
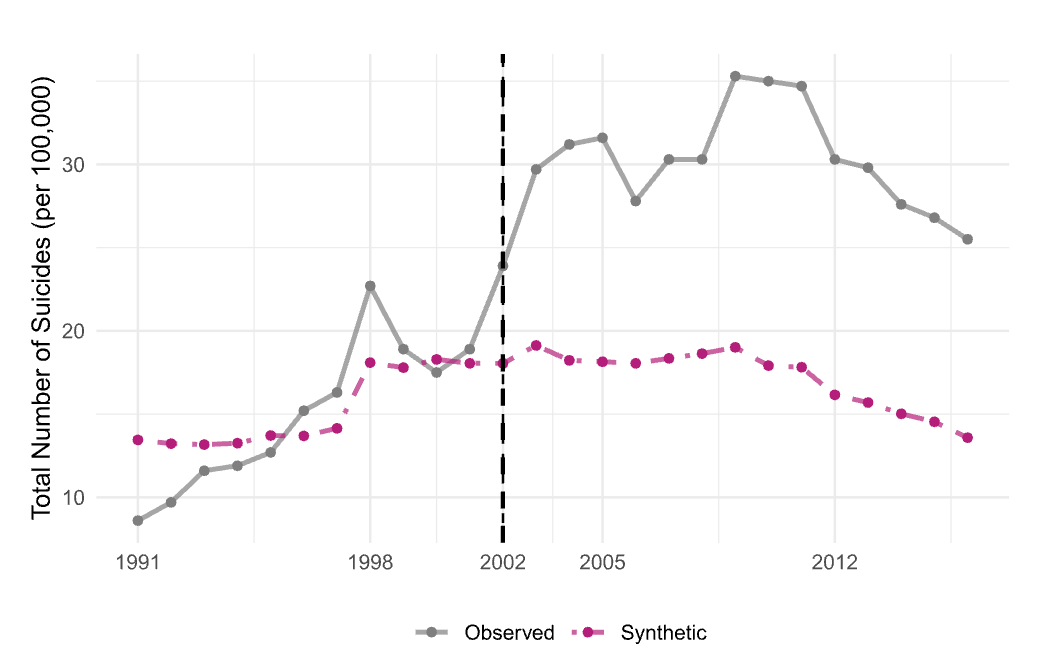
New reporting reveals RFK Jr. is exploring banning certain SSRIs, potentially barring drugs like Zoloft, Prozac and Lexapro. Decades of research shows SSRIs are safe and effective.
Alex Harding
3.3K posts


@AlexHarding7
An internist in biotech


New reporting reveals RFK Jr. is exploring banning certain SSRIs, potentially barring drugs like Zoloft, Prozac and Lexapro. Decades of research shows SSRIs are safe and effective.



This story makes no sense. 2012: Launched w/ $125M & big names 2016: $750M Sanofi R&D pact 2017: $387M Roche R&D deal 2017: GSK R&D pact 2018: Acq'd by another discovery stage biotech in all stock deal w/ just 43 employees it couldn't have burned through all that $$$

For the record, positioning this Warp Drive deal as a win-win begs credulity. endpts.com/six-years-afte…

RevMed is such a cool story. The trip from academia to a failed biotech (WarpDrive) to huge success is a microcosm of the circuitous path often taken in drug development. nytimes.com/2026/05/12/hea… via @NYTimes




Researchers show that a type of #AI known as a large language model often outperformed physicians at diagnosing complex and potentially life-threatening conditions, including decreased blood flow to the heart, even in the fast-moving stages of real ER care when information is limited. In early ER cases, the model identified the correct or a very close diagnosis in about 67% of cases, compared with roughly 50% to 55% for physicians. And the technology is only getting better. Learn more: scim.ag/4w909UX









Honor to work with this team on the oral PCSK9i - Enlicitide. Now in JACC.

⚠️All of the below images were FABRICATED by ChatGPT Images 2.0, each with a single prompt❗️ ⚠️


The effect of current anti-amyloid drugs vs Alzheimer's disease is "trivial" for cognitive function or dementia severity, not clinically meaningful, from a systematic @cochranecollab review of 17 trials, >20,000 patients cochranelibrary.com/cdsr/doi/10.10…