Sabitlenmiş Tweet
Francisco Soto, MD, MS, MBA
809 posts

Francisco Soto, MD, MS, MBA
@FSotoMD
Pulm/CritCare | Division Chief | Chair Pulm Vascular Disease Section ACCP/CHEST | Right🫀Cath Connoisseur |🫀🫁 #Hemodynamics | CritCareEcho | My Opinions
Katılım Ekim 2020
270 Takip Edilen2.1K Takipçiler

2nd Annual Chicago Hemodynamic Forum
@ChiHForum
Outstanding hemodynamic meeting
🔹Not only for Cardiologists, but also
🔹Pulmonologists with interest in Cardiopulmonary Physiology and Interaction
Learning from the masters:
@RyanTedfordMD @JonGrinsteinMD @HFpEF and many more




English
Francisco Soto, MD, MS, MBA retweetledi

Great pulmonary vascular and cardiovascular network meeting this morning at #chest2025 @accpchest
Lots of accomplishments and inspiration!
CHEST Pulmonary Vascular and Cardiovascular@CHESTPulmCardio
Great attendance and meeting of the Pulmonary Vascular and Cardiovascular Network this morning. Dr Shlobin led the session and updated the audience on the superb lectures and activities put together by the network for #chest2025 @accpchest
English

Great insight from @msiuba presentation on invasive CO talk.
Regardless of the love/hate relationship with PAC, can’t expect change in outcomes unless there is an intervention.
If no intervention, remove PAC.
See other pearls 👇🏻
#chest2025 #chestsome @accpchest @CHESTPulmCardio

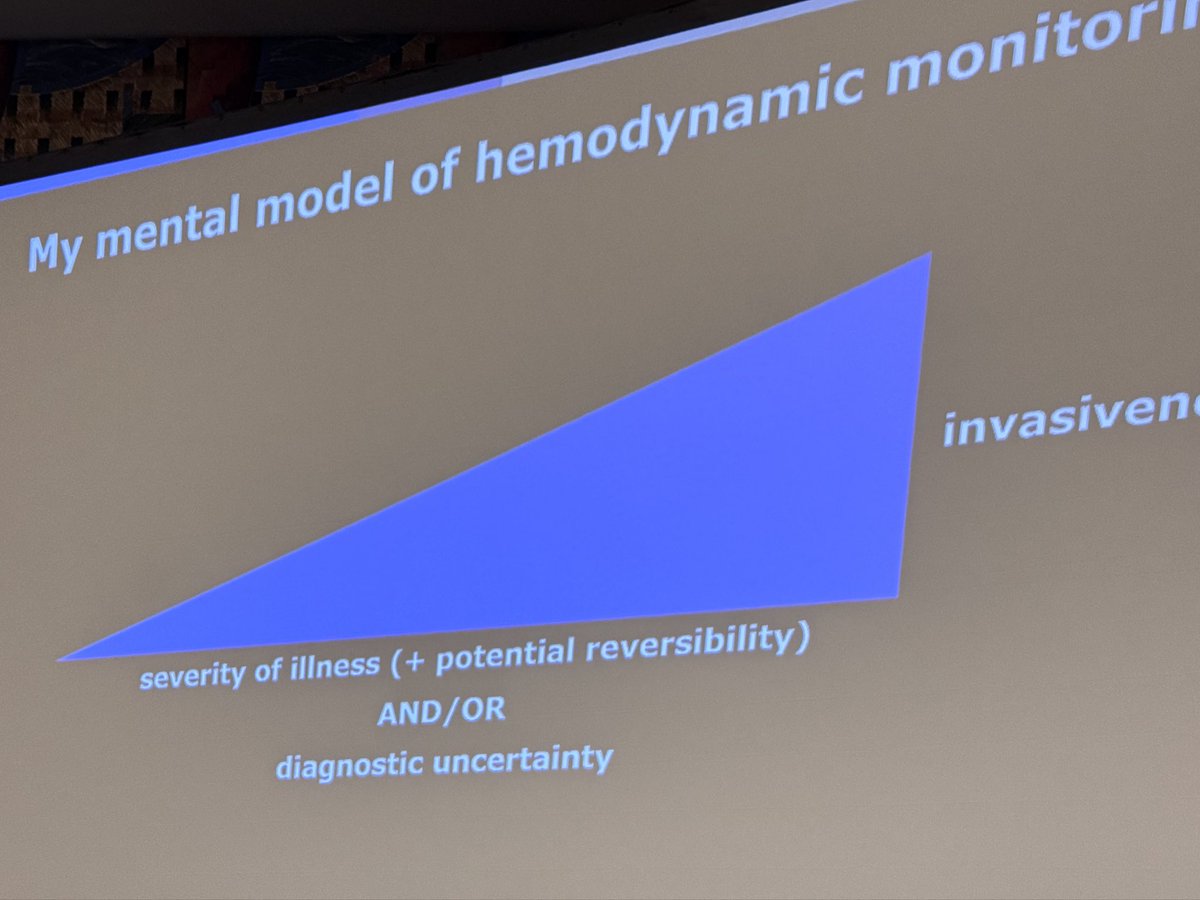


Matt Siuba@msiuba
Key point from my invasive CO talk the other day #CHEST2025
English

Colleague: “I wish I’d find a lecture explaining hemodynamics and cardiopulmonary interaction in an easier way…”
Me: “Wait, aren’t you going to Chicago’s #CHEST2025?
Colleague: “I am, but I don’t want generic concepts. I want to learn how the experts do it.”
Me: Say no more!
We put together an amazing session just for you!
Join us:
👇
🎯 Session Title: "Pulmonary Circulation Advanced Interrogation — How I Do It"
💡 Go beyond routine caths: unmask hidden shunts, interpret difficult wedge pressures, and master fluid/exercise challenges like the experts do.
📅 Tuesday, Oct 21 — 8-9 AM
📍 South Building 503 — Session ID 1067
@accpchest @ChestPulmCardio @ChestCritCare




English

@hraza222 @khaycock2 @NephroP @msiuba To Dr @msiuba point, lack of RAP (CVP) variation is a poor prognostic marker of RV dysfunction in pre-cap PH, something that your pt is showing….
sciencedirect.com/science/articl…
English

Why doesn't this VExUS correlate with the PAC? EF <20 in AKI on CKD, recent angiogram, cardiorenal syndrome. VExUS shows at least mod venous congestion. But the PAC didn't correlate. PCWP 10, CVP 11, filling pressures low. CI 2.2 by TD. @khaycock2 @NephroP @msiuba


English

Comment 2.
Meaning, the high PVRI suggests a component of precapillary PH (in addition to LV failure) so that this is not just a plain RV failure that could respond to inotropic agents.
Likely needs pulmonary vasodilators (and closely monitoring of wedge pressures), since improvement of R to L flow can worsen left heart filling pressures given such LV systolic dysfunction
English

Agree that not straightforward
Is the patient breathing spontaneously?
I’m making that assumption for the comments below.
I’m also assuming that every tracing has been zeroed/leveled, etc
—-
Looks like your RAP (end of exhalation) is around 12ish, which fits your IVC images.
Wonder if you are primarily dealing with pressure overload on the right side (plus very low LVEF w/o much pulmonary congestion)
The visual TAPSE appears quite abnormal.
PAP around 38/28, mean 31 (end exhalation calcs), with PVRI around 9.5 WU/m2.
IMHO, pulmonary vasodilation and biventricular cardiac optimization might provide better results by improving forward flow.
**CAVEAT
I am curious if improving RV performance could worsen left heart filling pressures.
Not infrequently, we observe unmasking of diastolic dysfunction in “PAH” pts once you start pulmonary vasodilation, or improve RV function.
The left heart pressures might be currently “protected” due to the right heart failure/dysfunction.
English

@msiuba Congratulations, Matt. Very well deserved!
We and your fellows have all benefited from your many generous contributions.
GIF
English

@msiuba @RyanTedfordMD @AHajduczok @JasonKatzMD @rjbernardoMD @AnnGageMD @CardsNYC @IM_Crit_ @GiessenPh @RRVdpool @chatterJ5 @ThinkingCC Looking forward to reading it!!
English

A few potentially interested parties:
@RyanTedfordMD @AHajduczok @JasonKatzMD @FSotoMD @rjbernardoMD @AnnGageMD @CardsNYC @IM_Crit_ @GiessenPh @RRVdpool @chatterJ5 @ThinkingCC
English

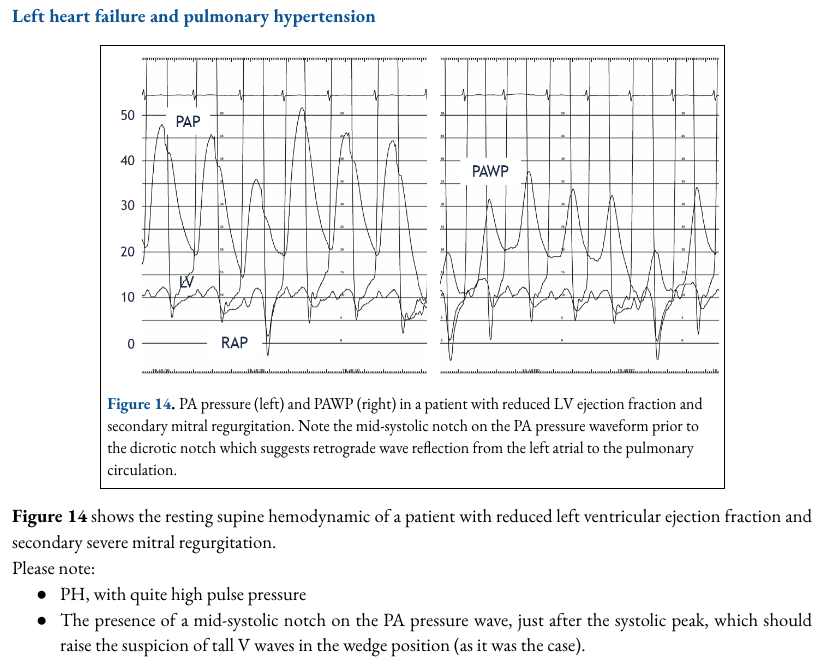
We present another publication-quality chapter from ShockWaves, the 1st chapter in the RHC section.
@CaravitaSergio presents a masterclass on the invasive PA waveform.
Section editors: @SophiaAirhartMD & @zilgiovineMD
Look out next week for the non-invasive correlates 👀

English

@redraiderpulmcc @UTK_PCCM Thanks Victor!
We are very excited that she matched with us. Your word and feedback reconfirms that! 🙏🏻
English
Francisco Soto, MD, MS, MBA retweetledi
Francisco Soto, MD, MS, MBA retweetledi

Let’s discuss “Contemporary Treatment of Pulmonary Arterial Hypertension: A U.S. Perspective”
Exciting PC Webinar on 11/25 2 PM EST ⏰ @ATS_PC
All star panelists @SandeepSahayMD @IoanaPreston @mardigomberg @JimWhiteCurePAH and MChakinala
Register here: bit.ly/4fyIz45

English

Important point 👍🏻
My opinion (but open to expert disagreement):
• With large V waves, “pulling” up the “a” wave, the WP is not truly higher than dPAP, but it’s an“artifactually” higher #
• If WP were truly ⬆️ than dPAP, it would cause backward flow
• In cases where the WP appears to truly be ⬆️ than dPAP (inaccurate #), confirmation with LVEDP should be considered
• Even in very tall V waves, I have “usually” found “a” waveform to correspond to = or < than PADP (see image 👇🏻of ⬆️ “v” wave and good WP (“a” wave/LVEDP correlation).
Not sure about the behavior in case of “giant” v waves
• I routinely capture the “wedge to PA pullback” for additional reassurance of WP to dPAP relation (shown on 🧵)
• Would love to see any examples of much higher WP than dPAP in large v waves (ideally with “pullback screens”)
Thanks for the comment!

English

@FSotoMD It actually might in some instances. Indeed mean WP is measured over the cardiac cycle while dPAP is a punctual value. When big V waves are present (severe MR, diastolic dysfunction, etc) the mean WP may results to be higher than dPAP. Do you agree?
English

@PacoDardon My 🤜🏻
Yes. For bedside PA caths, I
• Advance PAC into introducer to 20 cm PAC line
• Then, inflate 🎈full and advance with 🎈inflated (20cm PAC line will be at level of SVC or proximal RA)
• Always “sail away” with 🎈inflated
• Always “pull back to shore” with 🎈deflated
English

@FSotoMD Great thread!
I'm curious about this in particular, we usually inflate the balloon whilst in the RV in order for the catheter to be advanced in the direction of blood flow.
Do you advance your PA catheters completely deflated? And if so, when do you decide to inflate?
English

If you appreciated this thread, please:
PLEASE
• “Like” the thread (plus individual tweets if 👍🏻)
• Repost the FIRST tweet for others to benefit from this
#FOAMed
#MedTwitter
English