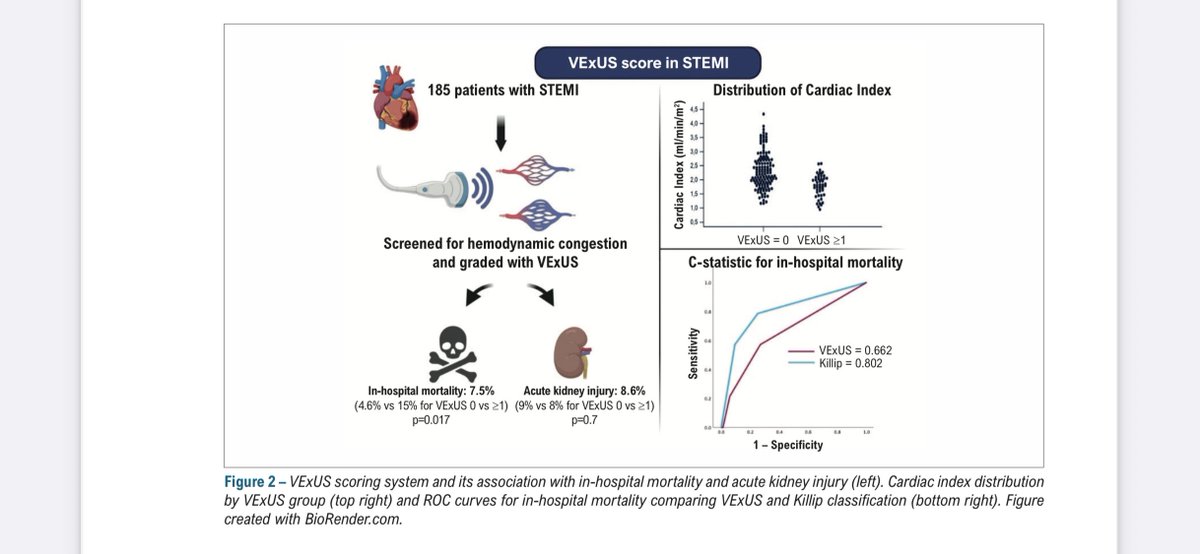
Our FASTEMI study is now published! 🎉 This quick and practical POCUS protocol in STEMI can be truly decisive: it guides management, identifies critical differential diagnoses, and achieves a 97% negative predictive value for in-hospital mortality. rdcu.be/eRSkX