rajEndiran retweetledi
rajEndiran
4.4K posts

rajEndiran
@rdpatho
Visiting Prof. Of Pathology, Sri Ramachandra Institute Of Higher Education & Research
Myrtle Beach, SC Katılım Aralık 2013
1.3K Takip Edilen2.4K Takipçiler
rajEndiran retweetledi

Challenges of staging appendiceal mucinous neoplasms
Mucin outside the appendix in a LAMN case, is it pT4 or not?
-Acellular mucin without inflammatory reaction, mesothelial hyperplasia, or neovascularization is presumed to be a result of carryover during handling or gross examination, and should not be designated as pT4a (Pic A)
- Organizing acellular mucin with neovascularization on the serosal surface is categorized as pT4a (Pic B)
Umetsu et al doi.org/10.1016/j.hump…

English
rajEndiran retweetledi

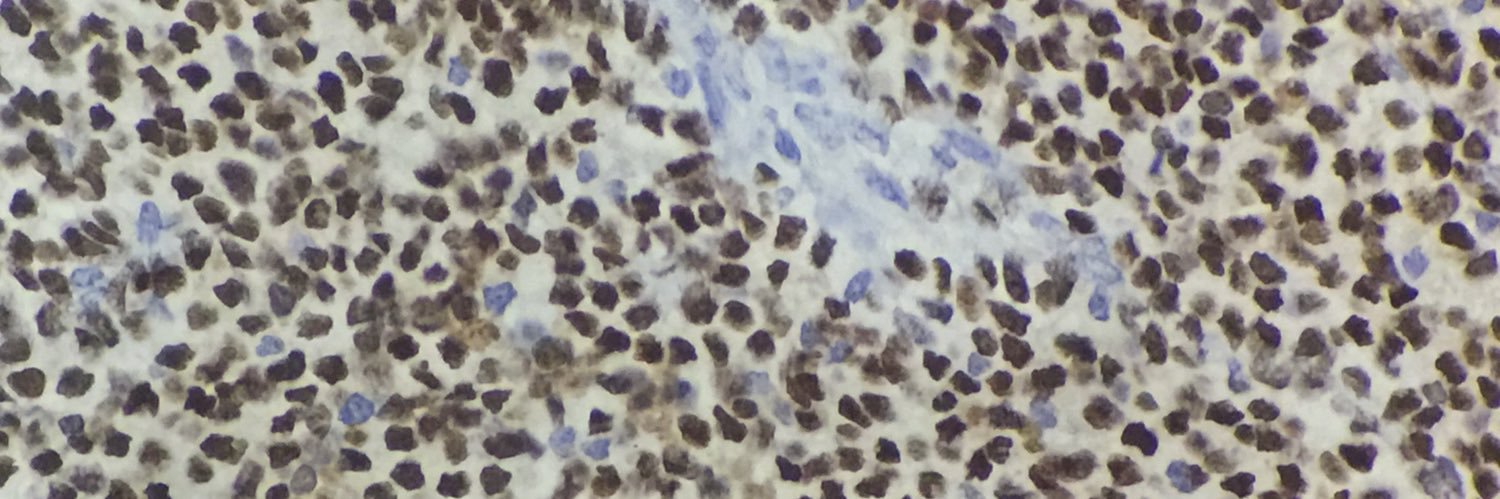
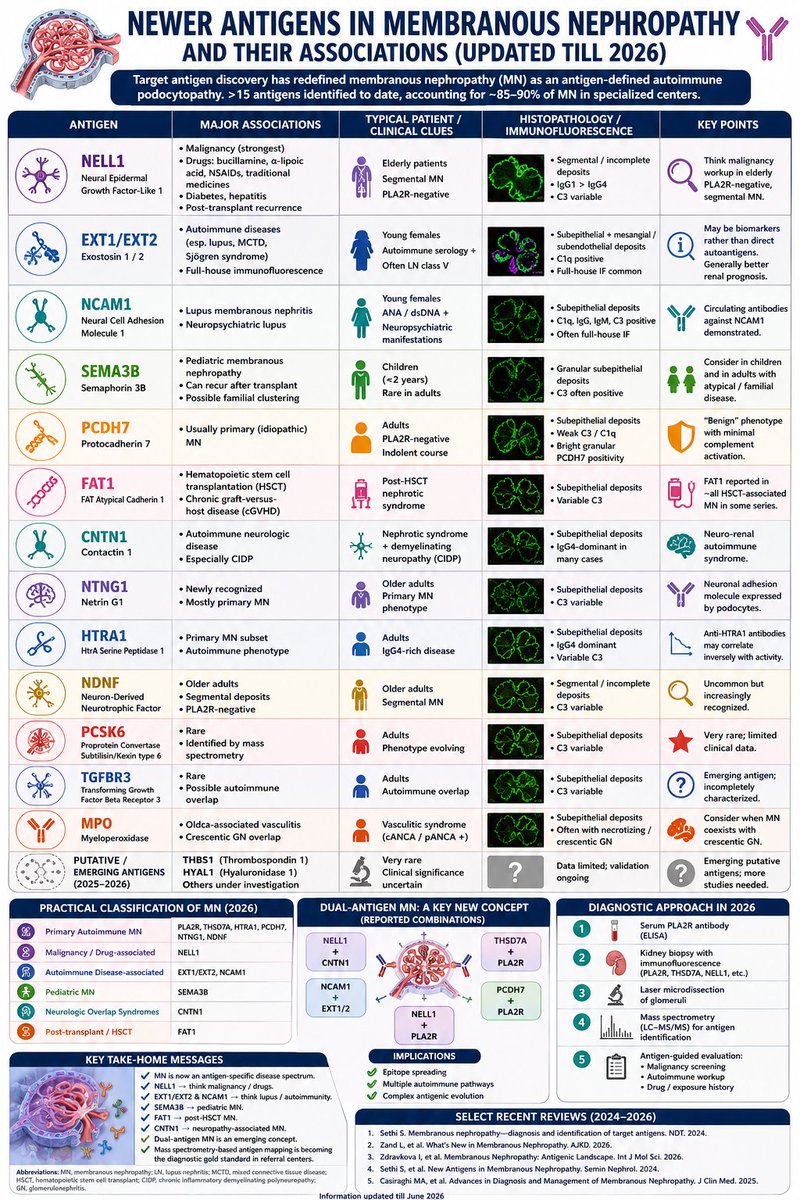
Membranous nephropathy is no longer just “primary vs secondary” disease — it is now an ANTIGEN-SPECIFIC podocytopathy.
🔬 Newer antigens are redefining diagnosis & prognosis:
▪️ NELL1 → malignancy/drug-associated MN
▪️ EXT1/EXT2 & NCAM1 → lupus/autoimmune MN
▪️ SEMA3B → pediatric MN
▪️ FAT1 → post-HSCT MN
▪️ CNTN1 → neuropathy-associated MN
▪️ PCDH7 → indolent MN phenotype
⚡ Emerging concept: Dual-antigen MN
(NELL1+PLA2R, NCAM1+EXT1/2 etc.) suggesting complex autoimmune evolution.
🧪 Mass spectrometry-based antigen mapping is becoming the future gold standard for PLA2R-negative MN.
#GSR #BuddingNephros #MembranousNephropathy #RenalPathology #NephTwitter #MedTwitter
English
rajEndiran retweetledi
rajEndiran retweetledi

🔬 Molecular Pathology of Adipocytic Tumors — High-Yield Map
Morphology 🧫 + genetics 🧬 + behavior ⚠️ in one glance.
Lipoma (HMGA2) → ALT/WDL (MDM2/CDK4) → DDL (JUN).
🎯 Rapid revision for FRCPath | NEET SS
#Pathology #MolecularPathology #Liposarcoma #Lipoma #FRCPath #NEETSS

English
rajEndiran retweetledi

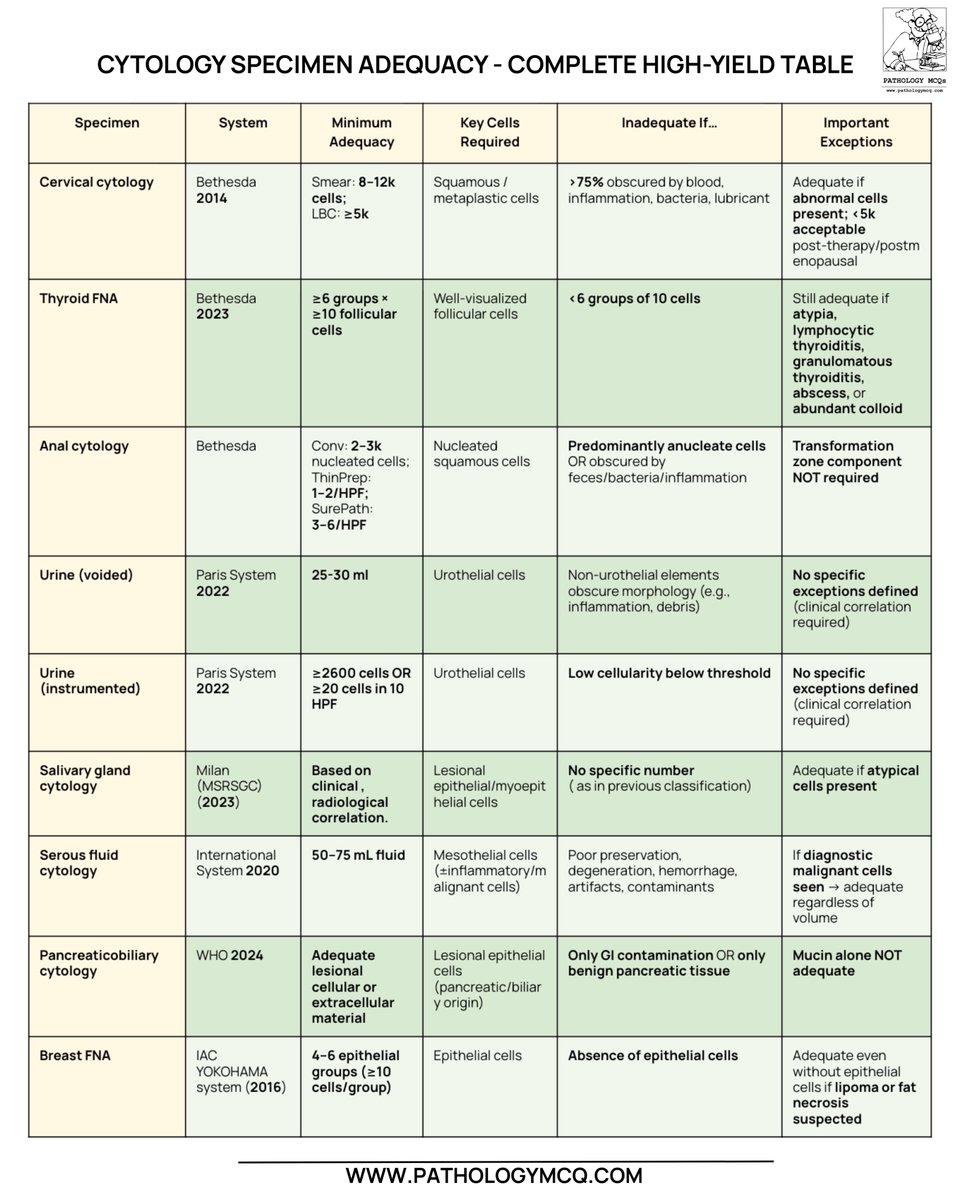
A one-stop revision sheet covering all major cytology systems with crucial numeric cut-offs 🔢, adequacy thresholds ✅, key cellular requirements 🧫, and diagnostic exceptions⚠️
Perfect for last-minute revision ⏱️and quick glance recall 👀
#Pathology #Cytology #HighYield #NEETSS
English
rajEndiran retweetledi
rajEndiran retweetledi
rajEndiran retweetledi

#TooCloseToDiagnose??? #PathQuiz 🔬☀️ #DermPath
A) Bowen disease
B) Actinic keratosis
C) Lichen planus-like keratosis
D) Seborrheic keratosis

English
rajEndiran retweetledi

Interesting case of the week. 63-year-old woman with a “breast cyst”. What do you think? #breastpath #dermpath #surgpath #pathology
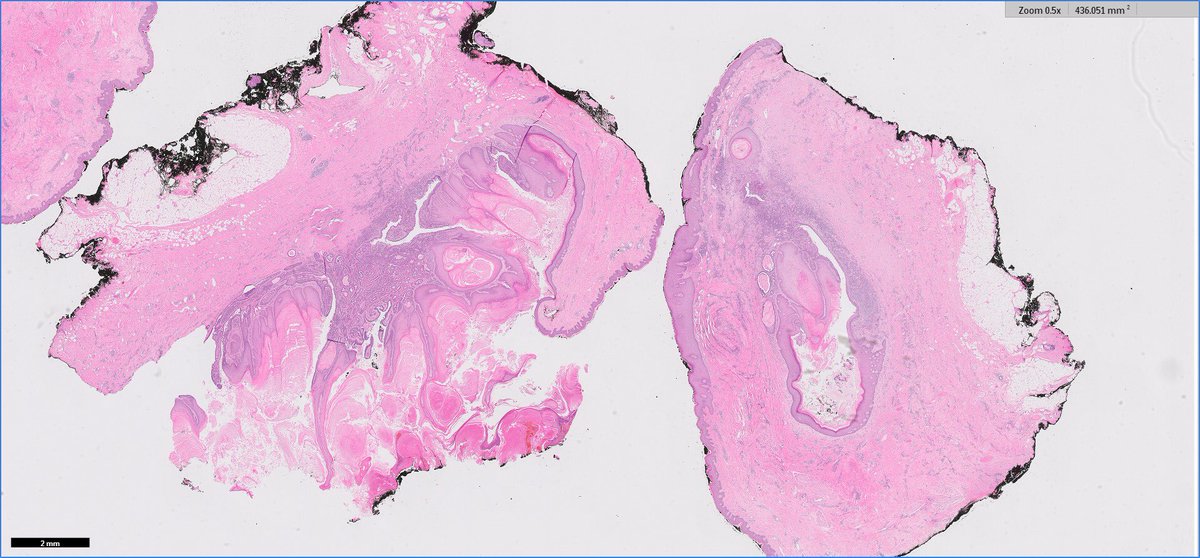

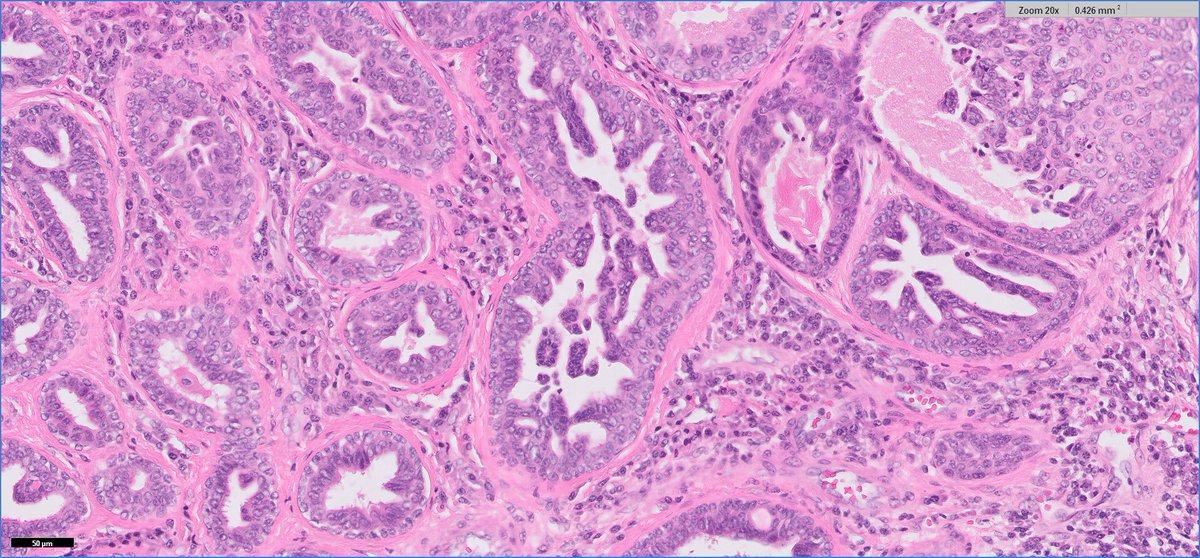

English
rajEndiran retweetledi

#slidearchiveseries vasculogenic mesenchymal tumor #gupath #pathtwitter #pathoutpic
🔬 neoplastic vessels in smooth muscle stroma
1️⃣ post-ChT resections of primary mediastinal GCT with YST components
2️⃣ risk of sarcoma
3️⃣ risk of leukemia/myelodysplasia
pubmed.ncbi.nlm.nih.gov/33136584/
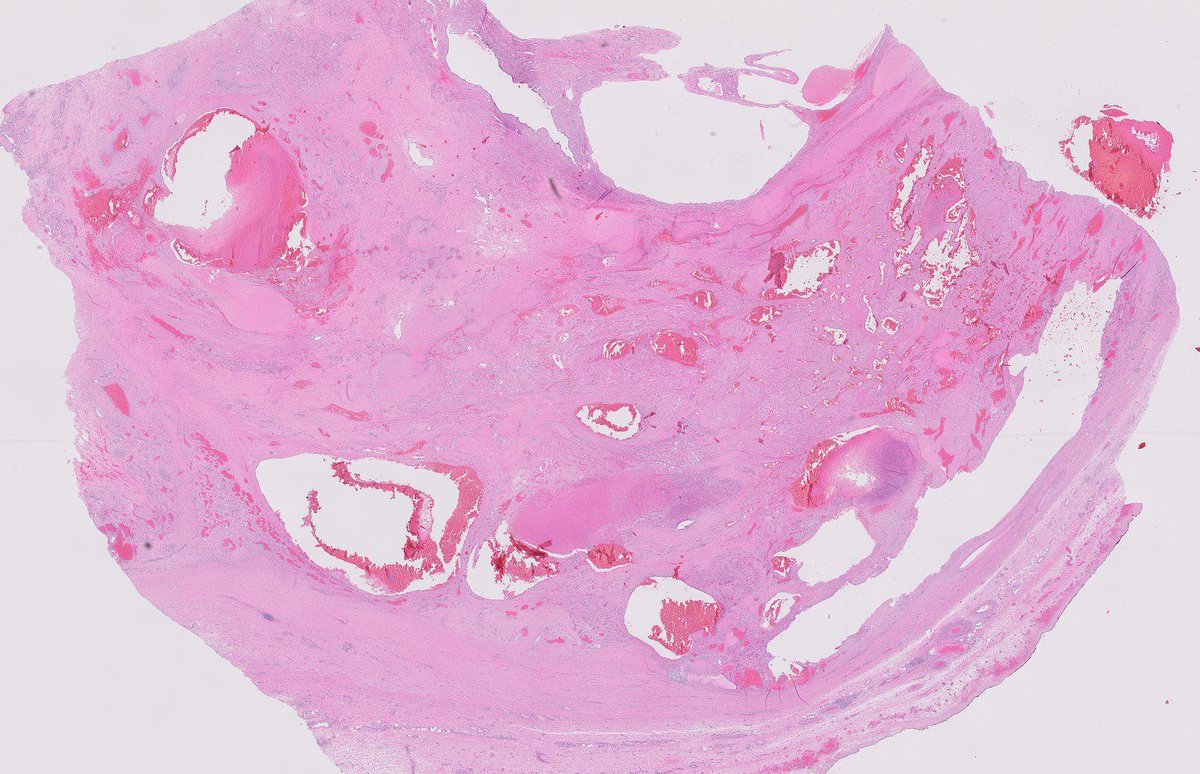



English
rajEndiran retweetledi

rajEndiran retweetledi

Hey! A short illustration on the approach of #lymphoma! Hope it may help! #pathology #pathresident #pathognosis

English
rajEndiran retweetledi
rajEndiran retweetledi
rajEndiran retweetledi
rajEndiran retweetledi
rajEndiran retweetledi
rajEndiran retweetledi

We recently discussed t(11;14), t(4;14), and t(14;16).
Today—let’s simplify what matters most at the bedside:
👉 t(11;14) = “Leaky myeloma” 💧
👉 t(14;16) = “Sticky myeloma” 🧲
Yes… leaky vs sticky.
💧 t(11;14) — LEAKY
• CD56 negative → no adhesion
• Cells don’t stay in marrow → spill into blood
• PB involvement, EMD more common
🧠 Think:
No glue → no home → they wander
🎯 Biology: BCL-2 dependent
→ Target the protein (venetoclax)
🧲 t(14;16) — STICKY
• MAF → adhesion molecules + IL-6 signaling
• Early disease: locked in marrow niche
• Protected, hidden, therapy-resistant
🧠 Think:
Glued in place… safe for now
💥 Then evolution happens:
→ Lose niche dependence
→ Break out → aggressive EMD
🎯 The big difference:
• t(11;14) → escapes early
• t(14;16) → escapes late… and worse
⚡ Clinical translation:
• Leaky → target the vulnerability (BCL-2)
• Sticky → disrupt the environment + multi-agent therapy
🧠 If you remember one thing:
💧 If it leaks → shut the valve
🧲 If it sticks → break the niche
✍️ Dr Fun + G
#myeloma #hemetwitter

English
rajEndiran retweetledi

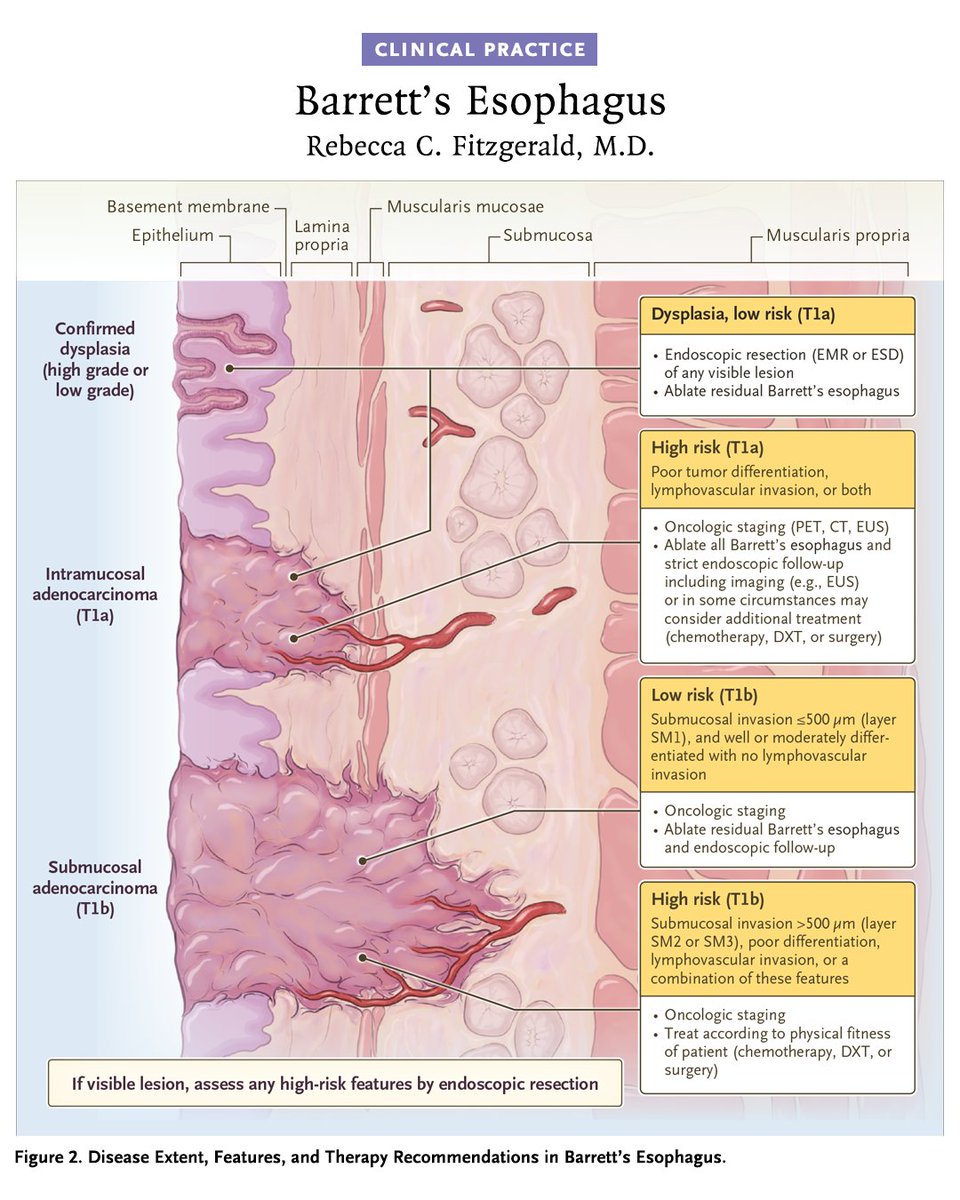
A new Clinical Practice article summarizes the pathogenesis, diagnosis, and management of Barrett’s esophagus, a reflux-related condition with increased adenocarcinoma risk, highlighting endoscopic diagnosis, surveillance, and early curative therapy.
Read “Barrett’s Esophagus” by Rebecca C. Fitzgerald, MD (@RFitzgerald_lab), from the University of Cambridge (@cambridge_uni): nejm.org/doi/full/10.10…
#Oncology
English