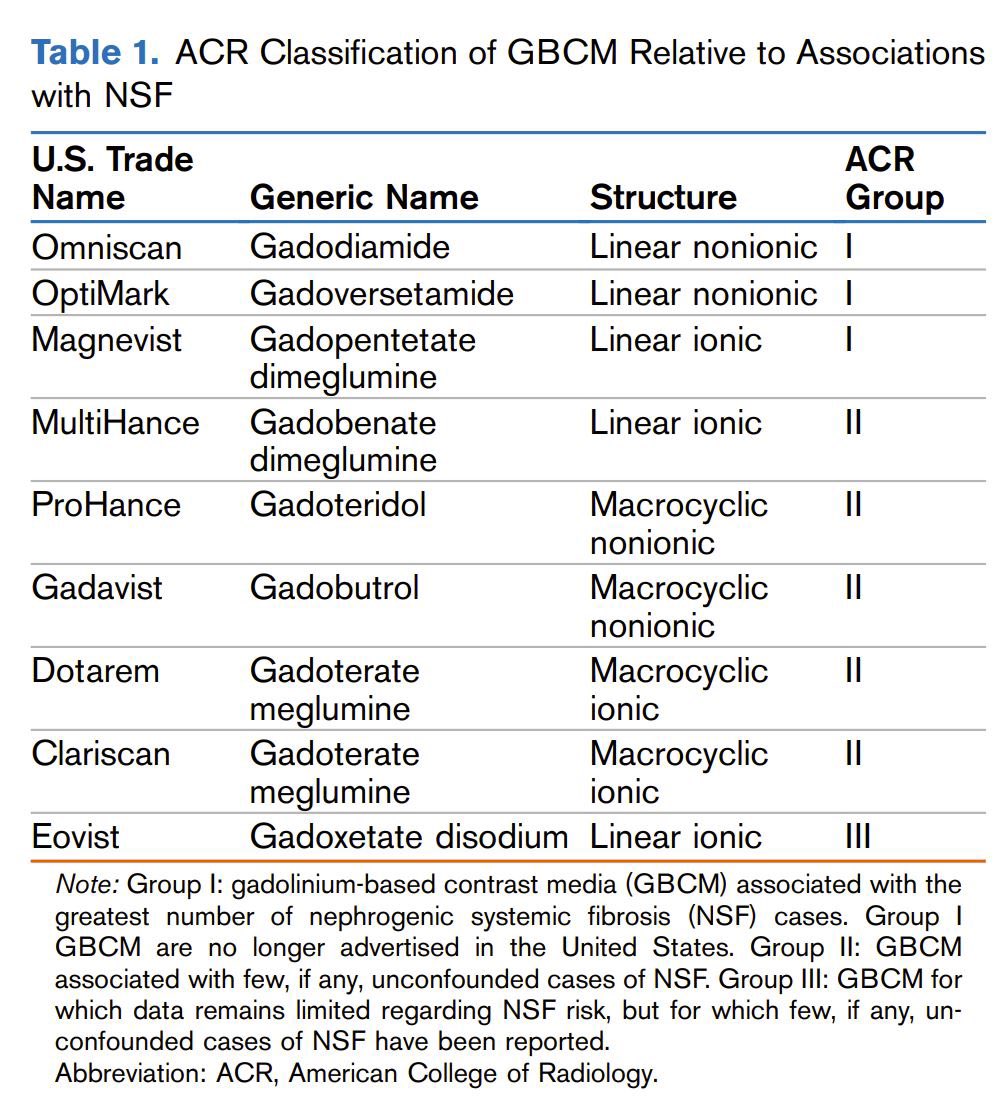

Trick question. Both are safe. Please get the right imaging for your patient when it matters!




🩻Contrast-induced AKI: one of the biggest myths still shaping clinical decisions For decades we were taught: 👉 “Contrast damages the kidneys” 👉 “Avoid CT with contrast in CKD” 👉 “Hydrate, protect, delay imaging if needed” But what if… most of this is wrong?🤔 ->The uncomfortable reality Modern evidence shows: 👉 Low-osmolar contrast rarely causes true nephrotoxicity 👉 Even in CKD, AKI, and ICU patients 👉 The risk is often overestimated—or nonexistent So where did the fear come from? 📍 1950s high-osmolar contrast (actually toxic) 📍 Poorly controlled observational studies 📍 “Creatinine rise = contrast injury” assumption 👉 Correlation became causation 👉 And the dogma stayed ⚠️What recent data tells us ✔ No difference in AKI rates with vs without contrast ✔ No benefit from bicarbonate, NAC, or aggressive hydration ✔ Even ICU and AKI patients show no worsening outcomes ->Translation to real life 👉 The patient was going to develop AKI anyway...Not because of contrast!! ->The real problem: “Renalism” 👉 Avoiding necessary imaging 👉 Delaying diagnosis 👉 Choosing inferior tests And that leads to: ❌ Missed PE ❌ Delayed sepsis source control ❌ Worse outcomes ->Clinical mindset shift Instead of asking: 👉 “Will contrast harm the kidneys?” We should ask: 👉 “Will NOT doing the scan harm the patient?” ->Who still deserves caution? ✔ eGFR <30 ✔ Severe hemodynamic instability ✔ Multiple nephrotoxins Even then: 👉 Optimize volume 👉 Minimize dose 👉 Don’t delay critical imaging 🤓Bottom line ✔ Contrast nephrotoxicity exists… but is rare ✔ The fear is bigger than the risk ✔ The harm of NOT imaging is often greater In critical care 👉 We don’t treat creatinine 👉 We treat patients And sometimes… 👉 The most dangerous thing is NOT the contrast 👉 It’s hesitation. 📃Reference Florens N, Demiselle J. Kidney360 7: 445–449, 2026. doi: doi.org/10.34067/KID.0…