Selvan Ramsamy
2.5K posts




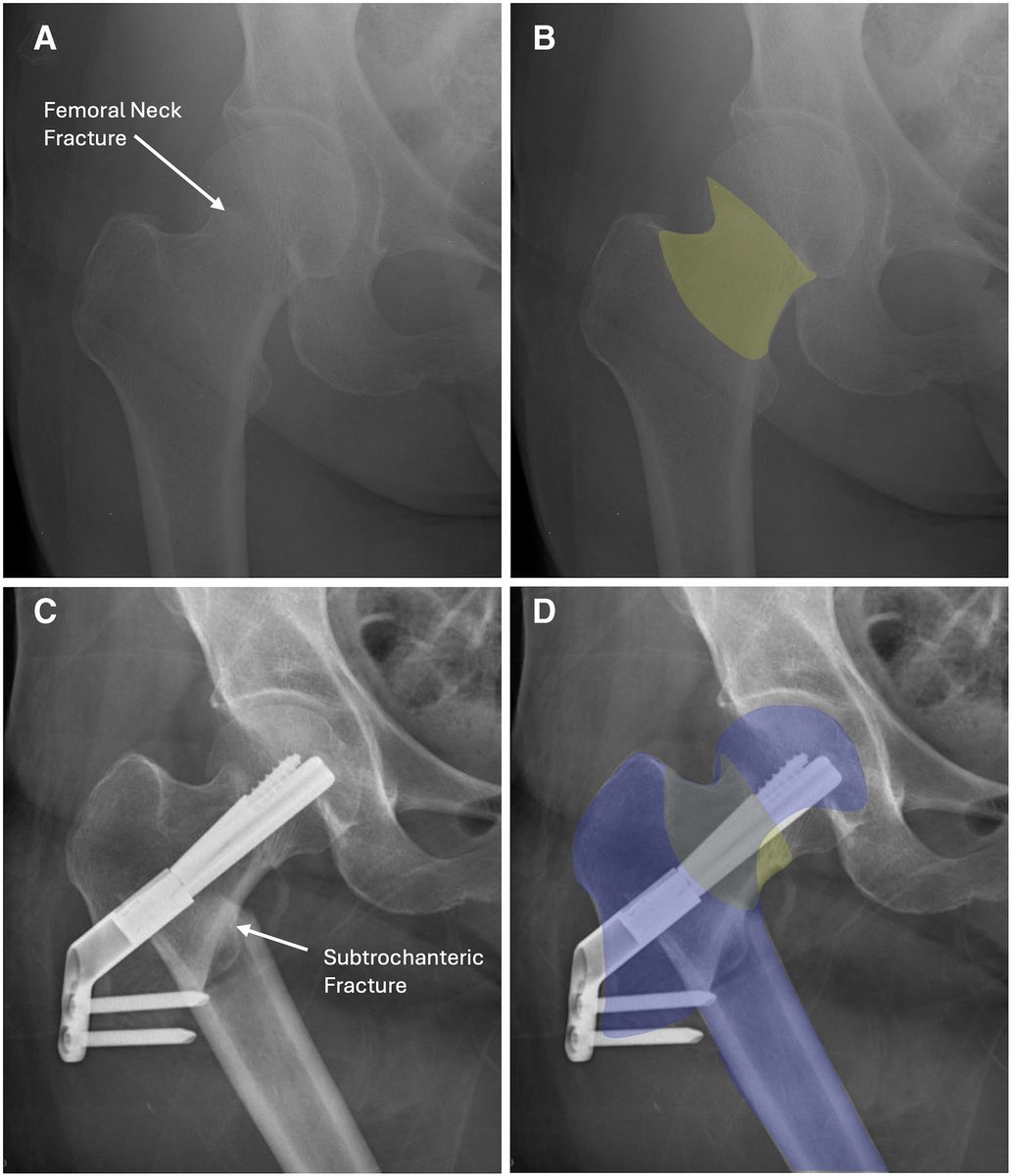





What is considered a high-value basic ultrasound-guided regional anaesthetic technique? #anaesthesia #regionalanaesthesia #regionalanesthesia #pain #MedTwitter doi.org/10.1111/anae.7…




Here's a humdinger.... "Assessing the incidence of ‘can see, cannot intubate easily’ during routine use of C-MAC videolaryngoscopy." Is it a real problem - with a MacVL - with a HAVL Well basically no! Another cracking science letter from the team @anaesthesia @Fionafionakel @mhillier93.bsky.social …-publications.onlinelibrary.wiley.com/doi/epdf/10.11…

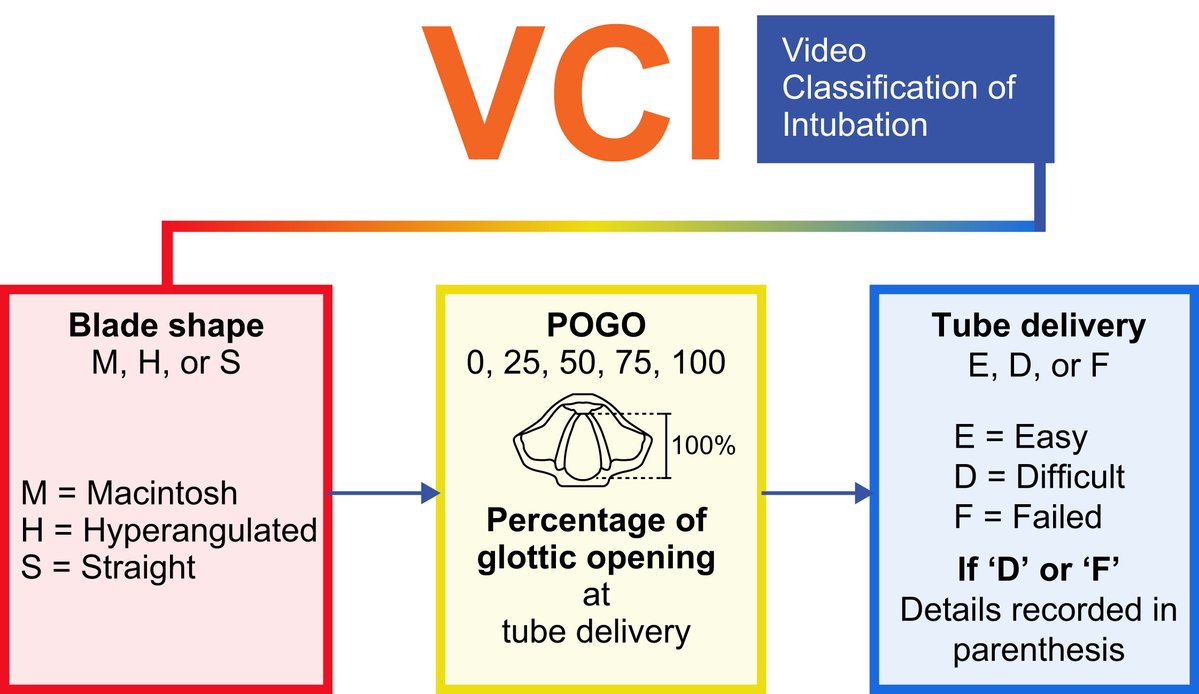
Introducing the #VCIscore: a reliable, standardised tool for reporting #videolaryngoscopy-assisted #trachealintubation. High inter-rater agreement means better data and safer care. Read more: bjanaesthesia.org/article/S0007-…