Tom Kaier
4.1K posts


Tom Kaier
@tomkaier
Interventional Cardiologist #CTOPCI, MBA, PhD in Cardiac Biomarkers @[email protected]


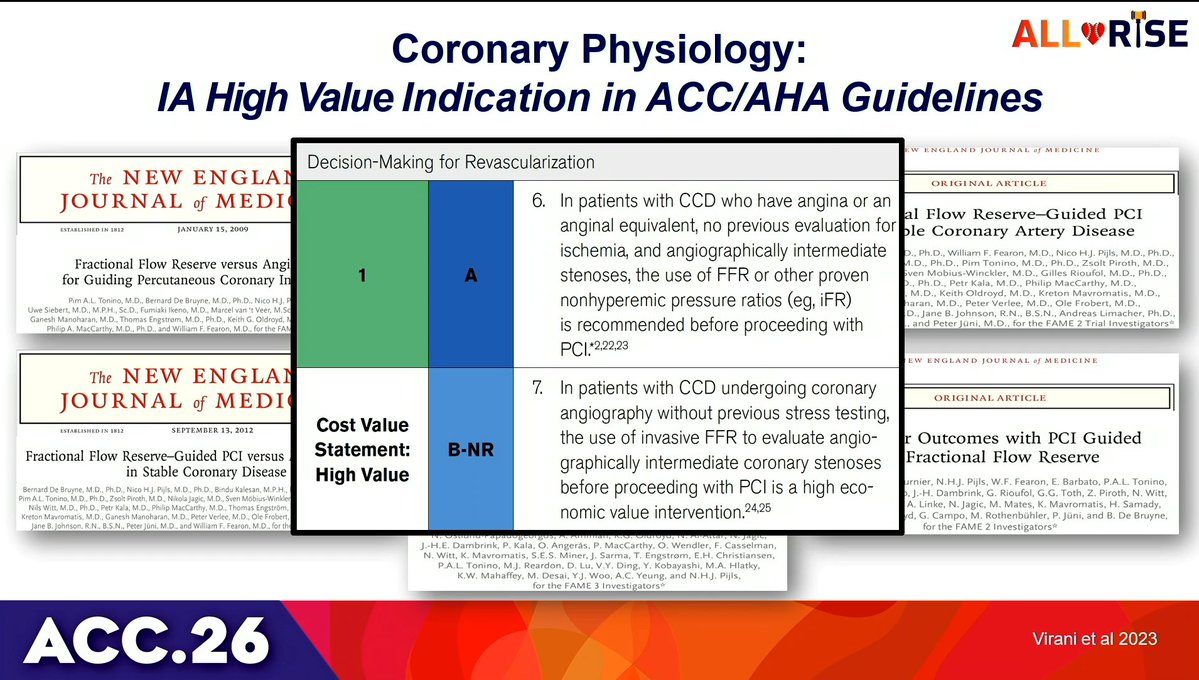
My thoughts on IVUS-CHIP & OPTIMAL Yes, I'm also still digesting the results from IVUS-CHIP and OPTIMAL. I think we all are. And I understand why we as a community are having some trouble sitting with these results. But first, I have to disclose my conflicts of interest: I'm a proctor and speaker for Boston Scientific, specifically for CHIP interventions. I've been doing this for years. So yes, I have skin in this game too, and these results challenge some of my own deeply held beliefs about how we do interventional cardiology. That's exactly why I think we owe it to ourselves to think clearly here, not defensively. So let's look at what happened. IVUS-CHIP: HR 1.25 (0.97–1.60). OPTIMAL: HR 1.11 (0.87–1.42). Two large, well-designed European trials, both published simultaneously in NEJM, both neutral — and both trending numerically against IVUS. That stings. I get it. But here's what's been bothering me about the reaction. The most common defense I keep seeing is: "IVUS-CHIP failed because only 48% of lesions met the predefined optimization criteria." And I understand the instinct — if the intervention wasn't properly delivered, how can we judge it? Fair enough. But let's check the receipts. ULTIMATE — the trial we all love to cite as proof that IVUS works — achieved optimization in 53%. RENOVATE — arguably the strongest positive IVUS trial we have — achieved ~58%. OCTIVUS — 55% in the IVUS arm. IVUS-CHIP: 48%. Do you see the problem? The difference is marginal, but the way we treat these numbers is completely asymmetric. We celebrate ULTIMATE at 53% as a win for IVUS. We dismiss IVUS-CHIP at 48% as a flawed trial. That's not consistent. Either suboptimal implementation invalidates all of these trials, or it invalidates none of them. We have to pick one. And honestly, I think the real answer is simpler than we want it to be. Maybe 50–55% optimization isn't a failure of any particular trial. Maybe it's a biological ceiling. Diffuse disease, heavy calcium, tortuous anatomy — there are lesions where clean landing zones simply don't exist, no matter how good the operator or the imaging. Look at the substrates: IVUS-CHIP had 45.8% severe calcification and a mean distal edge plaque burden of 47.6% — nearly failing the optimization criterion by definition. RENOVATE had 13.5% severe calcification and 40.6% distal plaque burden. Same tool, same criteria, vastly different biology. We can't keep blaming the operator when the anatomy won't cooperate. And this leads to an uncomfortable thought: maybe reaching stent optimization criteria says more about the anatomy you're working with than the technique you're using. We can achieve what the vessel allows us to achieve — nothing more. Better anatomy = higher optimization rates = better outcomes. That's not IVUS working better. That's easier disease behaving better. And if that's true, then the positive trials may have been telling us more about their patient population than about the tool itself. There's another criticism that deserves pushback: "In OPTIMAL, operators only acted on IVUS findings in about 30% of cases — so IVUS wasn't really used." But let's be fair here. A diagnostic tool can't do anything by itself. It depends entirely on how we react to what it shows us. And saying that operators "didn't act" in 70% of cases assumes there was something to act on. We don't actually know that. Maybe the result was already good. Maybe the IVUS confirmed what the operator had already achieved by angiography alone. And if that's the case, it doesn't indict the tool or the trial — it tells you something important about operator quality. These weren't operators ignoring IVUS. These were operators who were already so good that IVUS had nothing left to add. Now, here's the part that I think nobody really wants to say out loud: maybe IVUS already won. Not by proving superiority in a trial — but by making us better operators over the past decade. Look at the post-dilation rates in the angiography arm across the major IVUS trials: ULTIMATE 57%, RENOVATE 75%, IVUS-CHIP 84.5%, OPTIMAL 96%. Look at that progression. Operators who've used IVUS routinely for years have internalized everything it taught them — sizing, post-dilation, POT, landing zone selection. When they get randomized to the angiography arm, they turn off the screen, but they don't turn off the IVUS-calibrated brain. POT in 85% of cases. Systematic post-dilation. Aggressive sizing. The control arm in these trials isn't naive angiography. It's IVUS without IVUS. So the real comparison isn't imaging vs no imaging. It's formal IVUS vs the knowledge that IVUS has already embedded into how we practice. And when the gap between those two narrows to nothing, the incremental benefit of the screen disappears. That's not a failure. If anything, that's graduation. To be clear: this does NOT mean IVUS is useless, and it certainly doesn't mean you should stop using it. What it does mean is that in expert European centers — with operators who've spent years calibrating their eyes with imaging — the marginal gain of formal IVUS guidance over their IVUS-informed angiography is effectively zero. One thing I'd genuinely like to see from both trials: the same analysis ULTIMATE did — outcomes in patients who actually achieved optimization criteria vs those who didn't. In ULTIMATE, that landmark analysis showed TVF of 4.2% vs 9.2% (HR 0.44). That was the strongest argument we had that when IVUS-guided optimization is truly achieved, it works. If IVUS-CHIP and OPTIMAL show the same pattern, the conversation changes entirely: the problem isn't IVUS — it's that we can't implement it fully in half the patients. And if they don't show that pattern, we need to accept that too. But here's the pill I think we all need to swallow, myself included: we can't keep invoking "optimization failure" only when results disappoint us. 53% in ULTIMATE = proof IVUS works. 48% in IVUS-CHIP = proof the trial was flawed. That's not how science works. That's narrative fitting. And we're better than that. #CardiologyX #IVUS #PCI #OPTIMAL #CHIPIVUS #ACC26




I know I keep going on about this, but solar and battery storage is ace. If you’re in a position to have it, it’s a no brainer. Our old, outdated and modest system has produced over 45,000kWh since installation and our battery allows us to power shift to 98.7% cheap rate energy, which is now 5p/kWh thanks to @OctopusEnergy Plug-in solar will 100% help also. Germany have over 1.2 million units registered with phenomenal success. The same will happen here. This will save you money.