CrowdHealth
5.8K posts


CrowdHealth
@JoinCrowdHealth
EXIT THE SYSTEM! We provide easy to use tools that enable people to live free from the shackles of health insurance and the sickcare system.












A 47-year-old woman asked for an MRI. By the time her insurance company let her have one, the cancer in her hip was too far gone to save her leg. Her doctor had done the X-ray. Examined her. Sent her for physical therapy, the six weeks the insurer's own published criteria said she needed to complete before an MRI was on the table. No improvement. He told her she needed the scan. The insurance company said it was not medically necessary, until she finished six weeks of physical therapy. She had finished it. They had paid for it. He appealed. 38 days later, they reversed. The MRI showed sarcoma. The hospital told her that one month earlier, they could have treated it with chemotherapy alone. Instead, they amputated her leg, her hip, and her pelvis. She died two years later. Her family sued. The federal judge called it tragic, then threw the case out. Why? Because no law in New York holds an insurance company accountable when it gives bad medical advice. Doctors are accountable. Nurses are accountable. Hospitals are accountable. Insurance companies are not. That is the contrarian thesis worth holding onto. Prior authorization is not a billing decision. It is a medical decision being made by someone who, by law, is supposed to be a specialist in the relevant field, and who, by the federal HHS inspector general's own findings, often is not. When an insurer overrides a treating physician based on criteria the insurer itself does not follow, that is medical advice. When that advice causes harm, the law treats the insurer as untouchable. Every other party to the patient's care is held to a standard. The decision-maker with the most leverage is held to none. The framework worth saving: 1. By law, the reviewer denying a prior authorization is supposed to be a doctor in the relevant specialty. 2. The federal HHS inspector general has confirmed that often, they are not. 3. The published criteria insurers cite to defend denials are not always the criteria they actually follow. 4. Most insurance plans fall under ERISA, a federal statute that makes negligence cases against insurers nearly impossible. This case is in state court because the plan is for public employees, outside ERISA. 5. The AMA, the New York State medical society, and the Vermont and Connecticut medical societies have all filed amicus briefs supporting the family. Attorney Steve Cohen argued the case before the Second Circuit. Doctors who fight these denials should know what is at stake and who fought alongside them. Listen to the full conversation on The Podcast by KevinMD. Link in the replies. What is the longest a prior authorization denial has ever delayed care for one of your patients? #PriorAuth #ThePodcastbyKevinMD



People say Canadian healthcare is not free, because we pay taxes for it. But in America, people pay taxes and still have to pay for healthcare out of their pockets. And if they are broke, the hospital tells them to go die.

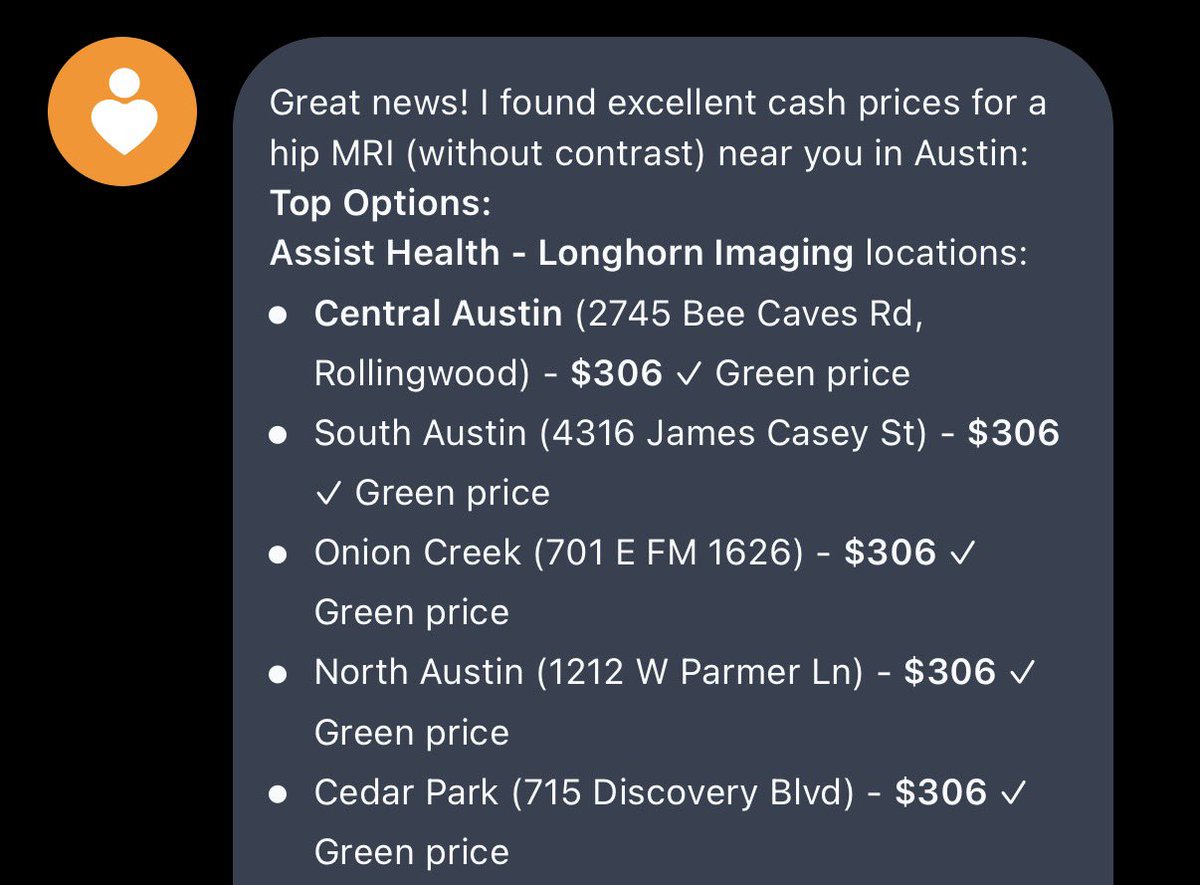
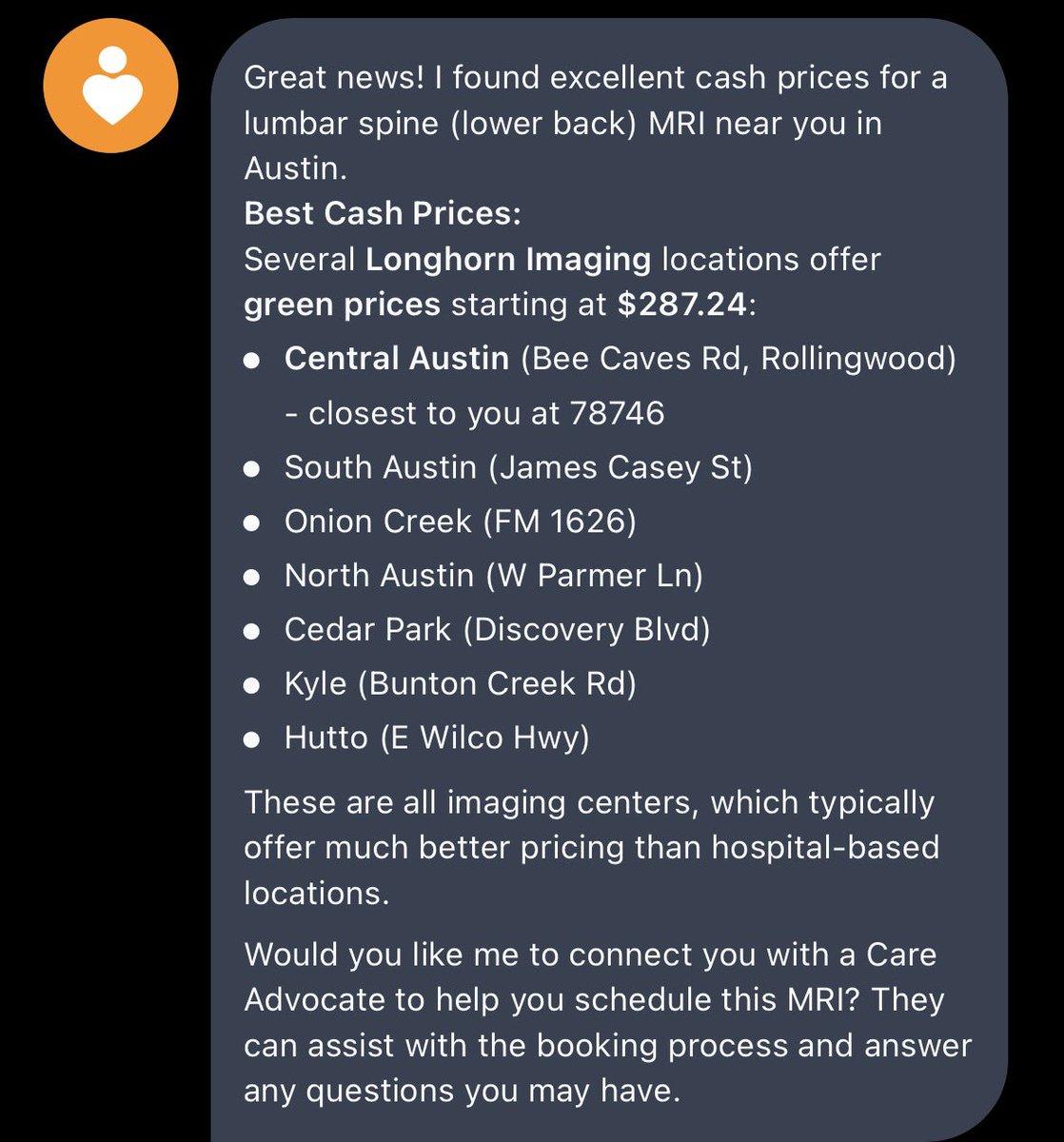
“They quoted me $5,100 for an MRI—with insurance.” “Without insurance, it drops to $700.” She asked to pay the $700. They refused—because she was insured. Health insurance is a legalized SCAM.





Texans deserve affordable healthcare, but right now there are twisted incentives in our system that are driving up costs. This is unsustainable. We had a great deep dive in the House Select Committee on Health Care Affordability during our hearing this week. Thanks to Chairman @RepJamesFrank for putting together our very informative panels and a robust agenda, and to Speaker @Burrows4TX for making the issue a House priority. I’m looking forward to working with my colleagues over the next weeks and months to find meaningful, market-driven solutions.