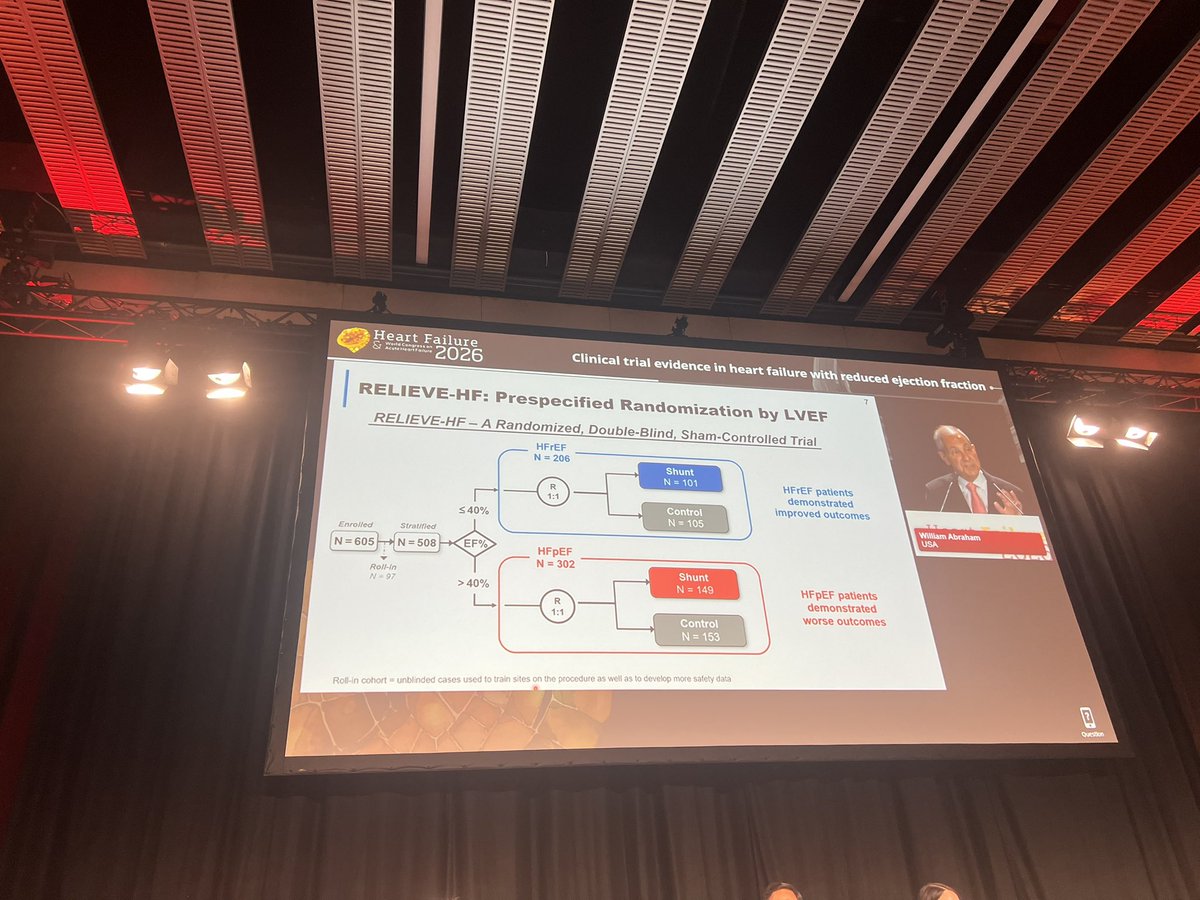
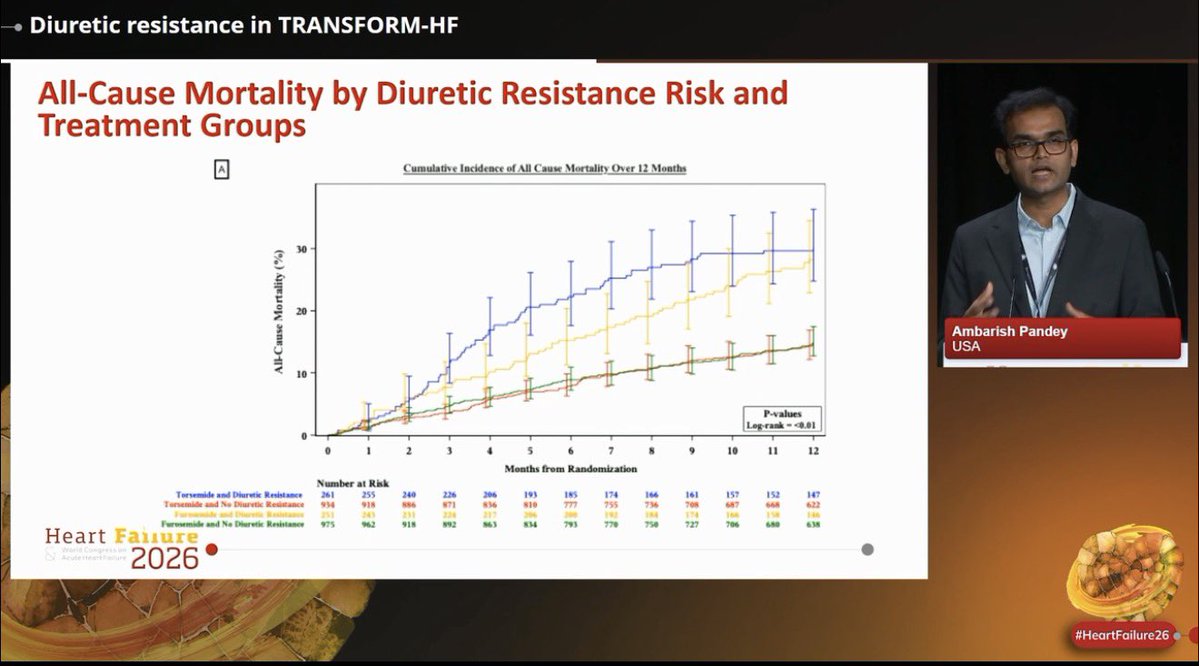
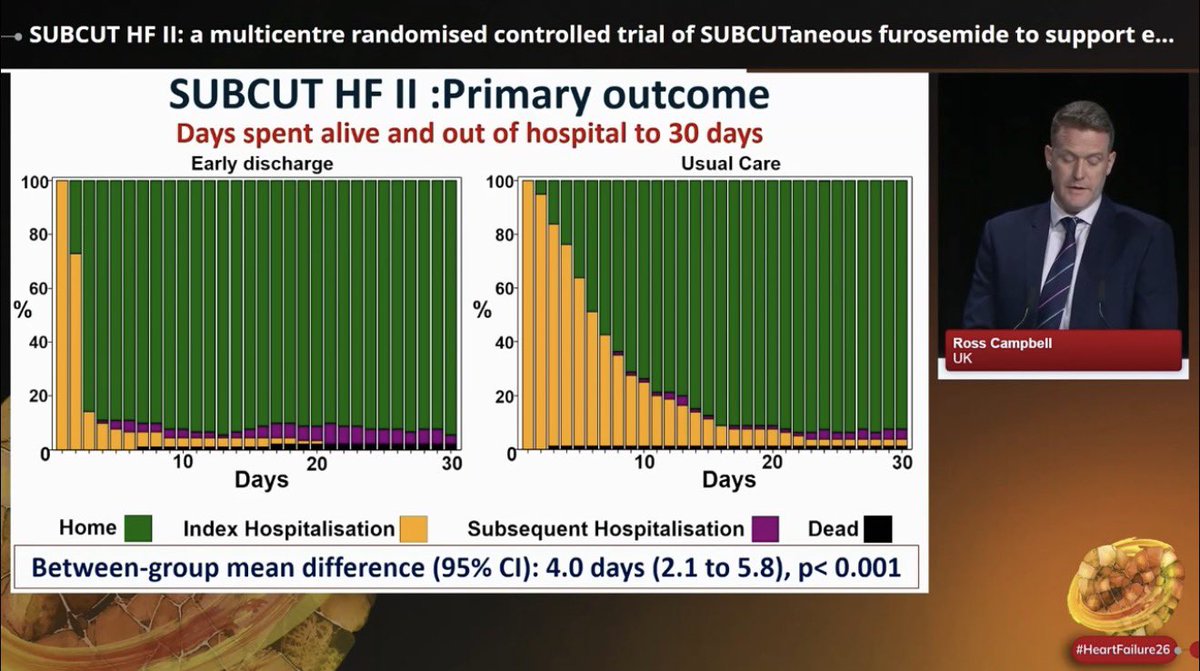
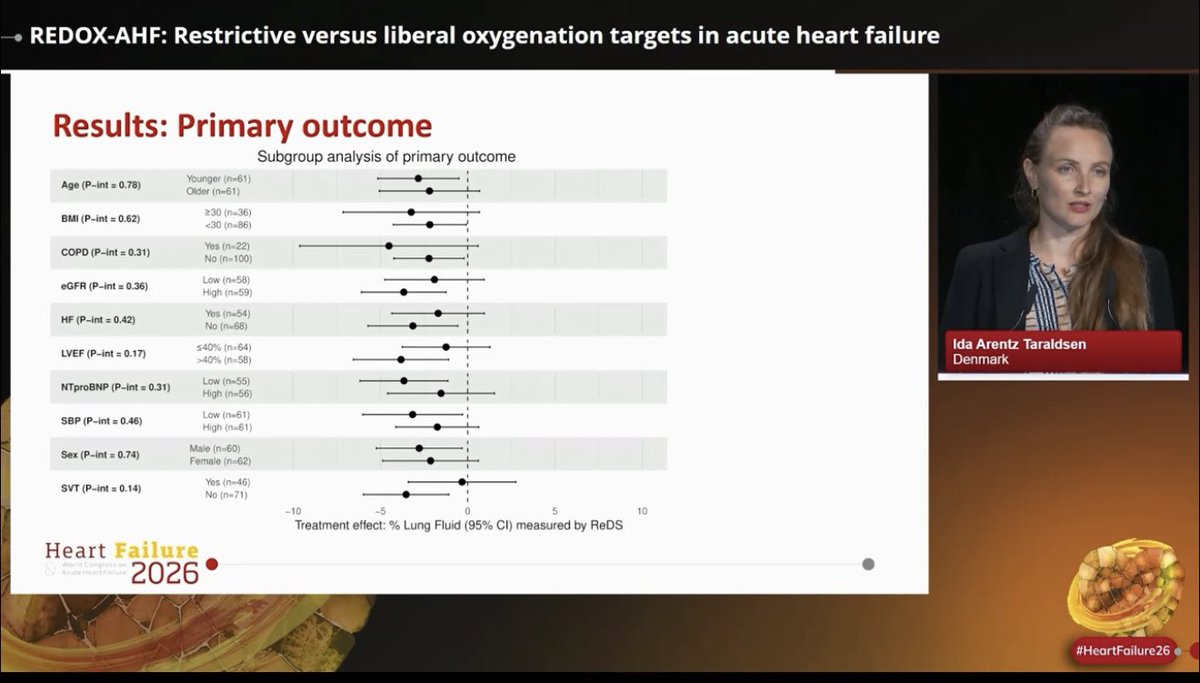
Mark it down ➡️ June 6, 2026 💙 Duke Heart Failure Symposium - The South-East Meeting on ALL around the topic of Heart Function, Implementation and Innovation. World-class faculty and exhibitors are guaranteed! Registration page ⬇️ medicine.duke.edu/education-and-…