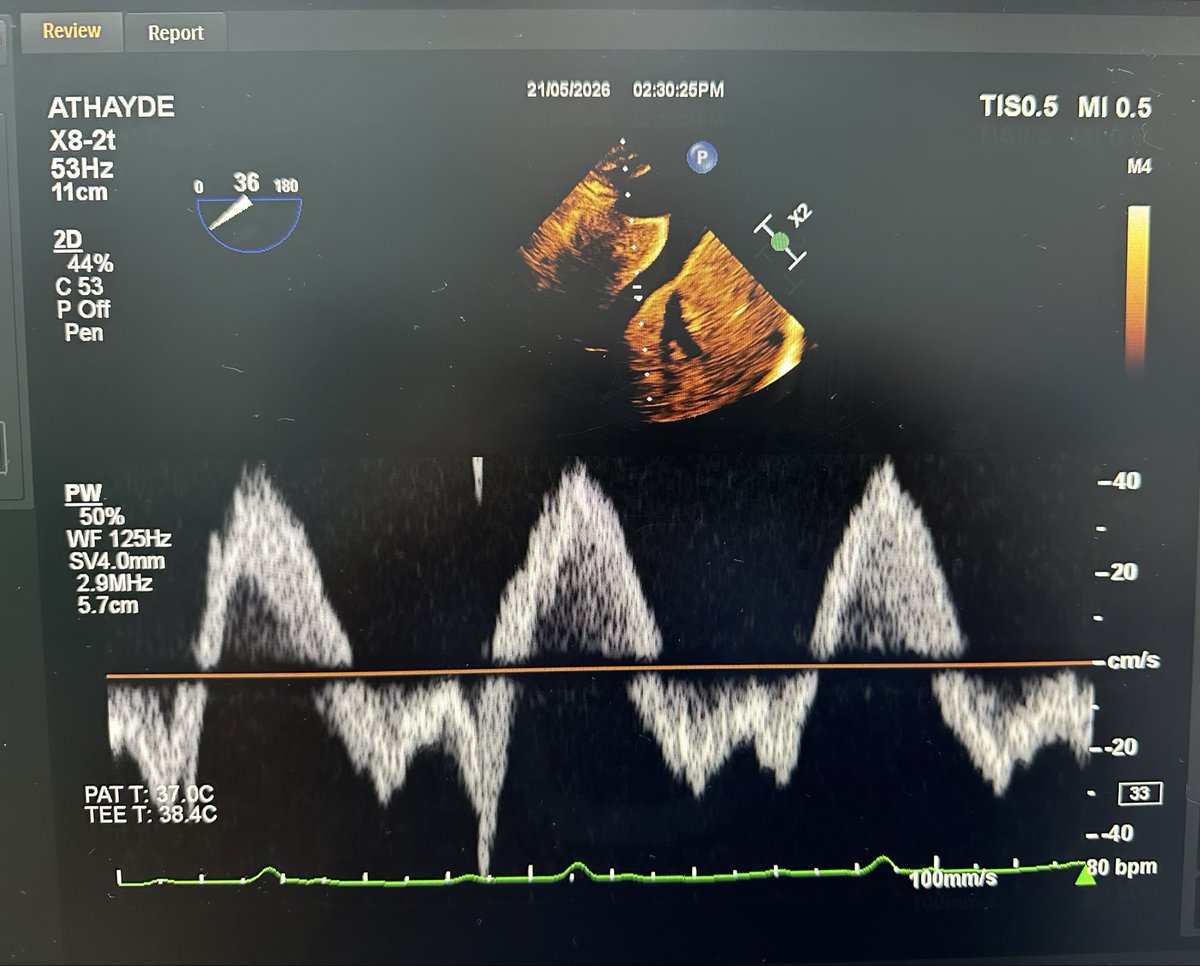
It’s well known that there is a certain delay between electrical activity and a mechanical phenomenon at the myocardial level. However, the temporal relationship between myocardial electrical activity and venous return flow has never been studied, so we will probably see these discrepancies between the Doppler spectrum of venous flow and the ECG. But it is only a theory; there is no evidence.
English