Special Interest Media
510 posts


Special Interest Media
@thoughtson_tech
Thoughts on healthcare markets and technology. Read our newsletter for free and paid essays on healthcare entrepreneurship, investing, technology & regs.













B2B SaaS is dead. Time to sell outcomes not tools.


















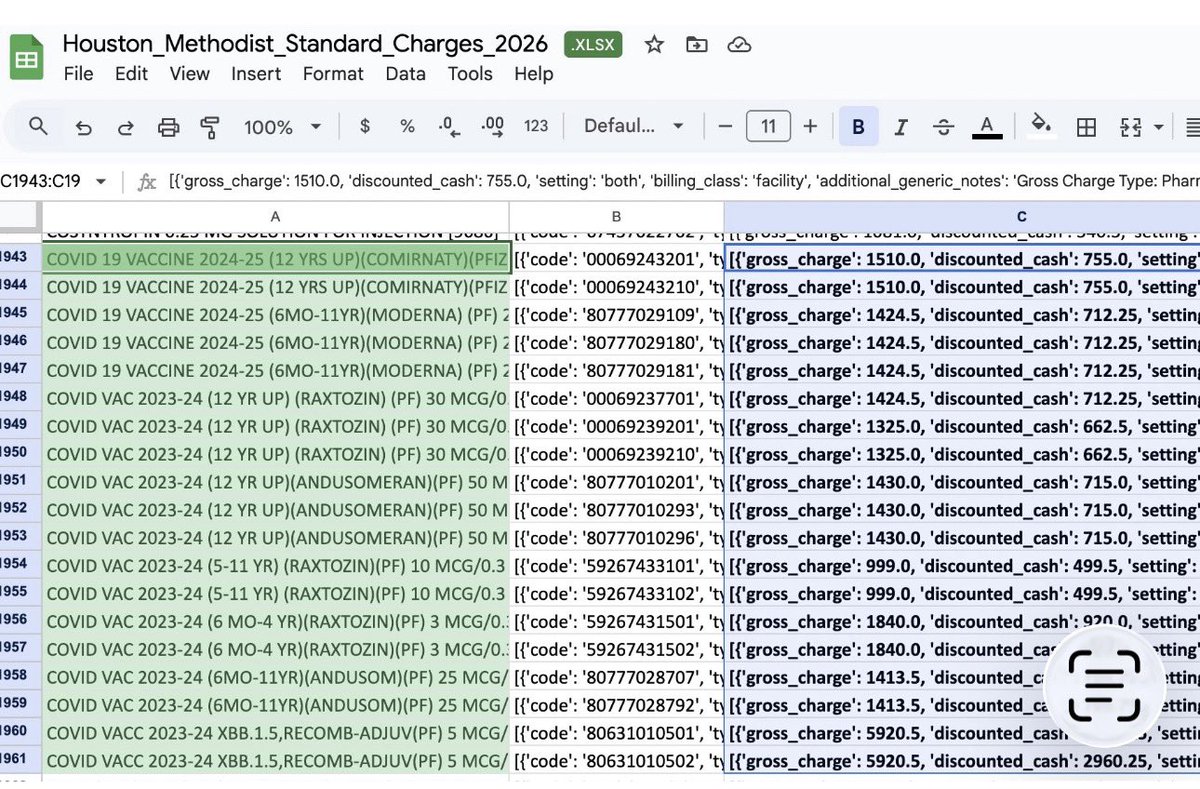
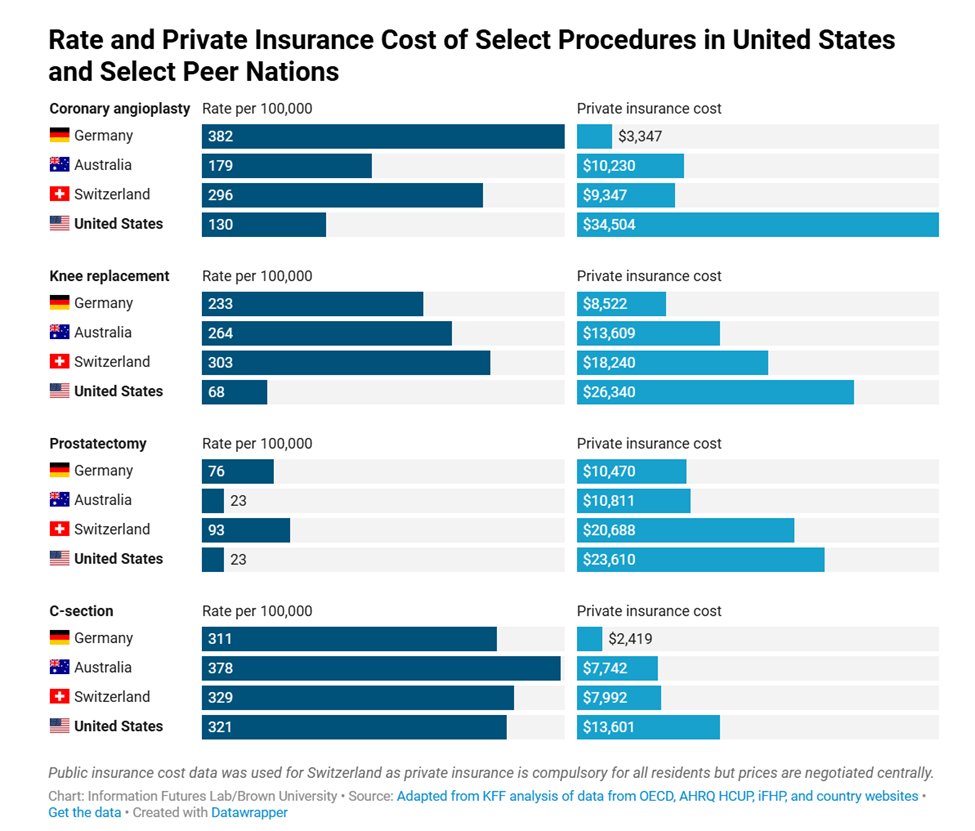
At today’s Health hearing on health care affordability, @HouseCommerce Republicans expressed concerns over the consolidation of health care providers and the lack of price transparency for patients. We are working to implement meaningful solutions that deliver more affordable health care to all Americans. Read more about today’s hearing ⬇️







Watch Chairman @RepMGriffith gavel in today's hearing on the role of providers in getting Americans access to affordable care. Health care providers play a critical role in caring for Americans across the country, but over time, they have formed localized monopolies, driving up cost and reducing choice.




There is no issue with physician-led hospitals- the issue is about the conflict of interest when physicians self-refer patients to their own hospitals. The data is clear: POHs tend to treat more commercially insured and healthier patients than full-service hospitals. In rural communities, this can leave rural hospitals with a greater financial burden, further threatening their ability to keep their doors open and keep 24/7 care available in their communities. Read more: fah.org/wp-content/upl…