Mitopapi 🧬🕊️
6.9K posts


@Mitopapi
God First☦️ | All Things Health Optimization, Chronic Illness Help & Sovereign Enlightenment | DM to work 1:1



I worked with @Mitopapi and @nickfrancisholz for less than 20 minutes on lighting and i knew i had to write this. It's book one of ??? on the basics of lighting yourself for your own content. Some anecdotes, some examples, and some theory. perrduction.gumroad.com/l/contentbasic…








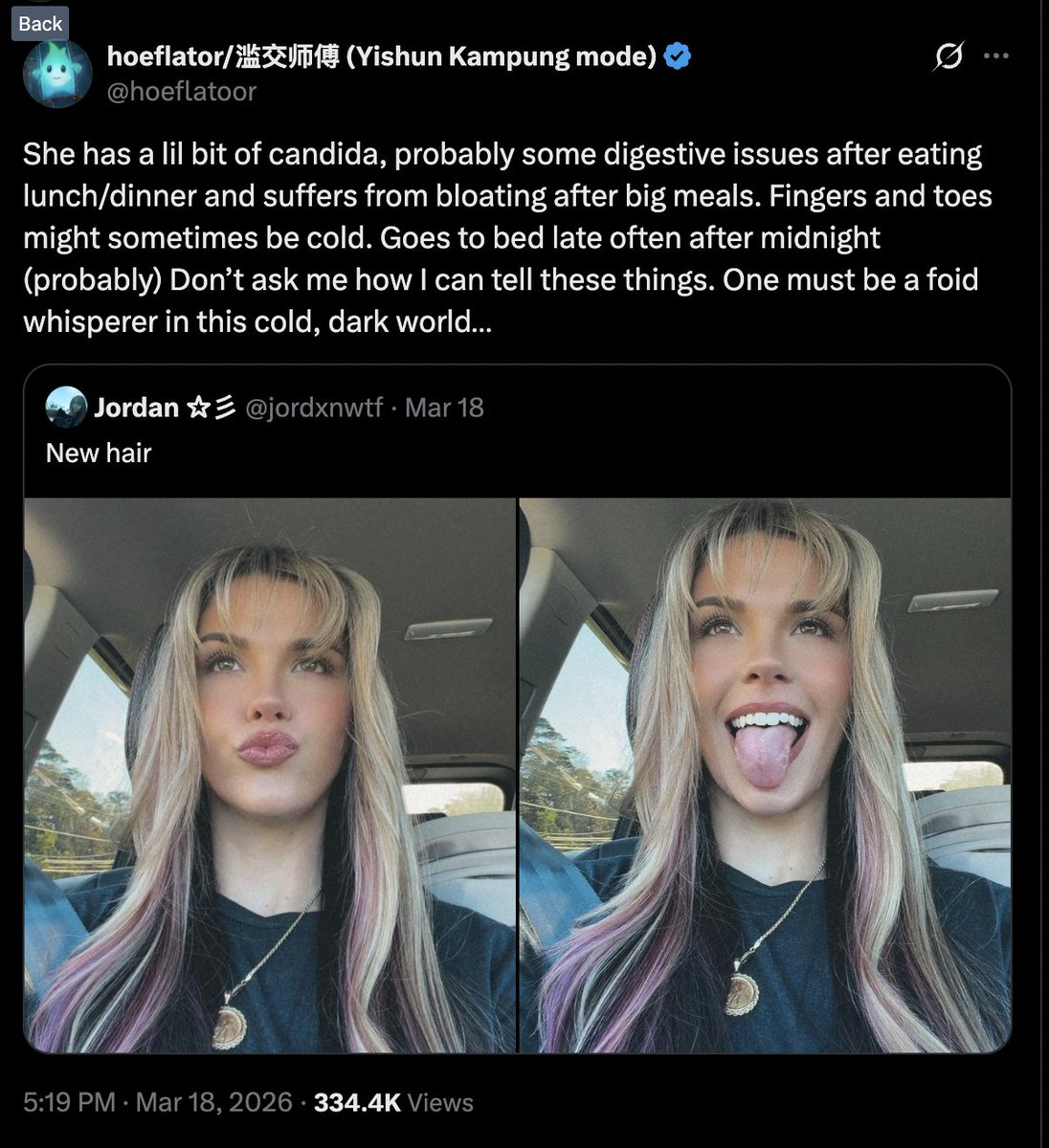
She has a lil bit of candida, probably some digestive issues after eating lunch/dinner and suffers from bloating after big meals. Fingers and toes might sometimes be cold. Goes to bed late often after midnight (probably) Don’t ask me how I can tell these things. One must be a foid whisperer in this cold, dark world…

Got to meet with @Mitopapi and @nickfrancisholz today to look at some sample lighting setups. Nothing greater in the world than showing people what's possible with simple fixture placement.